 |
 |
 |
| |
"Dual epidemics: the impact of HIV and obesity on pregnancy outcomes among women in South Africa"
'The impact of HIV and obesity on pregnancy outcomes among women in South Africa'
Obesity in 36% of Pregnant HIV+ South African Women--But No Impact on Outcomes
|
| |
| |
10th IAS Conference on HIV Science (IAS 2019), July 21-24, 2019, Mexico City
Download the PDF here
Mark Mascolini
More than one third of a group of HIV-positive pregnant South African women--and almost half of HIV-negative pregnant women--were obese in an 877-woman study [1]. Yet while most HIV-negative women with adverse pregnancy outcomes were obese, most HIV-positive women with adverse pregnancy outcomes had normal weight.
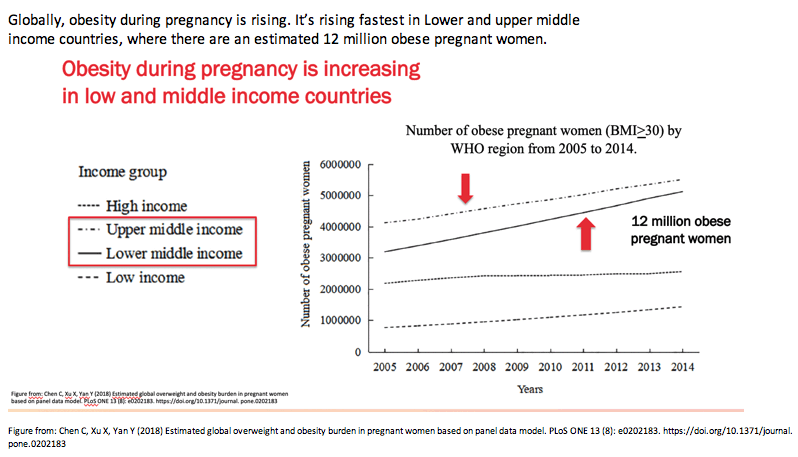
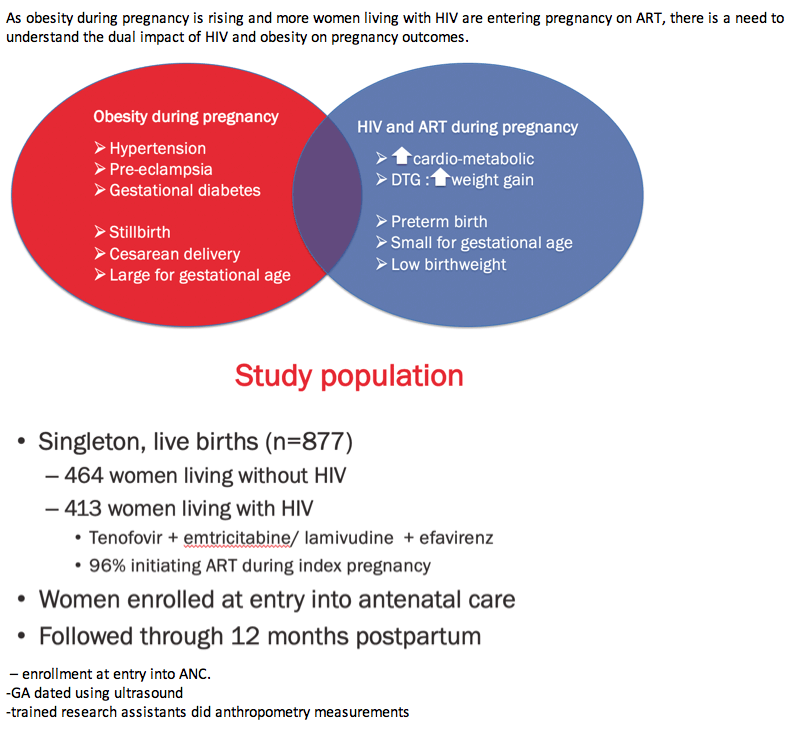
Collaborators from the University of Cape Town and New York's Columbia University noted that obesity rates are on the rise in low- and middle-income countries across the world--and HIV infection is often prevalent in these countries. Research links obesity during pregnancy to adverse outcomes (stillbirth, caesarean delivery, large for gestational age), while HIV and antiretroviral therapy (ART) are tied to other adverse outcomes (preterm birth, small for gestational age, low birthweight).
