 |
 |
 |
| |
Substance Use--Especially Meth--Tied
to Depression in Young HIV+/HIV- MSM
|
| |
| |
10th IAS Conference on HIV Science (IAS 2019), July 21-24, 2019, Mexico City
Mark Mascolini
Depressive symptoms proved significantly more frequent in young US men who have sex with men (MSM) who engaged in substance use--especially methamphetamine use--than in MSM without a substance use history [1]. In this California group of MSM with or at risk for HIV infection, depressive symptoms became less frequent over time for heavy users of a number of drugs, but not methamphetamine.
Depression remains highly prevalent and poorly treated in HIV populations throughout the world, including MSM [2]. Substance use also remains common in many HIV groups, though research indicates that alcohol use or illicit drug use does not moderate the antidepressant treatment response [3]. Researchers at the University of California, Los Angeles (UCLA) conducted this study to analyze prevalence, correlates, and changes in depressive symptoms among HIV-positive and at-risk negative MSM, with a particular focus on the impact of substance use.
Participants came from the mSTUDY, which aims to determine how substance use affects the immune system of HIV-positive and negative MSM [4]. Men had to be between 18 and 45 years old and male at birth. HIV-negative participants had to report condomless anal sex with a male partner in the past 6 months. At cohort entry and every 6 months, participants completed a self-interview, including the CES-D20 test for depressive symptoms.
At the initial study visit, age averaged 31 years, 43% of MSM identified as black, 37% Latino, and 14% white. Almost half had no job, and 35% reported unstable housing in the past 6 months. By design, half of the study group (267 of 534) had HIV infection.
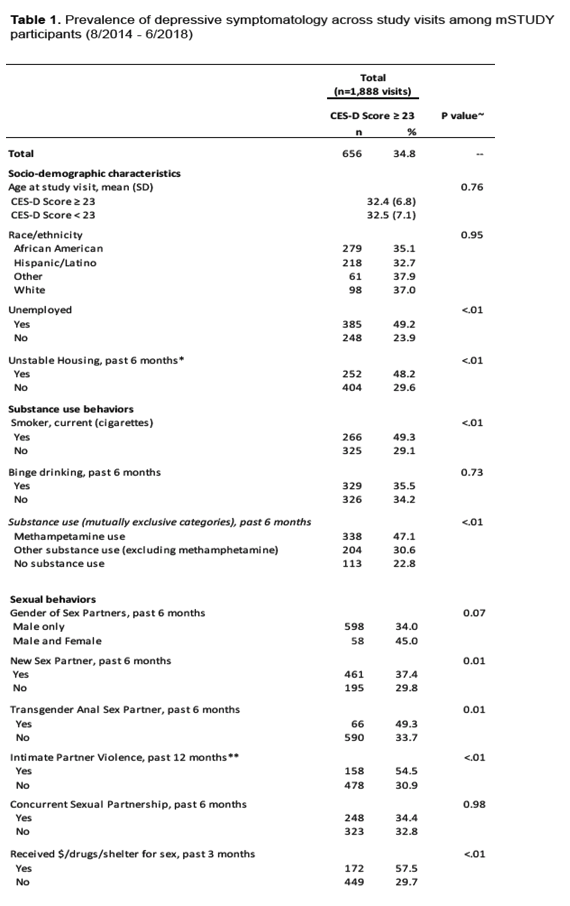
These men reported depressive symptoms (CES-D score at or above 23) at more than one third of study visits (656 of 1888, or 35%). Age at study visit was similar with a CES-D score above or below that mark (32.4 and 32.5 years). Race did not affect reporting depressive symptoms (35.1% black, 32.7% Latino, 37.0% white). But unemployed men were more likely to report depressive symptoms (49.2% versus 23.9% employed, P < 0.01), as were men with recent unstable housing (48.2% versus 29.6%, P < 0.01).
Men reported depressive symptoms more often if engaging in certain sexual behaviors, including having a new sex partner in the past 6 months, transgender anal sex in the past 6 months, intimate partner violence in the past 12 months, and receiving money, drugs, or shelter for sex in the past 3 months.
Substance use also significantly affected depression prevalence. Current smokers versus nonsmokers reported depressive symptoms at 49.3% versus 29.1% of visits (P < 0.01), and depressive symptoms proved more frequent with methamphetamine use (47.1%) or other drug use (30.6%) than with no substance use (22.8%) (P < 0.01).
