 |
 |
 |
| |
HIV Diagnosis After Age 50 Often Delayed Despite Clear Clues - Should age-associated, Non-AIDS conditions Invite HIV Testing, YES
|
| |
| |
25th Conference on Retroviruses and Opportunistic Infections (CROI), March 4-7, 2018, Boston
from Jules: Those Diagnosed with HIV at over 60 Years Old Are More likely to Have Certain Non-AIDS Conditions - the presence of these conditions is a clue to TEST for HIV
Mark Mascolini
HIV diagnoses remain frequent after age 50, though abundant diagnoses with more advanced disease suggest undue delay in spotting HIV in older adults [1]. Those conclusions emerged from analysis of data from the mostly male Veterans Aging Cohort Study (VACS), which pinpointed five non-AIDS indicators of HIV more common in people who do test positive--bacterial pneumonia, Herpes zoster, anemia, lymphocytopenia, and thrombocytopenia.
VACS investigators who conducted this study noted frequent "concerning stories" about older people diagnosed with advanced HIV infection after lengthy workups, even at "respected medical centers." To address this problem, the VACS team analyzed data from their large cohort of HIV-positive and negative veterans in care.
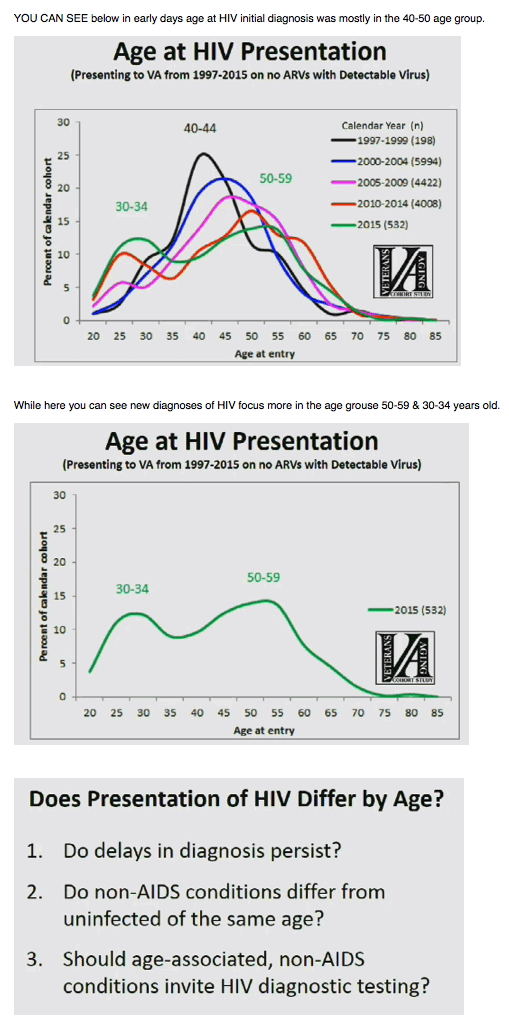
First the researchers calculated age distribution of veterans newly diagnosed with HIV at a VA facility from 1997 through 2015. All had a detectable viral load and none took antiretrovirals. The typical age at presentation changed from 40-44 years in 1997-1999 to a two-peak distribution in more recent years: By 2015 most new HIV infections in veterans involved two age groups: 30 to 34 years and 50 to 59 years.