The Cape Town/Columbia team conducted this study in Guguletu Township near Cape Town to explore the dual impact of obesity and HIV on pregnancy outcomes. This was a secondary analysis of the MCH-ART trial to evaluate integrating postpartum services into HIV care [2]. Almost one third of pregnant women in Guguletu have HIV infection and 40% of pregnant women are obese.
The study population included 464 women without HIV and 413 with HIV, all of whom delivered single infants. Almost all HIV-positive women, 96%, started ART during pregnancy with a regimen including efavirenz, tenofovir, and emtricitabine or lamivudine. Follow-up continued through 12 months after delivery.
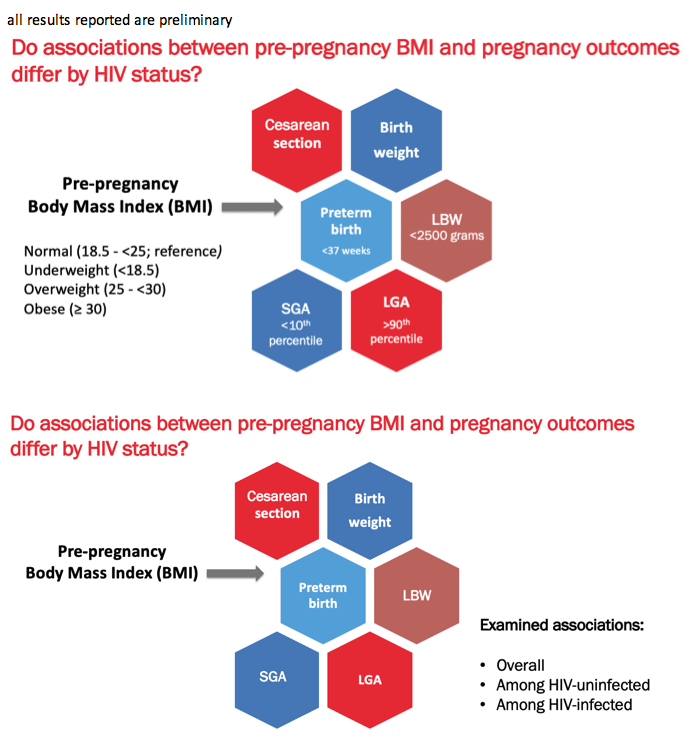
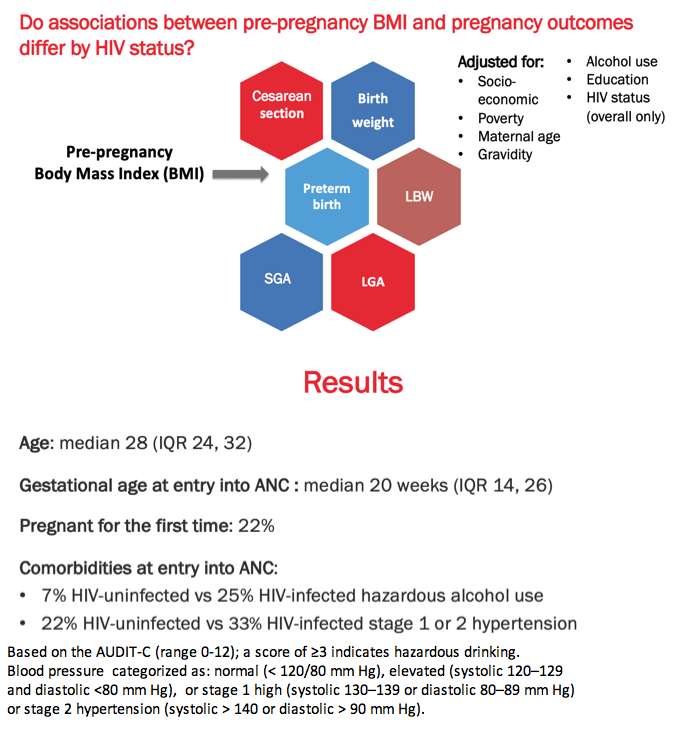
The researchers considered the impact of body mass index (BMI) on 6 adverse pregnancy outcomes: caesarean delivery, birthweight, preterm birth (before 37 weeks), low birthweight (below 2500 g), small for gestational age (below 10th percentile), and large for gestational age (above 90th percentile). Multivariable analysis to identify possible associations adjusted for socioeconomic status, poverty, maternal age, gravidity, alcohol use, education, and HIV status.
