 |
 |
 |
| |
Integrase inhibitors dolutegravir and raltegravir exert proadipogenic and profibrotic effects and induce insulin resistance in adipose tissue and adipocytes
|
| |
| |
21st Intl Co-morbidties & Adverse Drug Reactions Worksop
Basel, Switzerland, 5-6 November 2019
J Gorwood1, C Bourgeois2, V Pourcher3, F Charlotte3, G Pourcher4, M Mantecon1, C Rose1, R Morichon1, R Le Grand2, C Katlama3,5, B Fève1,6, O Lambotte2,7,
J Capeau1, V Bereziat1*, C Lagathu1*
*Both authors contributed equally to this work
1Sorbonne Universite, Inserm UMR_S 938, Centre de Recherche Saint-Antoine, ICAN, Paris, France; 2CEA, Universite Paris Sud,
Inserm U1184, ImVA, IDMIT, Fontenay-aux-Roses, France; 3AP-HP, Sorbonne Universite, Hôpital Pitie-Salpêtrière, Service de maladies infectieuses et tropicales, INSERM U1136, Institut Pierre Louis d’epidemiologie et de Sante publique et d’Anatomo- Pathologie, Paris, France; 4Institut Mutualiste Montsouris, Service de Chirurgie Digestive, Paris, France; 5Sorbonne Universite, Inserm, Institut Pierre Louis d’epidemiologie et de Sante Publique, Paris,
France; 6AP-HP, Hôpital Saint-Antoine, Service d’endocrinologie, Paris, France; 7APHP, Hôpital Bicêtre, Service de Medecine Interne et Immunologie Clinique, Kremlin-Bicêtre, France
program abstract
Objectives: There is growing evidence that integrase inhibitors (INSTI) dolutegravir and raltegravir promote peripheral and central adipose tissue/weight gain in
HIV-infected individuals, but the mechanisms involved remain unknown. We aimed to assess the effect of these molecules on adipose tissue morphology, function and metabolism.
Methods: Morphology and function of subcutaneous (SCAT) and visceral adipose tissue (VAT) were studied in: HIV-infected patients from the ObeVIH study, at the time of bariatric surgery (BMI 41.8 kg/m2): 14 patients received INSTI (10 dolutegravir, 2 raltegravir, 2 elvitegravir) and 5 an INSTI-sparing regimen; and uninfected cynomolgus macaques treated or not 15 days with dolutegravir/tenofovir/emtricitabine. Human adipose stem cells (ASCs) were chronically treated with dolutegravir or raltegravir before or during adipogenesis. Adipogenic capacities, insulin response and extracellular matrix component expression were analysed.
Results: SCAT from the ObeVIH patients presented peri-lobular and peri-adipocyte fibrosis in most samples. Conversely, VAT of INSTI-treated patient presented
a higher level of peri-adipocyte fibrosis than that of non-INSTI-treated patients.
Dolutegravir-treated macaques presented a higher level of fibrosis and an increased adipocyte size in both SCAT and VAT, when compared with untreated macaques. Adipogenic marker expression was increased in SCAT and VAT, whereas adiponectin expression was decreased in
SCAT, suggesting that, despite a pro-adipogenic effect, dolutegravir may favour insulin resistance. In ASCs, INSTI-treatment increased collagen 1 and 6
and a-smooth-muscle-actin expression indicating a pro-fibrotic effect. In ASC-differentiated adipocytes, dolutegravir, and to a lesser extent raltegravir, increased
lipid accumulation and adipogenic marker expression, decreased adiponectin expression and induced insulin resistance.
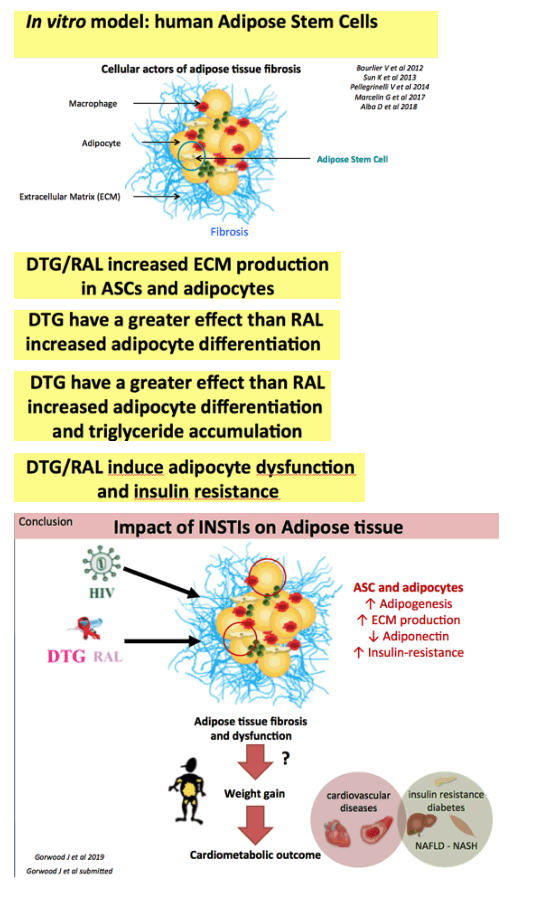
Conclusions: We demonstrate here for the first time, by using in vivo and in vitro complementary models, that INSTI exert a direct impact on adipose tissue adipogenesis, fibrosis and insulin resistance. These results, which reveal the adipose tissue toxicity of dolutegravir and raltegravir, are important to explain fat modifications reported in INSTI-treated HIV-infected patients.
|
| |
|
 |
 |
|
|