| |
Real-world use of elbasvir-grazoprevir in patients with
chronic hepatitis C: retrospective analyses from the TRIO network
|
| |
| |
April 03, 2018
"Among the patients with Stage 4 or 5 CKD, 99% achieved SVR12. One quarter of patients had Stage 4 or 5 CKD, 30% had diabetes and 54% had hypertension."
17 April 2018 - AP&T - S. L. Flamm1 | B. Bacon2 | M. P. Curry3 | S. Milligan4 | C. U. Nwankwo5 |
N. Tsai6 | Z. Younossi7 | N. Afdhal3
Summary
Background
Elbasvir-grazoprevir is indicated for chronic hepatitis C virus (HCV) genotypes 1 and 4.
Aims
To evaluate the utilization and outcomes of chronic HCV patients treated with elbasvir-grazoprevir in the United States.
Methods
We conducted a retrospective cohort study of adults treated with elbasvir-grazoprevir with or without ribavirin for chronic HCV genotypes 1 or 4 infection. Data were collected from healthcare providers and specialty pharmacies through Innervation Platform, a proprietary, cloud-based disease management program from Trio Health. The primary endpoint was per protocol sustained virological response 12 weeks post-treatment (SVR12).
Results
Among 470 patients treated in 2016, 95% had HCV genotype 1 infection, 80% (373/468) were HCV treatment naïve and 70% (327/468) had non-cirrhotic disease. Almost 3 quarters (73%) of patients received care in community practices. The majority (89%) of patients received elbasvir-grazoprevir for 12 weeks. Per protocol SVR12 rates were 99% (396/402) for HCV genotype 1 and 95% (21/22) for HCV genotype 4. Among patients with Stage 4 or 5 chronic kidney diseases, 99% (113/114) achieved SVR12. In univariate analyses, variables significantly associated with per protocol SVR12 for the entire sample were therapy duration (P = 0.001), treatment experience (P = 0.016), and cirrhosis status (P = 0.001). However, among HCV genotype 1 patients, no variables were significant. Intent-to-treat SVR12 rates were 89% (396/447) for HCV genotype 1 and 91% (21/23) for HCV genotype 4.
Conclusion
Elbasvir-grazoprevir is highly effective, and in this 2016 cohort, its use was predominantly in patients with HCV genotype 1 and as a 12-week therapy without ribavirin.
1 INTRODUCTION
In the United States, approximately 2.7 million persons are chronically infected with hepatitis C virus (HCV),1 which increases the risks of developing cirrhosis and hepatocellular carcinoma.2 Fortunately, successful treatment can lead to regression of hepatic fibrosis and reduces the likelihood of liver-related complications.3 Historically, treatment for HCV was limited to combination therapy with the immunomodulator peginterferon and the broad-spectrum anti-viral ribavirin. Interferon and ribavirin combination regimens were long in duration, difficult to administer, poorly tolerated and frequently ineffective. The recent advent of targeted anti-virals to HCV has dramatically changed the treatment landscape, providing options for shorter, simpler and better-tolerated regimens with high likelihood of cure.4 However, the initial direct-acting anti-viral (DAA) regimens were not approved in certain patient subpopulations, such as those with advanced kidney disease. Patients with renal dysfunction have a higher prevalence of HCV than the general population (9.5% vs 1.6%),5 and HCV-infected patients on hemodialysis have a higher risk of mortality vs uninfected patients.6, 7
In January of 2016, the US Food and Drug Administration approved the fixed-dose, once-daily combination of elbasvir, an NS5A inhibitor, and grazoprevir, an NS3/4A protease inhibitor, for treating chronic HCV genotype 1 or 4 infection in adults.8, 9 In clinical trials, elbasvir-grazoprevir with or without ribavirin for 12 or 16 weeks has shown high rates of sustained virological response (SVR) in treatment-naïve or -experienced patients and has demonstrated a favourable safety profile.10-14 Elbasvir-grazoprevir is metabolized in the liver vs the kidneys, and it was the first DAA regimen recommended by the American Association for the Study of Liver Diseases for treating patients with HCV genotypes 1a, 1b, or 4 and severe renal impairment (eGFR < 30 mL/min) or end-stage renal disease.4, 15
Efficacy of a treatment in clinical studies can be different from effectiveness in clinical practice, and analyses of elbasvir-grazoprevir use in real-world practice settings are lacking. To determine the types of patients treated with elbasvir-grazoprevir, compare real-world administration of elbasvir-grazoprevir with label recommendations, and capture outcomes of patients with and without renal failure, we conducted a retrospective analysis of hepatitis C patients treated with elbasvir-grazoprevir with or without ribavirin in clinical practice settings in the United States.
