| |
HIV drug resistance in a cohort of HIV-infected MSM in the United States
|
| |
| |
Engaging Disenfranchised U.S. Populations into HIV Care Helps Suppress the Virus
Download the PDF here
Jul 22, 2019
HPTN 078 was designed to compare the effectiveness of a combined HIV prevention strategy, including a peer-to-peer referral method to recruit MSM living with unsuppressed HIV and an intervention to help them achieve and maintain viral suppression, to the standard of care. Specifically, researchers used direct deep-chain, respondent-driven sampling (DC-RDS), augmented with direct recruitment, to identify gay, bisexual and other MSM with unsuppressed HIV......Overall, 1,305 individuals (95 percent identified as male, 69 percent as black and 12 percent as Latinx) were screened, among whom 902 (69 percent) were living with HIV and 154 (12 percent) were virally unsuppressed.....https://www.hptn.org/news-and-events/press-releases/engaging-disenfranchised-us-populations-into-hiv-care-helps-suppress
"In conclusion, we found a high prevalence of HIV drug resistance and multiclass drug resistance among viremic MSM from diverse regions in the United States, with a resistance rate greater than 50% in Birmingham, Alabama. Many MSM had INSTI resistance, and some had resistance to second-generation INSTIs. Resistance to TDF/FTC was also observed, which could impact use of PrEP in this population. These findings underscore the need for continued surveillance of drug resistance and improved HIV care in this high-risk population, for identification of alternatives to TDF/FTC for PrEP, and for including baseline integrase resistance testing when selecting ART regimens for MSM in the United States."
"High prevalence of drug resistance was observed among MSM........Multiclass resistance was observed in 17 (12.0%) of the 142 cases.....NRTI mutations associated with TDF and FTC resistance (M184I/V, K65R) were detected in 23 (16.2%) of the 142 cases (25% in Birmingham; 10-17% at the other sites) .....In the United States, the current administration's plan, 'Ending the HIV Epidemic: A Plan for America', includes interventions such as early antiretroviral therapy (ART) to achieve viral suppression and preexposure prophylaxis (PrEP) [1]. Goals of this program and other programs for HIV treatment and prevention may be compromised by HIV drug resistance......Drug resistance was detected more frequently at the Birmingham site (53.1%) compared with the other study sites (20.8-28.6%, P = 0.018, Table 2 and Fig. 1)......High-level resistance to at least one ARV drug was detected in 44 (31.0%) of the 142 cases; 30 (21.1%) had NNRTI resistance, 23 (16.2%) had NRTI resistance, and five (3.5%) had protease inhibitor resistance; 11 (8.0%) of 138 cases had INSTI resistance (Fig. 1, Table 1). Multiclass resistance was observed in 17 (12.0%) of the 142 cases (Fig. 1). Ten individuals had resistance to two drug classes, six had resistance to three drug classes, and one had resistance to all four drug classes (Table 1).....Findings from this study suggest that some individuals may have been infected with drug-resistant HIV.....Resistance was also more frequent among those who were directly recruited than among those who were recruited through DC-RDS......In conclusion, we found a high prevalence of HIV drug resistance and multiclass drug resistance among viremic MSM from diverse regions in the United States, with a resistance rate greater than 50% in Birmingham, Alabama. Many MSM had INSTI resistance, and some had resistance to second-generation INSTIs. Resistance to TDF/FTC was also observed, which could impact use of PrEP in this population. These findings underscore the need for continued surveillance of drug resistance and improved HIV care in this high-risk population, for identification of alternatives to TDF/FTC for PrEP, and for including baseline integrase resistance testing when selecting ART regimens for MSM in the United States.
