 |
 |
 |
| |
Past Substance Use Affects CNS Inflammation In HIV
|
| |
| |
Reported by Jules Levin
ID Week Oct 26-30 2016 New Orleans
Li Hui Chen, BS1, Fangyong Li, MPH2, Julia Peterson, BS3, Kevin Robertson, PhD4, Dietmar Fuchs, PhD5, Richard Price, MD3 and Serena Spudich, MD1
(1)Department of Neurology, Yale University School of Medicine, New Haven, CT, (2) Yale Center for Analytical Sciences, Yale School of Public Health, (3)Department of Neurology, University of California San Francisco, San Francisco, CA, (4)University of North Carolina School of Medicine, Chapel Hill, NC, (5)Division of Biological Chemistry, Innsbruck Medical University, Innsbruck, Austria
-----------------------
Low levels of HIV-1 RNA detected in the cerebrospinal fluid after up to 10 years of suppressive therapy are associated with local immune activation.......http://www.natap.org/2014/HIV/080814_02.htm........"In conclusion, in this study, we show that HIV-1 RNA can be detected in 17% CSF samples during suppressive therapy, which is significantly less than the 57% plasma samples that were positive. The concentration of HIV-1 RNA in CSF was also lower than in plasma. We found that HIV-1RNA could be detected in the CSF up to after 10 years of suppressive therapy and is associated with elevated neopterin levels. This suggests that HIV-1 virions continue to drive immune activation and possibly neurological injury during suppressive therapy. The findings of HIV-1 RNA in the CSF during suppressive therapy also indicate that the CNS could be a possible reservoir for HIV-1 during suppressive therapy."
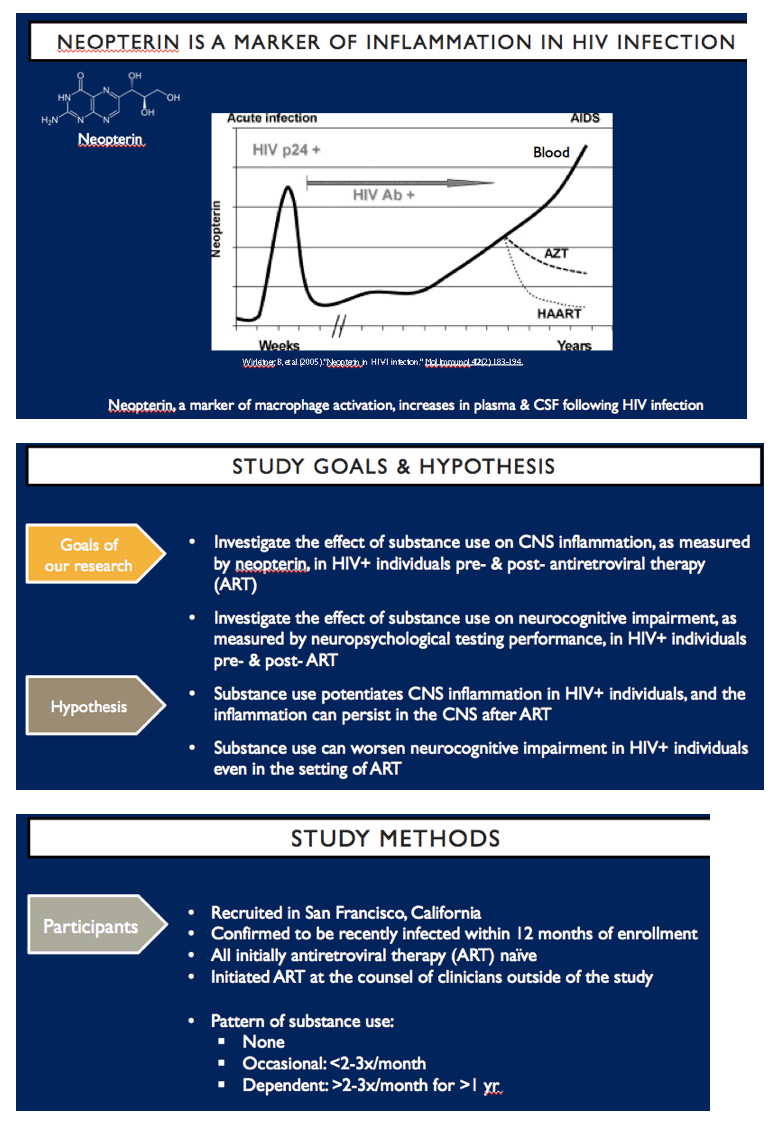
HIV-1 enters the central nervous system (CNS) early during systemic infection and can then be detected in the cerebrospinal fluid (CSF) throughout the subsequent course of untreated infection in most individuals [1-3]. The concentration of HIV-1 RNA in the CSF averages about one-tenth of that in plasma during chronic infection, though the CSF : plasma virus ratio varies among individuals and also may change over time within individual patients [1,2,4,5] related to both the stage of systemic infection and the origins of the CSF virus [2,6]. Through the course of infection, HIV-1 is accompanied by local inflammation and immune activation that is reflected in CSF lymphocytic pleocytosis and elevated concentrations of a number of CSF inflammatory biomarkers, including neopterin (a marker for macrophage activation), and chemokines CCL2 and CXCL10 [5,7].