2 METHODS
2.1 Data collection
Specialty pharmacies and physicians provided baseline information as well as outcome data on patients' ≥18 years of age that were treated with elbasvir-grazoprevir for genotype 1 or 4 HCV. Though the study population was not intended to be representative of the entire US population, the collected information was broadly distributed geographically across 34 states and the District of Columbia in the US. Data were entered into Trio Health's proprietary Innervation Platform, a portal for managing patient information, by a combination of nightly file feeds and manual user entry. Following input of clinical data, the portal applied proprietary logic to identify errors and prompted users to input missing data. Where mandated by state law, patients signed an electronic informed consent allowing the specialty pharmacies to collect the data. Each clinician and specialty pharmacy enrolled in the portal signed agreements attesting to compliance with all rules and regulations regarding the disclosure of patient information to a shared prescription database. FDA-mandated reporting of deaths and/or adverse events was assumed to be completed at the time of event. The causes and outcomes of individual events were not known. Trio Health Analytics was provided with de-identified, HIPAA-compliant patient information from the platform. This process and the study plan was approved by Western Institutional Review Board as an institutional review board exemption under 45 CFR 46.101(b)(4).
2.2 Retrospective analyses
This retrospective cohort study includes 470 patients treated with elbasvir-grazoprevir between February and December 2016. The primary endpoint was per protocol SVR12, defined as a negative hepatitis C viral load as assessed by PCR at 12 or more weeks following the completion of therapy. Treatment start and end dates were defined by pharmacy dispensing records. Baseline demographic and clinical characteristics that were captured at or prior to the start of therapy include age, gender, race, fibrosis, transplant status, select comorbidities, HIV coinfection, HBV coinfection, prior treatment failure, intended treatment and practice type. Collected laboratory values included HCV genotype, initial viral load, baseline aspartate aminotransferase (AST), alanine aminotransferase (ALT), haemoglobin, serum creatinine and platelets. Fibrosis stage was reported by the prescribing clinicians based on histological or noninvasive estimation. Estimated glomerular filtration rate (eGFR) values were calculated using the CKD-EPI Creatinine equation.16 Patients with eGFR at baseline <90 mL/min were considered to have chronic kidney disease (CKD) Stage 2 or higher, those with ≥90 mL/min were considered CKD Stage 1 if CKD was provider indicated. Academic centres were defined as tertiary care centres or clinics affiliated with academic centres. Any other practice (solo or group) was characterized as a community site.
Statistical analyses were performed using spss 24. Univariate analyses examining association of different variables with SVR12 were assessed on the per protocol population receiving any elbasvir-grazoprevir regimen/schedule. The evaluated variables included treatment characteristics (±ribavirin, 12 vs 16 week), baseline labs (haemoglobin, platelets, viral load, eGFR), patient gender, whether the patient had previously received any anti-HCV therapy, cirrhosis status, genotype subtype, practice type, payer type, and the presence of diabetes, hypertension, hyperlipidaemia, anxiety or depression. Univariate comparisons were conducted using chi-squared testing for proportions, Student t testing for continuous variables with normal distributions, or Wilcoxon rank-sums testing for non-Gaussian continuous variables. Significant P values were 2-tailed and <0.05.
