 |
 |
 |
| |
EPICARDIAL FAT, IMMUNE ACTIVATION, AND CORONARY
PLAQUE AMONG HIV+ AND HIV- WOMEN
|
| |
| |
Reported by Jules Levin
CROI Feb 14-16 Seattle, WA
Suman Srinivasa, MD*, Michael T. Lu, MD*, Kathleen V. Fitch, MSN, Travis R. Hallett, Tricia H. Burdo, PhD, Janet Lo, MD, Sara E. Looby, PhD, Udo Hoffmann, MD, Steven K. Grinspoon, MD, and Markella V. Zanni, MD
Program in Nutritional Metabolism, Massachusetts General Hospital and Harvard Medical School, Boston, MA; Cardiac MR PET CT Program, Massachusetts General Hospital and Harvard Medical School, Boston, MA; Department of Neuroscience, Temple University School of Medicine, Philadelphia, PA
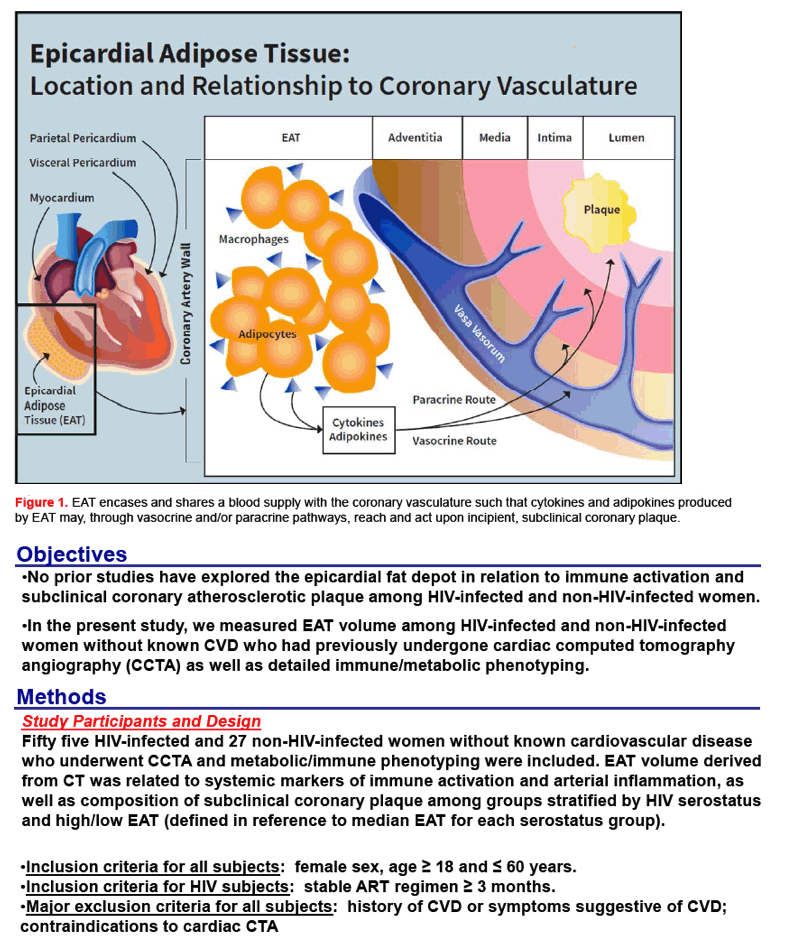
from Jules: HIV+ women without known cardiovascular risk factors, age around 47 for this study, had similar EAT fat [epicardial fat near the heart, see illustration below] as HIV-unifected women and women with more of this type of fat near the heart had higher markers of inflammation & immune activation compared to HIV+ women without this excessive fat as well as HIV-unifected women, and these women with thegreater fat had higher non-calcified artherosclerotic plaque, among HIV+ women EAT was not associated with traditional CVD risk factors but was associated with duration of NRTI use, VAT area [belly fat], commonly referred to as belly fat, lipodystrophy, VAT remained an independent predictor of EAT after controlling for age & NRTI duration. "Previous studies have reported that asymptomatic HIV+ women (vs non-HIV-infected women) have a significantly higherpercentageof non-calified, rupture-prone coronary plaque in relation to increased systemic levels of pro-inflammatory cytokines and immune activation markers….no prior studies have explored the epicardial fat depot 9near the heart] in relation to immune activation and suclinical coronary artherosclerotic plaque among HIV-infected & non-HIV-infected women.