---------------------
HIV drug resistance in a cohort of HIV-infected MSM in the United States
Fogel, Jessica M.a; Sivay, Mariya V.a; Cummings, Vanessaa; Wilson, Ethan A.b; Hart, Stephenc; Gamble, Theresad; Laeyendecker, Olivere,f; Fernandez, Reinaldo E.f; Del Rio, Carlosg; Batey, D. Scotth; Mayer, Kenneth H.i,j; Farley, Jason E.k; McKinstry, Laurab; Hughes, James P.l; Remien, Robert H.m; Beyrer, Chrisn; Eshleman, Susan H.a
AIDS: jan 1 2020
Objective: To analyze HIV drug resistance among MSM recruited for participation in the HPTN 078 study, which evaluated methods for achieving and maintaining viral suppression in HIV-infected MSM.
Methods: Individuals were recruited at four study sites in the United States (Atlanta, Georgia; Baltimore, Maryland; Birmingham, Alabama; and Boston, Massachusetts; 2016-2017). HIV genotyping was performed using samples collected at study screening or enrollment. HIV drug resistance was evaluated using the Stanford v8.7 algorithm.
A multiassay algorithm was used to identify individuals with recent HIV infection. Clustering of HIV sequences was evaluated using phylogenetic methods.
Results: High-level HIV drug resistance was detected in 44 (31%) of 142 individuals (Atlanta: 21%, Baltimore: 29%, Birmingham: 53%, Boston: 26%); 12% had multiclass resistance, 16% had resistance to tenofovir or emtricitabine, and 8% had resistance to integrase strand transfer inhibitors (INSTIs); 3% had intermediate-level resistance to second-generation INSTIs. In a multivariate model, self-report of ever having been on antiretroviral therapy (ART) was associated with resistance (P = 0.005). One of six recently infected individuals had drug resistance. Phylogenetic analysis identified five clusters of study sequences; two clusters had shared resistance mutations.
Conclusion: High prevalence of drug resistance was observed among MSM. Some had multiclass resistance, resistance to drugs used for preexposure prophylaxis (PrEP), and INSTI resistance. These findings highlight the need for improved HIV care in this high-risk population, identification of alternative regimens for PrEP, and inclusion of integrase resistance testing when selecting ART regimens for MSM in the United States.
Introduction
In the United States, the current administration's plan, 'Ending the HIV Epidemic: A Plan for America', includes interventions such as early antiretroviral therapy (ART) to achieve viral suppression and preexposure prophylaxis (PrEP) [1]. Goals of this program and other programs for HIV treatment and prevention may be compromised by HIV drug resistance [2,3]. Acquired drug resistance can emerge in HIV-infected individuals with sub-optimal adherence to ART, in individuals who become HIV-infected while taking PrEP [4,5], and in those taking antiretroviral (ARV) drugs for other reasons. Individuals can also be infected with drug-resistant HIV [transmitted drug resistance (TDR)]. Some studies have reported decreases in acquired drug resistance in high-income countries [6,7], which may reflect increased use of drugs with high genetic barriers for resistance and increased use of HIV genotyping and viral load monitoring to guide treatment. However, the frequency of acquired drug resistance remains high in many settings, and TDR has also increased in some settings [8-10].
Approximately two-thirds of new HIV infections in the United States occur in MSM [11]. In 2015, only 62% of MSM diagnosed with HIV were receiving care, and only 52% were virally suppressed [12]. Surveillance data have shown that most HIV infections among MSM in the United States are linked to infections in other MSM [13], and phylogenetic studies have found that active transmission clusters are more concentrated among MSM than other risk groups [14]. Data on drug resistance among MSM in the United States are limited. In a study of Black MSM in six cities in the United States [HIV Prevention Trials Network (HPTN) 061; enrollment 2009-2010], 28% of 169 HIV-infected study participants had drug resistance; 36% of those with resistance had ARV drugs detected, including many who did not report being in care [15]. Resistance to integrase strand transfer inhibitors (INSTIs) was not observed in that cohort [16]. Some studies have also reported higher rates of TDR among MSM compared with other risk groups [8,17,18].
