 |
 |
 |
| |
HIV tied to almost 2-fold lower breast cancer survival
|
| |
| |
Conference on Retroviruses and Opportunistic Infections (CROI), March 4-7, 2019, Seattle
Mark Mascolini
WEBCAST: http://www.croiwebcasts.org/console/player/41049?mediaType=slideVideo&&crd_fl=0&ssmsrq=1554044559378&ctms=5000&csmsrq=5062
A prospective cohort study in Botswana linked HIV infection to nearly 2-fold lower survival with breast cancer despite ready availability of antiretroviral therapy (ART) [1] and cancer treatment. The disparity between HIV-positive and negative women could not be explained by age, income, cancer stage, or cancer subtype.
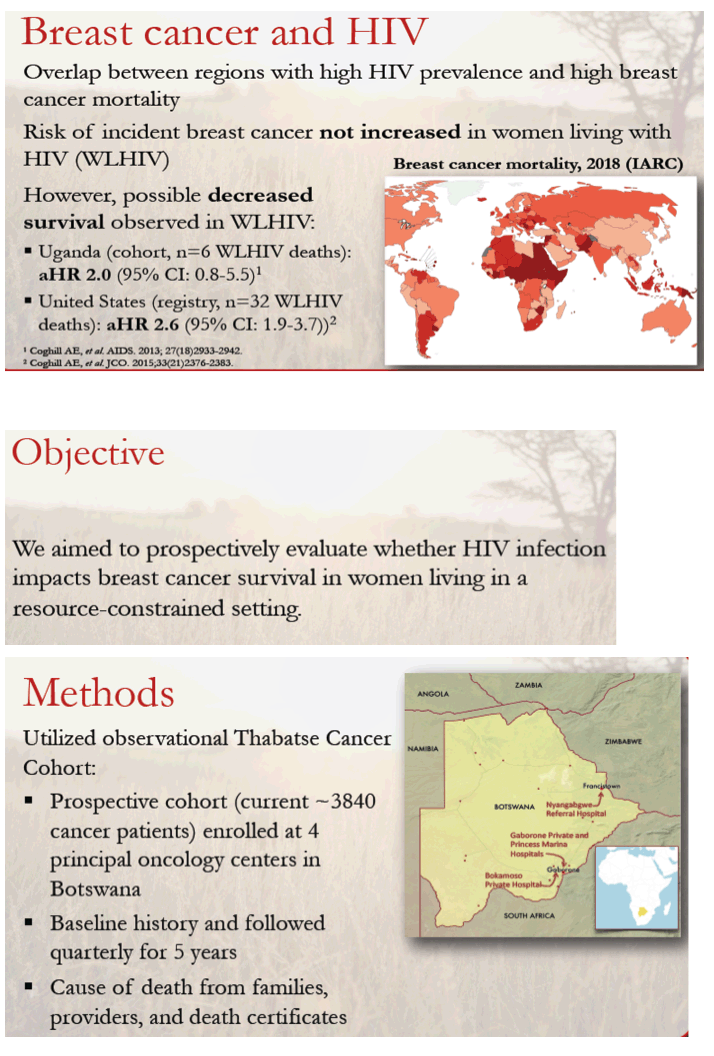
Researchers from the Botswana Harvard AIDS Institute Partnership and collaborators at other centers underlined the global overlap between HIV prevalence and high breast cancer mortality. Although breast cancer incidence is not elevated in women with HIV, breast cancer mortality proved twice higher with HIV in Uganda [2] and the United States [3].
The investigators assessed breast cancer survival in women with and without HIV by analyzing data from the observational Thabatse Cancer Cohort, which now includes more than 3800 cancer patients at 4 centers in Botswana. Causes of death are gleaned from families, providers, and death certificates. HIV therapy and cancer treatment are free in Botswana.
Participants in this analysis were female adult Botswana citizens with known HIV status who began care between October 2010 and September 2018. The researchers used Kaplan-Meier analysis to estimate survival. Cox proportional hazards models estimated overall survival after adjustment for cancer stage, tumor receptor status, age (under 45 versus older), and personal income (under $50 a month versus more).
