 |
 |
 |
| |
Adherence to Recommendations from Comprehensive Geriatric Assessment in an HIV+ Population
|
| |
| |
Low Provider and Patient Adherence to Recommendations in HIV Aging Clinic
8th International Workshop on HIV and Aging, October 2-3, 2017, New York
Mark Mascolini
Only about one third of providers and patients evaluated in a New York City HIV aging clinic followed through on geriatrician recommendations within 6 months [1]. Adherence to these recommendations, derived from geriatrician-patient consultations, proved similarly low in providers and patients.
The HIV clinic at Weill Cornell/New York Presbyterian set up an HIV aging program in 2015 and each week offers geriatric consultations upon provider referral. At these visits a geriatrician performs a Comprehensive Geriatric Assessment (CGA), a diagnostic process aiming to assess medical, psychological, and functional capabilities of elderly patients to establish an integrated treatment plan.
The New York team reviewed assessments of all HIV patients 50 or older with a CGA from June 2013 to June 2017. The researchers hoped to answer several questions, including what recommendations geriatricians derive from CGA and how well providers and patients follow through on that advice. They defined adherence as fulfilling recommendations within 6 months of the CGA visit. Recommendations could be directed at providers or patients.
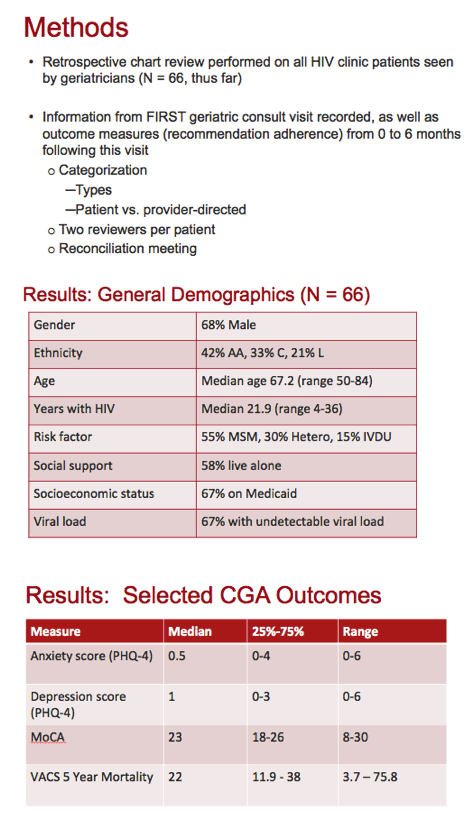
This retrospective chart review involved 66 patients so far, 68% of them men, 42% black, 33% white, and 21% Hispanic. The group had a median age of 67.2 years (range 50 to 84) and had HIV infection for a median of 21.9 years (range 4 to 36). While 55% of participants acquired HIV during sex between men, 30% picked up HIV heterosexually and 15% while injecting drugs. Two thirds had an undetectable viral load, two thirds used Medicaid, and 58% lived alone.
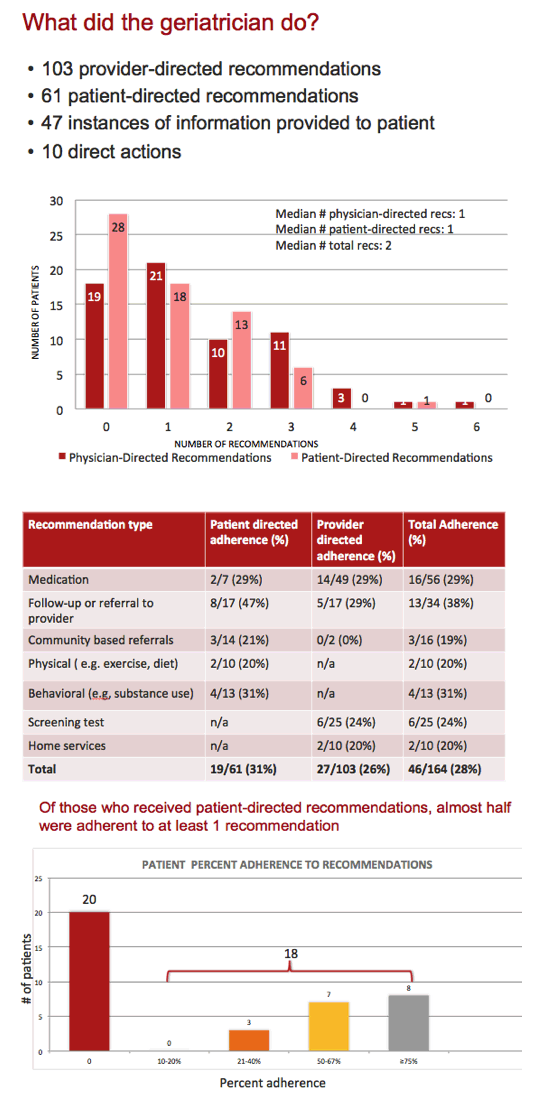
With these 66 people, consulting geriatricians made 103 provider-directed recommendations and 61 patient-directed recommendations; they provided patients information 47 times and recommended 10 direct actions. For each patient median numbers of provider and patient recommendations were 1 and 1 for a median of 2 total recommendations per patient.
Provider-directed recommendations usually involved medications (29%), follow-up or referral (29%), and screening tests (24%). Patient-directed recommendations most often involved follow-up or referral (47%), behavioral issues such as substance use (31%), and medications (29%). Adherence to both provider- and patient-directed recommendations reached only about 30% for each. But almost half of patients followed through on at least 1 recommendation. Neither patient characteristics nor CGA metrics predicted adherence.
The researchers plan to expand the analysis to include at least 75 patients. They hope that ongoing study will let them determine whether CGA improves patient outcomes over the long term.
Reference
1. Bitas C, Jones S, Singh HK, Ramirez M, Siegler E, Glesby M. Adherence to recommendations from comprehensive geriatric assessment in an HIV+ population. 8th International Workshop on HIV and Aging. October 2-3, 2017. New York. Abstract 9.
--------------------