--------------------

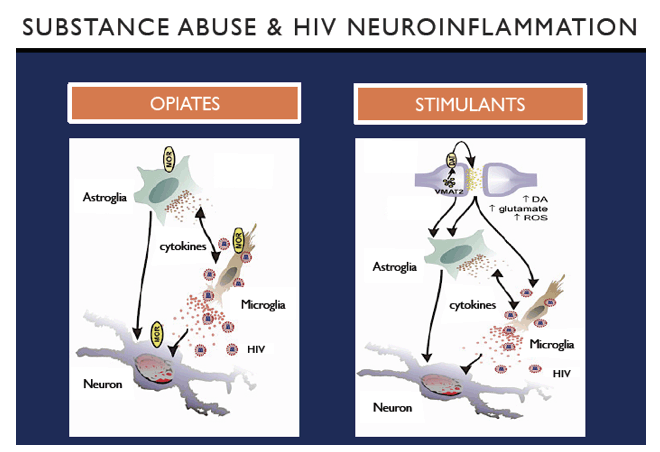
Adapted from Journal of Neurochemistry
Volume 100, Issue 3, pages 567-586, 5 OCT 2006 DOI: 10.1111/j.1471-4159.2006.04227.x
http://onlinelibrary.wiley.com/doi/10.1111/j.1471-4159.2006.04227.x/full#f1
Program Abstract
Background:
HIV infection is commonly associated with substance use. Although previous research has shown that drugs of abuse can alter blood brain barrier function, the effect of substance use on central nervous system (CNS) inflammation is unknown in HIV+ individuals. We examined the role of past drug use in neuroinflammation in HIV.
Methods:
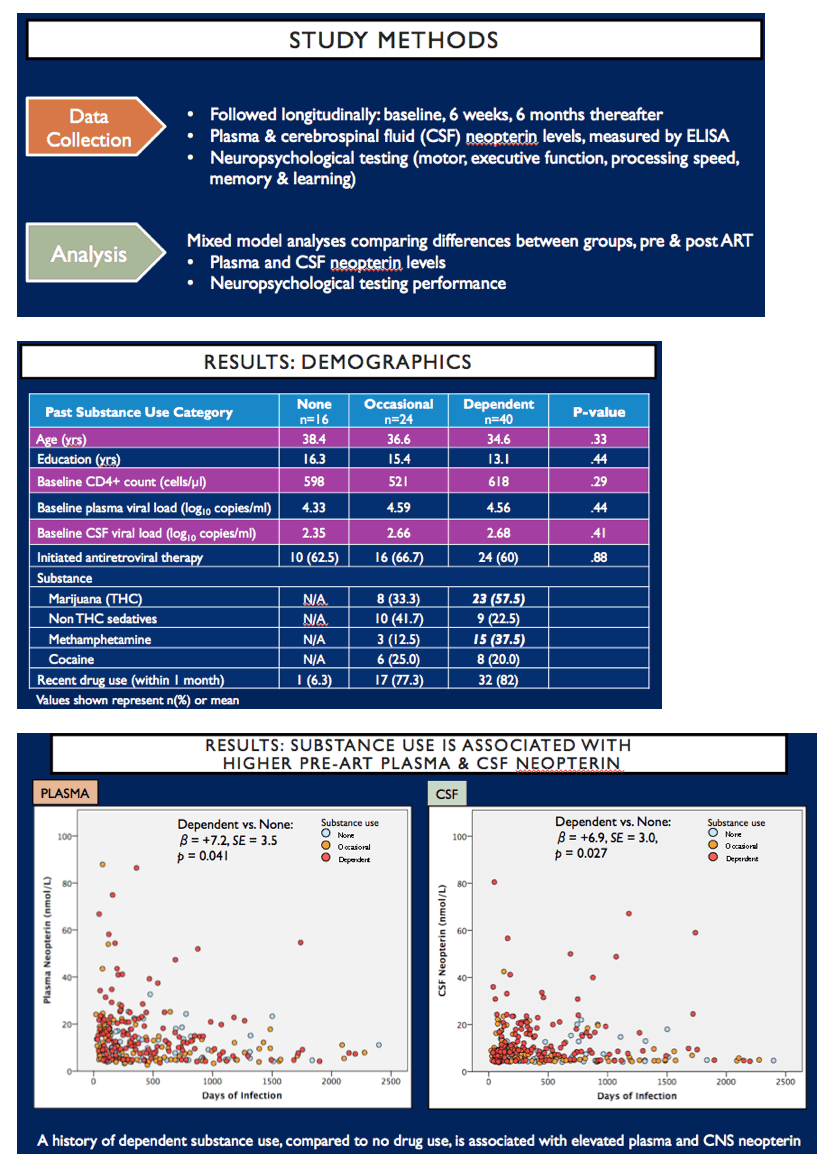
Participants with variable substance use history (defined as none, occasional, or dependent) were recruited into a CNS early HIV infection study. All participants were enrolled when antiretroviral therapy (ART)-naïve, and initiated ART during follow up outside of the study. Cerebrospinal fluid (CSF) and neuropsychological testing data were collected from participants at baseline, 6 weeks, and every 6 months thereafter for up to four years. Mixed model analyses were conducted to compare CSF and plasma neopterin, a marker of macrophage activation, and neuropsychological testing performance pre-and post-ART between groups with different past drug use.