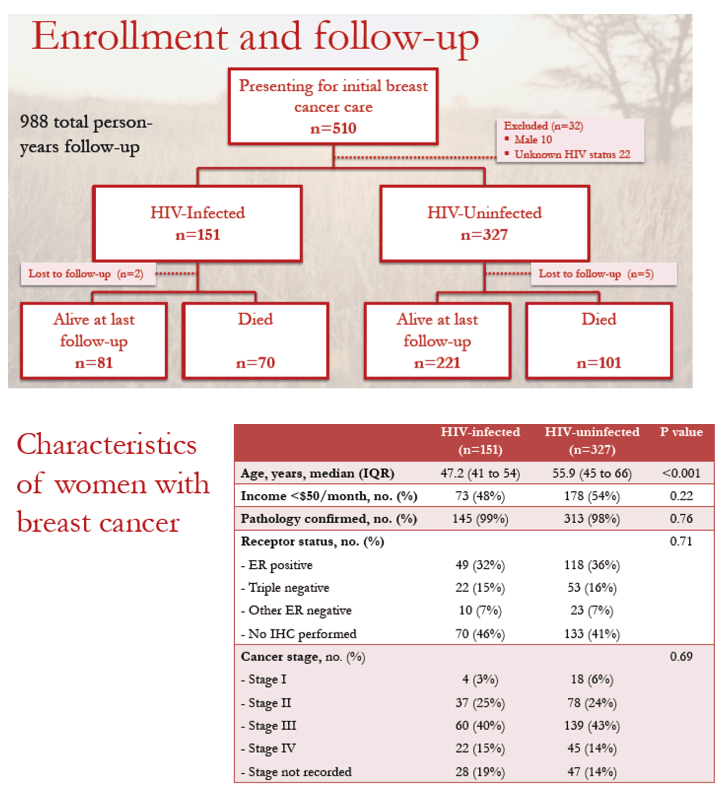
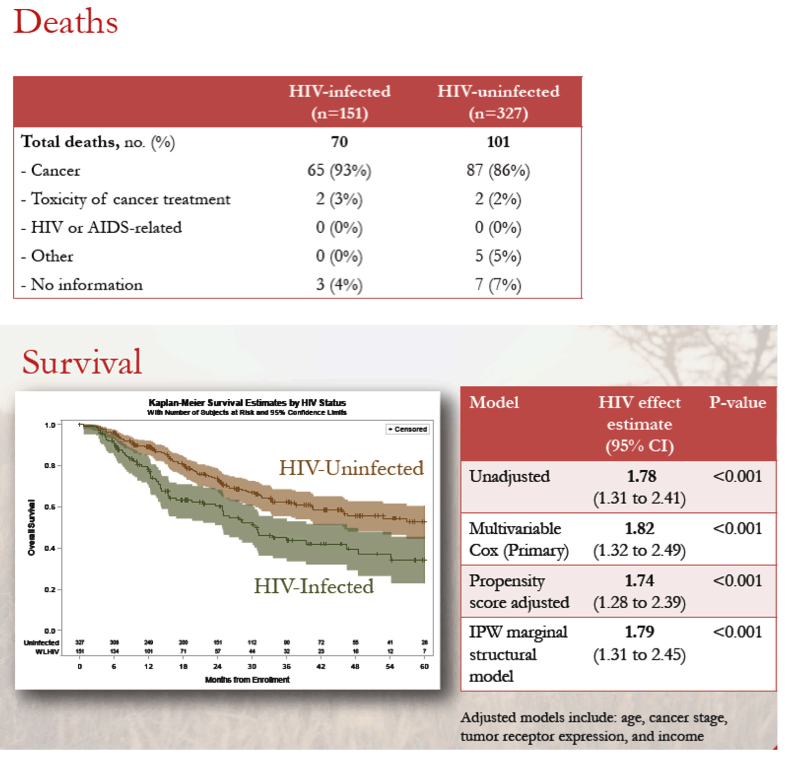
The analysis focused on 151 breast cancer patients with HIV, 70 of whom (46%) died during follow-up, and 327 breast cancer patients without HIV, 101 of whom (31%) died. Among women who died, cancer explained the deaths of 93% of the HIV group a 86% of the non-HIV group. Cancer treatment toxicity accounted for 3% and 2% of deaths in these groups.
