| |
County-Level Vulnerability Assessment for Rapid Dissemination of HIV or HCV Infections Among Persons Who Inject Drugs, United States
| | | | |
Download the PDF here
"Prompted by a recent outbreak of HIV infection among PWID in a rural community, we developed a method to identify other communities vulnerable to rapid dissemination of IDU-associated HIV, if introduced, and new or continuing high numbers of HCV infections. Identification of a county as vulnerable to this type of outbreak does not mean an outbreak is eminent; rather jurisdictions identified as at-risk might use potentially informative local data that were not available nationally and take action as recommended in the April 2015 CDC Health Alert Network advisory.34 Expanding epidemics of prescription opioid abuse and unsterile IDU and shifting demography and geography, heralded by national changes in patterns of acute HCV infection, are critical driving forces of vulnerability. To reduce vulnerability, targeted interventions in accordance with efforts to prevent and treat substance use disorder and to reduce risk of infectious complications of IDU are warranted."
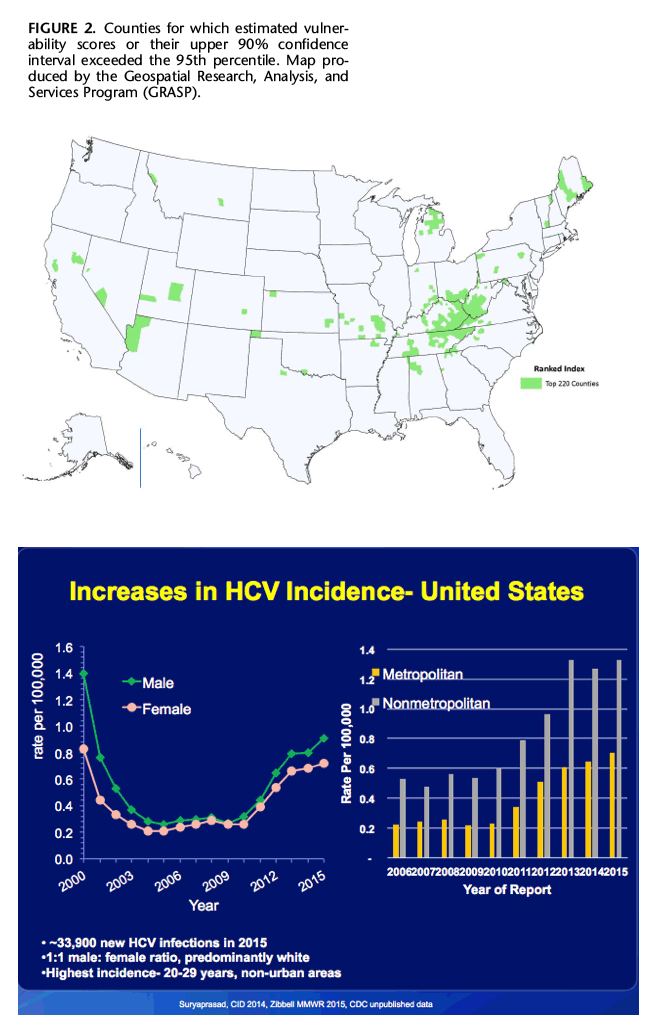
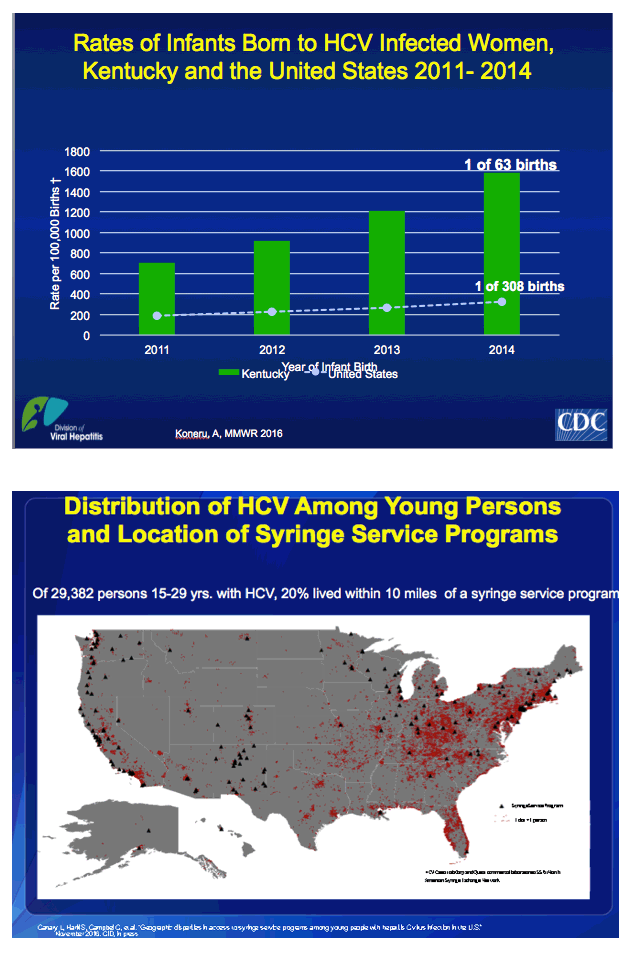
Increases in HCV among young persons, including women of childbearing age, is leading to increases in mother-to-child transmission nationally. Again, some states like Kentucky, which has one of the highest rates of new HCV cases in the country, are more affected than others. In that state during 2014, one of every 67 infants born was born to an HCV-infected mother.
