 |
 |
 |
| |
Antiretroviral treatment adherence, viremia, and psychiatric diagnosis throughout adolescence among perinatally HIV-infected youth.....
|
| |
| |
Reported by Jules Levin
Durban 2016 July 18-22
"53% of youth had any disorder, 35% missed doses in the past week, and 47% had a VL>1000"
[from Jules: this is a public health issue because mood disorder, disruptive behavior, substance use, anxiety associated with poor adherence & viral load > 1000 - remember detectable viral load & sub-optimal CD4 response to HAART increase risk for developing inflammation, immune activation and thus comorbidities & accelerated aging - authors conclude: an integrated care system that includes addressing mental health can improve adherence & health outcomes - meaning fiscal savings as well; this applies to adults as well]

Presenter
Claude Ann Mellins
Authors
A. Bucek1, C.-S. Leu1, S. Benson1, P. Warne1, E. Abrams2, K.S. Elkington1, C. Dolezal1, A. Wiznia3, C.A. Mellins1
Institutions
1Columbia University, HIV Center for Clinical and Behavioral Studies, New York, United States, 2ICAP, Columbia University, Mailman School of Public Health, New York, United States, 3Jacobi Medical Center, Albert Einstein College of Medicine, Bronx, United States
ABSTRACT
Background: Adolescence is associated with suboptimal medication adherence and is a time of increased risk for mental health and substance use disorders (SUD) that strongly predict antiretroviral treatment (ART) non-adherence in adults. Few studies of perinatally HIV-infected (PHIV+) youth have examined the relationships of psychiatric disorders to adherence and viral load (VL), longitudinally. This study utilized a diagnostic measure of psychiatric disorders including SUD to investigate the association of disorder with ART adherence and viremia as PHIV+ youth age.
Methods: We analyzed data from three follow-up interviews (FU2-4, N=179) spanning 2.7 years of a longitudinal study of PHIV+ youth (13-24 years at FU2; 51% female; 67% African-American/Black) in New York City. At FU2 and FU4, six categories of psychiatric disorder (anxiety, behavior, mood, SUD, any disorder, any disorder excluding SUD) were assessed with the Diagnostic Interview Schedule for Children. At each interview, participants reported on missed doses within the past week and 3 VL results +/-90 days from the interview were abstracted from medical charts.
Multiple logistic regression analyzed cross-sectional associations, at FU2 and FU4, between psychiatric disorders and two outcomes: 1)missed doses and 2)most recent VL>1000. Multiple linear regression analyzed the relationship between FU2 psychiatric disorder and proportion of VL tests >1000 across FU2-4. Analyses adjusted for age and sex.
Results: At FU2, 53% of youth had any disorder, 35% missed doses in the past week, and 47% had a VL>1000.
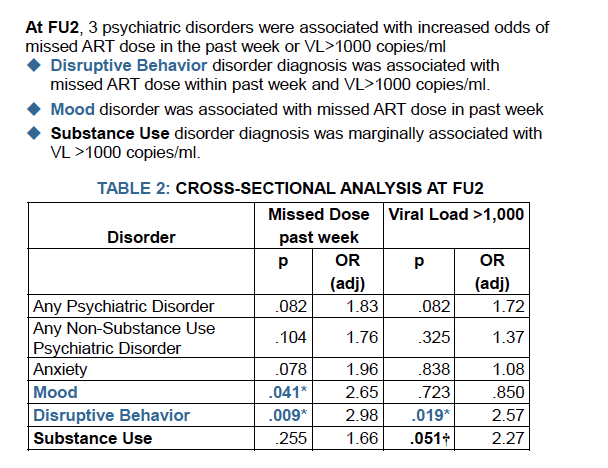
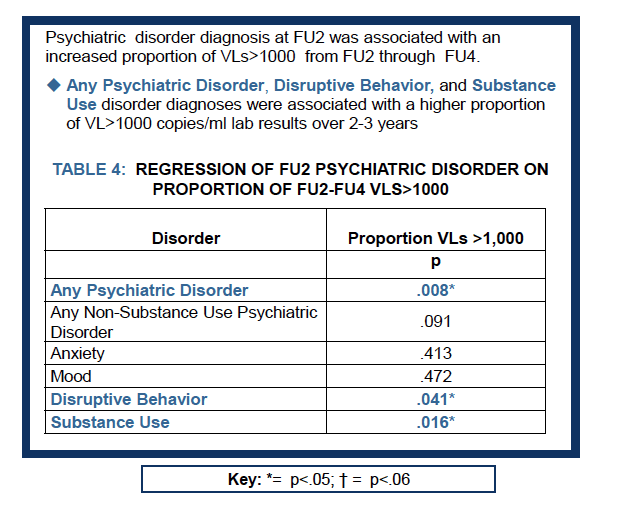
Cross-sectionally, at FU2, behavioral disorder was associated with missed dose (p=.009) and VL>1000 (p=.019) and mood disorder was associated with missed dose (p=.041). At FU4, behavioral disorder was associated with missed dose (p=.009). Behavioral disorder (p=.041), SUD (p=.016), and any disorder (p=.008) at FU2 were significantly associated with higher proportion of VLs >1000 across FU2-4. Other associations were not significant (p>.05).
Conclusions: This is the first study to identify that adolescent psychiatric diagnoses were concurrently associated with poor adherence and prospectively associated with viremia over time. Psychiatric disorders in adolescence may predict viremia over the next 2-3 years. Assessment and treatment of psychiatric and substance abuse problems may be critical to improving adherence and preventing poor health outcomes during this vulnerable stage.


|
| |
|
 |
 |
|
|