3 RESULTS
3.1 Patient population
Among the population of treated patients, 63% (298/470) were male, and the median age was 59 years (range 26 to 88 years) (Table 1). Ninety-five percent of patients had HCV genotype 1 infection, 80% (373/468) were HCV treatment naïve and 70% (327/468) had non-cirrhotic disease. Fibrosis stage was recorded by the physician as part of the medication approval process, as is usual in the US, and was determined by non-invasive biomarkers, elastography and liver biopsy. The physician-reported scores were evaluated by APRI, and the mean (SD) APRI scores were F0-2, 0.54 (0.64) n = 158; F3, 0.85 (0.6) n = 64; and F4, 1.61 (1.95) n = 111. For patients who were indicated as non-cirrhotic by the physician but lacked a reported fibrosis stage, the mean (SD) APRI score was 1.0 (1.14) n = 68. For 69 patients, APRI score could not be calculated. Approximately 1 quarter (27% [127/470]) of patients received care in academic centres, and the remainder were treated in community practices. Patients were most commonly (64% [303/470]) treated by a provider reporting a gastroenterology specialty. In two-thirds of cases, the primary insurer was Medicare.
Of the study patients with reported measures, 31% (131/413) had severe renal impairment (CKD 4/5), 30% (139/457) had diabetes, and 54% (248/457) had hypertension. Of the 131 patients with severe renal impairment, 105 had CKD Stage 5 and of those, 74/105 (70%) were on dialysis. Sixty-nine percent of HCV genotype 1a patients (202/293) had NS5A resistance testing at baseline, with 12% (24/202) having an NS5A resistance mutation at 1 or more positions of interest (28, 30, 31 or 93).