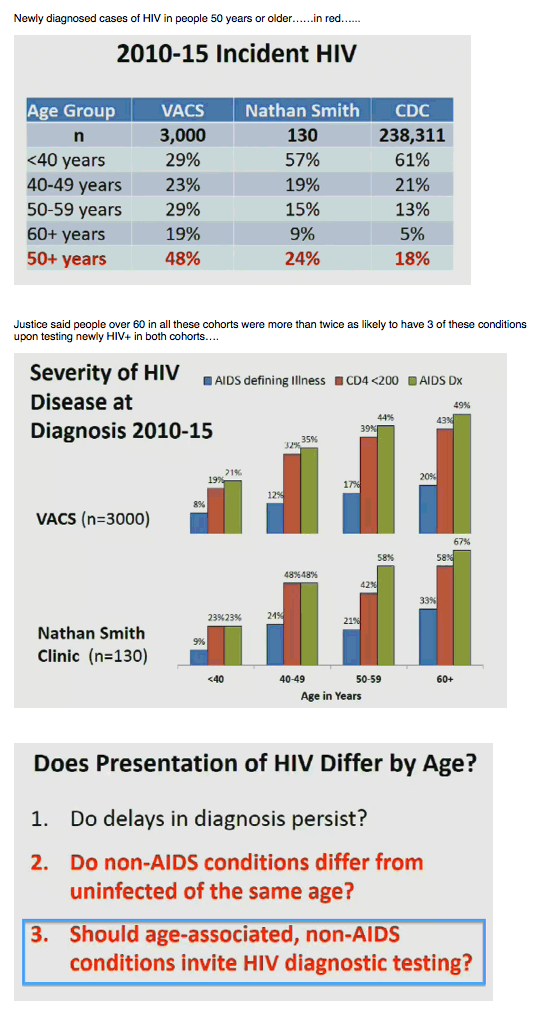
To learn whether HIV diagnosis delays persist and whether initial non-AIDS conditions differ in veterans with versus without HIV, the researchers probed VACS electronic records for 2010-2015. They also reviewed 2010-2015 data from the CDC HIV Surveillance Report and from the Nathan Smith Clinic at Yale New Haven Hospital. This analysis involved 3000 VACS participants with incident HIV infection, 130 newly diagnosed patients at Nathan Smith Clinic, and 238,311 incident HIV cases across the United States in the CDC database. The proportion of people with new HIV in 2010-2015 who were 50 or older was substantially higher in the VACS (48%) than at Nathan Smith (24%) or across the United States (18%). Respective proportions of HIV diagnoses at age 60 or older were 19%, 9%, and 5%.
In both the VACS and the Nathan Smith records, proportions of 2010-2015 HIV diagnoses with an AIDS illness or a sub-200 CD4 count rose steadily with age. In the VACS proportions with AIDS at diagnosis were 21% in people under 40 years old, 35% at age 40-49, 44% at age 50-59, and 49% at 60 or older. Proportions were even higher at Nathan Smith: 23% in people under 40 years old, 48% at age 40-49, 58% at age 50-59, and 67% at 60 or older.
Next the VACS investigators asked whether non-AIDS presenting conditions differed in veterans with versus without HIV in the age brackets spelled out in the preceding paragraph. They found that veterans with HIV had substantially higher rates of bacterial pneumonia, Herpes zoster, anemia (hemoglobin below 12 g/dL), lymphocytopenia (below 150K/mL), and thrombocytopenia (below 100K/mL). Proportions of veterans with each of the 5 conditions were always substantially higher in the HIV group across all age brackets, although prevalence of all conditions rose with age regardless of HIV status.
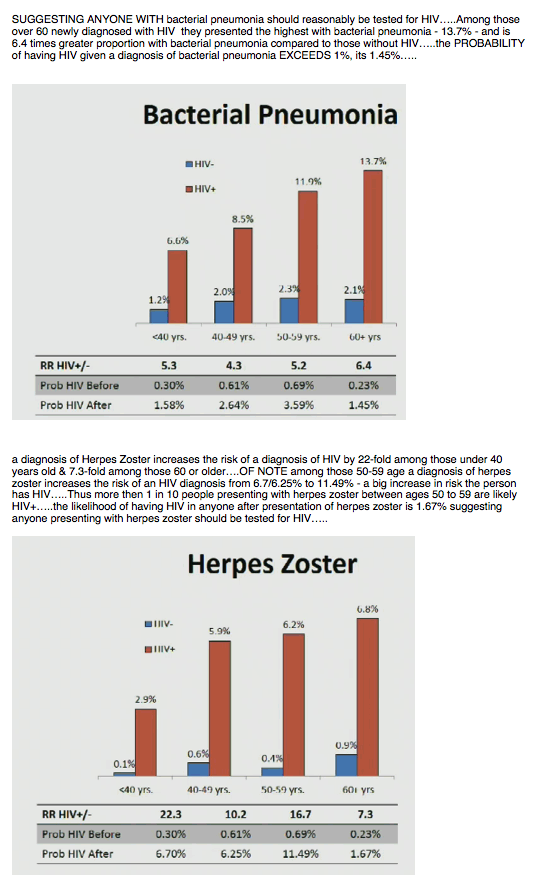
For example, proportions of HIV-positive and negative veterans with presenting bacterial pneumonia were 6.6% versus 1.2% under age 40, 8.5% versus 2.0% at 40-49, 11.9% versus 2.3% at 50-59, and 13.7% versus 2.1% at 60 or older. Relative risk of bacterial pneumonia was always at least 4-fold greater with HIV across the four age groups.
