 |
 |
 |
| |
"Switching boosters: are they equal? An analysis of patients
switching from ritonavir to cobicistat in a large London cohort"
|
| |
| |
Download the PDF here
Does Switch From RTV Boost to DRV/COBI Pose Rebound Risk?
16th European AIDS Conference, October 25-27, 2017. Milan
Mark Mascolini
Switching from a ritonavir (r)-boosted agent to darunavir/cobicistat (DRV/c) resulted in "higher than expected rates of detectable viremia" in a moderately large single-center study [1]. Researchers at London's Mortimer Market Centre found a lower (but not significantly lower) rebound rate upon switching to atazanavir/cobicistat (ATV/c).
Clinicians may offer patients taking DRV/r or ATV/r a switch to DRV/c or ATV/c, which come in single-tablet formulations that offer greater convenience and perhaps lower costs. But whether these boosted protease inhibitors (PIs) have the same potency with either booster remains less certain for DRV/c than for ATV/c. A 692-person double-blind, double-dummy trial randomized antiretroviral-naive people to ATV/r or ATV/c, both with emtricitabine and tenofovir disoproxil fumarate [2]. Virologic suppression rates were similar with the two boosters, regardless of whether pretreatment viral load was above or below 100,000 copies.
To address the question of whether switching to DRV/c or ATV/c consistently maintains viral suppression, in April 2017 Mortimer Market investigators identified everyone taking DRV/c or ATV/c in the previous 12 months and whether they switched to the cobicistat-boosted PI from another regimen. Among switchers they noted viral loads before and after the switch. They aimed to determine how many switchers had a detectable viral load after starting DRV/c or ATV/c and which had "clear failure"--defined as consecutive viral loads above 50 copies. People with a transient detectable viral load (a blip) or a clear reason for a detectable viral load (like poor adherence or treatment interruption) were not considered failures, but the researchers cautioned they did not have detailed adherence data.
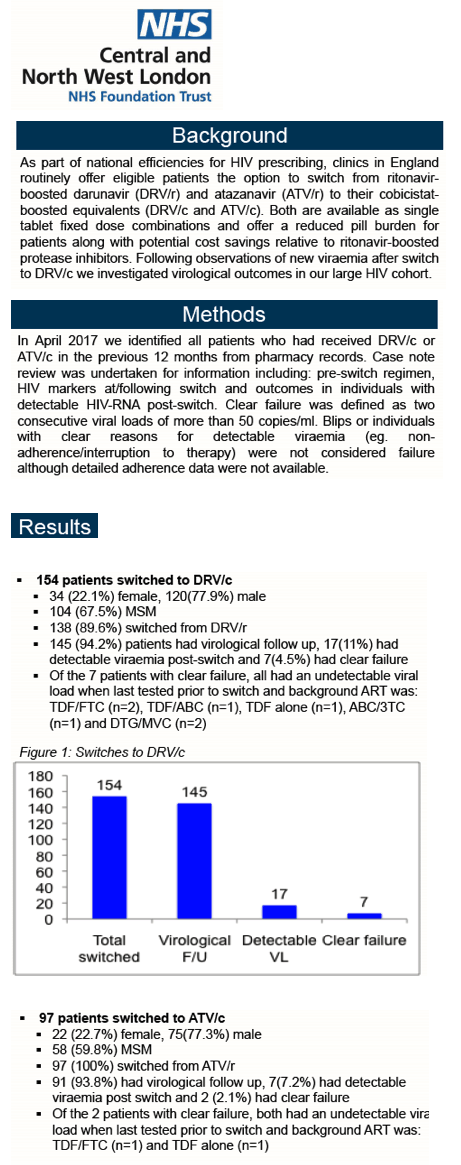
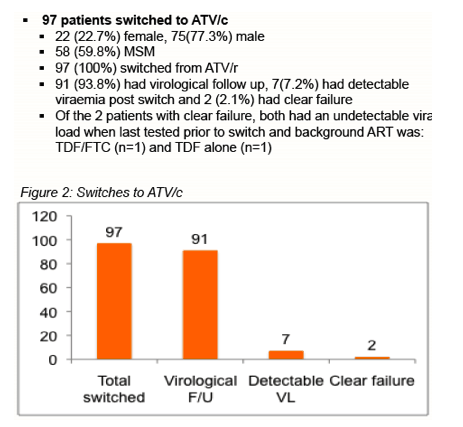
The analysis considered 154 people switching to DRV/c and 97 switching to ATV/c. Respective proportions of men were 78% and 77% and of gay/bisexual men 67.5% and 60%. Of the 154 people starting DRV/c, 138 (90%) switched from DRV/r. Everyone starting ATV/c switched from ATV/r.
Among DRV/c switchers, 145 (94%) had virologic follow-up, of whom 17 (11.7%) had a detectable viral load after starting DRV/c and 7 (4.8%) had clear failure. Among people with clear failure, all had an undetectable viral load when last tested before the switch to DRV/c. Among ATV/c switchers, 91 (94%) had virologic follow-up, of whom 7 (7.7%) had a detectable viral load an 2 (2.2%) had clear failure after the switch. Both people with clear failure had an undetectable viral load when last tested before the switch. The clinic has an overall detectable viral load rate around 1% among people with viral load suppression for 1 year.
The researchers called the viral detectability rate after switching to DRV/c "unexpected," though they noted that rate did not differ significantly from the detectability rate in people switching to ATV/r. They suggested a possible reason for viral detectability after starting DRV/c: Prior research in healthy volunteers charted a faster decay of darunavir levels with DRV/c than DRV/r [3]. In this study darunavir levels lay below the minimum effective concentration 30 hours after DRV/c dosing in 11 of 16 volunteers. The Mortimer Market group hypothesized that "the pharmacokinetic tail for DRV/c versus DRV/r is less forgiving for missed/delayed doses or reduced absorption."
The researchers noted they did not explore resistance data, but clinic guidelines prohibit switching to DRV/c in the face of DRV-associated resistance mutations. They believe their findings call for "further observation and reporting of virological outcomes" after a switch to DRV/c, and they advise clinicians to consider changing antiretrovirals if low-level viremia appears in people who have switched to DRV/c.
References
1. Nugent D, Hedley L, Bradley S, et al. Switching boosters, are they equal? An analysis of patients switching from ritonavir to cobicistat in a large London cohort. 16th European AIDS Conference. October 25-27, 2017. Milan. Abstract PE9/64.
2. Gallant JE, Koenig E, Andrade-Villanueva J, et al. Cobicistat versus ritonavir as a pharmacoenhancer of atazanavir plus emtricitabine/tenofovir disoproxil fumarate in treatment-naive HIV type 1-infected patients: week 48 results. J Infect Dis. 2013;208:32-329.
3. Elliot ER, Amara A, Pagani N, et al. Once-daily atazanavir/cobicistat and darunavir/cobicistat exposure over 72 h post-dose in plasma, urine and saliva: contribution to drug pharmacokinetic knowledge. J Antimicrob Chemother. 2017;72:2035-2041.

pdf of this Elliot publication attached
Download the PDF here
References: 1. Elliot et al. Once-daily atazanavir/cobicistat and darunavir/cobicistat exposure over 72 h post-dose in plasma, urine and saliva: contribution to drug pharmacokinetic knowledge. J Antimicrob Chemother. 2017; 72: 2035-41
|
| |
|
 |
 |
|
|