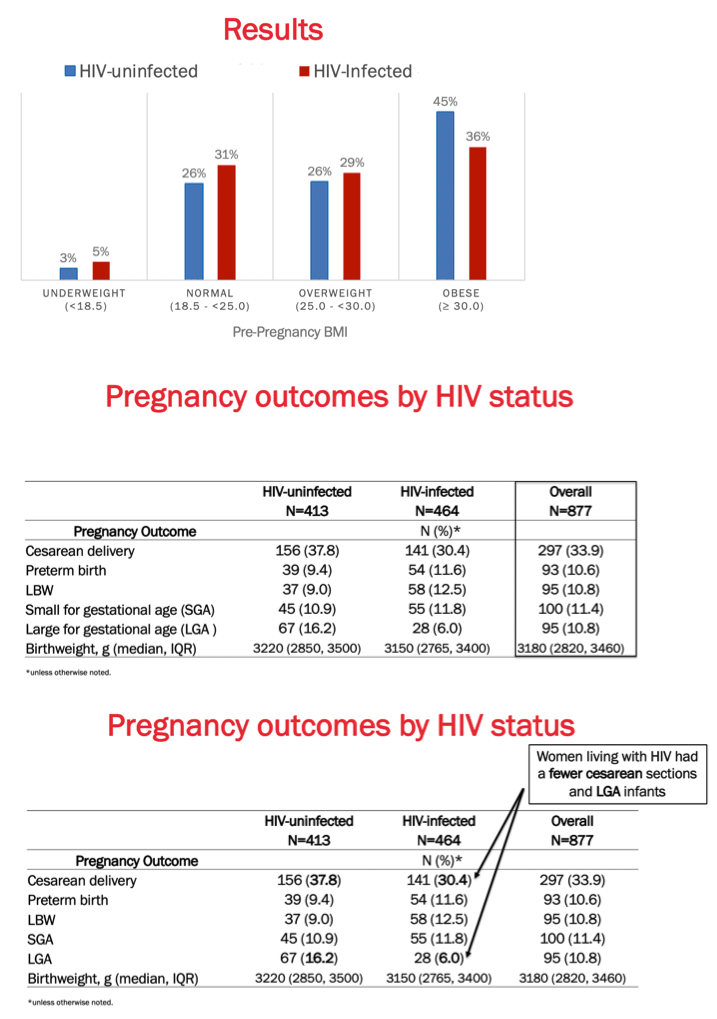
The study group had a median age of 28 years and a median gestational age of 20 weeks at entry into antenatal care. Almost one quarter of women (22%) were pregnant for the first time. While 7% of HIV-negative and 25% of HIV-positive women had hazardous alcohol use, 22% without HIV and 33% with HIV had stage 1 or 2 hypertension. Proportions of HIV-negative and positive women who were underweight were 3% and 5%, normal weight 26% and 31%, overweight 26% and 29%, and obese 45% and 36%.