3.2 Virological response
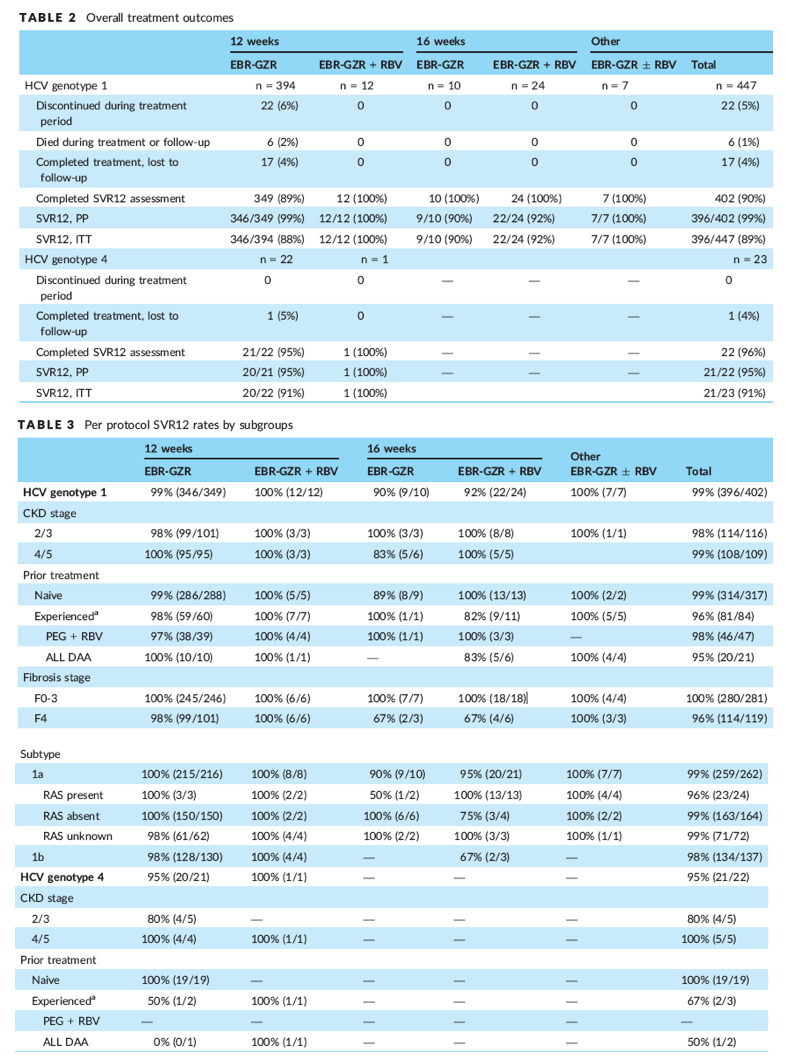
The majority (89%) of patients received elbasvir-grazoprevir for 12 weeks (Table 2). Among patients with HCV genotype 1, SVR12 rates were 99% (396/402) for the per protocol population (Table 3) and 89% (396/447) for the intent-to-treat population (Table 4). For patients with HCV genotype 4, SVR12 rates were 95% (21/22) for the per protocol and 91% (21/23) for the intent-to-treat populations. Patients with CKD Stages 4 or 5 had high rates of SVR12: 99% (108/109) for HCV genotype 1 patients and 100% (5/5) for HCV genotype 4 patients (Table 3). The SVR12 rates were 96% (114/119) in HCV genotype 1 patients with F4 fibrosis and 100% (280/281) for those with F0-F3.
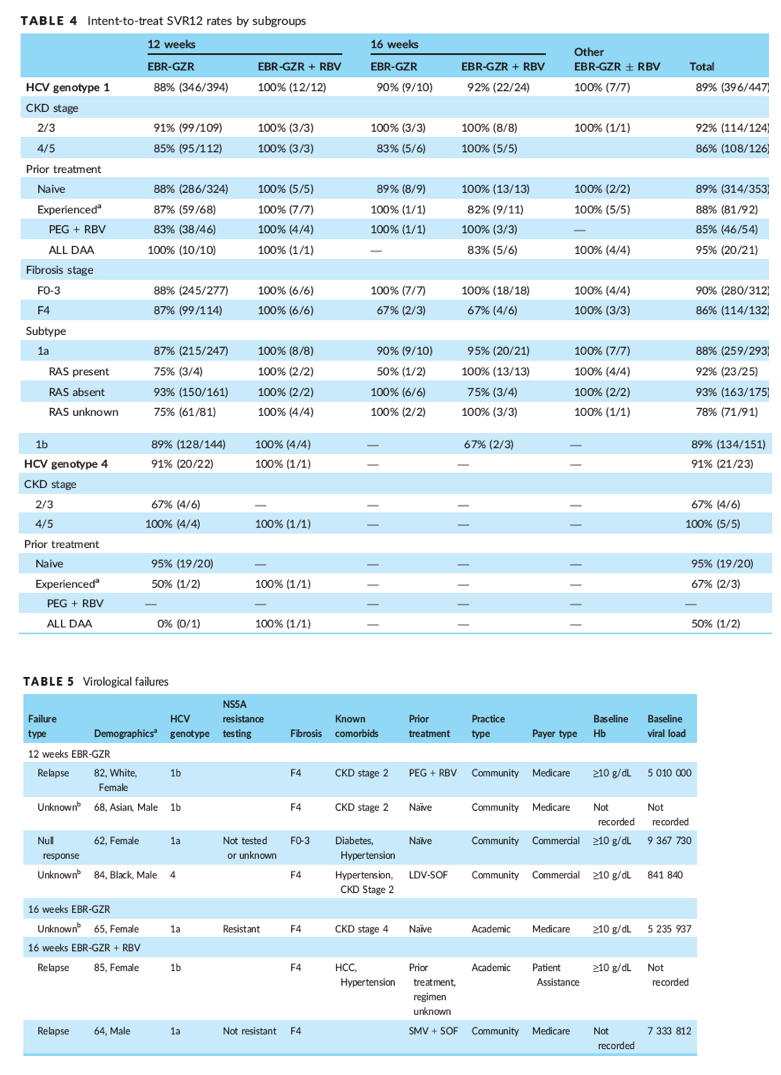
Seven patients who completed treatment did not reach SVR12 and were thus considered virological failures (Table 5). Six of them had comorbid conditions, most commonly CKD and hypertension. However, of the failures, only 1 patient had severe renal impairment (CKD Stage 4). Of the 3 failures with HCV genotype 1a, 1 patient was identified as having a baseline NS5A RAS. None of the patients with virological failure had reported anxiety, depression, HBV or HIV coinfection, or hyperlipidaemia, and none had received a liver transplant.