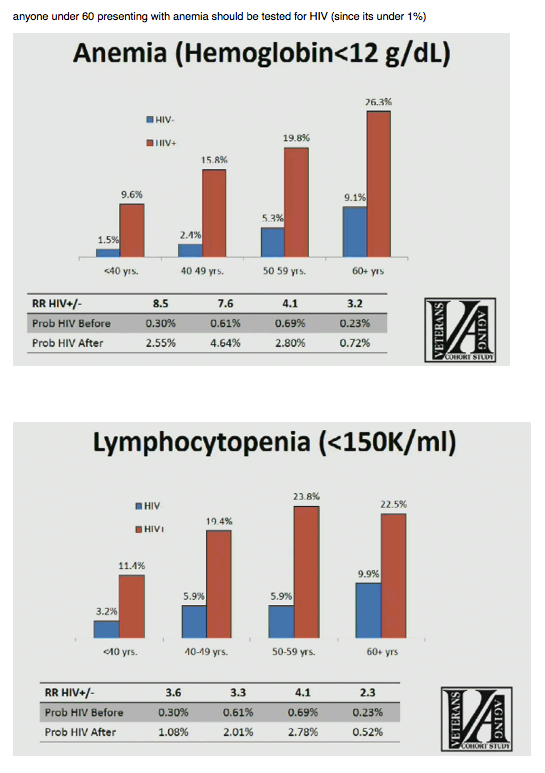
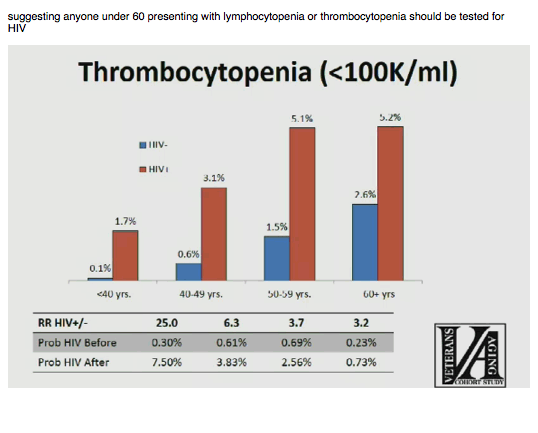
Among all five conditions, relative risk with HIV versus without HIV was highest for Herpes zoster: 22.3-fold under age 40, 10.2-fold at 40-49, 16.7-fold at 50-59, and 7.3-fold at 60 or older. The two most prevalent conditions in HIV-positive veterans were anemia (9.6%, 15.8%, 19.8%, and 26.3% across the four age groups) and lymphocytopenia (11.4%, 19.4%, 23.8%, and 22.5%). Respective proportions and relative risk with thrombocytopenia were 1.7% and 25.0-fold, 3.1% and 6.3-fold, 5.1% and 3.7-fold, and 5.2% and 3.2-fold.
The VACS team proposed that older people have a greater chance of getting diagnosed with advanced HIV and with five non-AIDS conditions. They suggested that "convergence of HIV and aging [is] likely to contribute to delays in [HIV] diagnosis." They proposed that the five "sentinel non-AIDS conditions," if otherwise unexplained, should prompt clinicians to test for HIV at any age.
Reference
1. Justice AC, Gordon KS, Feder S, et al. Clinical presentation of HIV differs by age in VACS (2010-2015). 25th Conference on Retroviruses and Opportunistic Infections (CROI). March 4-7, 2018. Boston. Abstract 92.
WEBCAST: http://www.croiwebcasts.org/console/player/37197?mediaType=slideVideo&&crd_fl=1&ssmsrq=1521726656000&ctms=5000&csmsrq=780

|
| |
|
 |
 |
|
|