| |
Predicting HIV-Life Expectancy, Comorbidities - Lifeexpectancyin HIV-positive persons in Switzerland: matched comparison with general population
|
| |
| |
Download the PDF here
from Jules: a new recent publication [full report below following links] reports on estimate to predict Life Expectancy in HIV in Swiss Cohort, reported previously at conference and reflects the problem with all these studies that try to estimate life expectancy. They are all estimates of a question that is impossible to predict because this study does not include consideration of comorbidities among aging patients, and none of the studies do that, and it is impossible to predict life expectancy even if you were to try to include comorbidities because no one knows the survival outcomes when patients over 60 years old have comorbidities. And by the way none of these studies can report on quality of life in older aging patients -BUT here are some recent presentations at Glasgow & Comorbidities/Aging Workshop,that reflect on how survival will be affected by aging & comorbidities; not to mention the costs associated with aging which everyone overlooks. and the burden the costs will be on HIV healthcare systems .....[ of note in looking at Table 3 below from the Swiss Cohort study nadir Cd4 <200 reduces estimate of life expectancy by 6 years.
And by the way none of these studies can report on quality of life in older aging patients
Data from 2005 Medicare expenditure costs, indicate that the annual costs for Medicare beneficiaries with one chronic condition are $7,172, and for beneficiaries with three or more chronic conditions $32,498.....50% in Wash DC not getting treated for comorbidities: study at Aging Workshop reports from large federal database
Glasgow: HEALTH-RELATED COSTS IN CHRONIC HIV INFECTION: A CASE-CONTROL STUDY VS. GENERAL POPULATION USING A CLAIMS-BASED APPROACH IN GERMANY....healthcare/drug costs soar for HIV+ aging compared to HIV-neg . - (11/08/16)
Glasgow: COMORBITY IN CHRONIC HIV INFECTION A CASE-CONTROL STUDY IN GERMANY USING HEALTH INSURANCE CLAIMS DATA [Examines 70-80+ Year Olds. Higher Prevalence of Comorbidities in HIV+ vs HIV-neg] - (11/08/16)
Italy: 50% frail now, 50% > 50 Years Old Projected to Increase a Lot.....Frailty / Aging Projections in Italy - Future challenges for clinical care of an ageing population infected with HIV: a "geriatric -HIV" modelling study .....Frailty 50% Now, Predicted to be 75% in Older Aging HIV in 14 years, requiring a large number of patients, perhaps 40%, to be confined in old age homes because they will not be able to function
GLASGOW: Mortality rates and excess mortality among HIV-positive persons according to age in Spain, 2004-2014 - (11/08/16)
Chicago Aging Cohort: Many aging HIV+ patients live alone, and the interplay of co-morbidities, poly-pharmacy, memory issues, and falls places them at an increased risk for non-independent living at an earlier age than the general population......median age stood at 56 years.....40% reported mental health is a concern...42% reported a history of depression.....One third reported memory problems or concerns, and 27% reported one or more falls in the past 12 months.....46%, lived alone.....54% took four or more prescription medicines daily".....IDSA: Assessing the needs of older HIV+ adults; Initial data from the CORE Healthy Aging Initiative (CHAI) - Money, Mental Health, Housing Top List of Concerns in Older HIV+ Chicago Group
GLASGOW: Proportion of US HIV Patients With 3 or More Comorbidities Will Rise 4-Fold by 2035
EuroSIDA - Doubling of Some Comorbidities - GLASGOW: Rates of All Age-Related Comorbidities Rise in EuroSIDA From 2006 to 2014
GLASGOW: Doubled & Tripled Rates of Comorbidities France - Prevalence of All Comorbidities Up From 2004 to 2014 in Big French Cohort. .
