 |
 |
 |
| |
Poor HIV Control, Black Race, Female Sex Boost Stroke Risk in US Cohort
|
| |
| |
Conference on Retroviruses and Opportunistic Infections (CROI), February 22-25, 2016, Boston
Mark Mascolini
A viral load above 200 copies conferred the same risk of stroke or transient ischemic attack (TIA) as 15 years of age in a longitudinal analysis of the US ALLRT cohort [1]. Blacks had higher stroke/TIA incidence than whites or Hispanics, and women--particularly those in their 40s--had higher incidence than men.
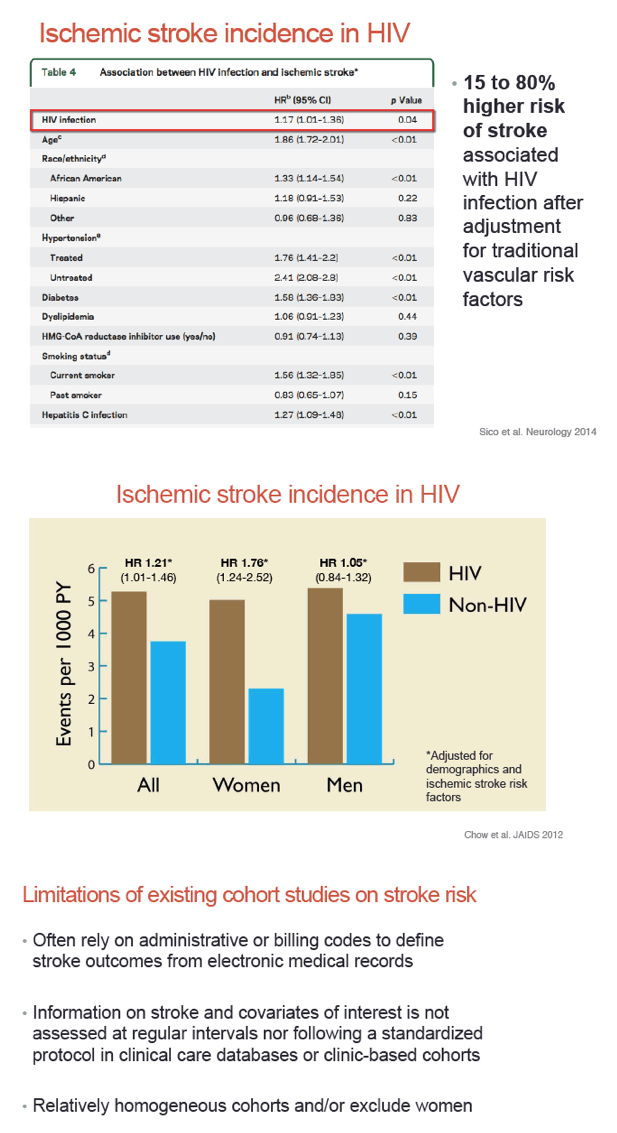
People with HIV infection have a higher stroke incidence than HIV-negative people the same age [2]. To learn more about stroke risk factors in people with HIV, researchers plumbed data from the ACTG Longitudinal Linked Randomized Trials (ALLRT) cohort and its parent studies.
The analysis focused on 6933 people without a history of stroke who began their first antiretroviral regimen between 1998 and 2011. The group included 1370 women (20%). Similar proportions of participants were white (40%) or black (37%), with lower proportions of Hispanics (21%) and others. Median age at study entry stood at 37 years. Only 625 people (9%) had a drug injection history, and only 14 people currently injected drugs. Median baseline CD4 count and viral load were 243 cells and 57,624 copies.
