 |
 |
 |
| |
TCM CD4 T cell infection extent before ART associated with immune failure and HIV persistence on ART
|
| |
| |
Download the PDF here
Reported by Jules Levin
9th IAS Conference on HIV Science (IAS 2017), July 23-26, 2017, Paris
Vincent C. Marconi MD1,2,3, Emily Ryan2, Luca Micci PhD2, Amelie PagliuzzaM.Sc4, Sol Aldrete MD1, Keith Delman MD1, Jacob Estes PhD5, Nicolas Chomont PhD6, Rafick Sekaly PhD7, Mirko Paiardini PhD2
1Emory University School of Medicine, 2Yerkes Non-Human Primates Research Center, 3Rollins School of Public Health, 4Centre de recherche du CHUM, 5Frederick National Laboratory, LeidosBiomedical Research, 6Université de Montréal, 7Case Western Reserve University
Abstract
Background: Despite antiretroviral therapy (ART) fully suppress HIV replication, immune dysfunction - including incomplete recovery of CD4 T-cells - inflammation, and HIV persistence endure for many individuals. Based on a large set of preliminary data, we hypothesized that differential infection of specific CD4 T-cell subsets could further explain divergent CD4 recovery and maintenance of the HIV reservoir during ART.
Methods: 30 HIV-positive individuals were enrolled. Immunologic responders (IR) were defined as having CD4 counts >500 cells/µL < 2 years after ART initiation; Immunologic non-responders (INR) as having CD4 counts < 350 cells/ µL up to 2 years after ART initiation. Before and during ART, the frequency of total (T) and integrated (I) HIV-DNA was measured in sorted blood naïve, central (CM), transitional (TM), and effector memory CD4 T-cells. T-cell levels, activation/proliferation states, and expression of co-inhibitory receptors (Co-IRs) were analyzed by flow cytometry.
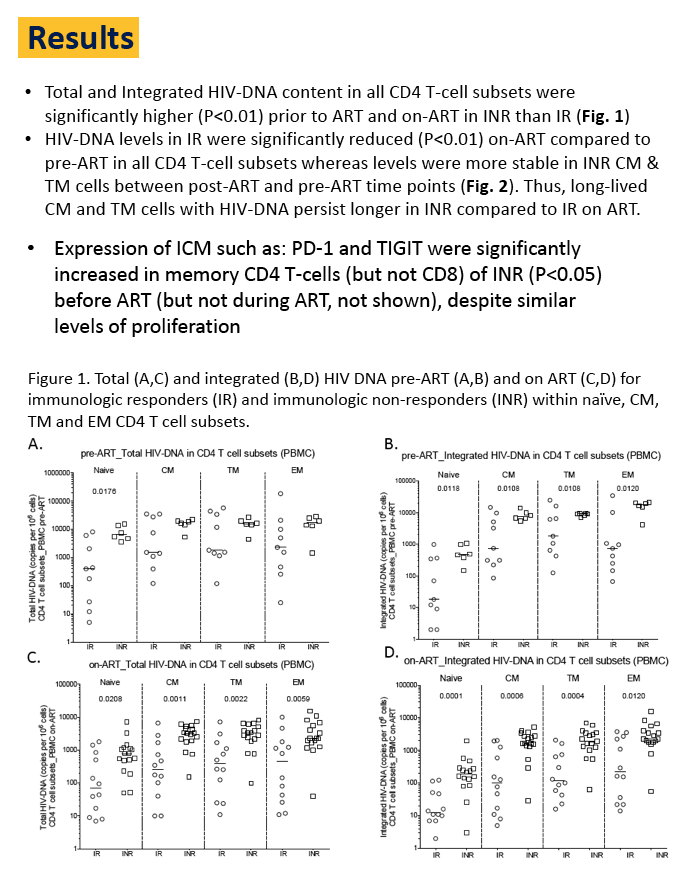
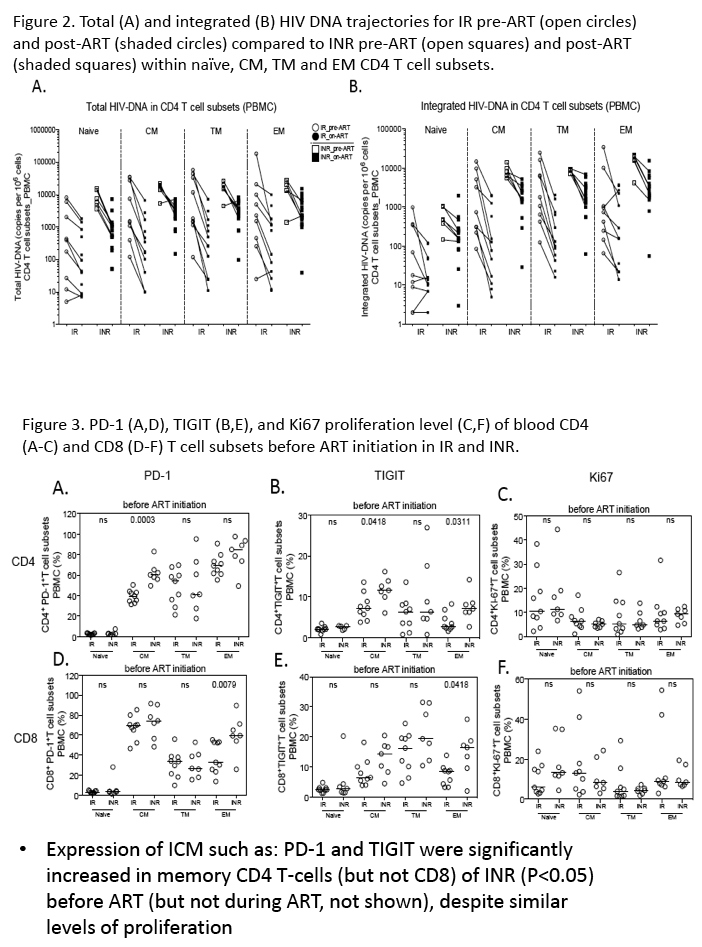
Results: Median age of the cohort was 46; 90% were male and 82.8% were African-American. T and I HIV-DNA content in all CD4 T-cell subsets were significantly higher (P< 0.01) prior to ART and on-ART in INR than IR. The increased HIV-DNA content in INR was associated with higher levels of T-cell proliferation and activation, both at pre- and on-ART (P< 0.05). Expression of Co-IRs such as: PD-1 and TIGIT was significantly increased in memory CD4 T-cells of INR (P< 0.05), with the frequency of these Co-IR-expressing T-cells correlating with levels of I HIV-DNA. HIV-DNA contents in IR were significantly reduced (P< 0.01) on-ART as compared to pre-ART in all CD4 T-cell subsets. Remarkably, INR T and I HIV-DNA levels were significantly more stable in CM and TM CD4 T-cells between pre- and on-ART, and despite INR have been on-ART longer than IR.
Conclusions: When compared to IR, INR demonstrate higher levels of T-cell activation, Co-IRs expression, and viral burden in all memory CD4 T cell subsets, both prior to and on-ART. Furthermore, CM and TM CD4 T-cells harboring HIV-DNA persist longer during ART in INR. These data link levels of inflammation and CD4 T-cell infection prior to ART, particularly in long-lived CD4 T-cell subsets, with immune recovery and HIV persistence.

|
| |
|
 |
 |
|
|