---------------------------------
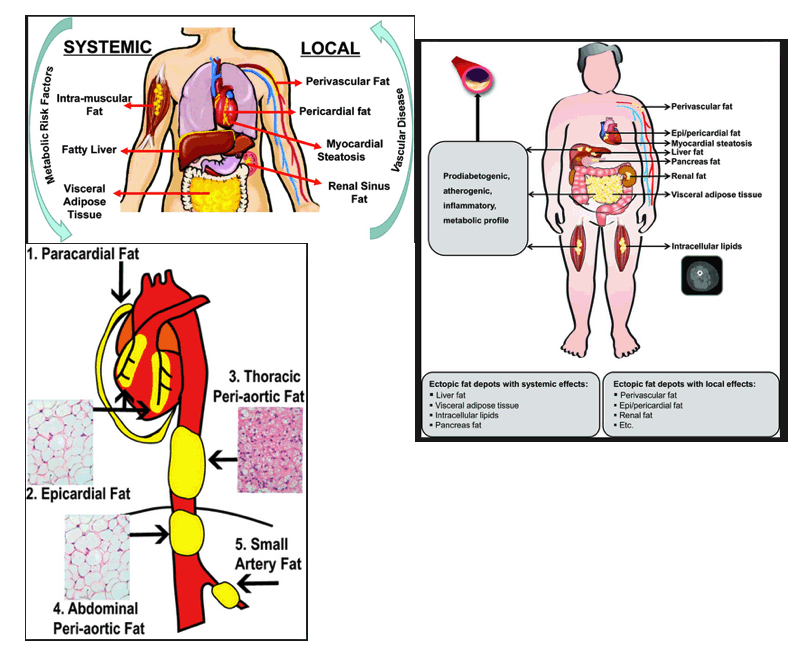
Ectopic and Visceral Fat Deposition inLean and Obese Patients With Type2Diabetes
Abstract
Background Type 2 diabetes (T2D) and obesity are associated with nonalcoholic fatty liver disease, cardiomyopathy, and cardiovascular mortality. Both show stronger links between ectopic and visceral fat deposition, and an increased cardiometabolic risk compared with subcutaneous fat.
Objectives This study investigated whether lean patients (Ln) with T2D exhibit increased ectopic and visceral fat deposition and whether these are linked to cardiac and hepatic changes.
Methods Twenty-seven obese patients (Ob) with T2D, 15 Ln-T2D, and 12 normal-weight control subjects were studied. Subjects underwent cardiac computed tomography, cardiac magnetic resonance imaging (MRI), proton and phosphorusMR spectroscopy, and multiparametric liver MR, including hepatic proton MRS, T1- and T2*-mapping yielding “iron-corrected T1” [cT1].
Results Diabetes, with or without obesity, was associated with increased myocardial triglyceride content (p= 0.01), increased hepatic triglyceride content (p= 0.04), and impaired myocardial energetics (p= 0.04). Although cardiac structural changes, steatosis, and energetics were similar between the T2D groups, epicardial fat (p= 0.04), hepatic triglyceride (p= 0.01), and insulin resistance (p= 0.03) were higher in Ob-T2D. Epicardial fat, hepatic triglyceride, and insulin resistance correlated negatively with systolic strain and diastolic strain rates, which were only significantly impaired in Ob-T2D (p< 0.001 and p= 0.006, respectively). Fibroinflammatory liver disease (elevated cT1) was only evident in Ob-T2D patients. cT1 correlated with hepatic and epicardial fat (p< 0.001 and p= 0.01, respectively).
Conclusions Irrespective of body mass index, diabetes is related to significant abnormalities in cardiac structure, energetics, and cardiac and hepatic steatosis. Obese patients with T2D show a greater propensity for ectopic and visceral fat deposition.
Type 2 diabetes (T2D) and obesity are both associated with nonalcoholic fatty liver disease (NAFLD), cardiomyopathy (1,2), and increased cardiovascular mortality (3,4). The incidence of T2D continues to increase, driven predominantly by the obesity epidemic. Although obesity is likely to be a strong contributor to diabetic cardiomyopathy (5), many patients with diabetic cardiomyopathy have normal body mass index (BMI), suggesting that diabetes and obesity may have different mechanisms by which they mediate cardiovascular change and that diabetic cardiomyopathy may occur in patients with T2D without obesity. Furthermore, evidence suggests that distribution of excess fat is an important determinant of cardiovascular risk, and ectopic and visceral adiposity confer a much higher risk than subcutaneous adiposity (6,7).
Ectopic and visceral fat storage may be linked to insulin resistance, and it is widely known that insulin resistance is the strongest predictor of development of diabetes (8).
Increasing evidence points to a strong association between insulin resistance and nonischemic heart failure (9), although there are differing opinions regarding whether this relationship is of a protective or pathological nature (10–12). Thus, the presence of ectopic and visceral fat deposition in patients with T2D even in the absence of a global increase in total body fat may potentially play a significant role in this association. Assessing body composition is, therefore, likely to be more important in patients with T2D than simple metrics of obesity. Liver fat is considered a key feature of ectopic fat associated with dysfunctional adipose tissue and visceral fat deposition (13), and there is also growing interest in the imaging of epicardial adipose tissue as a proxy measure of visceral fat.
Epicardial adipose tissue, a form of visceral fat, may affect the underlying myocardium by secreting awide range of adipokines (14). Furthermore, excessliver fat has been shown to be accompanied by cardiac structural and functional changes (15). Computed tomography (CT) allows quantification of epicardial fat volume, and proton magnetic resonance spectroscopy (1H-MRS) allows quantification oflipid content in the liver and the heart.
Multiparametric magnetic resonance (MR) of the liver, including 1H-MRS for assessment of steatosis and T1 and T2* mapping (yielding iron corrected T1 [cT1]) (16), allows noninvasive quantification of liver fatand identification of the presence of hepatic fibroinflammatory disease with a high diagnostic accuracy (16).
Myocardial energetic compromise is an important feature of both the diabetic (17) and the nondiabetic obese heart (5). However, changes in cardiac energy metabolism in lean patients with diabetes have not been previously studied. Myocardial phosphocreatine to adenosine triphosphate concentration ratio (PCr/ATP) is a sensitive indicator of the myocardial energy status, and phosphorus magnetic resonance spectroscopy (31P-MRS) allows noninvasive assessment of the PCr/ATP.
-----------------------------------
|
| |
|
 |
 |
|
|