 |
 |
 |
| |
Access to Online Tools Boosts Chances of HIV Control in Large US Group - "ASSOCIATION BETWEEN PATIENT PORTAL ACCESS & VIRAL SUPPRESSION AMONG PEOPLE LIVING WITH HIV"
|
| |
| |
Sarah Scott, MD,
IDWeek2017/IDSA, October 4-8, 2017, San Diego
Mark Mascolini
Patient portals--online patient-centered messaging tools--raised chances of viral suppression independently of clinical and demographic factors in a 4237-person study at Vanderbilt University in Nashville [1]. Black race and lower socioeconomic status decreased chances of HIV control.
Viral suppression remains the ultimate goal of the HIV care continuum for everyone with HIV. Much research has addressed factors that favor or impede viral suppression, but no one has studied the impact of patient portals, which the Vanderbilt team defined as "online tools that enable patient interaction with healthcare systems and may increase patient engagement and improve health outcomes." The Vanderbilt Comprehensive Care Clinic offers a portal that includes a patient's record, an appointment log, messaging capability, a tool to set health goals and track progress, and other features. The aim of this study was to see whether access to this portal affects viral suppression.
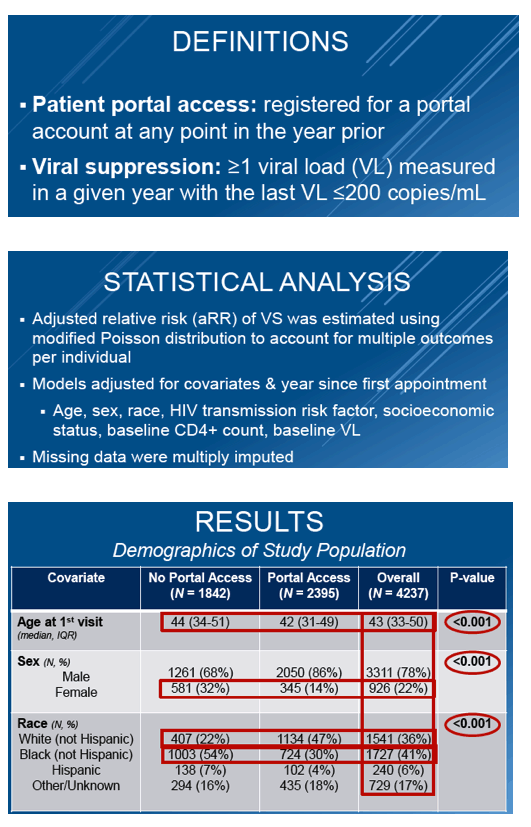
This observational cohort study enrolled HIV patients at least 18 years old who made at least one visit to the Vanderbilt clinic between January 2011 and December 2015. The researchers defined patient portal access as registration for a portal account any time in the previous year. They defined viral suppression as one or more viral loads measured in a given year, with the last load at or below 200 copies. To identify factors independently associated with viral suppression, the researchers used modified Poisson distribution adjusted for age, sex, race, HIV transmission risk factor, socioeconomic status, baseline CD4 count, baseline viral load, and years since first appointment.
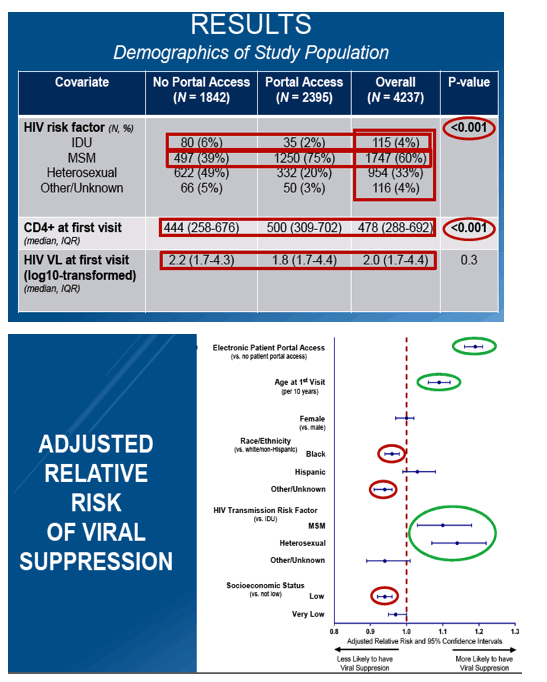
The analysis involved 4237 people with HIV, 2395 of whom (56.5%) had portal access. Median age was younger in people with versus without portal access (42 versus 44 years, P < 0.001). Portal users included a lower proportion of women (14% versus 32%), a higher proportion of whites (47% versus 22%), a lower proportion of blacks (30% versus 54%), a lower proportion of drug injectors (2% versus 6%), and a higher proportion of men who have sex with men (MSM, 75% versus 39%) (P < 0.001 for all differences). CD4 count at the first Vanderbilt visit was higher in portal users than nonusers (500 versus 444, P < 0.001).
Portal access independently improved chances of viral suppression about 20% (adjusted relative risk [aRR] about 1.2). Three other factors independently raised chances of suppression: older age (aRR about 1.1 per 10 years), heterosexual HIV risk versus injecting drugs (aRR about 1.15), and MSM risk versus injecting drugs (aRR about 1.1). Three factors independently lowered chances of viral suppression: black versus white race, other/unknown race, and low socioeconomic status (aRR about 0.95 for all three).
The Vanderbilt team noted that their analysis is limited by focusing on patient portal access rather than actual use and by possible unmeasured confounders, such as health and computer literacy and education level. With those limitations in mind, they proposed that "encouraging patient engagement through registering for institution-specific electronic patient portals may lead to improved clinical outcomes in people living with HIV."
Reference
1. Scott S, Jenkins C, Rebeiro P, et al. Association between patient portal access and viral suppression among people living with HIV in a large southeastern clinical cohort. IDWeek2017/IDSA. October 4-8, 2017. San Diego. Abstract 1689a.



|
| |
|
 |
 |
|
|