The proportion of infants born to HCV-infected women nationally increased 68%, from one in 536 (0.19%) to one in 308 (0.32%).
In KY, the proportion of infants born to HCV-infected women increased 124%, from one in 142 (0.71%) to one in 63 (1.59%)
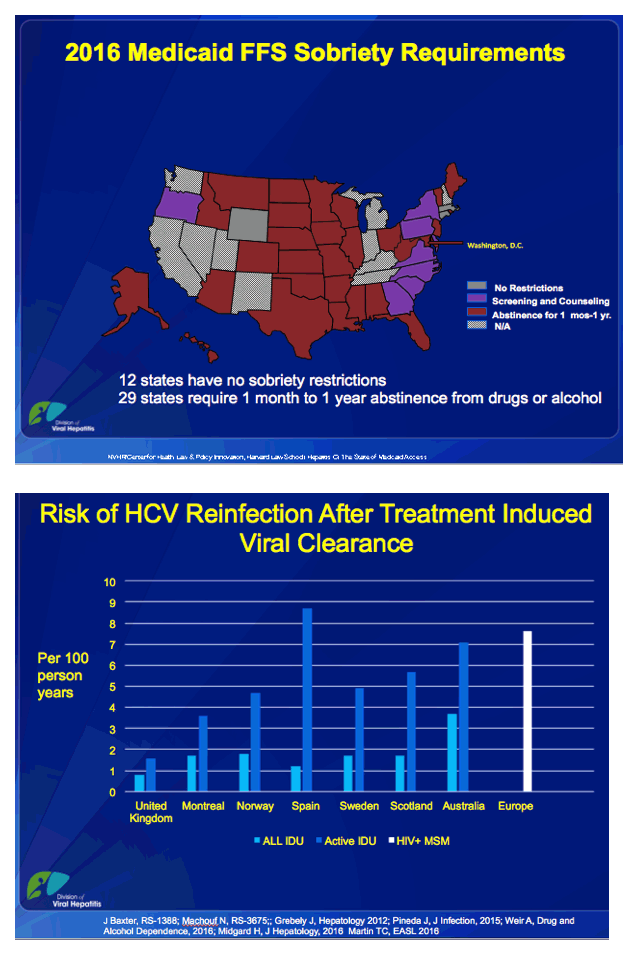
------------------------
County-Level Vulnerability Assessment for Rapid Dissemination of HIV or HCV Infections Among Persons Who Inject Drugs, United States
JAIDS Nov 2016 - Van Handel, Michelle M. MPH; Rose, Charles E. PhD; Hallisey, Elaine J. MA; Kolling, Jessica L. MPH; Zibbell, Jon E. PhD; Lewis, Brian BS; Bohm, Michele K. MPH; Jones, Christopher M. PharmD, MPH; Flanagan, Barry E. PhD; Siddiqi, Azfar-E-Alam MD, PhD; Iqbal, Kashif MPH; Dent, Andrew L. MA, MBA; Mermin, Jonathan H. MD, MPH; McCray, Eugene MD; Ward, John W. MD; Brooks, John T. MD
Objective: A recent HIV outbreak in a rural network of persons who inject drugs (PWID) underscored the intersection of the expanding epidemics of opioid abuse, unsterile injection drug use (IDU), and associated increases in hepatitis C virus (HCV) infections.