Results:
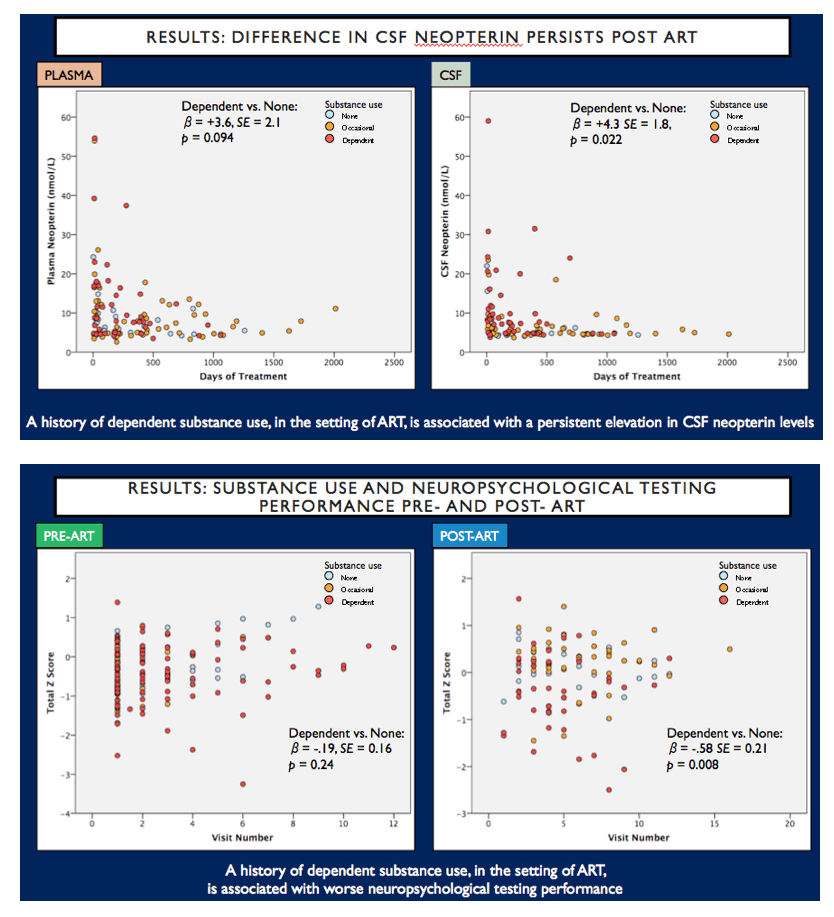
A total of 80 male participants (no past drug use: n=16, occasional past drug use: n=24, dependent past drug use: n= 40) were enrolled and followed longitudinally. No differences in age, plasma and CSF HIV viral load, or blood and CSF WBC count were observed between groups at baseline. Mixed model analyses revealed that pre-ART, plasma and CSF neopterin were elevated in the dependent past drug use group compared to no past drug use group (plasma: β= +7.2, SE = 3.5, p = 0.041; CSF: β= +6.4, SE = 3.0, p = 0.039). The difference in neopterin levels was attenuated post-ART in plasma (β=+3.5, SE = 2.1, p = .105), but persisted in the CSF (β= +7.2, SE = 3.5, p = 0.04). Although no difference was observed in neuropsychological testing performance pre-ART (β= -0.19, SE =.16, p =0.25), dependent past drug use group had reduced improvement in testing scores post-ART compared to the no past drug use group (β= -0.60, SE =.22, p <0.01).
Conclusion:
We observed elevations in plasma and CSF inflammation and sustained abnormal neuropsychological testing performance in HIV+ participants with a history of dependent drug use as compared to no drug use. Differences in the CNS persisted after ART. Drug use history should be actively considered in interpretation of HIV-related CNS research.
|
| |
|
 |
 |
|
|