 |
 |
 |
| |
Narrowing the gap in life expectancy for HIV+ compared with HIV- individuals...Life Expectancy Gap Between HIV+ and HIV- Narrows But Persists
|
| |
| |
Conference on Retroviruses and Opportunistic Infections (CROI), February 22-25, 2016, Boston
Mark Mascolini
WEBCAST link: http://www.croiwebcasts.org/console/player/29469?mediaType=audio&
The gap in life expectancy between people with and without HIV narrowed from 44 years in 1996-1997 to 12 years in 2011, according to a matched analysis of people in the Kaiser Permanente healthcare system in California [1]. The gap closed even further--but persisted--in HIV patients who started antiretroviral therapy (ART) at a CD4 count at or above 500.
Previous research found that life spans of people with HIV are approaching those of the general population. But Kaiser researchers noted that these studies had limited ability to account for critical sociodemographic and lifestyle differences between HIV-positive and negative populations. Extensive electronic record keeping allowed the Kaiser team to compare HIV-positive and negative patients in their healthcare system more closely and perhaps to get a sharper focus on how life expectancy has changed over the years in HIV-positive versus HIV-negative people.
The analysis considered HIV-positive and negative adults in care sometime between 1996 and 2011. Kaiser investigators matched each HIV-positive person to 10 HIV-negative people by age, sex, medical center, and year. They collected mortality data from death certificates and the Social Security Administration, even for people who left the Kaiser healthcare system. The researchers used abridged life tables to estimate expected remaining life years at age 20. They considered life expectancy by study year, gender, race/ethnicity, HIV risk group, CD4 count when ART began, and three risk factors: viral hepatitis, drug or alcohol abuse, and smoking.
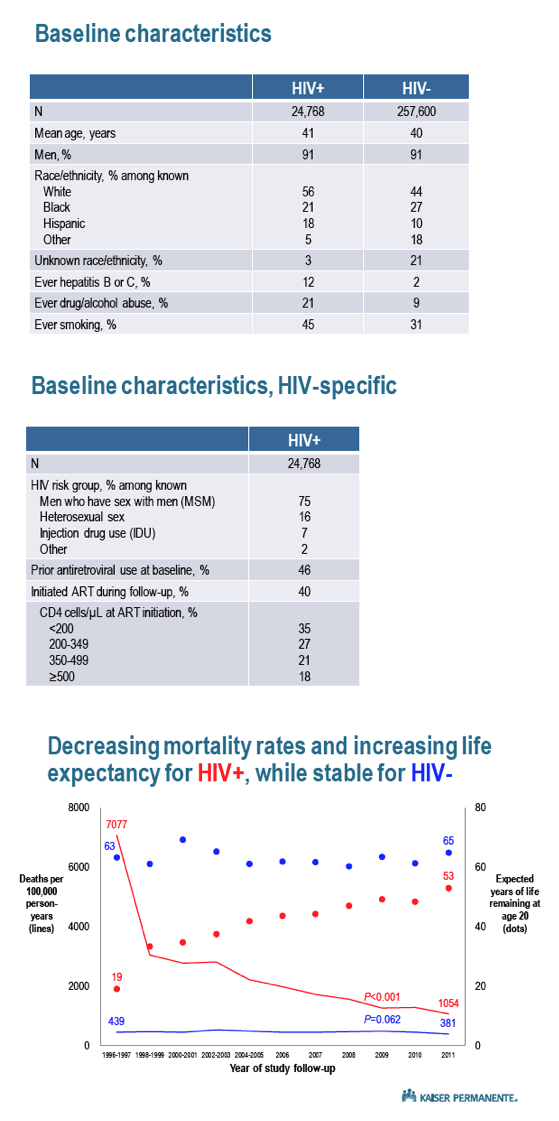
The study included 24,768 people with HIV and 257,600 without HIV. Age averaged 41 in the HIV group and 40 in the HIV-negative group; 91% of both groups were men. Whites made up 56% of the HIV group and 44% of the HIV-negative group. Respective proportions of blacks were 21% and 27% and of Hispanics 18% and 10%. Higher proportions of people with HIV ever smoked (45% versus 31%), had hepatitis B or C (12% versus 2%), or ever abused drugs or alcohol (21% versus 9%). In the HIV group, 75% became infected through sex between men, 16% through heterosexual sex, and 7% by injecting drugs. Among people who began ART, 18% did so at a CD4 count at or above 500.