3.3 Discontinuations
Based on information reported by physicians and pharmacies, 22 patients discontinued treatment; all had HCV genotype 1 infection and were receiving 12 weeks of elbasvir-grazoprevir (Table 6). The most common reason for discontinuation was patient noncompliance (n = 11), followed by insurance-related issues (n = 3), medical follow-up or hospitalization unrelated to treatment (n = 3), and side effects (n = 2). For 3 patients, no reason for discontinuation was specified. None of the patients who discontinued had HBV coinfection.
Eighteen patients did not complete post-treatment follow-up visits. Again, all had HCV genotype 1 infection and were receiving 12 weeks of elbasvir-grazoprevir. None of these patients was post-liver transplant or had HBV coinfection.
3.4 Safety
Six patients died during treatment or follow-up (Table 7). All were HCV genotype 1, and 3 had Stage 5 CKD. None of the patients who died were post-liver transplant or had HBV or HIV coinfection. Causes of death were not available.
3.5 Off-label administration
A total of 8 different elbasvir-grazoprevir-based regimens were administered. Seven patients received a regimen that is not listed in the US FDA labelling for elbasvir-grazoprevir: 3 patients received 12 weeks of elbasvir-grazoprevir plus sofosbuvir and ribavirin, 2 received 16 weeks of elbasvir-grazoprevir plus sofosbuvir and ribavirin, 1 received 20 weeks of elbasvir-grazoprevir, and 1 received 20 weeks of elbasvir-grazoprevir plus ribavirin. Twenty-three patients had a history of treatment with an all-oral, direct-acting antiviral regimen, although elbasvir-grazoprevir is not indicated for such patients.
3.5.1 Baseline resistance and prior NS5A exposure
Among patients with HCV genotype 1a, 31% were reported as either not tested for RASs or of unknown testing status. Per labelling recommendations, HCV genotype 1a patients with NS5A RASs should receive elbasvir-grazoprevir plus ribavirin for 16 weeks; therefore, patients without resistance testing are at risk for receiving a shorter regimen without ribavirin.
In this cohort, multiple patients with a baseline RAS or prior exposure to an HCV NS5A protease inhibitor were administered elbasvir-grazoprevir for 12 weeks, even though US FDA labelling recommends a longer regimen and one with ribavirin. In such cases, treatment response rates remained high. Four patients with HCV genotype 1 who failed prior HCV therapy with a protease inhibitor achieved SVR12 with elbasvir-grazoprevir for 12 weeks, even though addition of ribavirin is recommended. Eleven HCV genotype 1a patients with a baseline NS5A RAS received a regimen other than the recommendation (16 weeks elbasvir-grazoprevir plus ribavirin), and 91% (10/11) achieved SVR12. Three patients with HCV genotype 4 patients who were treatment experienced did not receive the recommended 16 weeks of elbasvir-grazoprevir plus ribavirin, and 2 (66%) achieved SVR12.
3.6 Assessment of variable association with per protocol SVR12
In univariate analyses, variables significantly associated with SVR12 across the entire sample were therapy duration (12 weeks vs 16 weeks, P = 0.001), treatment experience (naïve vs experienced, P = 0.016), and cirrhotic status (F0-3 vs F4, P = 0.001) (Figure 1).
In univariate analyses of the population of patients who were HCV genotype 1 and received elbasvir-grazoprevir for 12 weeks (n = 349), no variables were significantly associated with SVR12 (Table S1).
