 |
 |
 |
| |
EFFECT ON PLASMA NFL, A MARKER OF NEURONAL INJURY,
AFTER SWITCHING FROM TDF TO TAF
|
| |
| |
from Jules: of note in this presentation increased creatinine was found to be associated with increased NFL suggesting and in line with I think previous research that decreased renal/kidney function as evidenced by increasing creatinine may be associated with worsening cognitive impairment. The question for me is WHY, is it due strictly to decreasing kidney function causing retention of bad proteins or other things that in turn fact the brain or CNS, or is it a more direct affect of kidney function, I do not know. But this suggests to me a potential contributor to brain or CNS damage in HIV+ that is as far as I know never considered in studies that examine CNS & brain & HAND, cognitive function in HIV+. Should this be looked at in these HIV brain/CNS/cognitive function studies??? In particular the recent studies finding accelerated brain or cognitive impairment in older HIV+, I don’t think they looked at kidney function, so is declining kidney function affecting brain or cognitive decline? We know with aging all people & HIV+ suffer declining kidney function with aging & in HIV+ that decline is worse.
Reported by Jules Levin CROI2019 March 4-7 Seattle
Linn Hermansson1, Richard W. Price2, Aylin Yilmaz1, Staffan Nilsson3, Scott McCallister4, Tariro Makadzange4, Moupali Das4, Henrik Zetterberg1, Kaj Blennow1, Magnus Gisslén1
1Sahlgrenska Academy at the University of Gothenburg, Gothenburg, Sweden,2University of California San Francisco, San Francisco, CA, USA,3Chalmers University of Technology, Gothenburg, Sweden,4Gilead Sciences, Inc, Foster City, CA, USA
ProgramAbstract
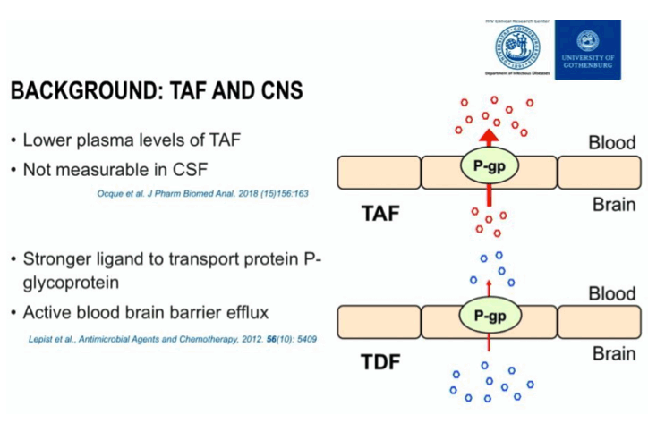
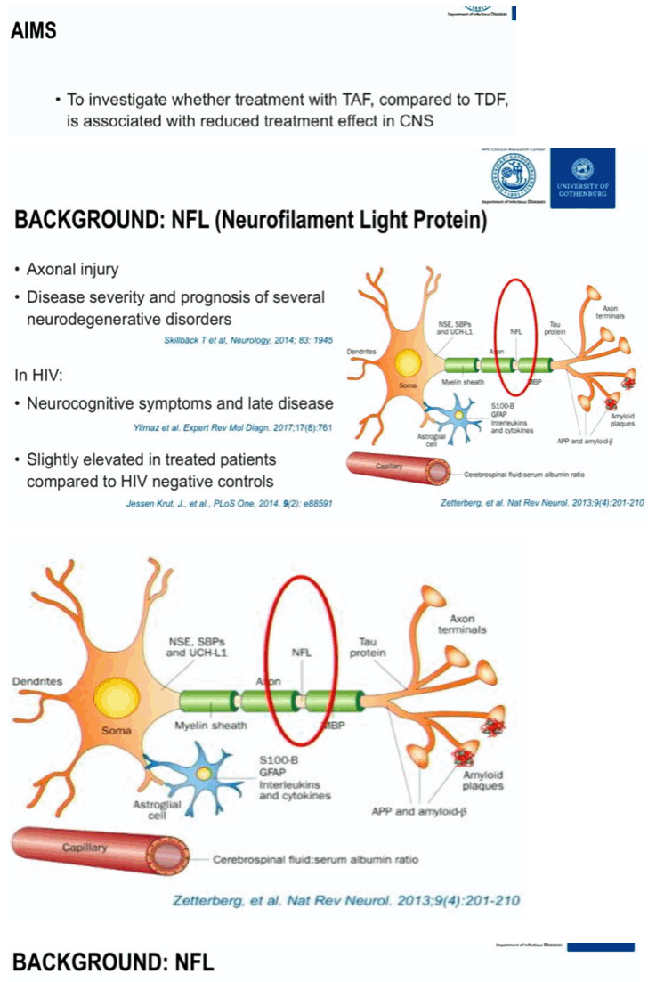
Tenofovir alafenamide (TAF) is associated with significantly lower plasma tenofovir concentrations than tenofovir disoproxil fumarate (TDF), thereby decreasing bone and renal side effects. Limited data are available on TAF pharmacokinetics and effect in the central nervous system (CNS). One concern that has been raised is that because TAF is a stronger substrate for P-glycoprotein (P-gp) than TDF, it could decrease its CNS exposure, since substrates for P-gp are subject to active blood-brain barrier efflux. Plasma neurofilament light protein (NFL) is a sensitive marker of neuronal injury in a variety of neurodegenerative conditions, including neuronal injury in HIV infection. To study whether treatment with TAF is associated with an increased risk of neuronal harm compared to TDF, we compared plasma NFL levels in patients switching from coformulated elvitegravir/cobicistat/emtricitabine/tenofovir disoproxil fumarate (E/C/F/TDF) to E/C/F/TAF with those who continued E/C/F/TDF.