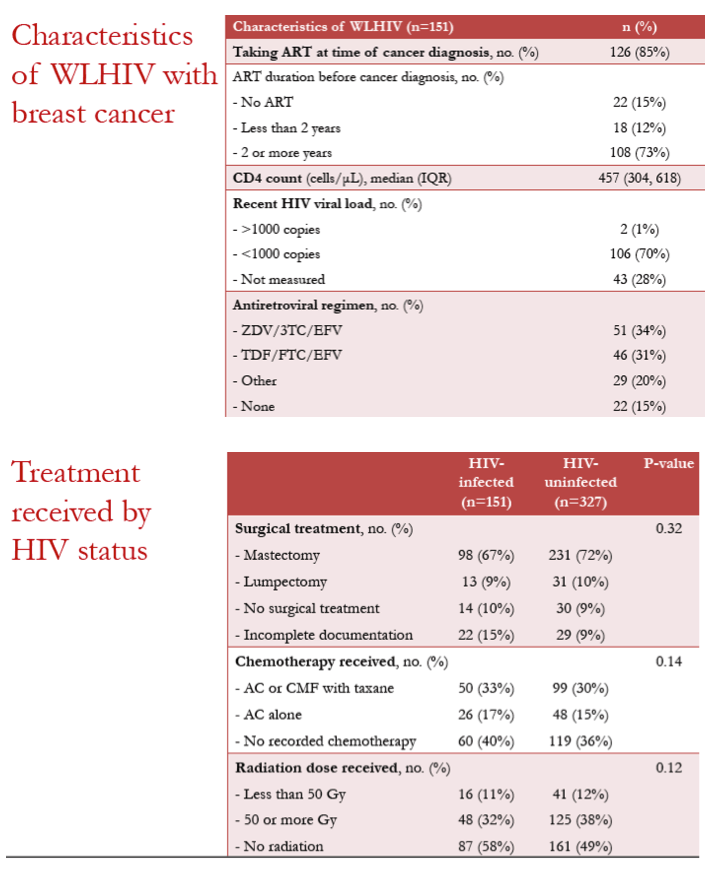
The 151 women with HIV were younger than the 327 without HIV (median 47.2 versus 55.9, P < 0.001), but they did not differ significantly in income, tumor receptor status, or cancer stage (15% and 14% stage 4, 40% and 43% stage 3). Most women with HIV (85%) were taking ART at breast cancer diagnosis, and 73% had taken ART for at least 2 years. HIV load lay below 1000 copies in 70% of women with HIV and had not been measured in 28%.
Women with HIV did not differ significantly from the HIV-negative group in whether they had surgical treatment, chemotherapy, or radiation therapy, or in types of these therapies.
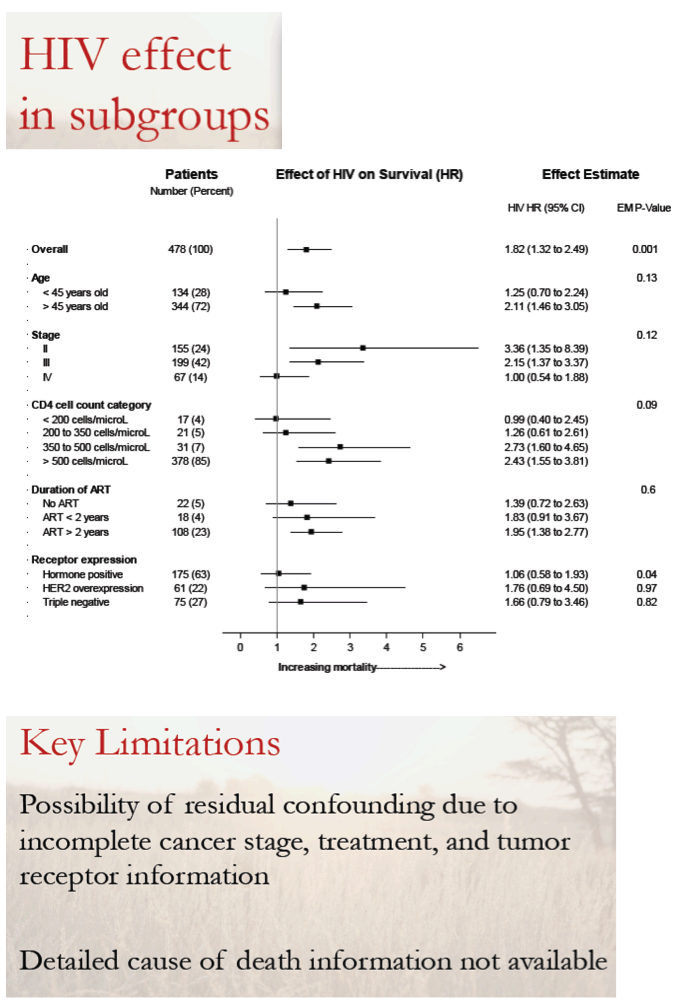
Multivariable Cox analysis adjusted for age, cancer stage, tumor receptor expression, and income linked HIV to almost 2-fold lower survival with breast cancer during follow-up HIV (hazard ratio [HR] 1.82, 95% confidence interval [CI] 1.32 to 2.49, P < 0.001). That estimate did not change substantially in a propensity score-adjusted analysis or an inverse probability weighted marginal structural model.
