 |
 |
 |
| |
MECHANISMS OF WHITE-MATTER LOSS DUE TO HIV INFECTION AND ANTIRETROVIRAL THERAPY
|
| |
| |
Reported by Jules Levin
CROI 2019
Poster pdf attached
Download the PDF here
Kelly L. Jordan-Sciutto1, Lindsay M. Roth1, Bassam N. Zidane1, Micah Romer2, Cagla Akay-Espinoza1, Judith B. Grinspan2
1University of Pennsylvania, Philadelphia, PA, USA,2Children's Hospital of Philadelphia, Philadelphia, PA, USA
Abstract:
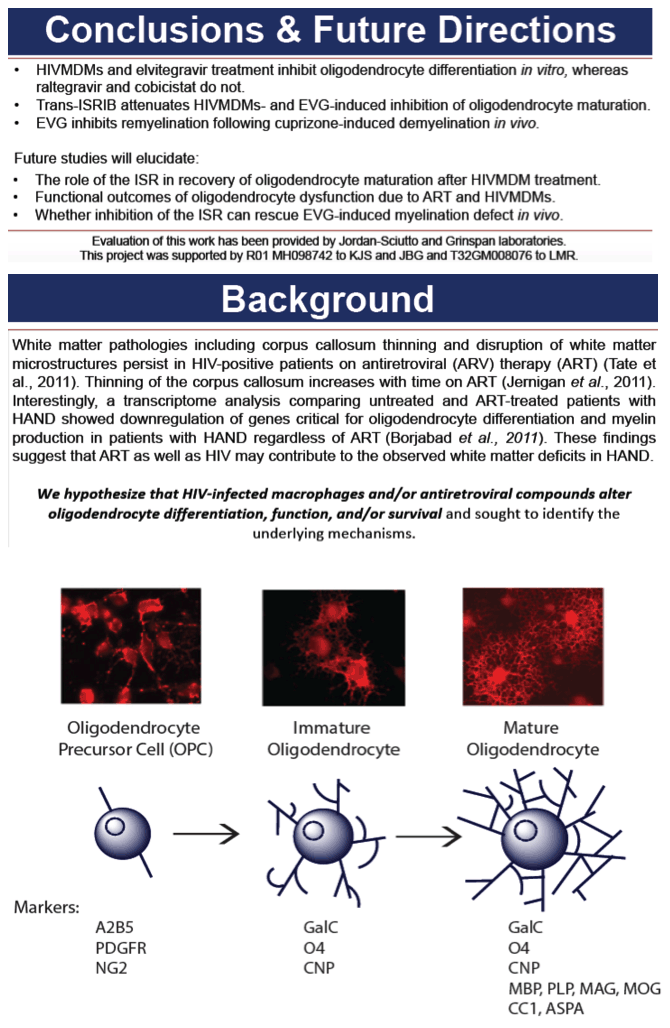
White matter pathologies including corpus callosum thinning and disruption of white matter microstructures persist in HIV-positive patients on combination antiretroviral (ARV) therapy (cART). Thinning of the corpus callosum increases with time on cART. Thus, we hypothesized that HIV-infected macrophages and/or antiretroviral compounds alter oligodendrocyte differentiation, function, and/or survival and sought to identify the mechanism underlying this effect.
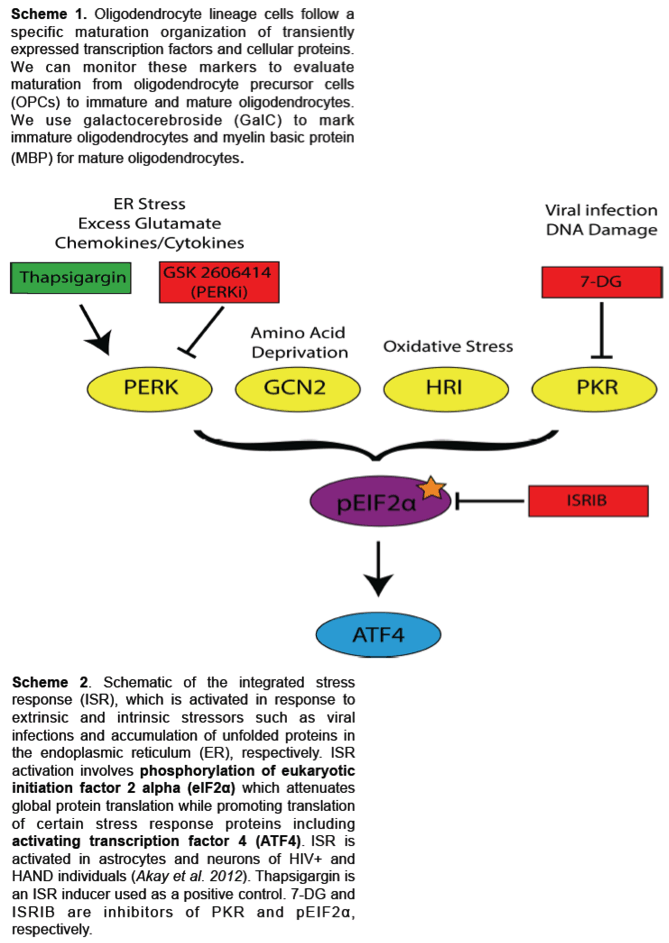
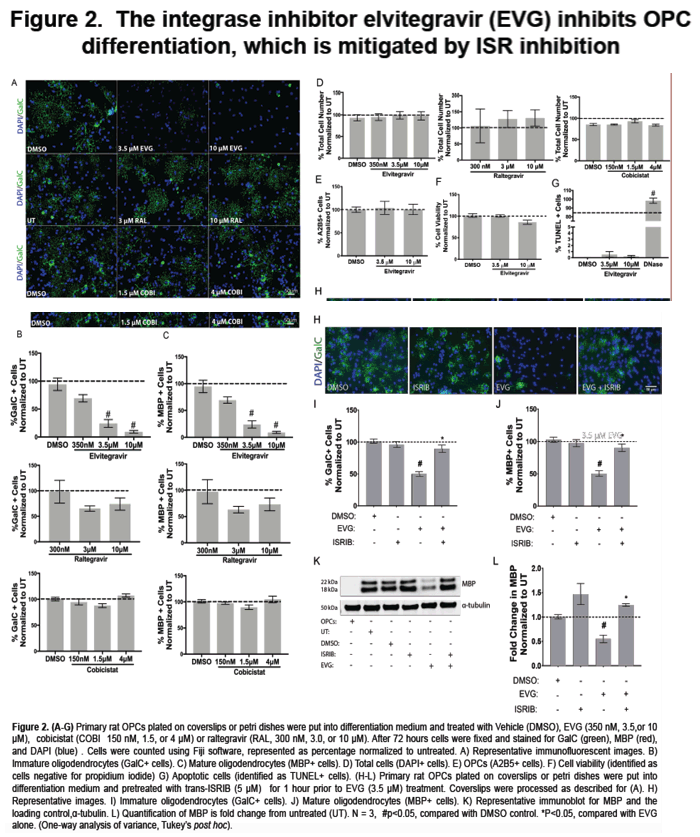
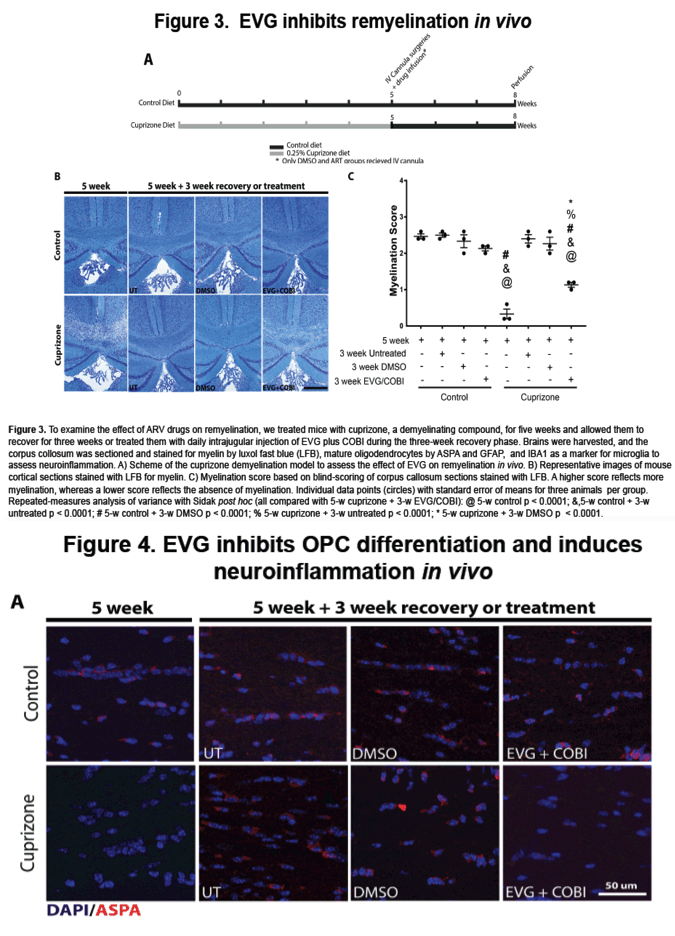
