 |
 |
 |
| |
HIV is Associated with Lung Function Impairment in the Multicenter AIDS Cohort Study
|
| |
| |
Reported by Jules Levin
CROI March 2019
Ken M. Kunisaki1,2, Mehdi Nouraie3, Robert Jensen4, Dong Chang5, Gypsyamber D'Souza6, Meghan E. Fitzpatrick3, Meredith C. McCormack7, Valentina Stosor8, Alison Morris3
1: Minneapolis VA Health Care System, Minneapolis/USA, 2: University of Minnesota, Minneapolis/USA, 3: University of Pittsburgh, Pittsburgh/USA, 4: University of Utah, Salt Lake City/USA, 5: LA BioMed, Torrance/USA, 6:
Johns Hopkins Bloomberg School of Public Health, Baltimore/USA, 7: Johns Hopkins University School of Medicine, Baltimore/USA, 8: Northwestern University, Chicago/USA
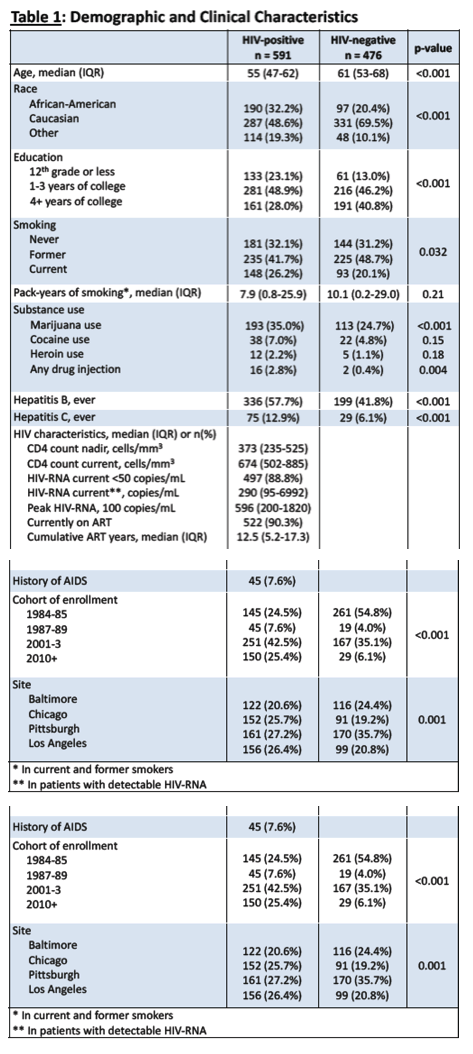
I will note in the baseline demographics Table 1 you will see 32% never smoked !!!!!! Jules

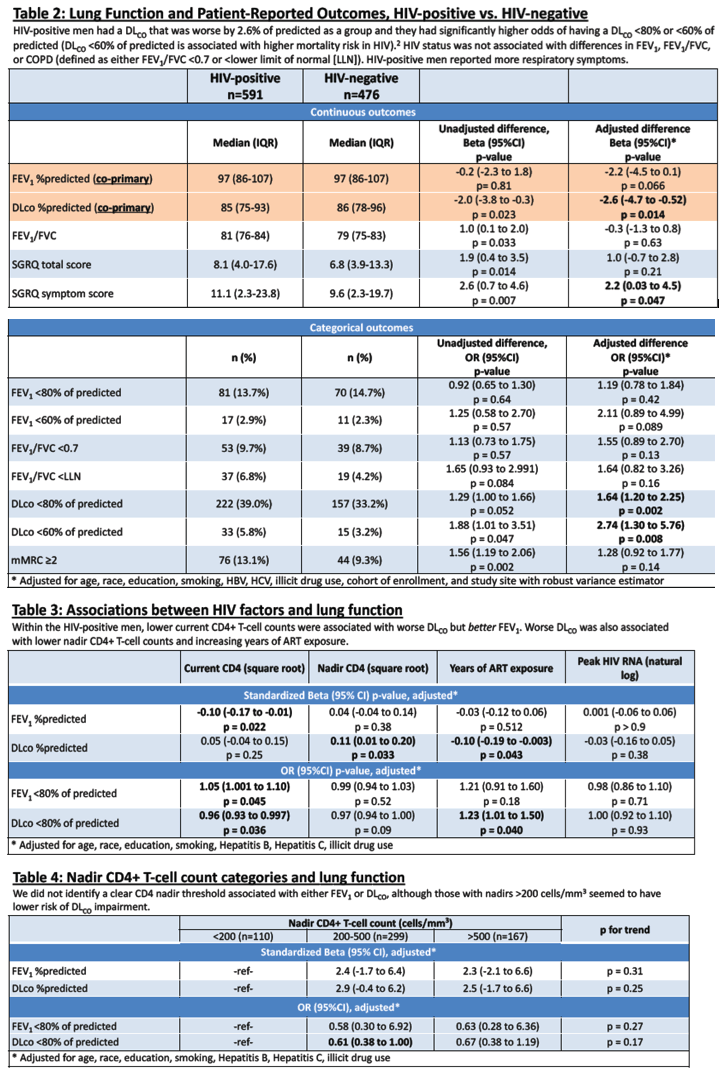
"HIV-positive men had a DLCO that was worse by 2.6% of predicted as a group and they had significantly higher odds of having a DLCO <80% or <60% of predicted (DLCO <60% of predicted is associated with higher mortality risk in HIV).2 HIV status was not associated with differences in FEV1, FEV1/FVC, or COPD (defined as either FEV1/FVC <0.7 or < lower limit of normal [LLN]). HIV-positive men reported more respiratory symptoms.......Within the HIV-positive men, lower current CD4+ T-cell counts were associated with worse DLCO but better FEV1. Worse DLCO was also associated with lower nadir CD4+ T-cell counts and increasing years of ART exposure......We did not identify a clear CD4 nadir threshold associated with either FEV1 or DLCO, although those with nadirs >200 cells/mm3 seemed to have
lower risk of DLCO impairment."
People living with chronic lung diseases, such as chronic obstructive pulmonary disease (COPD), emphysema and pulmonary fibrosis, often have their pulmonary function tested. Many doctors use lung function tests to help diagnose, monitor and treat chronic lung diseases. Lung function tests are also referred to as pulmonary function tests (PFTs). Two important measurements gained from pulmonary function tests are forced expiratory volume in one second (FEV1) and forced vital capacity (FVC). To help you better understand FEV1 and FVC, we've put together the important facts about what these measurements mean for you. https://lunginstitute.com/blog/fev1-and-fvc/