HPTN 078 evaluated an HIV prevention strategy focused on achieving and maintaining viral suppression in HIV-infected MSM in the United States (screening/enrollment: 2016-2017). The study enrolled HIV-infected individuals who were not virally suppressed at study sites in four US cities, including two study sites that participated in HPTN 061. Many individuals were recruited using respondent-driven sampling (RDS), which has been shown to help identify most-at-risk populations, including Black and Hispanic MSM and MSM with lower socioeconomic status [19-21]. In this study, we analyzed HIV drug resistance and the phylogenetic relationships of HIV among individuals recruited for participation in HPTN 078.
Results
Samples included in the resistance study
This study included analysis of samples from all HIV-infected individuals screened for participation in HPTN 078 who had a viral load at least 1000 copies/ml at study entry (144 who enrolled in HPTN 078 and 11 who did not enroll in the study). HIV genotyping was performed using samples obtained at study entry (screening or enrollment) from 145 individuals; 10 were excluded from testing (7 did not have a sample available for testing, and 3 had discrepant viral load results from testing performed at the study site vs. the HPTN Laboratory Center). Protease/RT genotyping results were obtained for 142 (97.9%) of the 145 samples; three failed genotyping. Among the 142 individuals with results, 121 (85.2%) were Black/African American; 138 (97.2%) identified as male individual, one identified as female individual, two identified as transgender, and one identified as gender variant/nonconforming. Six of the 142 individuals were identified as recently infected using a multiassay algorithm developed for cross-sectional HIV incidence estimation (2 from Birmingham; 4 from Atlanta). Integrase genotyping results were obtained for 138 of the 142 cases (4 failed analysis).
Analysis of HIV drug resistance
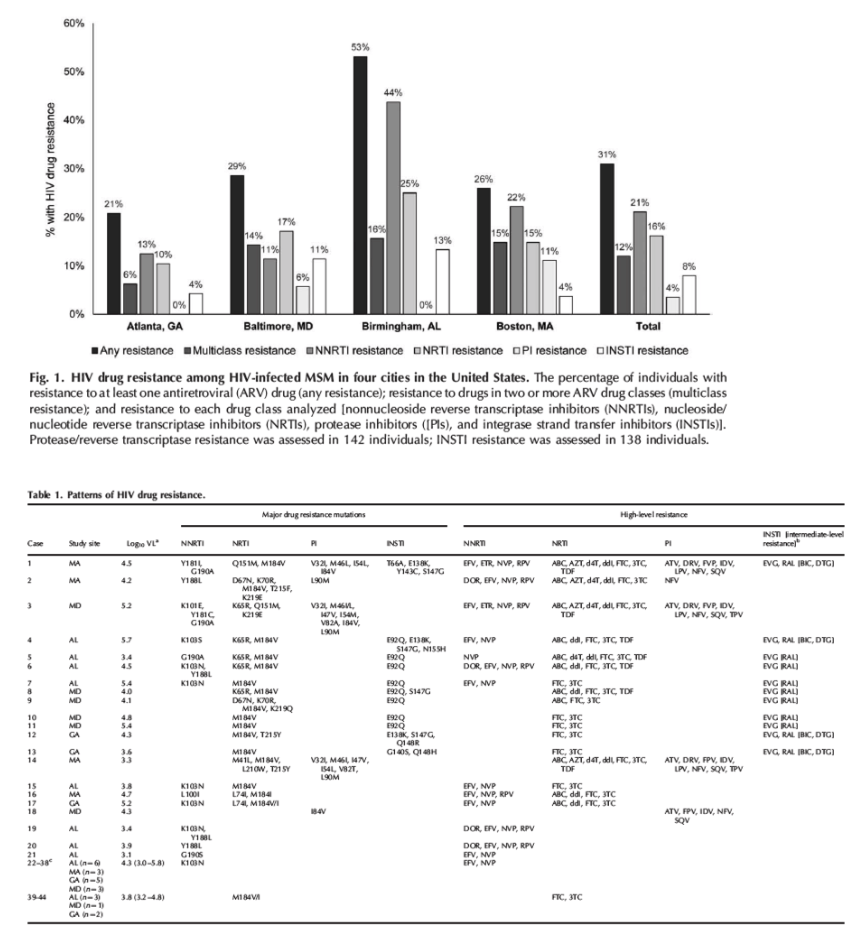
High-level resistance to at least one ARV drug was detected in 44 (31.0%) of the 142 cases; 30 (21.1%) had NNRTI resistance, 23 (16.2%) had NRTI resistance, and five (3.5%) had protease inhibitor resistance; 11 (8.0%) of 138 cases had INSTI resistance (Fig. 1, Table 1). Multiclass resistance was observed in 17 (12.0%) of the 142 cases (Fig. 1). Ten individuals had resistance to two drug classes, six had resistance to three drug classes, and one had resistance to all four drug classes (Table 1).