Anal cancer incidence is on the rise among US HIV-positive MSM, with rates as much as 37-fold higher than the in the general population
Increased risk of infection-related malignancies (IRMs) and infection-unrelated malignancies (IURMs) The incidences of both IURMs and IRMs increased with older age. It was projected that the incidence of IRMs would decrease by 29% over a 5-year period from 3.1 (95% CI 1.5-5.9) per 1000 person-years in 2011, whereas the IURM incidence would increase by 44% from 4.1 (95% CI 2.2-7.2) per 1000 person-years over the same period
Medicare HIV+ beneficiaries Comorbidities Prevalence...... HIV+ >65 on Medicare Have 2 Times More Comorbidities vs HIV-neg AND Blacks & Latinos Have 4-Fold Increased Risk for the 5 Comorbidities Examined vs Whites - CDC Report Chronic health conditions in medicare beneficiaries 65 years and older with HIV infection.
Aging in US - Worse Still To Come - polypharmacy, multiple comorbidities, decreased survival, impaired daily activities functioning - (12/21/16)
--------------------------
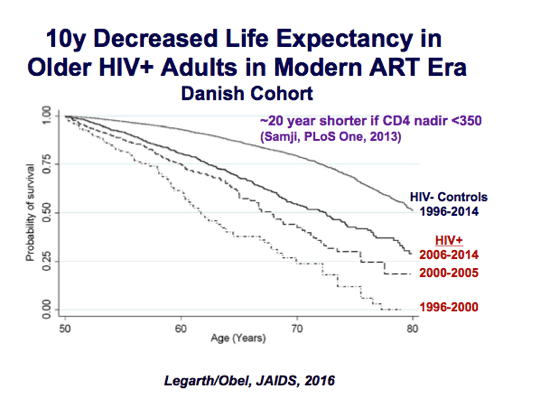
IAC: Aging & Inflammation: 10 yrs decreased life expectancy/T-cell activation remind high despite viral suppression/inflammation markers predict disease & death- "Pathophysiology of Non-Communicable Diseases in Treated HIV Infection: Is there a common path?" talk by Peter Hunt - (07/22/16)
Long-Term Mortality in HIV-Infected Individuals 50 Years or Older -Among HIV-infected individuals without comorbidity the estimated median survival time from age 50 years was 25.6 years (to age 75.6 years) (95% CI: 23.8 to NA) compared with 34.2 years (age 84.2 years) (95% CI: 29.6 to 38.3) among population controls without comorbidity. MRR was 1.7 (95% CI: 1.2 to 2.3) for HIV-infected individuals compared with population controls .....In our study the proportion of HIV-infected individuals ≥50 years with CCI ≥ 1 at study inclusion was higher than among the age-matched population controls. Lohse et al19 has previously shown that comorbidity achieved before HIV-diagnosis substantially influences mortality following HIV-diagnosis, and that HIV-infection and comorbidity interact synergistically with the risk of death among HIV-infected individuals. In our study we included a well-treated subpopulation of HIV-infected individuals ≥50 years with undetectable HIV RNA and CD4 cell count ≥350 cells per microliter after 1 year of cART. We detected a 1.6-fold increased risk of death of among HIV-infected individuals ≥ 50 years without comorbidity compared with population controls without comorbidity, which is in line with the findings of Lohse et al who found a 1.7-fold increased mortality in HIV-infected individuals with CCI = 0 compared with population controls with CCI = 0.
