 |
 |
 |
| |
Ending AIDS: myth or reality? New Infections
Increase in Key Populations, UN Update
|
| |
| |
Ending AIDS - What is the Real prospect: New Infections Up in Key Populations, Unsupressed Viremia High in Key Populations - (09/14/17)
Download the PDF here
Download the PDF here
Download the PDF here
from Jules: The suffering associated with Aging with HIV is reality, no confusion about myth or reality. But everything around HIV sucks all the air out of the room, there is nothing left for aging with HIV.
"....Yet in 2015, 15 million people living with HIV were estimated to be unaware of their status and 1⋅1 million died of AIDS-related complications, despite the fact that US$19 billion was invested in HIV in low-income and middle-income countries"
Lancet July 31 2017 - *Brian G Williams, Reuben Granich
South African Centre for Epidemiological Modelling and Analysis, Stellenbosch University, Stellenbosch 7602, South Africa (BGW); and International Association of Providers of AIDS Care, Washington, DC, USA (RG)
In 2014, prompted by the realisation that an expansion of HIV treatment can prevent illness, death, and transmission of infection, the Joint UN Programme on HIV/AIDS announced their 90-90-90 target and goal to end AIDS by 2030.1 This target and goal were informed by the strategic objective that if at least 90% of people infected with HIV knew their status, and at least 90% of those who knew their status were on antiretroviral therapy, and at least 90% of those who were on antiretroviral therapy were virally suppressed, ending AIDS would be achievable by 2030. When the 90-90-90 target is reached in each country, such that 73% of people living with HIV are on treatment and virally suppressed, the government should not rest on its laurels, but instead continue to expand treatment. In the words of the Joint UN Programme on HIV/AIDS, "the aim in the post-2015 era is nothing less than the end of the AIDS epidemic by 2030";1 however, what is meant by the phrase, "the end of AIDS", is yet to be agreed upon. The working definition states there should be fewer than one new HIV infection and one new AIDS-related death per 1000 people in the population, such that HIV is no longer a major threat to public health.2, 3 Ending AIDS does not mean ending HIV and, if the world does end AIDS by 2030, 35 million people will still live with HIV for the next 30 years or more, and will need ongoing care and support unless, and until, a cure is found.
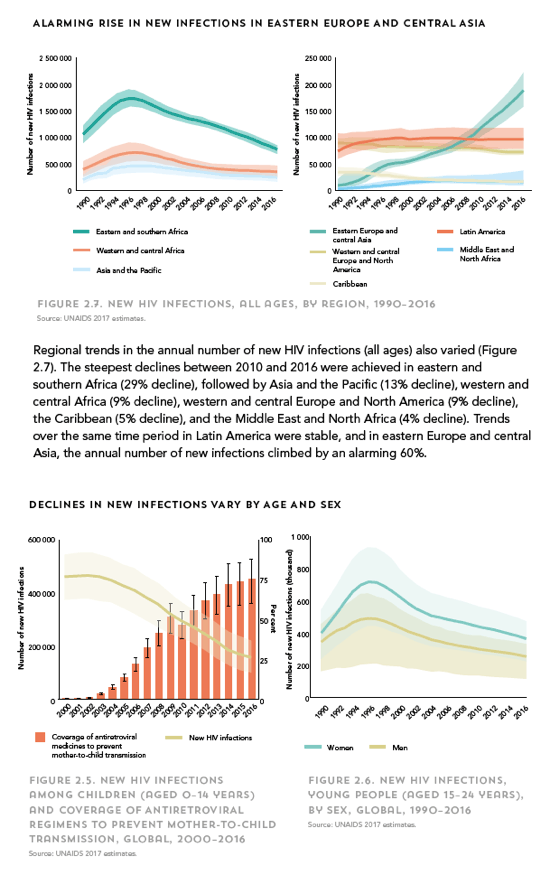
Globally, between 2010 and 2015, about 2 million people started taking antiretroviral therapy each year, and by mid-2016 an estimated 18 million people were on treatment.4 An estimated 60% of those infected with HIV know their status, 50% of those who know their status are on antiretroviral therapy, and 90% of those who are on antiretroviral therapy are virally suppressed.5 Although much still needs to be done to ensure 27 million people are on treatment by 2020, the global progress has been impressive. The case reproduction number for HIV (ie, the number of secondary cases caused by one primary case in a susceptible population) is around seven in most settings and is dependent on the mode of transmission, but with immediate treatment and good adherence, the treatment of one person with antiretroviral therapy could avert up to seven subsequent infections. A 2016 report5 suggests the number of new infections in each of the five regions defined by the Joint UN Programme on HIV/AIDS has remained unchanged from 2010 to 2015, except in eastern Europe where the number has risen. Between 2010 and 2015, an estimated US$20 billion per year-$100 billion in total-was spent on the global management of the HIV epidemic, with approximately 50% of these resources spent on the expansion of access to treatment.6 If this massive spending and roll-out of antiretroviral therapy has not significantly reduced the rate of new HIV infections, the prospect of ending AIDS in the foreseeable future is bleak. By contrast, other estimates suggest that the continued expansion of antiretroviral therapy will substantially reduce the rate of new infections and AIDS-related deaths in sub-Saharan Africa and elsewhere,6, 7, 8, 9 the money has been well spent, and further expansion of treatment will reduce costs.7