The mutation detected most frequently was K103N (n = 22), which causes high-level resistance to the NNRTIs, efavirenz and nevirapine. The Y188L mutation was detected in four cases; this mutation causes high-level NNRTI resistance, including resistance to the newly approved NNRTI, doravirine. NRTI mutations associated with TDF and FTC resistance (M184I/V, K65R) were detected in 23 (16.2%) of the 142 cases (25% in Birmingham; 10-17% at the other sites). All 11 cases with high-level INSTI resistance had resistance to elvitegravir; four also had high-level resistance to raltegravir and intermediate-level resistance to the second-generation INSTIs, bictegravir and dolutegravir. All 11 individuals with INSTI resistance had NRTI resistance; five also had NNRTI resistance, and one also had protease inhibitor resistance (Table 1).
We also analyzed cases of possible TDR. Of the 142 individuals, 117 reported that they had been tested for HIV and had received the test result. Eight of those 117 individuals reported that the test was negative, that they did not recall the result, or that they preferred not to provide information about the test result. Resistance mutations were detected in three (37.5%) of those eight cases [one case from Baltimore (NRTI: M184V; INSTI: E92Q); two cases from Atlanta (NNRTI: K103N in one case and NRTI: M184V; INSTI: T97A in the other case)]. Resistance mutations were also detected in one of six individuals classified as recently infected using a multiassay algorithm (NNRTI: K103N; NRTI: K219Q).
Factors associated with HIV drug resistance
We next evaluated the association of drug resistance with behavioral, demographic, and clinical factors (Table 2). Drug resistance was detected more frequently at the Birmingham site (53.1%) compared with the other study sites (20.8-28.6%, P = 0.018, Table 2 and Fig. 1). Drug resistance was also significantly higher among those who reported ever taking ART (P = 0.011, Table 2) and among those who were recruited using non-RDS methods (P = 0.044, Table 2). In a multivariate model, self-report of ever taking ART was the only factor significantly associated with resistance (P = 0.005, Table 2). The adjusted odds ratio for resistance was 13.0 (95% CI 2.45-69.2) for those who reported ever taking ART vs. those who did not report ART, and was 3.06 (95% CI 0.32-29.0) for those who reported 'don't know' or 'prefer not to answer' vs. those who did not report ART.
Phylogenetic analysis of HIV-1 strains
Among the 142 individuals with protease/reverse transcriptase genotyping results, 138 (97.2%) had subtype B HIV (all subtyping tools in agreement); the other four sequences were potential inter-subtype recombinants [recombinant with REGA (n = 3) and RIP (n = 1)]. All 138 integrase sequences were subtype B HIV.