1 Albrand G, Terret C, Mignotte H, Gaujard S, Droz JP, Courpron P; Geriatric Oncology Program.. Early breast cancer in elderly women: The value of Comprehensive Geriatric Assessment (CGA). J Clin Oncol. 2005 Jun;23(16_suppl):8172.
2 Caillet P, Laurent M, Bastuji-Garin S, et al. Optimal management of elderly cancer patients: usefulness of the Comprehensive Geriatric Assessment. Clinical Interventions in Aging. 2014;9:1645-1660.
3 Ellis G, Whitehead MA, O'Neill D, Langhorne P, Robinson D. Comprehensive geriatric assessment for older adults admitted to hospital. Cochrane Database Syst Rev. 2011 Jul 6;(7):CD006211. doi: 10.1002/14651858.CD006211.pub2. Review. PubMed PMID: 21735403; PubMed Central PMCID: PMC4164377

4 Reuben DB, Maly RC, Hirsch SH, Frank JC, Oakes AM, Siu AL, Hays RD. Physician implementation of and patient adherence to recommendations from comprehensive geriatric assessment. Am J Med. 1996 Apr;100(4):444-51. PubMed PMID: 8610732.
-------------------------
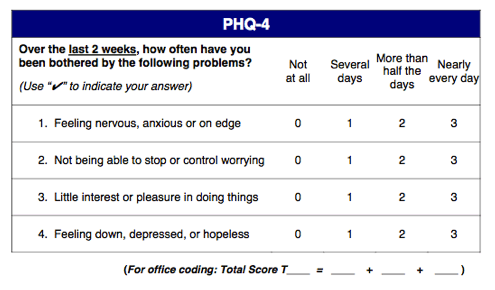
from Jules - What is PHQ-4?
Kroenke, K., Spitzer, R. L., Williams, J. B. W., Lowe, B. (2009). An ultra-brief screening scale for anxiety and depression: the PHQ-4 Psychosomatics, 50, 613-621.
Primary use / Purpose:
The 'Patient Health Questionnaire-4' (PHQ-4) is a 4 item inventory rated on a 4 point Likert-type scale. Its items are drawn from the first two items of the 'Generalized Anxiety Disorder-7 scale' (GAD-7) and the 'Patient Health Questionnaire-8' (PHQ-8). Its purpose is to allow for very brief and accurate measurement of depression and anxiety.
Background:
Anxiety and depression are the two most prevalent illnesses among patients, and in the general population. Because these two mood disorders are frequently co-morbid they can have especially problematic outcomes. The nature of these mood disorders can make filling out long questionnaires difficult if patients are suffering from fatigue or loss of concentration. Furthermore, time is at a premium in any clinical practice. Therefore, the 'Patient Health Questionnaire-4' (PHQ-4) was developed and validated by Kroenke, Spitzer, Williams, & Lowe, (2009) in order to address these needs
Psychometrics:
The psychometric propertie of the 'Patient Health Questionnaire-4' (PHQ-4) are discussed in Kroenke, Spitzer, Williams, & Lowe, (2009)
An ultra-brief screening scale for anxiety and depression: the PHQ-4.
Psychosomatics. 2009 Kroenke K1, Spitzer RL, Williams JB, Lowe B.
Abstract
BACKGROUND:
The most common mental disorders in both outpatient settings and the general population are depression and anxiety, which frequently coexist. Both of these disorders are associated with considerable disability.
OBJECTIVE:
When the disorders co-occur, the disability is even greater. Authors sought to test an ultra-brief screening tool for both.
METHOD:
Validated two-item ultra-brief screeners for depression and anxiety were combined to constitute the Patient Health Questionnaire for Depression and Anxiety (the PHQ-4). Data were analyzed from 2,149 patients drawn from 15 primary-care clinics in the United States.
RESULTS:
Factor analysis confirmed two discrete factors (Depression and Anxiety) that explained 84% of the total variance. Increasing PHQ-4 scores were strongly associated with functional impairment, disability days, and healthcare use. Anxiety had a substantial effect on functional status that was independent of depression.
CONCLUSION:
The PHQ-4 is a valid ultra-brief tool for detecting both anxiety and depressive disorders.
--------------------------------
back to slide presentation

|
| |
|
 |
 |
|
|