A review of the assumptions used to project the effects of antiretroviral therapy on the rate of new infections and AIDS-related mortality is urgently needed. If the rate of new infections is not falling, and falling rapidly at that, the global strategy for the management and control of the epidemic of HIV must be revised. If the rate of new HIV infections is falling, then agreement must be reached as to what the effects of expanded treatment and other preventive interventions have been, and are likely to be in the future. These discussions can then be translated into improved prioritisation among testing, treatment, care, and prevention to ensure the most efficient use of the resources available to end AIDS.
---------------------
End Aids UN Report
Joint United Nations Programme on HIV/AIDS (UNAIDS


--------------------------
90-90-90 and ending AIDS: necessary and feasible, Comment
Lancet July 31 2017 - *Reuben Granich, Brian Williams, Julio Montaner, José M Zuniga
More than three decades into the global HIV pandemic, there are still 2⋅1 million new infections each year and 36⋅7 million people are living with HIV.1 By mid-2016, 18⋅2 million people were on antiretroviral treatment-about 50% of people living with HIV.1 Yet in 2015, 15 million people living with HIV were estimated to be unaware of their status and 1⋅1 million died of AIDS-related complications, despite the fact that US$19 billion was invested in HIV in low-income and middle-income countries.1
Although its history is complex, the HIV pandemic can be characterised by three phases: devastation; discovery and action; and ending AIDS (figure). The initial response was defined by overwhelming devastation of marginalised individuals and their communities, the root causes of which were widespread denial, ignorance, stigma, fear, and neglect. It was a time when affected communities and beleaguered health-care providers struggled in isolation to minister to the sick and dying while governments, experts, and other authorities exercised little if any political will to address a burgeoning health crisis or exacerbated the crisis through their policies.4 Out of this suffering emerged a determined community response that demanded leadership and resources from governments. The discovery and action phase resulted from the growing community, scientific, and political response that unravelled the secrets of HIV. Despite remarkable progress, the accepted wisdom was that ending AIDS was not feasible without a vaccine or cure. Without effective treatment, the focus was on prophylaxis and treatment of opportunistic illnesses, palliative care, ensuring human rights, tackling stigma and discrimination, community support for people with HIV, and prevention methods.5 The development of life-saving, triple drug therapy in 1996 gave hope along with the realisation that most of the people infected with HIV lived in low-income countries and it was morally unacceptable to deny them treatment.6, 7 The creation of the Global Fund to Fight AIDS, Tuberculosis and Malaria in 2001 and the US President's Emergency Plan for AIDS Relief (PEPFAR) in 2003, the Millennium Development Goals, and the launch of WHO's 3 by 5 initiative, signalled the translation of discovery to action. In the face of considerable scepticism, antiretroviral treatment was delivered at scale and it was subsequently shown that ART leads to a near normal disease-free lifespan and virtually eliminates the risk of HIV transmission.8 By 2006, the old "test and wait" strategy of withholding antiretroviral treatment until people's immune systems were severely compromised no longer made sense.9 These and other developments provided the foundation for the next phase of the HIV pandemic-ending AIDS.