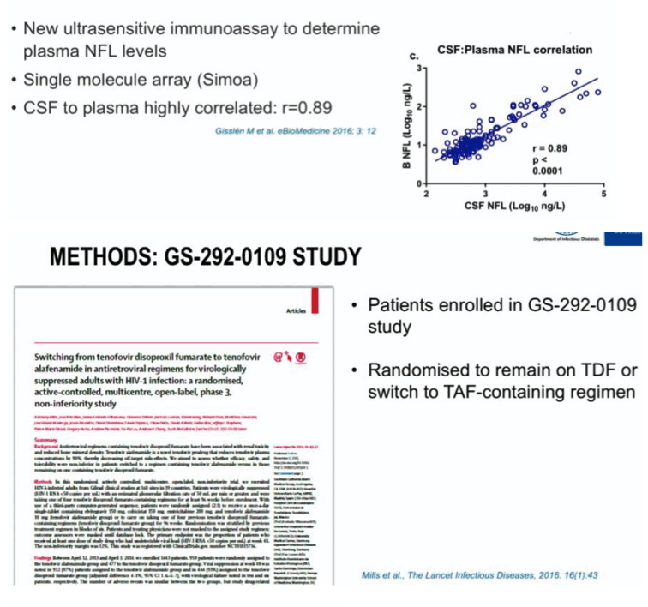
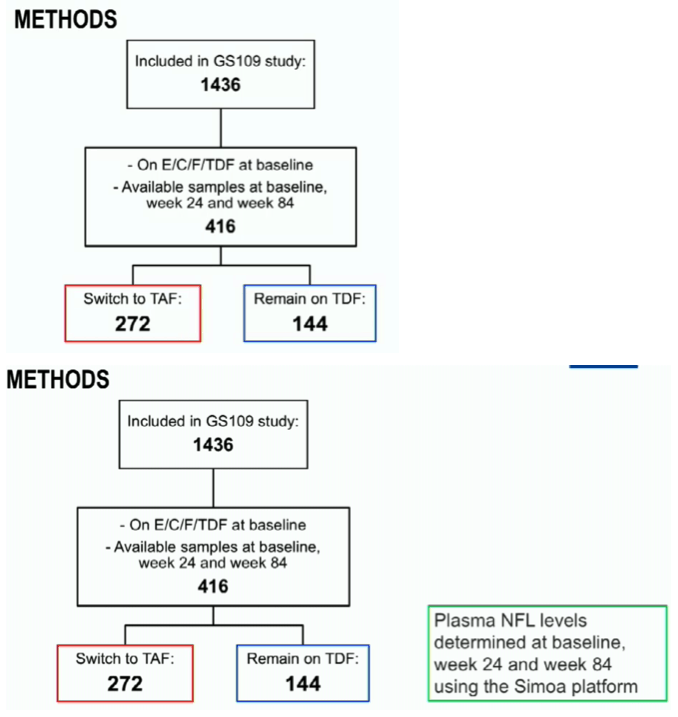
Plasma NFL was analysed at baseline, week 24, and week 84, in stored plasma samples from 414 participants (272 switching to E/C/F/TAF and 142 continuing E/C/F/TDF) enrolled in the randomized, active-controlled, multicenter, open-label, noninferiority Gilead GS-109 trial. For quality control (QC) plasma samples with NFL concentrations of 12.1 pg/mL and 188 pg/mL, intra-assay coefficients of variation (CVs) were 7.8% and 6.7%, respectively.
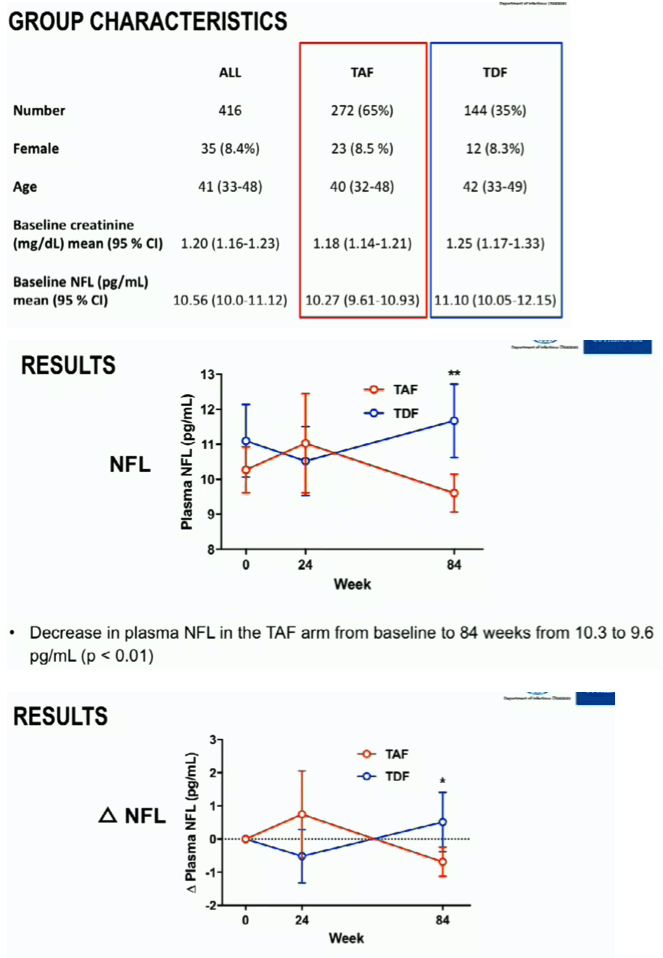
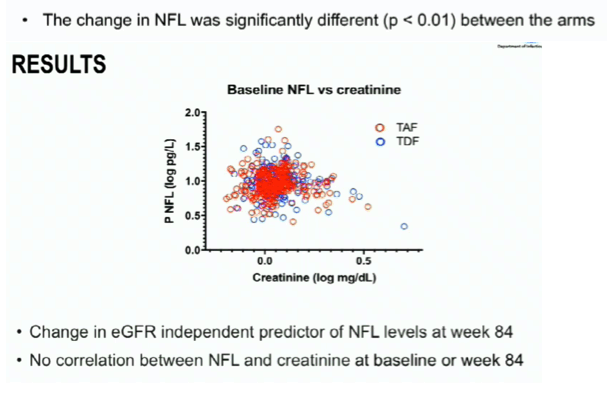
We found a small but statistical significant decrease in plasma NFL in the E/C/F/TAF arm after 84 weeks from 10.3 to 9.6 pg/mL, p<0.01 (Figure). The change was significantly different (p<0.01) from the E/C/F/TDF arm, in which plasma NFL increased from 11.1 to 11.7 pg/mL (ns). As expected, eGFR increased in the E/C/F/TAF arm but not in the E/C/F/TDF arm. Plasma NFL was significantly correlated with age and eGFR. Delta eGFR and treatment group were both found as independent predictors of plasma NFL changes from baseline to week 84 in a multiple linear regression analysis.