From 1996-1997 to 2011, deaths per 100,000 person-years dropped from 7077 to 1054 in the HIV group (P < 0.001) while declining nonsignificantly in the HIV-negative group from 439 to 381 (P = 0.062). Expected life years remaining at age 20 jumped from 19 to 53 in the HIV group from 1996-1997 to 2011 while inching up from 63 to 65 in the HIV-negative group. Thus the gap between the groups shrunk from 44 years in 1996-1997 to 12 years in 2011.
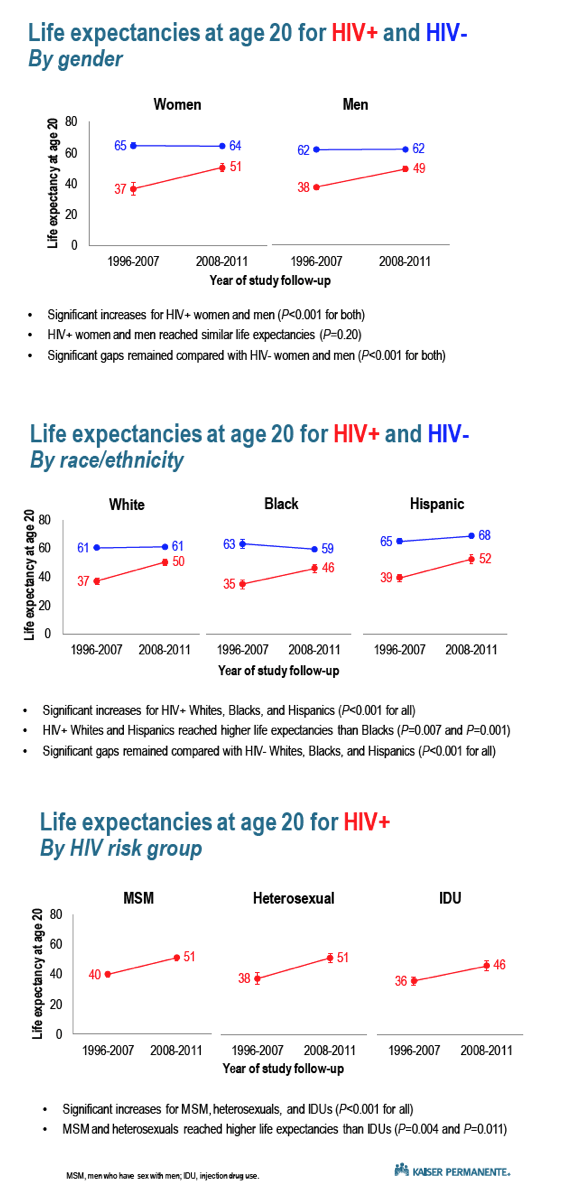
In people with HIV, additional life years at age 20 rose from 37 to 51 in women from 1996-2007 to 2008-2011 and from 38 to 49 in men. But in this comparison, significant gaps remained between life expectancy of HIV-negative women (64 additional years) and men (62 additional years) (P < 0.001 for both). From 1996-2007 to 2008-2011, life expectancy at age 20 improved from 37 to 50 more years in HIV-positive whites (versus 61 to 61 in controls), from 35 to 46 in blacks (versus 63 to 59 in controls), and from 39 to 52 in Hispanics (versus 65 to 68 in controls). The improvement among whites and Hispanics was significantly greater than among blacks (P = 0.007 and P = 0.001).
By HIV transmission risk group, gains in life expectancy at age 20 from 1996-2007 to 2008-2011 were similar in gay men (40 to 51 additional years) and heterosexuals (38 to 51) but less marked in injection drug users (36 to 46). All these improvements were statistically significant (P < 0.001), but improvements in gay men and heterosexuals were significantly greater than in drug users (P = 0.004 and P= 0.011).
