 |
 |
 |
| |
Is on-demand PrEP a suitable tool for MSM who practice chemsex? Results from a sub-study of the ANRS-IPERGAY trial - Chemsex Users in IPERGAY Twice as Likely to Use As-Needed PrEP
|
| |
| |
Chemsex Users in IPERGAY Twice as Likely to Use As-Needed PrEP
9th IAS Conference on HIV Science (IAS 2017), July 23-26, 2017, Paris
Mark Mascolini
IPERGAY trial participants who practice chemsex--using psychoactive drugs before or during sex--proved twice as likely to take tenofovir/emtricitabine (TDF/FTC) PrEP the last time they had sex compared with participants who avoided chemsex [1]. Chemsex users felt they ran a higher risk picking up HIV during sex.
Chemsex is a growing concern among MSM because it boosts sexual risk taking and may raise chances of acquiring HIV infection [2]. Favored chemsex drugs include crystal meth, GHB/GBL, and cathinones. The randomized IPERGAY trial in MSM found that as-needed PrEP--taken only before and after sex--cut HIV transmission risk by 86% [3]. IPERGAY investigators conducted a substudy to assess as-needed PrEP among trial participants who engaged in chemsex.
IPERGAY recruited men or transgender women who have sex with men at high risk for HIV acquisition. Every 2 months participants completed online questionnaires about alcohol and drug use, sexual behavior, and PrEP adherence. The chemsex substudy involved 331 IPERGAY participants with a median 10 months of follow-up during an open-label extension phase of the trial. The researchers aimed to determine whether chemsex users took at least one TDF/FTC pill during their most recent sex.
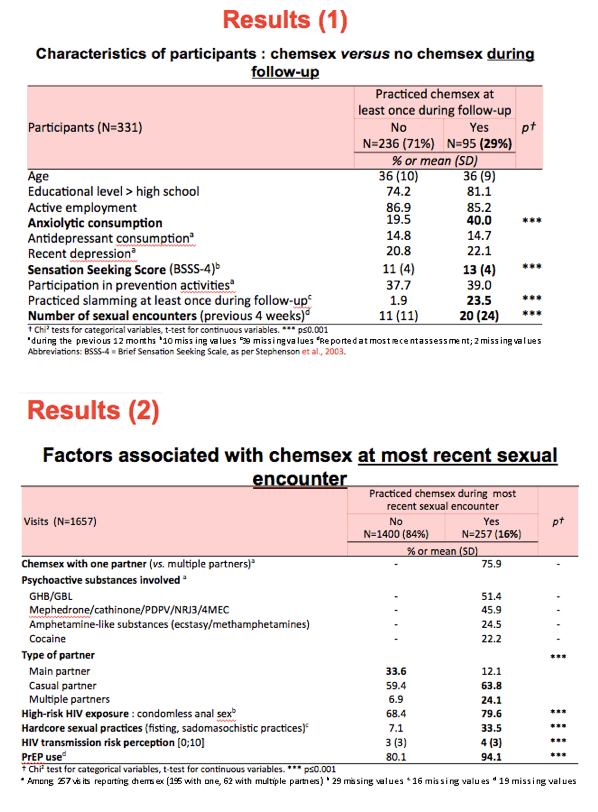
Of the 331 participants, 95 (29%) practiced chemsex and 236 (71%) did not. Both groups averaged 36 years in age, and similar high proportions had more than a high school education and steady employment. A significantly higher proportion of the chemsex groups took anxiolytics (40% versus 19.5%, P
Compared with men who did not practice chemsex, those who did were more likely to have a casual rather than a main partner the last time they had sex (63.8% versus 59.4%, P
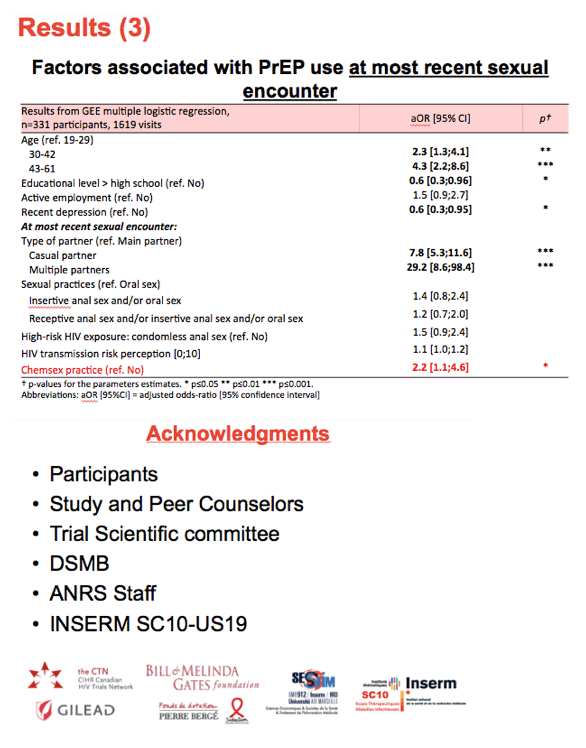