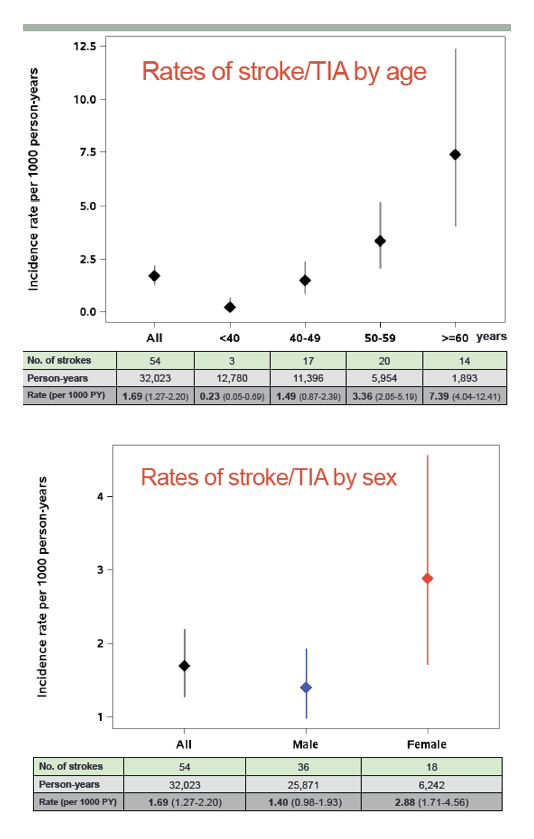
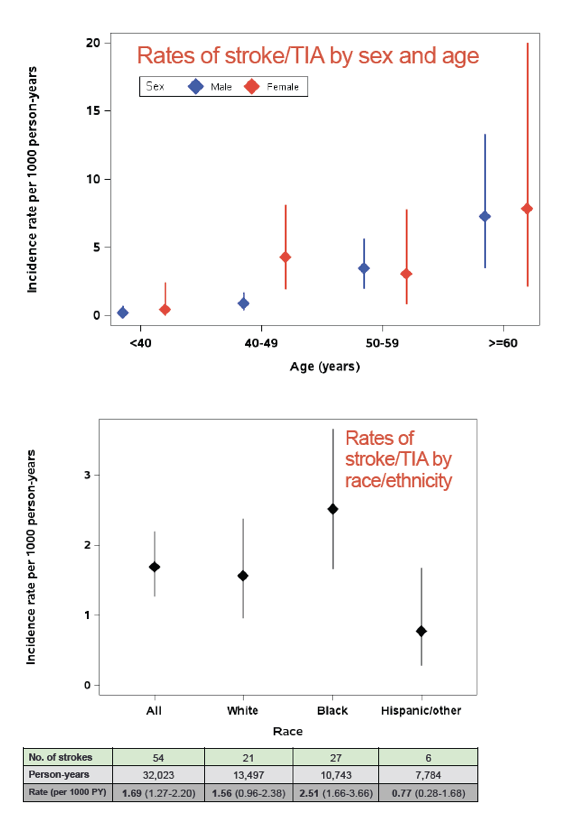
Overall incidence of stroke or TIA measured 1.69 per 1000 person-years. That rate rose from 0.23 in people under 40 to 1.49 in the 40-to-49 group, 3.36 in the 50-to-59 group, and 7.39 in older people. Stroke/TIA incidence was higher in women than men (2.88 versus 1.40 per 1000 person-years). People between 40 and 49 years old accounted for almost all of this difference between women and men; in other age groups the stroke/TIA rate was similar in women and men. Stroke/TIA incidence was higher in blacks (2.51 per 1000 person-years) than in whites (1.56) or Hispanics and others (0.77).