-------------------
In 2008-2011, HIV-positive 20-year-olds could expect another 49.3 years of life, compared with 62.3 in HIV-negative people for a difference 13 years. That gap dwindled to 7.9 years when the researchers considered only HIV-positive people who started ART at a CD4 count of 500 or higher. And the gap shriveled further if early ART starters did not have hepatitis B or C (7.2 years), did not abuse alcohol or drugs (6.6 years), or did not smoke (5.4 years).....http://www.natap.org/2016/CROI/croi_25.htm
A recent 282,000-person comparison of people with versus without HIV in the US Kaiser Permanente healthcare system found that the difference in life expectancy narrowed from 44 years in 1996-1997 to 12 years in 2011 [2]. But the gap persisted in 2011 even among people who started antiretroviral therapy at a CD4 count above 500. In a nationwide study of HIV-positive people in Denmark, survival at age 50 doubled from 11.8 years in 1996-1999 to 22.8 years in 2006-2014 [3]. But people with HIV still had a shorter life expectancy than people the same age and gender in the general population......http://www.natap.org/2016/IAC/IAC_27.htm
-----------------------
Life expectancy in HIV-positive persons in Switzerland: matched comparison with general population. AIDS
Gueler et al. analyzed life expectancy in the Swiss HIV Cohort Study 1988–2013 and compared life expectancy across levels of education with life expectancy in the general Swiss population, using matched controls from the Swiss National Cohort. 16’532 HIV-positive patients from the Swiss HIV Cohort Study and 927’583 residents from the Swiss National Cohort were included.
The proportion of patients who died during follow-up declined from 65.1% among patients enrolled in the monotherapy era to 2.4% among those enrolled in the most recent combination antiretroviral therapy (cART) era. In the most recent cART era, life expectancy at age 20 years was 52.7 years among participants with compulsory education, compared to 60.0 years among those with higher education. Only slight increases were observed in the general population, from 62.3 to 63.0 years overall, and from 61.1 to 61.5 years in people with compulsory education, and from 65.4 to 65.6 years in people with higher education.
In the most recent cART period, HIV-positive people continued to have an estimated life expectancy that was lower than their peers from the general population. Life expectancy in highly educated HIV-positive patients was similar to the life expectancy of individuals from the general population with compulsory education only. Male sex, smoking, injection drug use, and low CD4+cell counts at enrolment were independently associated with mortality.
In conclusion, the study-results suggest that life expectancy among HIV-positive persons could be further improved and educational inequalities reduced by earlier start of cART and effective smoking-cessation programs tailored to the HIV-positive population.
------------------------
Life expectancy in HIV-positive persons in Switzerland: matched comparison with general population.
AIDS Nov 2016 Gueler, Aysel; Moser, André; Calmy, Alexandra; Günthard, Huldrych F.; Bernasconi, Enos; Furrer, Hansjakob; Fux, Christoph A.; Battegay, Manuel; Cavassini, Matthias; Vernazza, Pietro; Zwahlen, Marcel; Egger, Matthias; for the Swiss HIV Cohort Study, Swiss National Cohort
Abstract
Objectives: To estimate life expectancy (LE) over 25 years in HIV-positive people and compare their LE with recent estimates for the general population, by education.
Methods: Patients aged 20 years or older enrolled in the Swiss HIV Cohort Study 1988-2013 were eligible. Patients alive in 2001 were matched to up to 100 Swiss residents, by sex, year of birth, and education. LE at age 20 was estimated for monotherapy (1988-1991), dual therapy (1992-1995), early combination antiretroviral therapy (cART, 1996-1998), later cART (1999-2005) and recent cART (2006-2013) eras. Parametric survival regression was used to model life expectancy.
Results: 16,532 HIV-positive patients and 927,583 residents were included. LE at age 20 of HIV-positive individuals increased from 11.8 years (95% CI 11.2-12.5) in the monotherapy era to 54.9 years (95% CI 51.2-59.6) in the most recent cART era. Differences in LE across educational levels emerged with cART. In the most recent cART period, LE at age 20 years was 52.7 years (95% CI 46.4-60.1) with compulsory education, compared to 60.0 years (53.4-67.8) with higher education. Estimates for the general population were 61.5 years and 65.6 years, respectively. Male sex, smoking, injection drug use and low CD4 counts at enrolment were also independently associated with mortality.
Conclusion: In Switzerland educational inequalities in LE were larger among HIV-infected persons than in the general population. Highly educated HIV-positive people have an estimated LE similar to Swiss residents with compulsory education. Earlier start of cART and effective smoking cessation programs could improve HIV-positive LE further and reduce inequalities.
|
|
| |
| |
|
|
|