Diffusing capacity of the lungs for carbon monoxide (DLCO) is a medical test that determines how much oxygen travels from the alveoli of the lungs to the blood stream. Learn what DLCO is, how DLCO a good measure of lung disease severity, and why we use carbon monoxide instead of oxygen or carbon dioxide.
FEV1 is the maximal amount of air you can forcefully exhale in one second. It is then converted to a percentage of normal. For example, your FEV1 may be 80% of predicted based on your height, weight, and race. FEV1 is a marker for the degree of obstruction with your asthma: FEV1 greater 80% of predicted= normal.
Forced expiratory volume in 1 second (FEV1) FEV1 is the volume of air that can forcibly be blown out in first 1 second, after full inspiration. Average values for FEV1 in healthy people depend mainly on sex and age, according to the diagram. Values of between 80% and 120% of the average value are considered normal.
DLCO or TLCO (diffusing capacity or transfer factor of the lung for carbon monoxide (CO),[1]) is the extent to which oxygen passes from the air sacs of the lungs into the blood. Commonly, it refers to the test used to determine this parameter. It was introduced in 1909.[2] A DLCO of less than 60% predicted portends a poor prognosis for lung cancer resection. https://en.wikipedia.org/wiki/DLCO
Overlooking a reduced Dlco can delay early diagnosis and treatment of a disease. For example, Dlco is low in chronic obstructive pulmonary disease (COPD) with emphysema, or amiodarone lung toxicity, and it is even lower in ILD with PAH. While Dlco serves as a surrogate marker of the available lung surface area and its properties that enable diffusion to take place, blood in the capillaries—or more accurately, unbound hemoglobin—is the essential driver in the diffusion of CO from the alveolar air across the alveolar-capillary membrane barrier into hemoglobin in red blood cells. Remember, blood in the airways also can bind CO, hence Dlco can rise with hemoptysis and pulmonary hemorrhage. Variability in how Dlco is reported is a concern.
https://www.consultant360.com/articles/using-and-interpreting-carbon-monoxide-diffusing-capacity-dlco-correctly




|
| |
|
 |
 |
|
|