4 DISCUSSION
In this analysis of HCV treatment in clinical practice settings, response rates to elbasvir-grazoprevir with or without ribavirin were high. Per protocol SVR12 rates were 99% for patients with HCV genotype 1 and 95% for those with HCV genotype 4. These rates are similar to those reported in clinical trials of elbasvir-grazoprevir.10-14 In our study population, there were considerable numbers of patients with CKD and related co-morbidities. Almost all patients had at least grade 2 CKD and although we do not know which of the many variables went into treatment choice, there was a clear prevalence of the use of ELB/GRZ in this population. One quarter of patients had Stage 4 or 5 CKD, 30% had diabetes and 54% had hypertension. Among the patients with Stage 4 or 5 CKD, 99% achieved SVR12.
In our cohort, patients were most commonly HCV treatment naïve with mild or no fibrosis, and they more often received treatment in community vs academic practice settings.
Fibrosis assessment was assessed as clinically reported by the physician when they applied for treatment. We analysed APRI scores in evaluable patients, and overall 109 of 401 had severe fibrosis as defined by an APRI > 1.0. It is likely that trends in the broader HCV treatment environment are shifting, and patients who had more advanced disease accounted for a higher percentage of those treated in the early years of direct-acting anti-viral therapy, while more recently the percentage of patients with milder disease receiving treatment in community settings is increasing. The population was derived from treating physicians including academic and community, multiple specialties and is representative of the current treatment trends in the US.
Of the 470 patients who initiated treatment in our cohort, 46 (10%) did not have SVR12 results, and therefore were not included in the per protocol analysis. The most common reason for not having SVR12 results was not completing follow-up visits. The next most common reason was failure to comply with treatment. In the earlier era of hepatitis C treatment with interferon and ribavirin, discontinuation rates were high in part because of poor tolerability associated with both drugs. All DAA regimens have more favourable side effect profiles than interferon and ribavirin regimens,17 and in our study, only 2 patients discontinued because of adverse events. Yet completion of treatment and follow-up visits remains problematic for some patients, as evidenced by this study and other analyses. In a real-world analysis of patients treated with elbasvir-grazoprevir in the Veterans Affairs healthcare system,18 in which 33% had CKD stages 3-5, the per protocol SVR12 rate was 97%, similar to our per protocol rates, although our study had a higher percentage of patients with CKD stages 3-5 (43%). In the VA study, of 2985 patients who initiated treatment, 549 (18%) did not have available SVR12 data. In a real-world analysis of ledipasvir-sofosbuvir ± ribavirin, also in the Veterans Affairs healthcare system, 5.6% of patients receiving ledipasvir-sofosbuvir did not complete treatment.19 Future analyses that more specifically address adherence and reasons for discontinuing treatment or follow-up in the era of all DAA regimens are needed.
In our cohort, the vast majority of patients (89%) received elbasvir-grazoprevir for 12 weeks, although a total of 8 different regimens were administered. Our results suggest that in clinical practice settings, elbasvir-grazoprevir is predominantly administered for 12 weeks without ribavirin, even in the presence of a baseline NS5A RAS or history of previous usage of a protease inhibitor, and that baseline resistance testing for HCV genotype 1a patients is not universally performed. Although the SVR rate was high with nonrecommended regimens, it remains important to educate providers regarding the appropriate usage of the therapy and the need for baseline resistance testing in HCV genotype 1a patients. Educating practitioners in community settings should be a priority.
One limitation of our study is the reliance on practitioners and pharmacists to capture and report data, and therefore data capture was incomplete. For example, in some cases, treatment history or baseline resistance testing were unknown or unreported. Therefore, we do not fully know how many patients received therapy recommended by the label and how many did not.
In summary, the results of our analysis indicate that elbasvir-grazoprevir is highly effective in real-world settings for treating patients with HCV genotypes 1 or 4. In this cohort from 2016, its use was predominantly as a 12-week therapy without ribavirin.
| |
| |
| |
|
|
|