 |
 |
 |
| |
Shorter time to treatment failure in PLHIV switched to dolutegravir plus either rilpivirine or lamivudine compared to integrase inhibitor-based triple therapy in a large Spanish cohort - VACH
Doubled Failure Risk After Switch to DTG/RPV or DTG/3TC Versus Triple-INI Regimen
|
| |
| |
17th European AIDS Conference, November 6-9, 2019, Basel
Mark Mascolini
Treatment failure proved twice as likely when switching to a two-drug dolutegravir (DTG) regimen than when switching to a three-drug integrase inhibitor (INI) combination in a large Spanish cohort [1]. A differing adverse event rate did not explain why two-drug DTG maintenance came up short.
Two-drug antiretroviral regimens, particularly DTG with rilpivirine (RPV) or lamivudine (3TC), have gained popularity with randomized trial demonstration of their virologic noninferiority to triple therapy as a maintenance regimen and even as first-line therapy [2]. To evaluate maintenance therapy with DTG/RPV and DTG/3TC in the clinic, researchers working with the Spanish VACH cohort of adults with HIV conducted this retrospective analysis.
The study included everyone in the VACH cohort switching to INI-based triple therapy or to DTG/RPV or DTG/3TC between May 2, 2016 and May 15, 2019. Researchers excluded people who switched to their previous regimen or their new regimen for a planned treatment interruption or intermittent therapy. The study had four main endpoints: (1) time to discontinuation due to treatment failure (clinician report of virologic failure, immunologic failure, or disease progression), (2) risk of discontinuation due to treatment failure, (3) time to discontinuation due to adverse events, and (4) risk of discontinuation due to adverse events. Cox proportional hazards models to assess risk of discontinuation adjusted for patient demographics, viral load, CD4 count, number of previous regimens or virologic failures, and years on antiretroviral therapy.
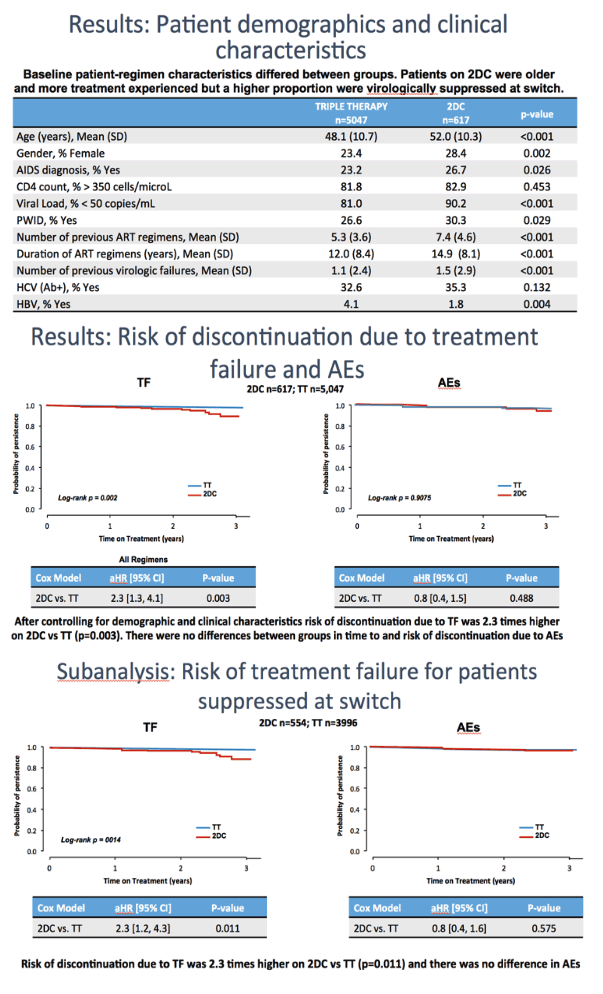
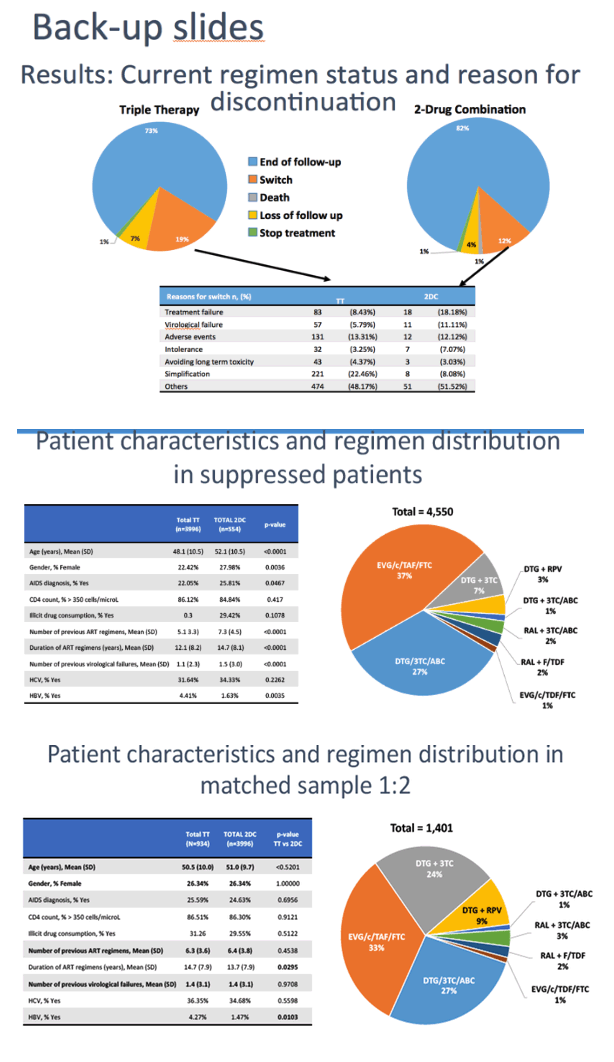
The analysis included 617 people switching to DTG dual therapy and 5047 switching to triple therapy. Two thirds of the dual-therapy group switched to DTG/3TC and the rest to DTG/RPV. The most popular triple regimens were elvitegravir/cobicistat/TAF/FTC in 51% and DTG/ABC/3TC in 40%.