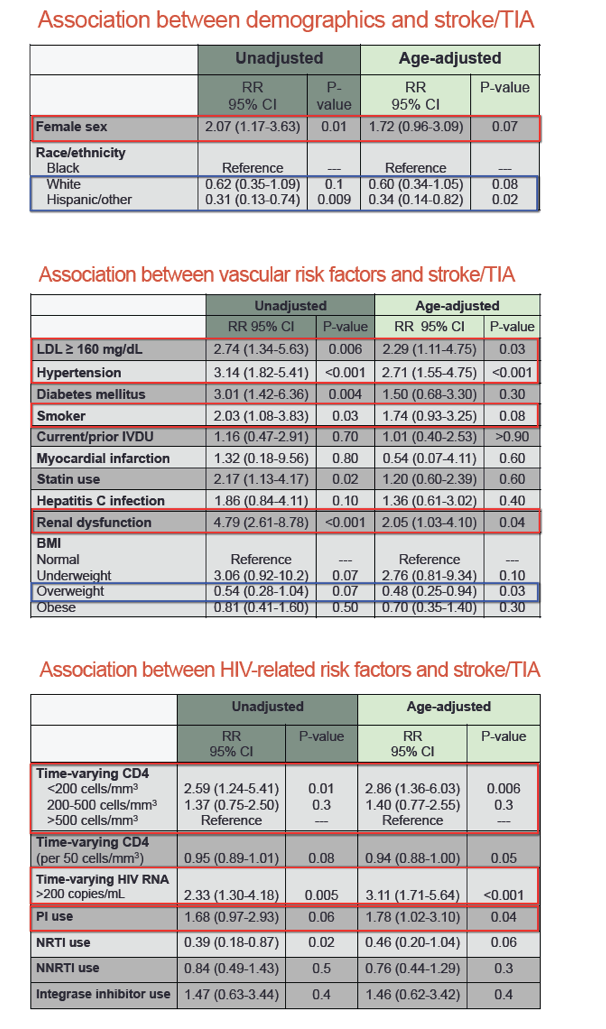
In an age-adjusted analysis, women had a 72% higher stroke/TIA risk than men, but that difference fell just short of statistical significance (relative risk [RR] 1.72, 95% confidence interval [CI] 0.96 to 3.09, P = 0.07). The Hispanic/other group had a significantly lower stroke/TIA risk than blacks (RR 0.34, 95% CI 0.14 to 0.82, P = 0.02). The lower stroke/TIA risk in whites than blacks stopped short of statistical significance (RR 0.60, 95% CI 0.34 to 1.05, P = 0.08).
Age-adjusted analysis identified several other independent predictors of stroke/TIA:
-- Low-density lipoprotein cholesterol >/= 160 mg/dL: RR 2.29, P = 0.03
-- Hypertension: RR 2.71, P < 0.001
-- Renal dysfunction: RR 2.05, P = 0.04
-- CD4 count below 200 versus above 500: RR 2.86, P = 0.006
-- Viral load above 200 copies versus below: RR 3.11, P < 0.001
-- Protease inhibitor use: RR 1.78, P = 0.04
A separate analysis to determine the adjusted relative risk of stroke/TIA pinpointed four risk factors:
-- Every 10 years of age: RR 2.10
-- Time-varying LDL >/= 160 mg/dL: RR 2.54
-- Hypertension: RR 2.79
-- Time-varying viral load above 200 copies: RR 3.10
The researchers observed that the link between an unsuppressed viral load and higher stroke/TIA risk corresponds to the impact of aging 15 years. They stressed that both hypertension and high LDL cholesterol conferred more than a 2.5-fold greater risk of stroke/TIA.
References
1. Chow F, Wilson MR, Wu K Ellis R, Bosch R, Linas BP. Stroke incidence highest in women and black HIV-infected participants in ALLRT cohort. Conference on Retroviruses and Opportunistic Infections (CROI), February 22-25, 2016, Boston. Abstract 43.
2. Chow FC, Regan S, Feske S, Meigs JB, Grinspoon SK, Triant VA. Comparison of ischemic stroke incidence in HIV-infected and non-HIV-infected patients in a US health care system. J Acquir Immune Defic Syndr. 2012;60:351-358. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3670086/
--------------
Reported by Jules Levin
STROKE INCIDENCE HIGHEST IN WOMEN AND BLACK HIV-INFECTED PARTICIPANTS IN ALLRT COHORT
Felicia C. Chow1, Michael R. Wilson1, Kunling Wu2, Ron Ellis3, Ronald Bosch2, Benjamin Linas4
1University of California, San Francisco, Department of Neurology 2Center for Biostatistics in AIDS Research, Department of Biostatistics, Harvard
School of Public Health 3University of California, San Diego, Department of Neurology 4Boston University School of Medicine, Department of Medicine




|
| |
|
 |
 |
|
|