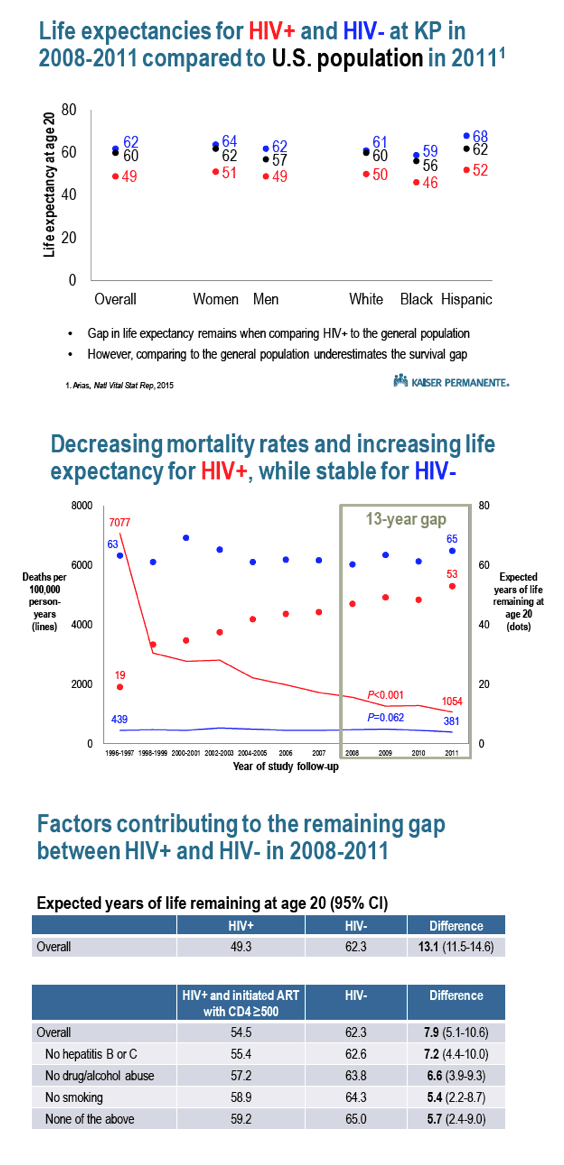
In 2008-2011, HIV-positive 20-year-olds could expect another 49.3 years of life, compared with 62.3 in HIV-negative people for a difference 13 years. That gap dwindled to 7.9 years when the researchers considered only HIV-positive people who started ART at a CD4 count of 500 or higher. And the gap shriveled further if early ART starters did not have hepatitis B or C (7.2 years), did not abuse alcohol or drugs (6.6 years), or did not smoke (5.4 years).


PROGRAM ABSTRACT- Survival of HIV-infected individuals has dramatically improved with combination antiretroviral therapy (ART). However, it is unclear how large a gap in life expectancy remains between HIV-infected and HIV-uninfected individuals, and how much of that gap is attributable to underlying differences in demographics or risk factors.
We conducted a cohort study of HIV-infected adults who were members of Kaiser Permanente California during 1996-2011, and HIV-uninfected members matched 10:1 on age, gender, medical center, and year. Deaths were comprehensively ascertained through 2011 from the electronic health record, California death certificates, and Social Security Administration datasets. We used abridged life tables to estimate the average number of years of life remaining at age 20 ("life expectancy at age 20") in HIV-infected and HIV-uninfected individuals in 1996-2006 and 2007-2011. For the recent era, we estimated life expectancy at age 20 by demographics and HIV risk group. We also estimated life expectancy in recent years among patients who initiated ART early (i.e., with CD4 ≥500 cells/μL), and in subgroups of these early-treated HIV patients and HIV-uninfected individuals without modifiable risk factors.
Among 25,768 HIV-infected and 257,600 HIV-uninfected individuals, there were 2,229 and 4,970 deaths, with mortality rates of 1,827 and 326 per 100,000 person-years, respectively. In 1996-2006, life expectancies at age 20 among HIV-infected and HIV-uninfected individuals were 36.0 and 62.3 years, respectively, corresponding with a gap of 26.3 years (95% confidence interval: 24.8-27.8). In 2007-2011, life expectancy at age 20 for HIV-infected individuals increased to 48.5 years, narrowing the gap to 13.8 years (Table). The lowest life expectancies at age 20 for HIV patients in 2007-2011 were among blacks (45.2 years) and those with a history of injection drug use (42.6 years). In 2007-2011, HIV patients who initiated ART with ≥500 cells/μL had a life expectancy at age 20 of 53.8 years, corresponding with a gap, relative to HIV-uninfected individuals, of 8.5 years. The gap narrowed further to 6-7 years in subgroups without a history of hepatitis B or C infection, drug/alcohol abuse, or smoking.
Even with early ART initiation, an approximately nine-year gap in life expectancy remains between HIV-infected and HIV-uninfected individuals with access to care. Mitigation of risk factors among HIV-infected individuals may further reduce the survival disparity.
"ART has dramatically improved survival," the Kaiser team concluded, "but HIV-positive individuals have not yet reached a normal life expectancy." Besides starting ART promptly, they proposed that other risk-reduction strategies--like quitting smoking--could narrow the survival gap between people with and without HIV.
Reference
1. Marcus JL, Chao C, Leyden W, et al. Narrowing the gap in life expectancy for HIV+ compared with HIV- individuals. Conference on Retroviruses and Opportunistic Infections (CROI), February 22-25, 2016, Boston. Abstract 54.


|
| |
|
 |
 |
|
|