We sought to identify US communities potentially vulnerable to rapid spread of HIV, if introduced, and new or continuing high rates of HCV infections among PWID.
Design: We conducted a multistep analysis to identify indicator variables highly associated with IDU. We then used these indicator values to calculate vulnerability scores for each county to identify which were most vulnerable.
Methods: We used confirmed cases of acute HCV infection reported to the National Notifiable Disease Surveillance System, 2012-2013, as a proxy outcome for IDU, and 15 county-level indicators available nationally in Poisson regression models to identify indicators associated with higher county acute HCV infection rates. Using these indicators, we calculated composite index scores to rank each county's vulnerability.
Results: A parsimonious set of 6 indicators were associated with acute HCV infection rates (proxy for IDU): drug-overdose deaths, prescription opioid sales, per capita income, white, non-Hispanic race/ethnicity, unemployment, and buprenorphine prescribing potential by waiver. Based on these indicators, we identified 220 counties in 26 states within the 95th percentile of most vulnerable.
Conclusions: Our analysis highlights US counties potentially vulnerable to HIV and HCV infections among PWID in the context of the national opioid epidemic. State and local health departments will need to further explore vulnerability and target interventions to prevent transmission.
INTRODUCTION
During the past decade, the US opioid epidemic has fueled an increase in illicit, unsterile injection drug use (IDU) and new hepatitis C virus (HCV) infections, especially within nonurban communities.1-6 For the first time, late in 2014, injection of prescription opioids was linked to an outbreak of HIV infections in a rural US community (Austin in Scott County, Indiana). This event raised concerns about the vulnerability of similar communities to the rapid spread of HIV infection if introduced into a network of persons who inject drugs (PWID). The socioeconomic context within which this outbreak occurred was not unique: unemployment and poverty in the county exceeded national levels,7 educational attainment was low,7 and life expectancy was poor.8 During November 2014-October 2015, 181 persons were diagnosed with HIV infection, of whom 92% were coinfected with HCV.9 This county of approximately 24,000 persons reported fewer than 5 new HIV infections in the preceding 10 years.9,10
Rapid recognition of the outbreak and implementation of intensive control efforts likely reduced new HIV and HCV infections and limited their geographic spread.9 Identifying jurisdictions particularly vulnerable to a similar outbreak can increase awareness of current vulnerability and guide public health efforts to detect and prevent this type of event. To this end, we conducted a multistep analysis (Fig. 1) to identify which set of indicators (independent variables) is highly associated with unsterile IDU, then used each US county's values for these indicators to calculate a vulnerability score for each county, and finally identified which states and specific counties are most vulnerable.
DISCUSSION
We have developed a method to identify US counties potentially vulnerable to rapid spread of HIV, if introduced, and new or continuing high numbers of HCV infections among PWID. The method employed a proxy measure for county-level unsterile IDU (ie, acute HCV infection). Ecological-level measures have been used previously to create CDC's Social Vulnerability Index. That index was designed to identify socially vulnerable populations that are more likely to be adversely affected during disaster events (eg, elderly, people living in poverty).18 It assesses overall census tract vulnerability on the basis of 14 census variables and calculates an overall percentile rank of social vulnerability for each area.18 Our method builds on this approach by first identifying the specific indicators associated with HCV (proxy for unsterile IDU). We then calculated an index score to rank counties and account for the relative contribution of each indicator to identify the most vulnerable communities. The evolution of IDU in the United States is dynamic and this method can be applied periodically to account for those changes. Improved reporting of acute HCV infections to NNDSS and the identified indicators will increase the accuracy of the method for identifying vulnerable counties over time.
Deaths from drug overdose have grown exponentially in the past decade, surpassing motor vehicle traffic accidents as the leading cause of unintentional injury-related death in the United States.19 Overdose death rates because of prescription opioids increased nearly 4-fold from 2000 to 2013.20 Prescription opioids are the most commonly abused prescription drug, and an estimated 10%-20% of people who abuse prescription opioids escalate to injection of prescription opioids or heroin,21-23 creating opportunity for IDU-associated outbreaks of HIV or HCV infection.24,25Rates of acute HCV infection have increased steadily nationwide from 2006 to 2012, most notably east of the Mississippi River and particularly among states in central Appalachia.4 The potential for an HIV outbreak within an opioid-injecting population was realized in Scott County, Indiana,26 which ranked 32nd among the top 220 counties in our vulnerability analysis.
