 |
 |
 |
| |
Incidence and correlates of STIs among black men who
have sex with men participating in a US PrEP study
|
| |
| |
STI Rates Similar in US Black MSM Who Accept or Decline PrEP
21st International AIDS Conference (AIDS 2016), July 18-22, 2016, Durban, South Africa
Mark Mascolini
Black men who have sex with men (MSM) who opted to start preexposure prophylaxis (PrEP) in a three-city US study had sexually transmitted infection (STI) rates similar to MSM who declined PrEP [1]. Being younger than 25 quadrupled odds of having an STI at screening for the study. STI rates were lower in this MSM study than in other recent studies of MSM.
Young black MSM account for the largest proportion of new HIV infections in the United States. HIV Prevention Trials Network (HPTN) researchers who conducted this study noted that the number of new HIV diagnoses in US black MSM 13 to 24 years old jumped 87% from 2005 to 2014. Young black MSM are prime PrEP candidates. HPTN 073 explored the feasibility, acceptability, and safety of PrEP in this group.
Incidence of STIs among MSM has ranged from 28% to 57% in recent PrEP studies in the US [2,3], France [4], and Britain [5], the HPTN team observed. A recent meta-analysis determined that, compared with MSM not using PrEP, those on PrEP had an 11.2-fold higher chance of getting chlamydia, a 25.3-fold higher chance of getting gonorrhea, and a 44.6-fold higher chance of getting syphilis [6]. The HPTN investigators planned this analysis to learn more about STI acquisition in young black MSM who use PrEP.
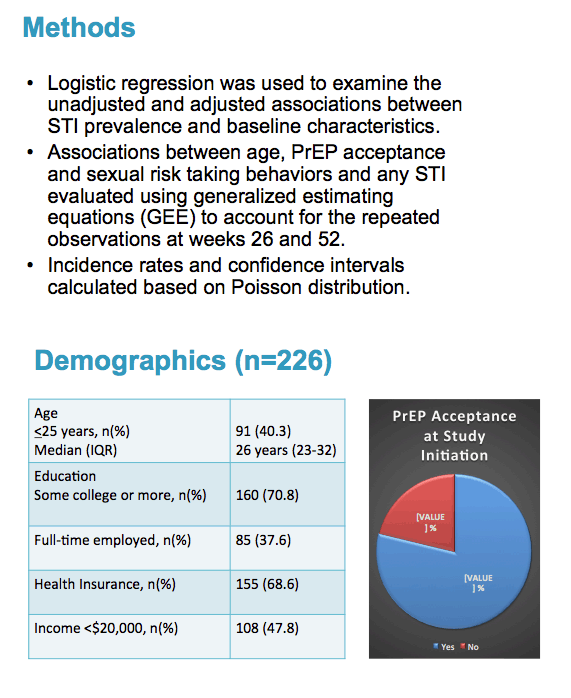
HPTN 073 enrolled 226 HIV-negative black MSM from August 2013 to September 2014 in three cities: Los Angeles, Washington, DC, and Chapel Hill, NC. All men received intensive risk-reduction counseling and were offered daily PrEP with tenofovir/emtricitabine. Follow-up over 12 months included visits at weeks 26 and 52 for gonorrhea, chlamydia, and syphilis testing.
Median age of the study group stood at 26 years (interquartile range [IQR] 23 to 32), and 91 men (40.3%) were 25 or younger. High proportions of men had at least some college education (70.8%) and health insurance (68.6%). Only 37.6% of participants had full-time employment, and 47.8% had an annual income below $20,000. More than three quarters of men (78.8%) accepted PrEP when they entered the study.