The DTG dual-therapy group differed from the triple-therapy group in average age (52 versus 48.1, P < 0.001), proportion of women (28.4% versus 23.4%, P = 0.002), proportion with an AIDS diagnosis (26.7% versus 23.2%, P = 0.026), proportion with a viral load below 50 copies at the switch (90.2% versus 81%, P < 0.001), average number of previous antiretroviral regimens (7.4 versus 5.3, P < 0.001), and average number of virologic failures (1.5 versus 1.1, P < 0.001).
Follow-up after the switch lasted 3 years. A proportional hazards model determined that people switching to a two-drug regimen had more than a doubled risk of discontinuation due to treatment failure (adjusted hazard ratio [aHR] 2.3, 95% confidence interval [CI] 1.3 to 4.1, P = 0.003). The same model saw no difference between the regimens in discontinuation for adverse events.
When the VACH researchers limited the analysis to people with an undetectable viral load when switching to the new regimen, dual therapy still carried more than a doubled risk of treatment failure (aHR 2.3, 95% CI 1.2 to 4.3, P = 0.011), while discontinuation for adverse events remained similar with the two switch strategies.
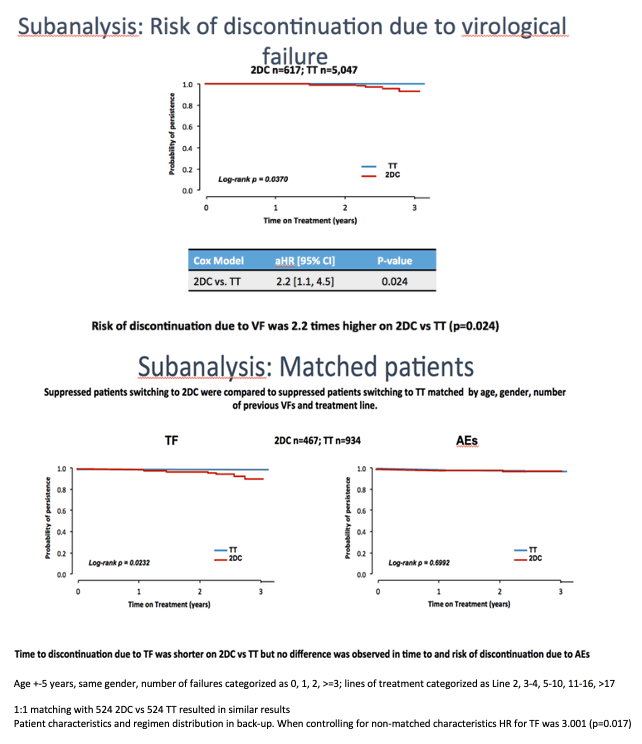
Next the investigators limited the analysis to risk of discontinuation for virologic failure alone. Dual-DTG therapy still more than doubled the risk of failure compared with triple therapy (aHR 2.2, 95% CI 1.1 to 4.5, P = 0.024). Then the VACH team compared failure rates in 467 dual-therapy patients and 934 triple-therapy patients matched for age (within 5 years), gender, number of previous failures, and number of previous regimens. Time to treatment failure through 3 years was significantly shorter in the dual-therapy group (P = 0.0232), but the groups did not differ in time to discontinuation for adverse events.
The researchers noted that dual therapy combinations may have had a disadvantage in these comparisons because both were multitablet regimens at the time of this analysis, while the major triple therapies were available as single-tablet regimens. Still, the findings raise concern about the relative durability of maintenance therapy with DTG/3TC or DTG/RPV versus triple therapy with an integrase inhibitor.
References
1. Teira R, Diaz-Cuervo H, Aragao F, et al. Shorter time to treatment failure in PLHIV switched to dolutegravir plus either rilpivirine or lamivudine compared to integrase inhibitor-based triple therapy in a large Spanish cohort - VACH. 17th European AIDS Conference, November 6-9, 2019, Basel. Abstract PS8/5.
2. Cahn P, Madero JS, Arribas JR, et al. Dolutegravir plus lamivudine versus dolutegravir plus tenofovir disoproxil fumarate and emtricitabine in antiretroviral-naive adults with HIV-1 infection (GEMINI-1 and GEMINI-2): week 48 results from two multicentre, double-blind, randomised, non-inferiority, phase 3 trials. Lancet. 2019;393:143-155


|
| |
|
 |
 |
|
|