 |
 |
 |
| |
Neurosymptomatic HIV-1 CSF Escape can Occur with Replication in CD4+ T Cells in the CNS
|
| |
| |
Reported by Jules Levin
CROI 2019 March 4-7 Seattle
Laura P. Kincer1, Magnus Gisslen2, Serena Spudich3, Mattia Trunfio4, Andrea Calcagno4, Paola Cinque5,
Ronald Swanstrom1, Richard W. Price6, and Sarah B. Joseph1
ABSTRACT
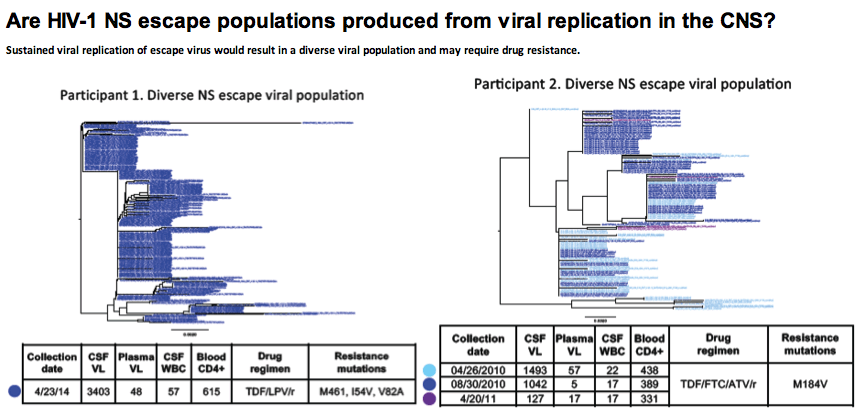
Background: Some HIV-infected individuals presenting with neurologic symptoms have increased levels of cerebrospinal fluid (CSF) HIV-1 RNA despite being on antiretroviral therapy (ART) and having undetectable, or low, plasma viral load (VL)-i.e. neurosymptomatic (NS) CSF escape. Genetic diversity and phenotypic characteristics of NS CSF escape viruses have not been previously examined, and the cells producing these populations are unknown.
Methods: We examined archived blood plasma and CSF samples from 14 individuals with NS CSF escape. All individuals were ART-treated and had a CSF VL >40 copies/ml and greater than the VL in plasma. Single genome amplification (SGA) and/or Illumina MiSeq deep sequencing with Primer ID were used to assess diversity in env and drug resistance in pro-pol. Full-length env genes were cloned from the CSF of three individuals and assessed for macrophage tropism
based on their ability to efficiently enter cells with a low density of CD4 on their surface.
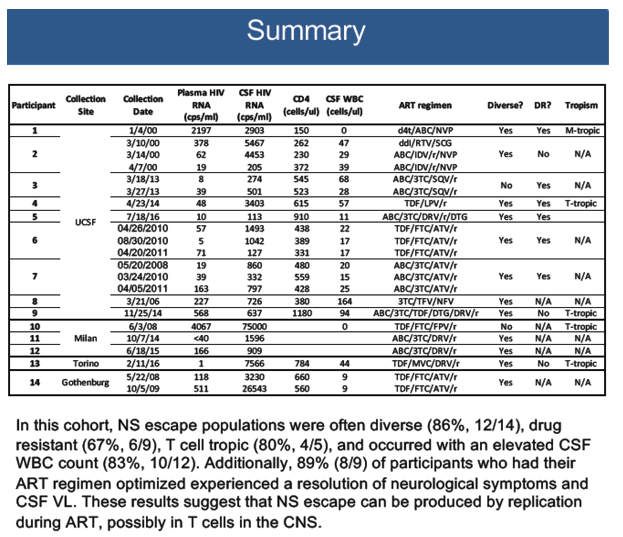
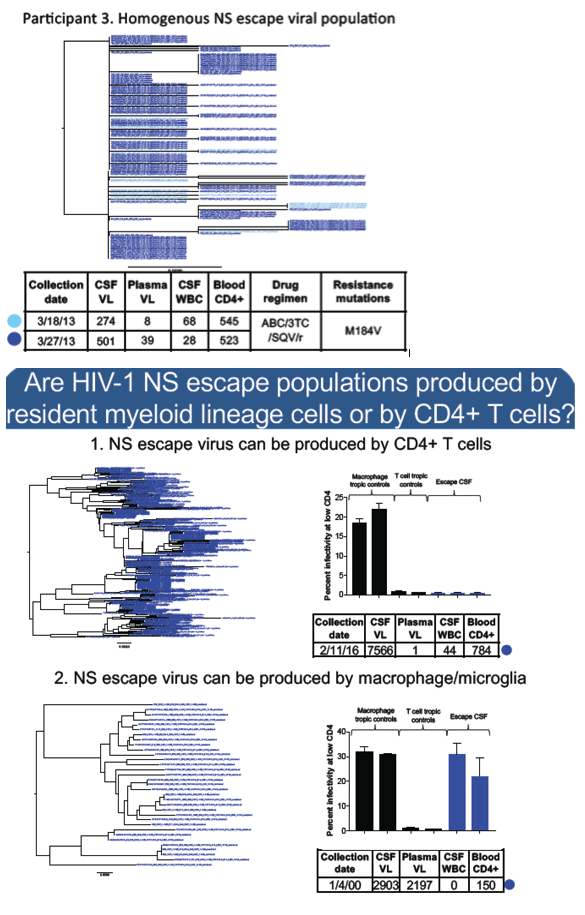