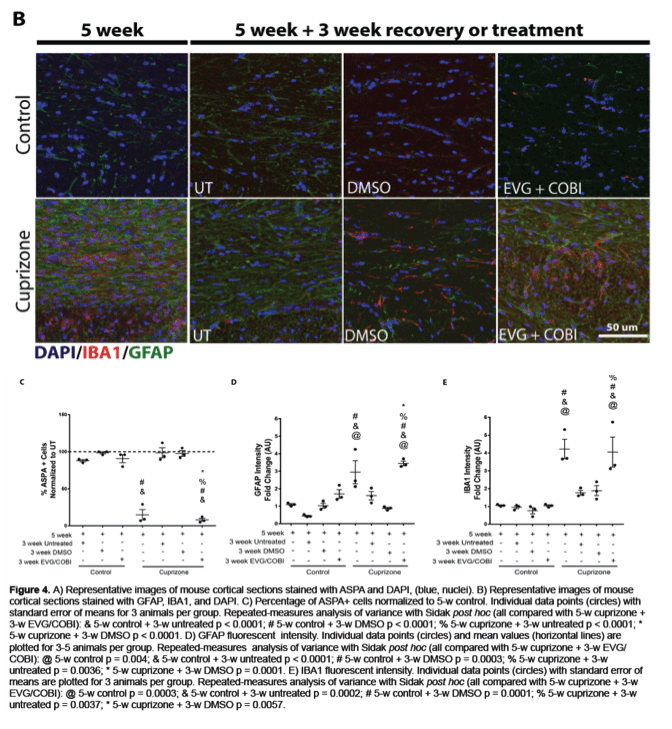
To model the effect of HIV infection in the CNS on oligodendrocytes, we stimulated primary rat oligodendrocyte precursor cells (OPCs) to differentiate into mature oligodendrocytes in vitro, with concomitant treatment with HIV-infected monocyte-derived macrophage supernatant (HIVMDMS) or ARV compounds from the integrase strand transfer inhibitor class, elvitegravir, raltegravir or cobicistat, the bioavailability boost. To examine the effect of ARV drugs on remyelination, we treated mice with cuprizone, a demyelinating compound, for five weeks and allowed them to recover for three weeks (a time frame that permits remyelination) or treated them with daily intrajugular injection of elvitegravir and cobicistat during the three-week recovery phase. Brains were harvested, and the corpus collosum was sectioned and stained for myelin by luxol fast blue, mature oligodendrocytes by ASPA and neuroinflammation by GFAP and Iba1.
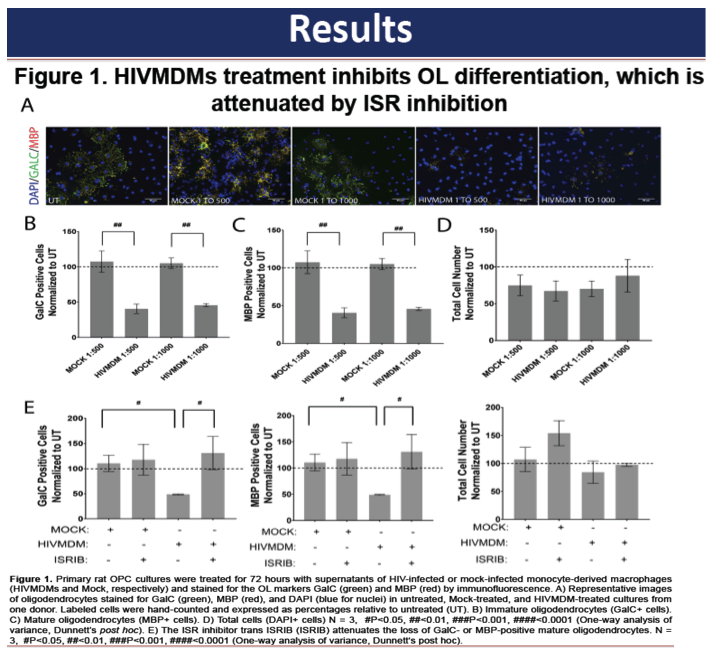
In our in vitro model, OPC differentiation was inhibited by HIVMDMS and elvitegravir, whereas raltegravir and cobicistat did not affect oligodendrocyte differentiation. The inhibition of OPC differentiation by HIVMDMs and elvitegravir was reversed by inhibiting the integrated stress response using the small molecule trans-ISRIB. Finally, administration of elvitegravir during the recovery phase following cuprizone-induced demyelination resulted in failure of remyelination, indicated by reduced ASPA and luxol fast blue staining. Persistent neuroinflammation was evident in the corpus callosum in elvitegravir-treated mice compared with the untreated controls.
These studies suggest that both HIV infection and elvitegravir inhibit OPC differentiation in vitro and in vivo. Further studies of the effects of HIV and/or first-line ARV compounds are warranted to provide insights into the observed persistent white matter changes seen in patients with HIV-associated neurocognitive disorders and their potential contribution to cognitive impairment.
|
| |
|
 |
 |
|
|