Cluster analysis was performed using 132 of the 138 subtype B protease/reverse transcriptase sequences (six additional sequences were excluded from analysis; two had sequence ambiguity >5%; four had evidence of intra-subtype recombination with RDP4). The median pairwise genetic distance was 6.4% [interquartile range (IQR): 5.6-7.2] among the 132 sequences and was similar across the four study sites. Study sequences from all four study sites were interspersed with background sequences, and no large clusters of study sequences were observed (Fig. 2 ). Four small clusters of sequences were detected that included two study sequences with zero, one, or two background sequences (Supplemental Digital Content, http://links.lww.com/QAD/B545). Cluster analysis was also performed using all 138 integrase sequences. The median pairwise genetic distance among these sequences was 4.8% (IQR: 4.1-5.5). This analysis identified the same four clusters observed for protease/reverse transcriptase sequences and one additional cluster of two study sequences that was identified using integrase sequences only (Supplemental Digital Content, http://links.lww.com/QAD/B545). Three of the five clusters included sequences from individuals recruited at different study sites [Atlanta and Birmingham (n = 2); Atlanta and Boston (n = 1)]. None of the sequences from the six individuals identified as recently infected clustered with other study sequences.
We next evaluated whether any of the five clusters included drug-resistant HIV strains (note that codons associated with drug resistance were removed prior to phylogenetic analysis). In one cluster, K103N was present in both study and background sequences. The pairwise genetic distance between the study sequences in this cluster was less than 0.5% for protease/reverse transcriptase and integrase, indicating a recent transmission linkage (Supplemental Digital Content, Case 1, http://links.lww.com/QAD/B545). In another cluster, one study sequence had NRTI and INSTI resistance mutations, and the other study sequence had a shared NRTI mutation (T215C; Supplemental Digital Content, Case 2, http://links.lww.com/QAD/B545).
Discussion
We evaluated HIV drug resistance among MSM in four US cities who were recruited for participation in the HPTN 078 study. Some individuals were identified for study screening using DC-RDS, in an attempt to reach those who were less likely to be engaged in care. HIV drug resistance was detected in 31% of the cases. Multiclass resistance was detected in 12% of the cases, including six individuals with three-class resistance and one individual with four-class resistance. Individuals with multiclass resistance have limited treatment options. Some individuals with multiclass drug resistance have achieved viral suppression when the postattachment inhibitor, ibalizumab, was added to an optimized background regimen [35,36].
The prevalence of NNRTI, NRTI, and protease inhibitor resistance in this cohort was similar to what we observed among MSM in an older study (HPTN 061: 28%; data from 2009 to 2010) [15]. In this study, more than half of those with drug resistance had resistance to at least one of the NRTI drugs approved for PrEP (TDF/FTC). This is concerning, as resistance to these drugs may reduce the efficacy of PrEP for high-risk HIV-uninfected MSM. INSTI resistance was detected in 8% of the individuals in this study. This is high compared with the rate of INSTI resistance in other reports. INSTI resistance was not observed in the older HPTN 061 study [16]. INSTI resistance was only detected in less than 2% of HIV-infected individuals living in Washington, DC (2013), whereas the overall prevalence of resistance was high [6]. A surveillance study among newly diagnosed individuals in the United States from 2010 to 2014 showed that integrase testing was performed more frequently among MSM than other risk groups; in that study, the prevalence of INSTI resistance was low (0.4%) [37].
Three new INSTIs were recently approved by the US FDA for HIV treatment and INSTI-containing ART regimens are now used for first-line HIV treatment in the United States [38]. The first-generation INSTIs, elvitegravir and raltegravir, have a lower barrier to drug resistance and have overlapping resistance profiles [39]. Second-generation INSTIs, such as dolutegravir or bictegravir [40], have different resistance profiles. In this study, we identified 11 individuals with high-level INSTI resistance, including four who had intermediate resistance to dolutegravir and bictegravir. All individuals with INSTI resistance also had high-level NRTI resistance; five also had high-level NNRTI resistance, and one also had high-level PI resistance, further limiting their treatment options. The mutation Q148R, which causes high-level resistance to several INSTIs, was detected in one case; this mutation has been observed in individuals who experience virologic failure after taking cabotegravir, which is being evaluated for HIV treatment and prevention [41,42]. Although dolutegravir, bictegravir, and cabotegravir have been shown to have activity against INSTI-resistant HIV [43], persons with both INSTI and NRTI resistance may not respond to co-formulated regimens that include a second-generation INSTI with emtricitabine and tenofovir or tenofovir alafenamide.