Further analysis determined that the negative impact of HIV on survival appeared to be worse with older age, earlier cancer stage, higher current CD4 count, and longer ART:
-- Age over 45 vs younger: HR 2.11
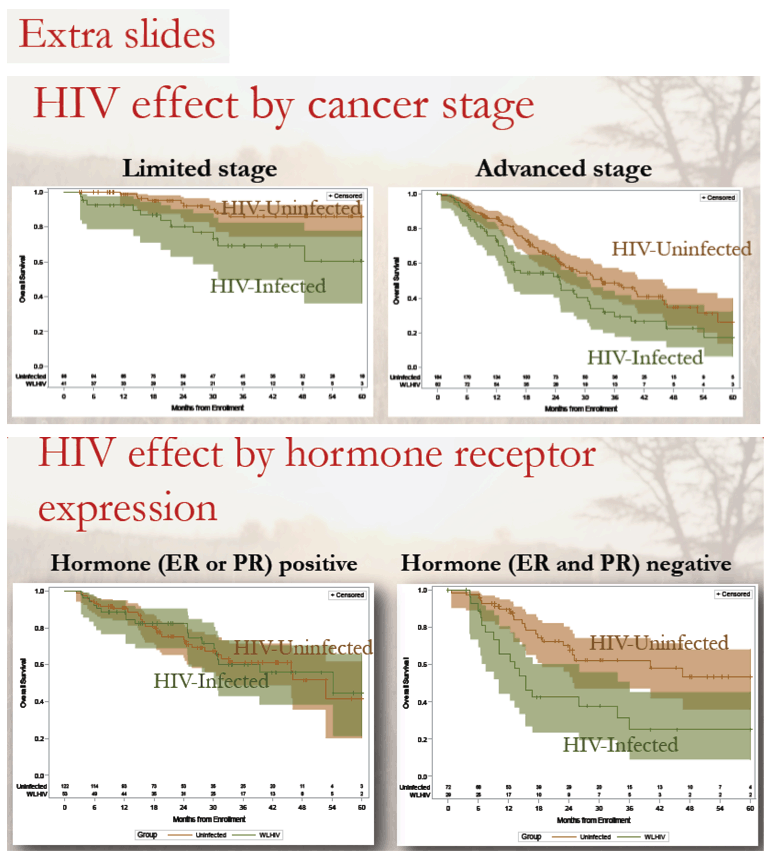
-- Breast cancer stage 2 vs 4: HR 3.36
-- Breast cancer stage 3 vs 4: HR 2.15
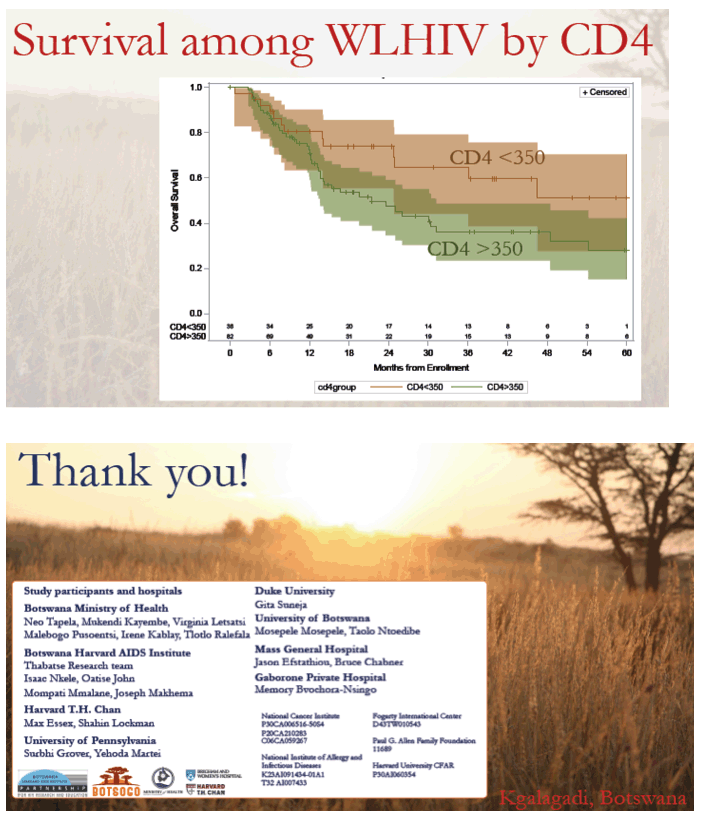
-- 350 to 500 CD4s: HR 2.73
-- 500 or more CD4s: HR 2.43
-- More than 2 years of ART: HR 1.95
The primary multivariable analysis, the researchers stressed, shows that lower breast cancer survival with HIV cannot be attributed to worse cancer stage or subtype. They noted that poor overall survival with or without HIV underlines the need for strategies to speed breast cancer diagnosis and care.
References
1. Sadigh KS, Hodgeman RM, Tapela N, et al. HIV is associated with decreased breast cancer survival: a prospective cohort study. Conference on Retroviruses and Opportunistic Infections (CROI). March 4-7, 2019. Seattle. Abstract 16.
2. Coghill AE, Newcomb PA, Madeleine MM, et al. Contribution of HIV infection to mortality among cancer patients in Uganda. AIDS. 2013;27:2933-2942.
3. Coghill AE, Shiels MS, Suneja G, Engels EA. Elevated cancer-specific mortality among HIV-infected patients in the United States. J Clin Oncol. 2015;33:2376-2383.


|
| |
|
 |
 |
|
|