 |
 |
 |
| |
Effect of a multidisciplinary intervention for early ART initiation for inpatients with newly diagnosed HIV: Inpatient Program Yields Higher Linkage and ART Rates in Atlanta Hospital
|
| |
| |
Inpatient Program Yields Higher Linkage and ART Rates in Atlanta Hospital
IDWeek2017/IDSA, October 4-8, 2017, San Diego
Mark Mascolini
An intervention aimed at faster linkage to care and antiretroviral therapy (ART) in inpatients newly diagnosed with HIV attained those goals in a before-and-after comparison at Atlanta's Grady Memorial Hospital [1]. But most people did not start ART while in the hospital.
Prompt linkage to HIV care, initiation of ART, and viral suppression are key goals of the HIV care continuum. Emory University and Grady researchers who conducted this study underlined the "significant attrition" that lies between HIV diagnosis and the start of ART, especially in indigent populations. They aimed to assess the impact of a multidisciplinary intervention for early-ART initiation in inpatients newly diagnosed with HIV.
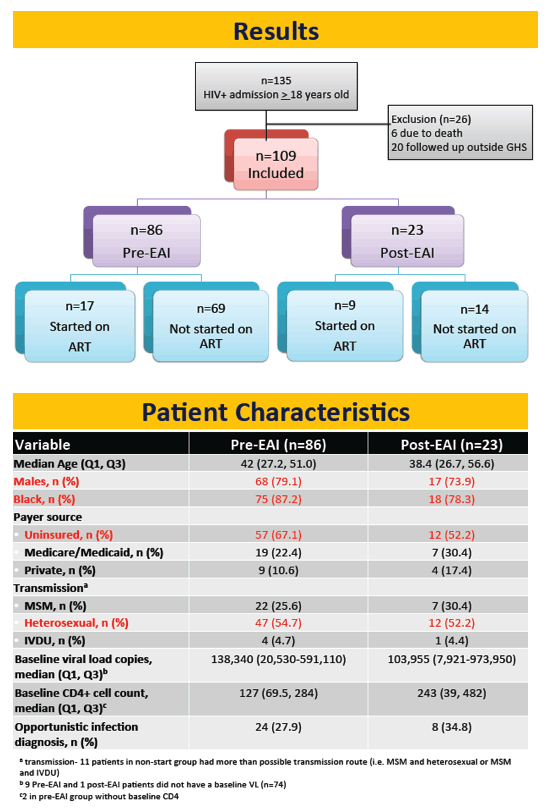
This single-center retrospective chart review with 6 months of follow-up involved adults with a new HIV diagnosis in the Grady Health System and admitted to Grady Memorial Hospital from January 2015 through September 2016. Everyone was naive to ART or off treatment since before January 2015. Researchers defined enrollment as keeping a clinic appointment within 30 days of hospital discharge; they defined viral suppression as a viral load at or below 200 copies within 6 months of discharge. The investigators compared outcomes before and after the early ART intervention began in May 2016.
The analysis included 109 adults, 86 in the preintervention period and 23 in the postintervention period. Median age was 42 in the preintervention group and 38.4 in the postintervention group. Respective proportions of men were 79% and 74%, blacks 87% and 78%, and heterosexuals 55% and 52%. The preintervention group had a higher proportion of uninsured people (67% versus 52%) and a lower median baseline CD4 count (127 versus 243) but also a lower proportion with an opportunistic infection diagnosis (28% versus 35%).
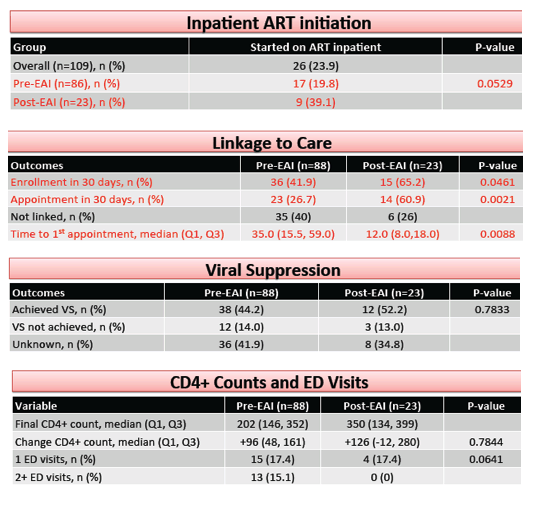
Outcome variables proved consistently better in the group seen after the early-ART intervention took hold, as indicated by these preintervention/postintervention comparisons:
-- Started ART as an inpatient: 19.8% versus 39.1%, P = 0.0529
-- Enrollment in care within 30 days: 41.9% versus 65.2%, P = 0.0461
-- Appointment within 30 days: 26.7% versus 60.9%, P = 0.0021
-- Median time to first appointment: 35 versus 12 days, P = 0.0088
A lower proportion of the preintervention group attained viral suppression, but the difference lacked statistical significance (44.2% versus 52.2%, P = 0.78).
The researchers concluded that their early-ART intervention yielded a strong trend favoring starting ART as an inpatient and significantly faster enrollment in care and time to a first appointment. But even after the intervention began, 61% of inpatients did not start ART before discharge, a finding indicating substantial room for improvement.
Reference
1. Root H, Tidwell A, Nguyen ML, et al. Effect of a multidisciplinary intervention for early ART initiation for inpatients with newly diagnosed HIV. IDWeek2017/IDSA. October 4-8, 2017. San Diego. Abstract 1423.



|
| |
|
 |
 |
|
|