Multiple logistic regression determined that chemsex practitioners were twice as likely to use PrEP the last time they had sex (adjusted odds ratio [aOR] 2.2, 95% confidence interval [CI] 1.1 to 4.6, P < 0.05). This analysis identified six other factors that raised or lowered chances of PrEP use at last sex (aOR below 1.0 indicates a lower chance):
-- 30-42 years old vs 19-29: aOR 2.3, 95% CI 1.3 to 4.1, P < 0.01
-- 43-61 years old vs 19-29: aOR 4.3, 95% CI 2.2 to 8.6, P < 0.001
-- More than high school education vs less: aOR 0.6, 95% CI 0.3 to 0.96, P < 0.05
-- Recent depression: aOR aOR 0.6, 95% CI 0.3 to 0.95, P < 0.05
-- Casual vs main partner: aOR 7.8, 95% CI 5.3 to 11.6, P < 0.001
-- Multiple partners vs main partner: aOR 29.2, 95% CI 8.6 to 98.4, P < 0.001
The IPERGAY investigators concluded that chemsex users have "a more vulnerable psychological profile" characterized by greater anxiolytic use and higher sensation-seeking scores. They proposed that "PrEP is a suitable tool to reduce HIV transmission in chemsexers." They added that prescribing PrEP to these men affords an opportunity to discuss other HIV prevention interventions and to institute comprehensive care.
References
1. Roux P, Fressard L, Suzan-Monti M, et al. Is on-demand HIV pre-exposure prophylaxis (PrEP) a suitable tool for men who have sex with men (MSM) who participate in chemsex? Results from a sub-study of the ANRS-IPERGAY trial. 9th IAS Conference on HIV Science (IAS 2017), July 23-26, 2017, Paris. Abstract TUAC0503.
2. Bourne A, Reid D, Hickson F, Torres-Rueda S, Weatherburn P. Illicit drug use in sexual settings ('chemsex') and HIV/STI transmission risk behaviour among gay men in South London: findings from a qualitative study. Sex Transm Infect. 2015;91:564-568.
3. Molina JM, Capitant C, Spire B, et al. On-demand preexposure prophylaxis in men at high risk for HIV-1 infection. N Engl J Med. 2015;373:2237-2246. http://www.nejm.org/doi/full/10.1056/NEJMoa1506273
--------------------------
Is on-demand PrEP a suitable tool for MSM who practice chemsex? Results from a sub-study of the ANRS-IPERGAY trial
Roux P1, Fressard L1, Suzan-Monti M1, Chas J2, Capitant C3, Meyer L3, Tremblay C4, Molina JM5, Pialoux G2, Spire B1
1INSERM UMR912 - SESSTIM, Marseille; 2Hopital Tenon, Paris; 3INSERM SC10, Le Kremlin-Bicetre; 4Université de Montréal; 5Hopital Saint-Louis, Paris



|
| |
|
 |
 |
|
|