The demography of PWID and persons diagnosed with acute HCV infection in the United States has changed substantially. From 1999 to 2002, HCV diagnoses in the United States were greater among men, non-Hispanic blacks, and persons aged 40-49 years.27 Persons diagnosed with acute HCV infection now are equally likely to be male as female are predominantly of white, non-Hispanic race/ethnicity, and younger age.2,4,13,28,29 Our finding that white, non-Hispanic race/ethnicity was significantly associated with county-level acute HCV infection reflects these changes.
The counties identified in our analysis were overwhelmingly rural. Since 2006, rates of acute HCV infection have increased faster in rural than in urban areas4 consistent with introduction and spread of this infection into populations made newly vulnerable by the expansion of IDU in rural America. The outbreak in Scott County, IN was notable for the absence or minimal availability of harm-reduction strategies to prevent IDU-associated HIV and HCV infections, such as addiction treatment and rehabilitation, medication-assisted therapy (MAT), and syringe service programs (SSPs).9This outbreak illustrated the need for harm-reduction strategies suited to the rural context. Our analysis can help identify those rural areas at highest risk of infectious complications from IDU where interventions can be prioritized. Unemployment and income were also significantly associated with risk for acute HCV infection. It has been hypothesized that financial stressors increase vulnerability to drug use, so that young adults in economically deprived areas may accumulate more risk factors for drug use and be more likely to establish drug dependencies at a younger age than persons in more economically privileged areas.30 Since the Great US Recession of 2007-2009, rural areas have experienced persistent and greater unemployment and poverty than urban areas.31
Buprenorphine is approved for MAT of opioid-use disorder. The indicator "buprenorphine prescribing potential by waiver per 10,000 population" represents the potential availability of this form of MAT to the population of a county, reflecting the capacity to treat in response to demand for services and not the actual rate of people receiving treatment.32 In 2011, 43% of US counties had no buprenorphine-waivered physicians,32 indicating that capacity to prescribe MAT likely lags behind the need. It is important that these indicators are not interpreted as causally associated, rather are understood as indicators of potential vulnerability for this type of outbreak.
The risk for introduction and spread of HIV infection into a vulnerable community of persons will vary according to the estimated HIV proximity of the community and the community's IDU practices. We found that the estimated HIV proximity was lower than the national average for nearly all of the 220 counties identified as most vulnerable. Although we could not measure IDU practices systematically for each US county, it is important to consider the estimated HIV proximity in the context of local IDU practices. For example, Scott County, IN was in the second highest estimated HIV proximity group relative to the 220 vulnerable counties and lower than the national average, but the injection practices in Scott County, IN were notable for the high frequency of injections and combined with the relatively large and dense network of PWID9 in the absence of effective strategies to reduce IDU-associated infection leaving the community vulnerable to this type of outbreak.
All health officials can review these results along with the most recent sources of data on HIV and acute HCV diagnoses available to them. Additional local insight may be gained by examining data sources about other factors associated with IDU that were not available for inclusion in our analysis. There are a number of indicators we would like to consider that are not available nationwide but may provide substantial local insight on vulnerability to rapid spread of HIV infections associated with unsterile IDU. These data include emergency department and hospital admissions for drug overdose or intoxication; arrests for drug possession or sales; and opioid prescribing patterns from state prescription drug monitoring programs and data on local injection practices and availability of effective strategies to reduce IDU-associated infection (eg, drug type injected, injection frequency).33 CDC is preparing additional advice to assist health departments, so they can assess whether their jurisdiction is experiencing or at risk of new HIV and HCV infections potentially related to IDU (personal communication).