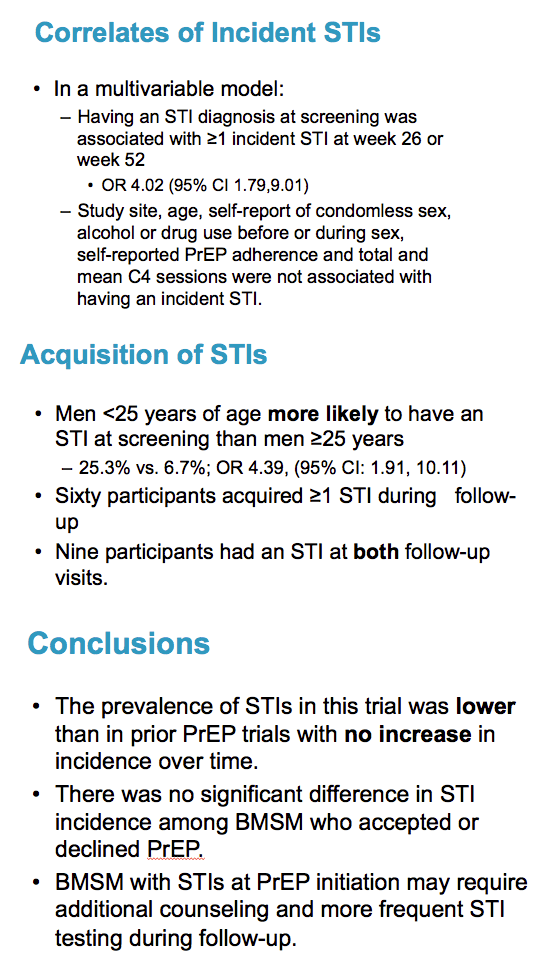
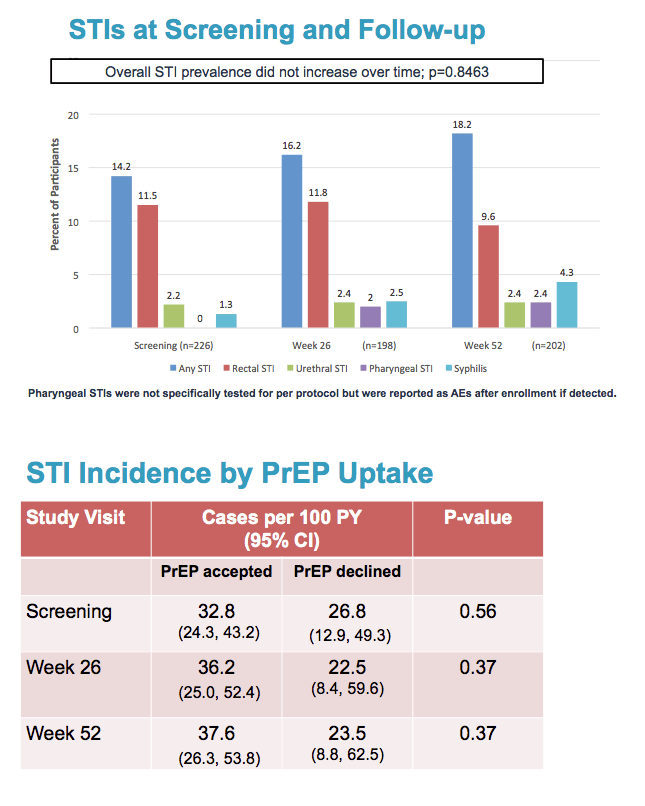
STI prevalence stood at 14.2% at the screening visit, lower than in other recent studies of MSM [2-5]. That rate did not change substantially at week 26 (16.2%) or week 52 (18.2%) (P = 0.85). Rectal STIs accounted for the largest proportion of infections at all three visits (11.5%, 11.8%, and 9.6%). At the screening visit, men younger than 25 had a higher STI prevalence than older men (25.3% versus 6.7%), and those rates translated into 4 times higher odds of an STI in younger men (odds ratio [OR] 4.39, 95% confidence interval [CI] 1.91 to 10.11).
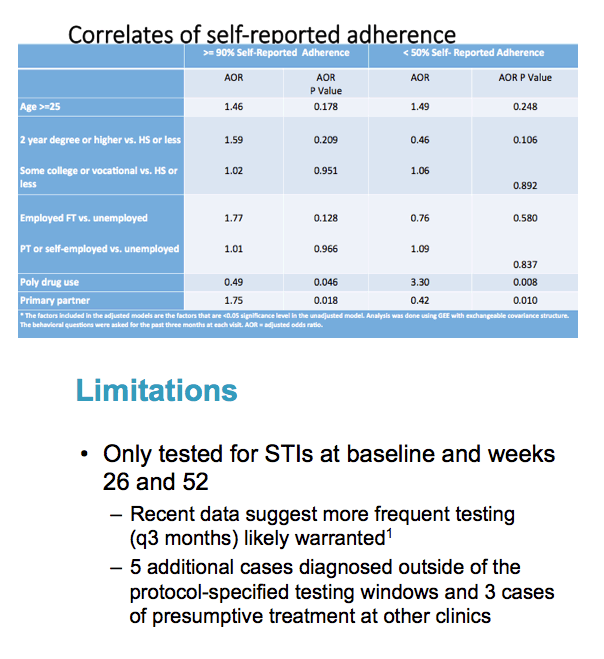
STI incidence--the new infection rate--did not differ significantly between men who accepted PrEP and those who did not at the screening visit (32.8 versus 26.8 cases per 100 person-years, P = 0.56), week 26 (36.2 versus 22.5 per 100 person-years, P = 0.37), or at week 52 (37.6 versus 23.5 per 100 person-years, P = 0.37). Sixty men (26.5%) acquired an STI during follow-up, and 9 men (4%) had an STI at both follow-up visits. These numbers do not reflect 5 other new STIs diagnosed outside the protocol-specified testing windows or 3 new STIs apparently treated at other clinics.