Some guidelines do not recommend routine testing for INSTI resistance in drug-naïve individuals [44]. Detection of resistance to first-generation and second-generation INSTIs in this cohort highlights the importance of including baseline integrase resistance testing when selecting ART regimens for MSM in the United States. Although regimens that include dolutegravir and bictegravir may be useful in this population, ∼10% of those in this cohort with drug resistance also had intermediate resistance to these drugs, highlighting the urgent need to address issues related to drug resistance in this population.
Findings from this study suggest that some individuals may have been infected with drug-resistant HIV. We detected drug resistance in three of the eight individuals who reported that they did not have a prior HIV-positive test and in one of six individuals who were classified as recently infected using a multiassay algorithm. These cases may reflect TDR. However, it is also possible that one or more of these individuals was aware of their HIV status and had taken ART, but chose not to report this to study staff; they may also have used ARV drugs for another reason (e.g. PrEP, hepatitis treatment, recreational use). In a study of newly diagnosed MSM attending a community clinic in Los Angeles, the rate of drug resistance among recently infected persons was similar to those with longer-standing infection [45].
In other studies, the rate of HIV drug resistance among MSM in the United States, was higher among MSM who were older [15], Black, or had transgender partners [45]. In this study, age and race were not associated with resistance. The rate of resistance was higher in Birmingham (53%), compared with the other three study sites (21-29%). Resistance was also more frequent among those who were directly recruited than among those who were recruited through DC-RDS. However, neither of these factors (study site, recruitment method) was statistically associated with resistance in a multivariate model. In the multivariate model, self-report of ever taking ART was the only factor independently associated with resistance. In contrast, self-report of currently taking ART was not associated with drug resistance. This suggests that many of those with resistance may have received suboptimal care or had poor ART adherence at some point in the past. Future ARV drug testing is planned to investigate the reasons for lack of viral suppression in the study cohort (e.g. nonadherence vs. good adherence with drug resistance).
This study also included phylogenetic analysis of HIV strains. The analyses revealed no geographic clustering, suggesting a high degree of mobility. Four clusters that included at least two study sequences were identified using both the protease/reverse transcriptase and integrase sequences; a fifth cluster was identified using the integrase sequences only. The HIV integrase region is more conserved compared with protease/reverse transcriptase, which may explain the identification of one additional cluster using integrase sequences [46]. In this study, the median genetic diversity was lower in integrase compared with protease/reverse transcriptase (4.76 vs. 6.41%, respectively). Three of the five clusters included individuals recruited from different cities (two cases: Birmingham and Atlanta; one case Atlanta and Boston). Study investigators were aware that some participants traveled between sites/cities. In one cluster, the genetic distance between study sequences was below the 0.5% threshold; suggesting a recent transmission linkage [33]. Two clusters included individuals with drug resistance. None of the clusters included individuals identified as recently infected.
In conclusion, we found a high prevalence of HIV drug resistance and multiclass drug resistance among viremic MSM from diverse regions in the United States, with a resistance rate greater than 50% in Birmingham, Alabama. Many MSM had INSTI resistance, and some had resistance to second-generation INSTIs. Resistance to TDF/FTC was also observed, which could impact use of PrEP in this population. These findings underscore the need for continued surveillance of drug resistance and improved HIV care in this high-risk population, for identification of alternatives to TDF/FTC for PrEP, and for including baseline integrase resistance testing when selecting ART regimens for MSM in the United States.
|
|
| |
| |
|
|
|