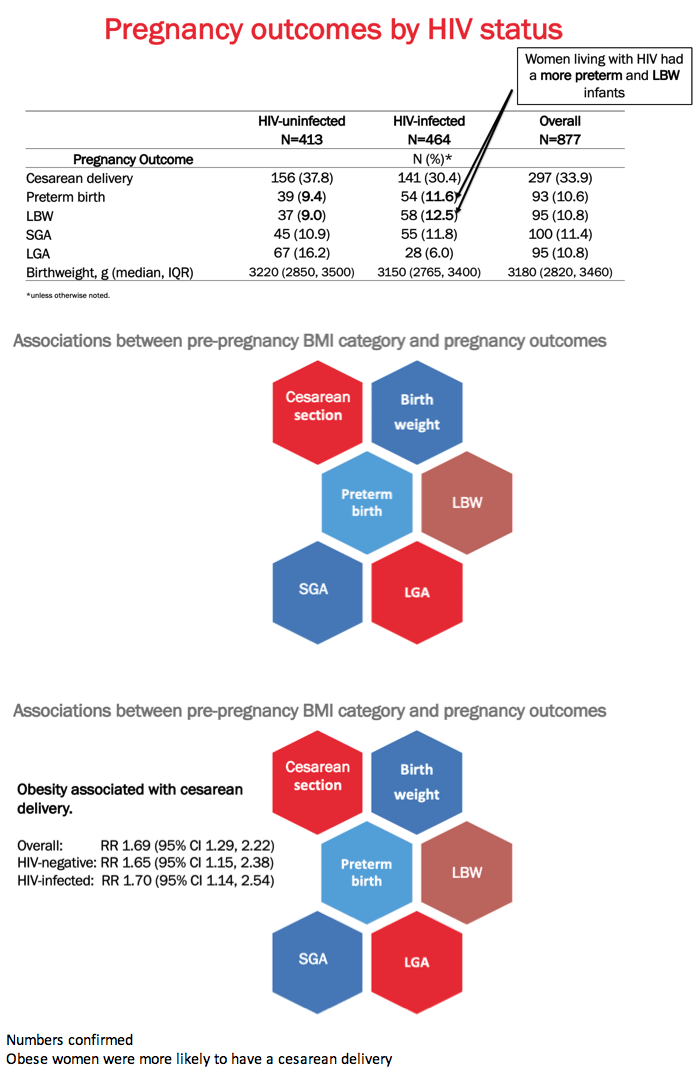
Compared with HIV-negative women, those with HIV had fewer caesarean deliveries (30.4% versus 37.8%) and large for gestational age infants (6.0% versus 16.2%) and more preterm births (11.6% versus 9.4%) and low birthweight infants (12.5% and 9.0%). Proportions of small for gestational age infants were similar in the HIV-negative group (10.9%) and the HIV-positive group (11.8%).
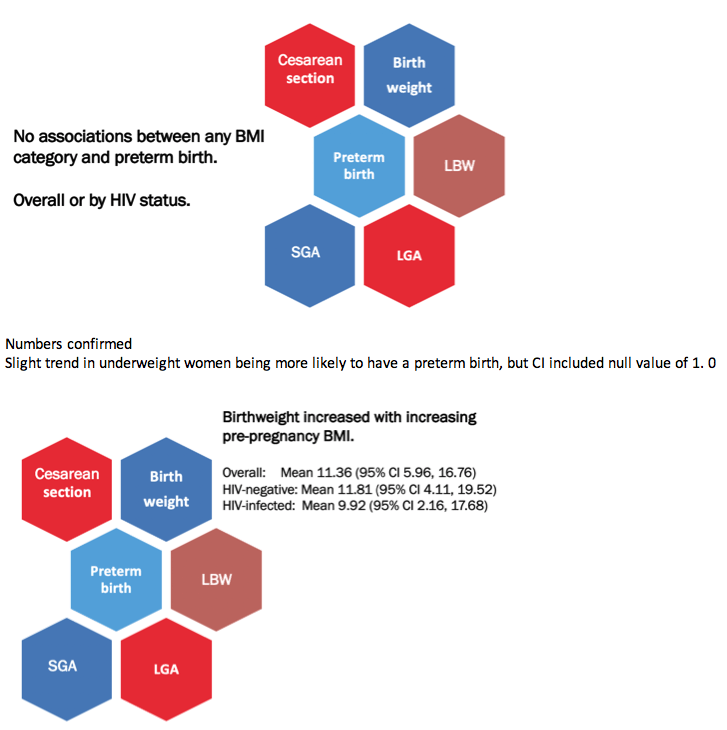
Obesity independently predicted caesarean delivery overall (relative risk [RR] 1.69, 95% confidence interval [CI] 1.29 to 2.22), in HIV-negative women (RR 1.65, 95% CI 1.15 to 2.38), and in HIV-positive women (RR 1.70, 95% CI 1.14 to 2.54). Statistical analysis uncovered no associations between any BMI category and preterm birth.
