 |
 |
 |
| |
The Additional Impact of Chronic Kidney Disease on Cardiovascular Outcomes and Death Among HCV Patients
|
| |
| |
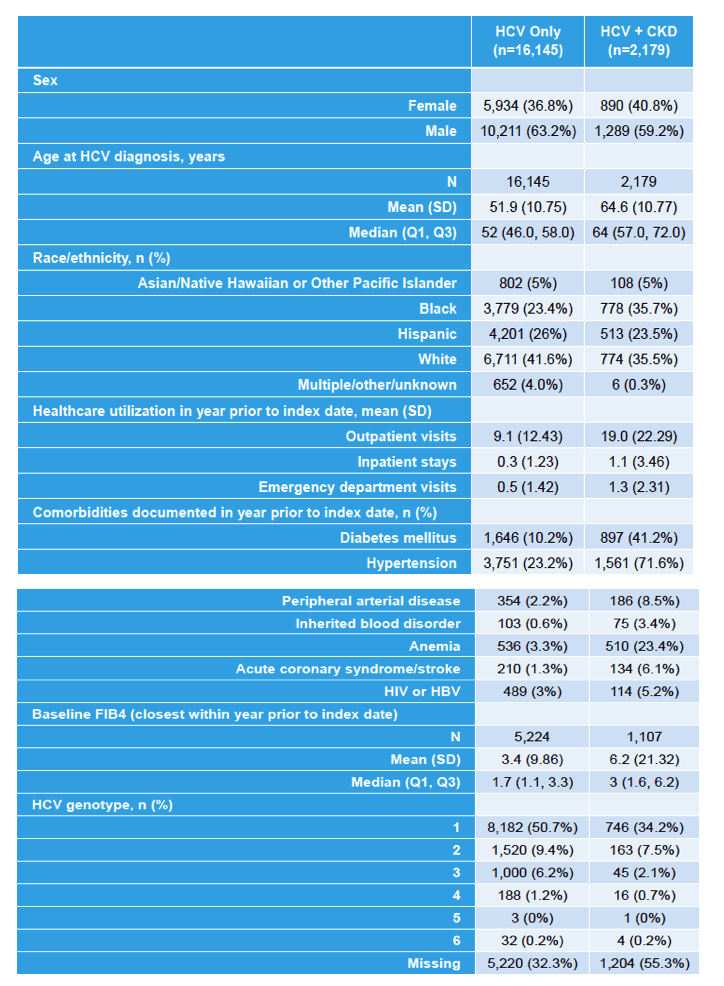
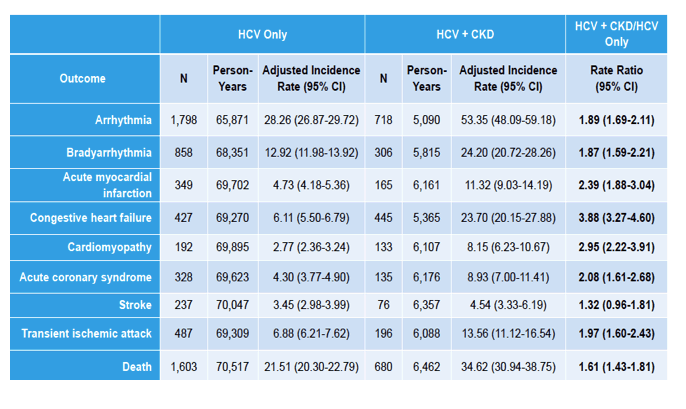
'kidney disease associated with 60% death increase....patients with HCV+CKD more likely to be Black, more likely to have comorbidities & heart disease'
Reported by Jules Levin
EASL 2016 April 14-17 Barcelona
Sara Y Tartof1; Jean Marie Arduino3; Rong Wei1; Jin-Wen Hsu1; Kevin B Rubenstein2; Haihong Hu2; Michael Horberg2; Stephen Derose1; Steven Jacobsen1; Carla V Rodriguez2
1Department of Research & Evaluation, Kaiser Permanente Southern California, Pasadena, CA, USA; 2Mid-Atlantic Permanente Research Institute, Kaiser Permanente Mid-Atlantic States, Rockville, MD, USA; 3Merck & Co., Inc., Kenilworth, NJ, USA
from Jules: the impact of not treating HCV+ with a history of drug abuse & IDU clearly is reflected in this study, the long term cost to healthcare system is dismissed when restrictions prevent treating this patient population, it is short-sighted & not cost-effective. There is no other disease for which those with a history of substance abuse are restricted from receiving treatment: heart disease; diabetes, etc. What gets forgotten in the claims by insurers in imposing restrictions because of costs is that HCV is a cure with a one-time 12 week treatment with 95% SVR rates. In the US domestically the annual cot for HIV for Medicaid & Medicare is $10 Billion. The cost to treat HCV is nothing compared to that. For example, in NYS there are 57,000 patients on Medicaid with HCV, with the current costs of HCV drug regimens of about $35000 it would cost NYS a one-time expense of $2.5 billion to treat all with HCV in Medicaid, instead NYS restricts access to these medications for those with a history of substance. NYS spends more every year on HIV ARTs than HCV drugs & it is an annual cost that goes on forever.


|
| |
|
 |
 |
|
|