| |
Pitavastatin 4 mg vs. Pravastatin 40 mg in HIV Dyslipidemia: Post-Hoc
Analysis of the INTREPID Trial Based on the Independent CHD Risk Factor for Age / Inflammation / Heart Disease Problem in HIV
|
| |
| |
Download the PDF here
Download the PDF here
------------------
Editorial from - Colleen Hadigan, MD; Catharine I. Paules, MD; Anthony S. Fauci, MD, National Institute of Allergy and Infectious Diseases
December 21, 2016
JAMA Cardiol.
Association Between Human Immunodeficiency Virus Infection and Cardiovascular Diseases - Finding a Solution to Double Jeopardy
......concomitant with this favorable outcome, noninfectious causes of morbidity and mortality, particularly cardiovascular disease (CVD), have had a disproportionately negative affect on ART-treated individuals with HIV, creating a “double jeopardy” phenomenon.
Traditional risk factors for CVD, exposure to ART, and the inherent immune activation associated with HIV infection all contribute to the increased incidence of CVD and may represent targets for intervention. Traditional CVD risk factors, such as hypertension, diabetes, smoking, and dyslipidemia, are increased among HIV-infected individuals and play a role in the development of CVD.2
Hepatitis C virus (HCV) coinfection is also common in HIV-infected individuals and has been shown to increase the risk of CVD in these patients independent of other risk factors.6
Independent of traditional risk factors and exposure to ART, HIV infection alone has been shown to increase the risk of CVD. Chronic inflammation and immune activation associated with HIV infection are widely felt to be key mediators of end-organ injury, including atherosclerosis, and appear to play a role in CVD even when HIV replication is seemingly well-controlled when receiving ART. Human immunodeficiency virus–infected individuals have significantly increased levels of inflammatory biomarkers, such as C-reactive protein, interleukin 6, D-dimer, and cystatin C, which have all been associated with CVD risk.7 Additionally, arterial inflammation in HIV has been associated with increased plasma levels of soluble cluster of differentiation 163, a monocyte/macrophage marker linked to low-grade inflammation and atherosclerosis.8
Lipid-lowering agents, such as statins, are used to mitigate CVD risk in the general population and have a wide range of immunomodulatory effects that may prove particularly beneficial for individuals with HIV. Administrative health care database research indicates decreased rates of MI in HIV–infected patients were associated with increased prescribing of lipid-lowering therapy between 1996 and 2011.11 To further investigate the role of statins in decreasing CVD risk in HIV–infected individuals, a clinical trial funded by the National Institutes of Health called REPRIEVE began in 2015.
As life expectancy in patients with HIV receiving ART continues to approach that of the general population, CVD will play an increasing role in morbidity and mortality.
-----------------------------------
http://www.natap.org/2012/CROI/croi_69.htm Consequences of Inflammation - CVD. The relation between CVD and inflammation in well established both in HIV and the general population. Soluble CD14 (sCD14) is a marker of monocyte/macrophage activation, which is pathogenically important in the development of atherosclerotic plaque. sCD14 is also used as a marker of microbial translocation, since CD14 is a major receptor for bacterial lipopolysaccharide (LPS). Kelisides et al. (abstr. 122) presented a study of HIV+ individuals (n=55) and matched HIV-negative controls (n=36), all at fairly low risk for CVD, who had baseline biomarkers measured and were followed longitudinally with measurement of carotid intima-media thickness (cIMT), an established correlate of atherosclerotic vascular disease. In an multivariable analysis adjusting for many potentially confounding variables, baseline levels of sCD14 and LPS were strongly and independently correlated with the rate of increase of cIMT [plaque/heart disease] over 96 weeks of follow-up. This correlation was seen in the HIV+ but not the HIV-negative group.
ASM: Effects of Pitavastatin on Markers of Arterial Inflammation and Immune Activation in HIV Patients - (06/24/16)
http://www.natap.org/2016/HIV/062416_01.htm
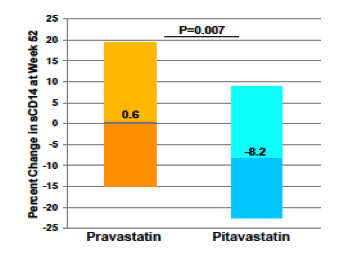
At Week 52, participants randomized to pitavastatin demonstrated significantly greater reductions in sCD14 (P=0.007) (Figure 2a), OxLDL (P=0.02) (Figure 2b) and Lp-PLA2 (P=0.003) (Figure 2c), compared to participants randomized to pravastatin, whereas changes in other markers were similar between the groups at 52 weeks. Greater effects on LDL-C were seen in the pitavastatin group (-31% vs. -21% pitavastatin vs. pravastatin)....Conclusions: Pitavastatin significantly lowered sCD14, OxLDL and Lp-PLA-2 over 52 weeks in dyslipidemic HIV participants. These effects were more prominent than seen with pravastatin, a commonly prescribed statin in HIV. Combined with more potent efficacy on LDL-C, these novel results suggest that pitavastatin may be an ideal statin to optimally improve lipids and inflammatory markers in HV-infected patients. Further studies are needed to determine if these effects translate into improved CVD events in the HIV population.