This analysis is subject to limitations. First, we excluded potential indicators, as noted above, because we established strict inclusion criteria to assess vulnerability for each county. Second, this analysis was intended to identify areas currently vulnerable; however, some of the data were ≥3 years old. Third, all ecologic analyses based on reported cases of notifiable disease and deaths are subject to potential underreporting (eg, HCV data) or misclassification (eg, cause of death) biases. Reporting of acute HCV infections throughout the United States to NNDSS is susceptible to underreporting12 not only because reporting is passive and voluntary but also because the surveillance case definition captures only persons with symptoms of an illness that is often asymptomatic. The implementation of complete and timely acute HCV surveillance by all states will increase the accuracy of this method. Fourth, the HIV proximity measure might not accurately measure risk of IDU-associated HIV transmission. Our estimate is limited by the distance of the buffer zone selected and may not reflect the population distribution within each county or underlying characteristics of PLWH in these areas (eg, percent with suppressed viral load). Lastly, the indicators used may result in bias against identifying urban areas as vulnerable because the percentages of certain characteristics (eg, percentage white, non-Hispanic) are lower in urban counties. However, the historic concentration of IDU in urban areas has likely resulted in these areas having already taken preventive actions (eg, SSPs, access to MAT) to reduce risk for infections from IDU.
Prompted by a recent outbreak of HIV infection among PWID in a rural community, we developed a method to identify other communities vulnerable to rapid dissemination of IDU-associated HIV, if introduced, and new or continuing high numbers of HCV infections. Identification of a county as vulnerable to this type of outbreak does not mean an outbreak is eminent; rather jurisdictions identified as at-risk might use potentially informative local data that were not available nationally and take action as recommended in the April 2015 CDC Health Alert Network advisory.34 Expanding epidemics of prescription opioid abuse and unsterile IDU and shifting demography and geography, heralded by national changes in patterns of acute HCV infection, are critical driving forces of vulnerability. To reduce vulnerability, targeted interventions in accordance with efforts to prevent and treat substance use disorder and to reduce risk of infectious complications of IDU are warranted.
HIV Proximity
For each vulnerable county, we sought to assess the likelihood that HIV might be introduced into a network of PWID in that county based on the prevalence of HIV infection in that county and nearby. We defined "HIV proximity" as the weighted average rate of people living with diagnosed HIV infection (PLWH) in and around that vulnerable county at year-end 2012. We demarcated a 20-mile buffer zone around the border of each vulnerable county based on data from the US Department of Transportation National Household Travel Survey that the average daily distance traveled per person per day was 36 miles (approximately 20 miles when rounded for a radius).15 Using a method of spatial smoothing,16 we calculated the area proportion of each county adjacent to the vulnerable county that intersected the vulnerable county's 20-mile buffer zone and the corresponding weighted numbers of PLWH and total population represented by the buffer zone. We summed these buffer zone values with the values for the vulnerable county to calculate an estimated HIV proximity rate of PLWH per 10,000 population. We used Jenks natural breaks to group counties by estimated HIV proximity.17
RESULTS
The number of acute HCV infection cases reported to CDC in 2012 and 2013 were 1778 and 2138, respectively. Of the reported cases, 1710 (96%) in 2012 and 2074 (97%) in 2013 were reported from 2970 counties with valid county FIPS codes and were included in modeling. There were 173 counties in 8 states and the District of Columbia with no data during 2012-2013; these jurisdictions were excluded from modeling analyses (Alaska, Arizona, Delaware, District of Columbia, Hawaii, Mississippi, New Hampshire, Rhode Island, and Wyoming). Descriptive statistics are presented in Table 2.
In the univariable regression models, all indicators were significant at P < 0.1, except mental health providers and percentage of the population without high school diploma (Table 2). We found neither substantial departures from linearity nor collinearity between the continuous indicators. Based on the final multivariable model, the following indicators were most significantly associated with the county-level acute HCV infection rate: drug-overdose deaths per 100,000 population [regression coefficient (β) 0.016; P < 0.0001], prescription opioid sales per 10,000 population (β 0.024; P = 0.0015), median per capita income, log10 (β -2.181; P < 0.0001), percent of population of white, non-Hispanic race/ethnicity (β 0.027; P < 0.0001), percent of population aged ≥16 years unemployed (β 0.038; P = 0.0095), and buprenorphine prescribing potential by DATA 2000 waiver per 10,000 population (β 0.002; P = 0.0095) (see Supplemental Digital Content, http://links.lww.com/QAI/A844, Supplemental Results and Supplemental Figs. 2 and 3, which describe the model fit results, show the reported rate of acute HCV infection and model-estimated rate of acute HCV infection by county, and illustrate the model fit and 90% confidence intervals for the counties identified as vulnerable).
|
| | | | | | |
|