We found no evidence of increased risk of CNS injury when switching from TDF to TAF. It should be noted that the NFL levels in both arms were within the limits normally found in HIV-negative controls; it is unclear whether the small decrease in plasma NFL found after switch to TAF is of any clinical significance. This study indicates that switching from TDF to TAF appears safe with regard to neuronal injury.
WEBCAST:
http://www.croiwebcasts.org/console/player/41290?mediaType=slideVideo&&crd_fl=0&ssmsrq=1554037859576&ctms=5000&csmsrq=5072

————————————
Ocque reference:
Development and validation of an LC–MS/MS assay for tenofovir and tenofovir alafenamide in human plasma and cerebrospinal fluid
EXTRACTS
Andrew J. Ocquea,∗, Colleen E. Haglera, Gene D. Morsea, Scott L. Letendreb, Qing MaaaTranslational
A liquid chromatography with triple quadrupole mass spectrometry method was developed and validated for the determination of tenofovir and tenofovir alafenamide concentrations in human plasma and cerebrospinal fluid. The validated methods were applied to the analysis of plasma and cerebrospinal fluid samples of a patient undergoing tenofovir therapy which involved the switch from Stribild® (elvitegravir 150 mg/cobicistat 150 mg/emtricitabine 200 mg/tenofovir disoproxil fumarate 300 mg) to Genvoya® (elvitegravir 150 mg/cobicistat 150 mg/emtricitabine 200 mg/tenofovir alafenamide 10 mg). The therapeutic use of TAF entails remarkably lower dose and therefore lower concentrations of TFV are expected. In this context, the aim of this study was to develop a highly sensitive method to measure TAF and TFV simultaneously in both plasma and CSF matrices. The developed and validated method was used to quantify and compare the concentrations of TFV and TAF in a human study subject when they were taking TDF (week 1) and TAF (week 24). TFV was measureable in plasma at all time points when either Stribild® or Genvoya® was taken. TFV concentrations were 5–20 times lower when Genvoya® was administered. TAF was only present in the plasma with concentrations of 23.5 ng/mL and 4.71 ng/mL at 2 h and 4 h post-dose in the week 24, respectively. TFV was measurable in the CSF at both weeks with 3.03 ng/mL at week 1 and 0.458 ng/mL at week 24. Table 5 shows the concentrations of TFV and TAF measured. TAF was less than 0.1 ng/mL in the CSF at 7 h after a dose of 10 mg TAF. The undetected TAF in the CSF at the 7 h time point was consistent with its rapid metabolism and high intracellular TFV concentrations. The plasma concentrations of TAF and TFV measured in the study subject are comparable to prior reports [19,20]. The present study utilized the PK booster of cobicistat and the concentrations of TAF and TFV may only be best compared to studies with the same medications [30]. To our knowledge, this is the first study to report CNS exposure of TFV from an oral administration of TAF (10 mg) with the combination of elvitegravir, cobicistat, and emtricitabine. This study reports similar TFV concentrations in CSF after TDF (300 mg) oral administration [17,18]. The comparative results of this study further prove the accuracy and usefulness of the LC–MS/MS assay that was developed and validated.
Pdf attached above
------------------------
|
| |
|
 |
 |
|
|