-------------------------
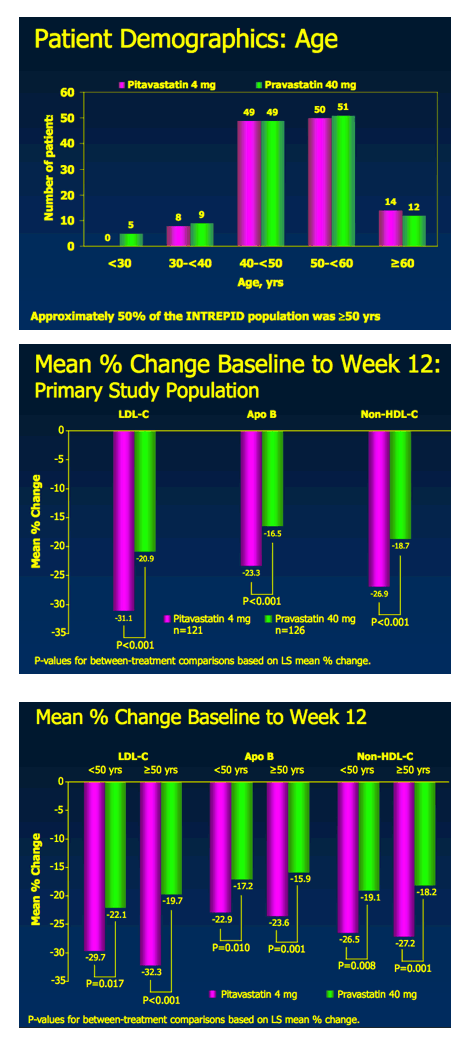
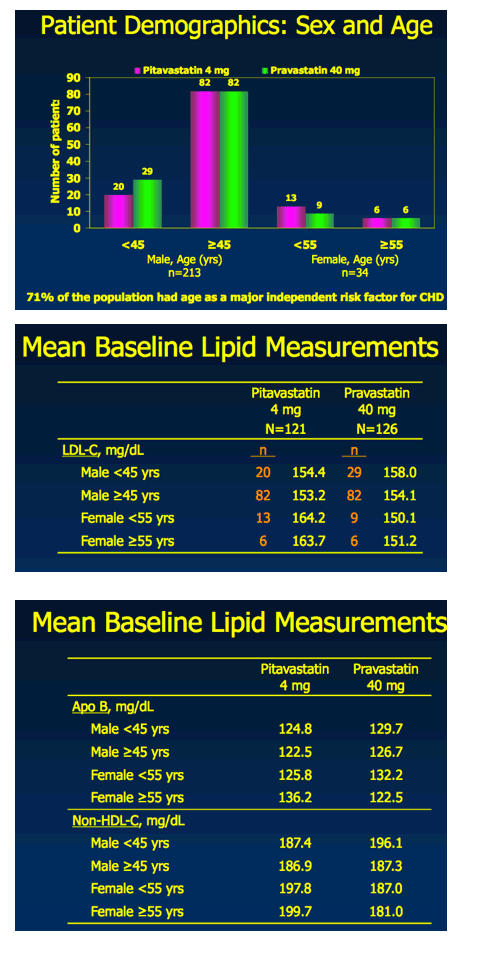
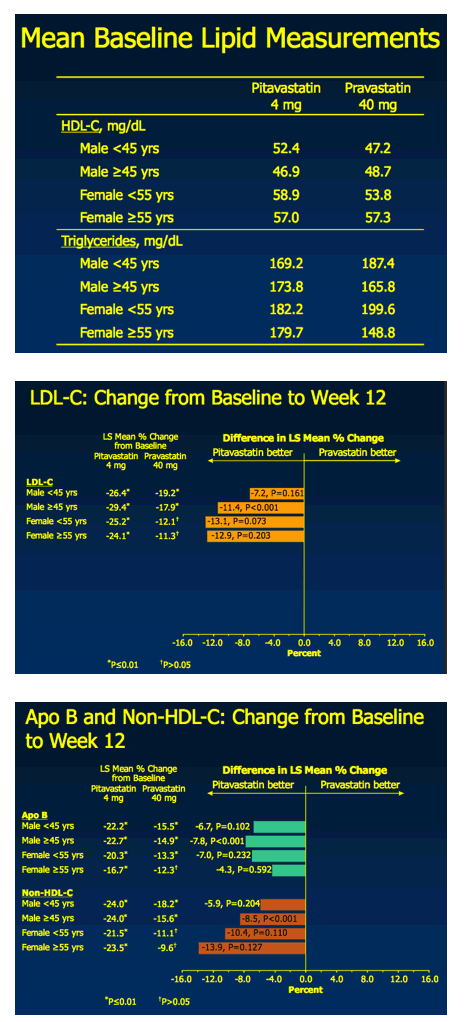
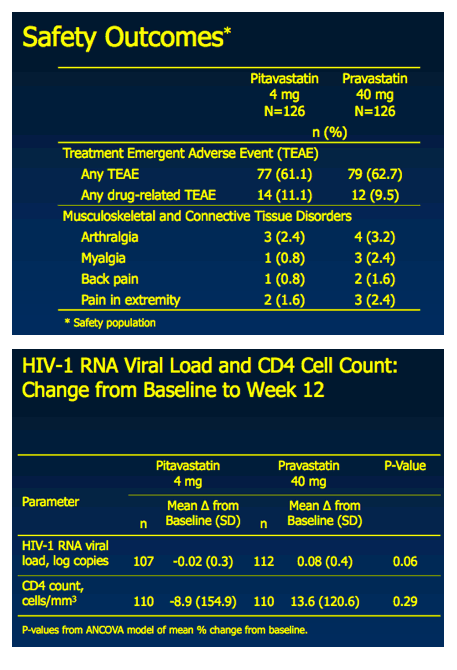
Pitavastatin 4 mg vs. Pravastatin 40 mg in HIV Dyslipidemia: Post-Hoc
Analysis of the INTREPID Trial Based on the Independent CHD Risk Factor for Age
Reported by Jules Levin
Aging Workshop 2013
Craig A. Sponseller, Masaya Tanahashi,
Hideki Suganami, Vladimir A. Kryzhanovski,
Judith A. Aberg





|
|
| |
| |
|
|
|