This phase reflects the political shift from a struggle to contain the epidemic to the right to universal HIV treatment as part of a winnable public health battle-a goal embodied in Sustainable Development Goal 3 (table). Ending AIDS means providing treatment for at least 35 million people living with HIV for the rest of their lives or until a cure is developed. Elimination is measured as incidence of less than one case per 1000 population per year.11 HIV eradication (zero global incidence) is not feasible without deploying a cure or vaccine alongside treatment. Other prevention interventions-eg, behavioural change, pre-exposure prophylaxis, condoms, voluntary male circumcision, opioid substitution therapy, and needle and syringe programmes-will be necessary, but not sufficient on their own without universal treatment, to end AIDS in most settings.
UNAIDS, PEPFAR, national governments, and many cities have adopted the 90-90-90 target by 2020. This target calls for 90% of people living with HIV diagnosed, 90% of people diagnosed on sustained antiretroviral treatment, and, of those, 90% virally suppressed by 2020.12 The 90-90-90 and the subsequent 95-95-95 by 2030 targets translate into 73% and 86% of people living with HIV being virally suppressed on antiretroviral treatment, respectively.12 In late 2015, after the example of the USA (2012), France (2013), Brazil (2013), and seven other countries, WHO recommended starting antiretroviral treatment irrespective of CD4 cell count.13 As of July, 2017, 51 countries (73% of global HIV burden) have published test and treat guidelines.13
As part of the 90-90-90 efforts, the Fast-Track Cities Initiative is a partnership between the City of Paris, International Association of Providers of AIDS Care (IAPAC), UNAIDS, and the UN Human Settlements Programme, in collaboration with other stakeholders, and includes more than 75 cities focused on achieving the 90-90-90 target and zero stigma through the acceleration of local AIDS responses.14 Reaching the end of AIDS, as defined by low levels of HIV incidence and AIDS-related mortality, has already been achieved in some settings. However, to end AIDS globally will require continued effort and a near doubling of the number of people on treatment.
There remains controversy about the feasibility, cost, and epidemiological impact of the 90-90-90 target, with calls for increased prioritisation of other HIV prevention methods15 and other appeals for a 30% increase in annual funding to end AIDS as a public health threat by 2030.16 Using a conservative $300 per person for antiretroviral treatment would result in an $11 billion annual price tag for 36⋅7 million people living with HIV-far below the current $19 billion annually available resources and the UNAIDS $26⋅1 billion resource needs estimate.16 Although the true cost is unknown, resources, time, and targets will probably stay fairly fixed and needs projections should explore a more efficient, evidence-based service delivery model that prioritises achieving the 90-90-90 target.
Four major innovations will accelerate progress towards 90-90-90 and the end of AIDS. First, reliable, easy-to-use, rapid HIV self-tests that, like pregnancy self-tests a generation ago, will democratise access to HIV testing.17 Second, safer and more effective integrase inhibitors-based antiretroviral treatment, together with same-day offer of treatment and reduction of follow-up clinic visits, will increase efficiency of antiretroviral treatment programmes;18 over time long-acting injectable antiretroviral treatment might be able to further accelerate this trend.19 Third, comprehensive integrated community HIV service delivery models for HIV and other health services will help reach the 90-90-90 target and beyond with the potential added value of destigmatising both HIV and HIV services. Fourth, the information technology revolution, mobile computing, crowd-sourcing, and cloud-based monitoring and evaluation software are already changing the way we do public health by providing near real-time information on programme progress, and more open data and transparency for improved community engagement.
Global public health security and human rights demand a focus on ending AIDS. Prioritising expanded access to HIV self-testing, delivering life-long treatment through community-based comprehensive HIV services, efficiently using limited resources, harnessing new information technology, and enabling meaningful community engagement will all be necessary. Although there are signs of cynicism and complacency, now is not the time to falter on the collective global HIV response. It is time to double down on investment and finish the job of ending AIDS.
RG, BW, and JMZ declare no competing interests. JM has received research grants paid to his institution from the Public Health Agency of Canada, BC Ministry of Health, Canadian Institutes of Health Research/Genome BC, the US National Institutes of Health, Johnson & Johnson, and Merck Canada; and has served on the Teva Scientific advisory board participant in 2015, providing feedback as an expert in HIV.
|
| |
|
 |
 |
|
|