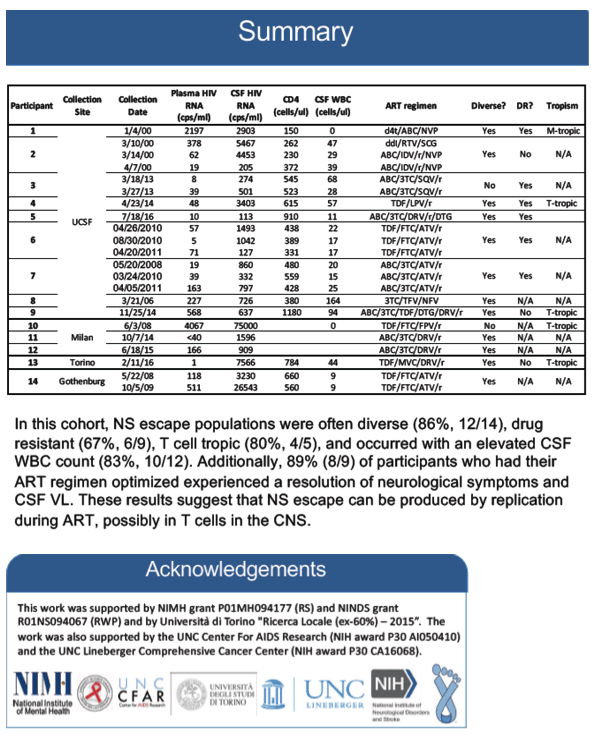
Results: For these 14 participants, median values were: CSF VL = 1,253 copies/ml, plasma VL = 120 copies/ml, blood CD4 count = 534 cells/μl and CSF WBC count = 29 cells/ μl. 86% (12/14) of participants had a genetically diverse CSF escape HIV-1 population. 67% of individuals examined for drug resistance (6/9) had mutations in their CSF virus conferring at least partial resistance to their current ART regimen. 8 of 9 participants experienced an improvement in neurologic symptoms upon ART optimization. Five individuals were examined longitudinally and four had persistent CSF escape. Of the five participants examined for viral tropism, 4 had CSF HIV-1 variants that were adapted to entering CD4+ T cells (i.e. R5 T cell-tropic) while 1 had HIV-1 variants that were adapted to entering macrophages (i.e. R5 Macrophage-tropic).
Conclusions: Most individuals with symptomatic CSF escape have characteristics that are consistent with ongoing viral replication such as genetically diverse CSF viral populations, CSF drug resistance and resolution of neurologic symptoms after ART optimization. The results here suggest that NS CSF escape virus can be adapted to entering T cells and is likely produced by CD4+ T cells in the CNS. It remains unknown whether these infected cells represent long-lived viral reservoirs in the CNS or transient populations producing virus during treatment failure due to drug resistance or non adherence.

|
| |
|
 |
 |
|
|