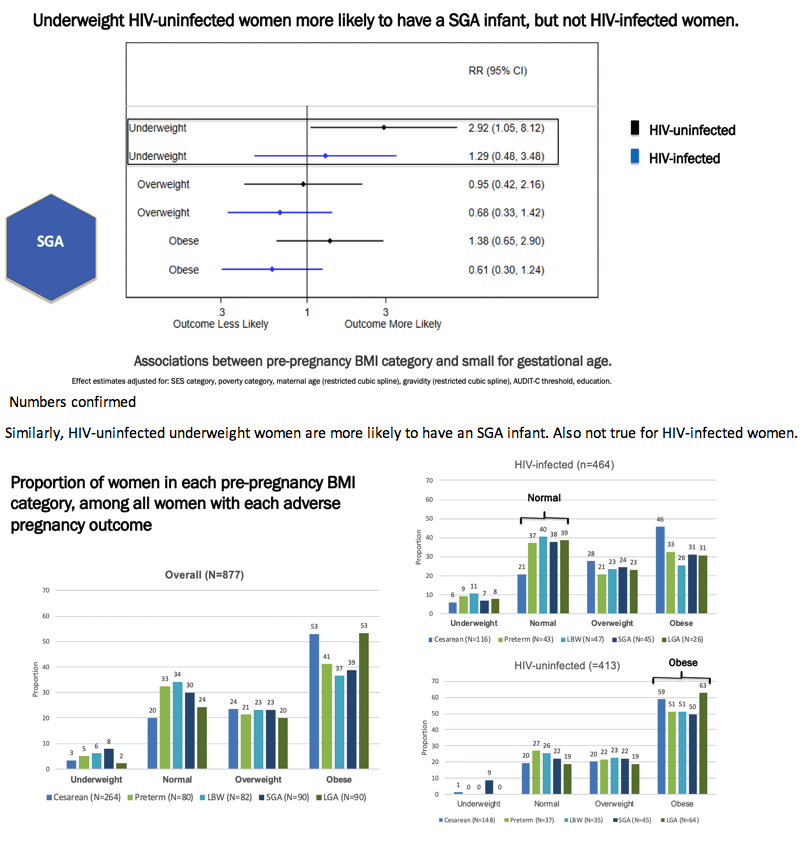
Birthweight rose with increasing prepregnancy BMI, and women with higher BMI were less likely to have a low-birthweight infant. This association stopped just short of statistical significance for women with HIV (RR 0.50, 95% CI 0.24 to 1.05). The impact of obesity on large for gestational age infants differed by HIV status: Obese HIV-negative women had almost an 80% higher risk of large infants, though that association fell short of statistical significance (RR 1.79, 95% CI 0.96 to 3.28), while a nonsignificant association ran in the other direction for HIV-positive obese women (RR 0.45, 95% CI 0.18 to 1.14). Underweight HIV-negative women had almost a 3-fold higher risk of small for gestational age infants (RR 2.92, 95% CI 1.05 to 8.12), but that association did not hold true for HIV-positive women.
Among HIV-negative women, all adverse pregnancy outcomes proved most likely in obese women (59% for caesarean, 51% for preterm birth, 51% for low birthweight, 50% for small for gestational age, and 63% for large for gestational age). But among HIV-positive women, most of these adverse outcomes were most frequent in normal-weight women (37% for preterm birth, 40% for low birthweight, 38% for small for gestational age, and 39% for large for gestational age). Among women with HIV, obese women had the highest caesarean frequency (46%).
The researchers stressed that obesity during pregnancy "is a growing public health concern in low-to-middle-income countries for both HIV-infected and HIV-uninfected women." But for women with HIV, antiretroviral therapy and infection itself "may influence fetal growth more strongly than maternal body mass index." More research, they urged, should address those potential associations in women with HIV.
References
1. Bengtson A, le Roux SM, Phillips TK, et al. Dual epidemics: The impact of HIV and obesity on pregnancy outcomes among women in South Africa. 10th IAS Conference on HIV Science (IAS 2019), July 21-24, 2019, Mexico City. Abstract TUAB0105.
2. ClinicalTrials.gov. Strategies to Optimize Antiretroviral Therapy Services for Maternal and Child Health: the MCH-ART Study (MCH-ART). ClinicalTrials.gov identifier NCT01933477.
Video - http://programme.ias2019.org/Search/Search?search=TUAB0105
IAS: Neural Tube Defect Rate 0.40% With Dolutegravir in Pregnancy--But Data Still Slim - Mark Mascolini - (07/25/19)






|
| |
|
 |
 |
|
|