Men with an STI at the screening visit were more likely to pick up another STI during follow-up. Multivariable analysis determined that having an STI at the screening visit quadrupled the odds of acquiring one or more new STIs at week 26 or 52 (OR 4.02, 95% CI 1.79 to 9.01). Factors that did not predict picking up a new STI were age, self-reported condomless sex, alcohol or drug use before or during sex, self-reported PrEP adherence, and study site.
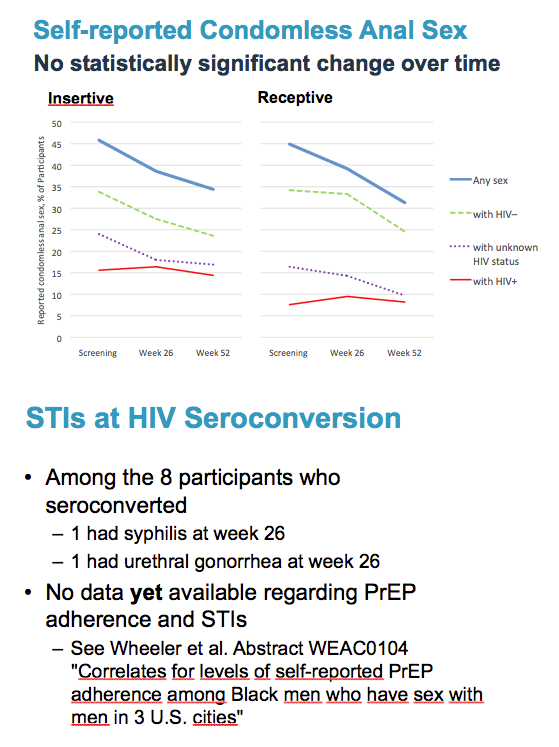
From the screening visit through weeks 26 and 52, the self-reported rate of condomless receptive anal intercourse fell from about 45% of men to almost 30%. That decline reflected drops in condom-free receptive anal sex with HIV-negative partners (about 35% to about 25% of men) and with a partner of unknown HIV status (about 15% to 10% of men). Fewer than 10% of men reported condomless receptive anal sex with an HIV-positive partner at any of the three study visits.
Eight men became infected with HIV during the study. One of them had syphilis at week 26 and 1 had urethral gonorrhea at week 26.
The researchers concluded that STI prevalence in these young black MSM was lower than in MSM enrolled in other recent PrEP studies. And the new STI rate did not differ substantially between men who accepted or declined PrEP. The investigators suggested that black MSM who have an STI when they start PrEP "may require additional counseling and more frequent STI testing during follow-up."
References
1. Hightow-Weidman L, Magnus M, Beauchamp G, et al. Incidence and correlates of STIs among black men who have sex with men participating in a US PrEP study. 21st International AIDS Conference (AIDS 2016). July 18-22, 2016. Durban, South Africa. Abstract THAC0105LB.
2. Volk JE, Marcus JL, Phengrasamy T, et al. No new HIV infections with increasing use of HIV preexposure prophylaxis in a clinical practice setting. Clin Infect Dis. 2015;61:1601-1603.
3. Liu AY, Cohen SE, Vittinghoff E, et al. Preexposure prophylaxis for HIV infection integrated with municipal- and community-based sexual health services. JAMA Intern Med. 2016;176:75-84.
4. Molina JM, Capitant C, Spire B, et al. On-demand preexposure prophylaxis in men at high risk for HIV-1 infection. N Engl J Med. 2015;373:2237-2246.
5. McCormack S, Dunn DT, Desai M, et al. Pre-exposure prophylaxis to prevent the acquisition of HIV-1 infection (PROUD): effectiveness results from the pilot phase of a pragmatic open-label randomised trial. Lancet. 2016;387:53-60.
6. Kojima N, Davey DJ, Klausner JD. Pre-exposure prophylaxis for human immunodeficiency virus and sexually transmitted infection acquisition among men who have sex with men. AIDS. 2016 Jun 14. Epub ahead of print.




|
| |
|
 |
 |
|
|