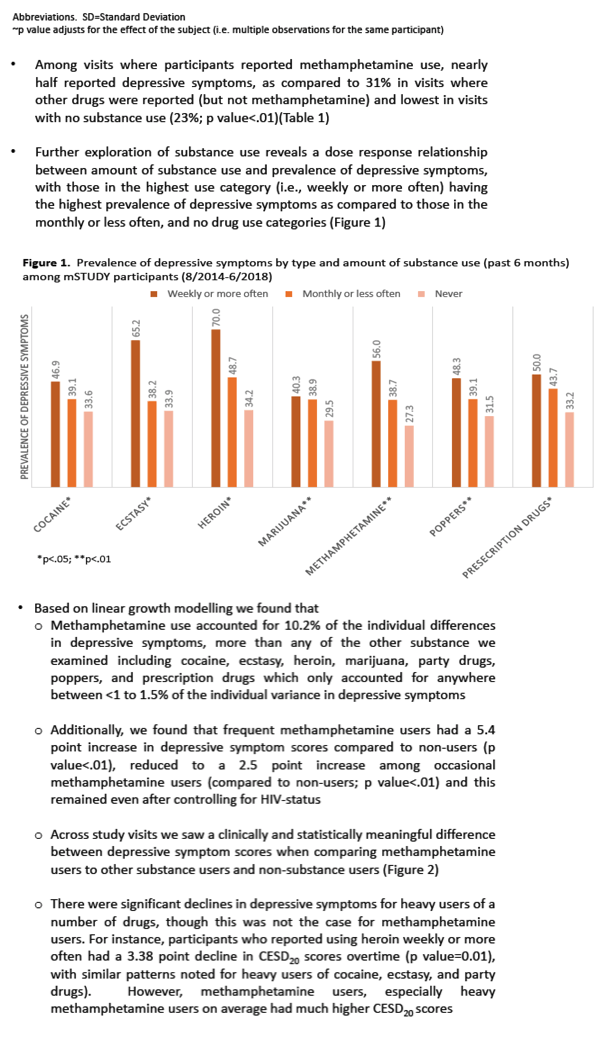
A closer look at substance use showed that more frequent use of individual drugs meant more depressive symptoms. For methamphetamine, weekly or more frequent use was associated with a depressive symptom prevalence of 56%, compared with 38.7% for monthly or less frequent use and 27.3% for never using meth (P < 0.01). The same dose-response effect held true for marijuana (P < 0.01), poppers (P < 0.01), prescription drugs (P < 0.01), cocaine (P < 0.05), ecstasy (P < 0.05), and heroin (P < 0.05). Depressive symptom rates reached 50% or higher for at least weekly abuse of prescription drugs (50.0%), methamphetamine (56.0%), ecstasy (65.2%), and heroin (70.0%).
Linear growth modeling determined that methamphetamine use accounted for 10.2% of individual differences in depressive symptoms, a much higher rate than for any other drug studied, which accounted for 1.5% or less of individual variance in depressive symptoms.
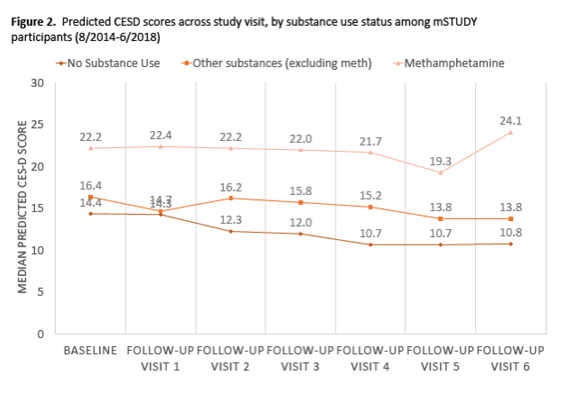
From the initial visit to follow-up visit 6, rates of depressive symptoms dropped for heavy users of substances excluding meth, from a median predicted CES-D score of 16.4 to 13.8. In contrast, over the same follow-up period, rates of depressive symptoms rose among heavy meth users, from 22.2 to 24.1.
The UCLA team concluded that depressive symptom prevalence is relatively high in this cohort of MSM with or at risk for HIV infection, especially among substance users. They proposed that "reducing substance use and methamphetamine in particular may reduce harms from related depressive symptoms and other co-occurring issues such as sexual risk behaviors."
References
1. Javanbakht M, Shoptaw S, Ragsdale A, Gorbach PM. Depressive symptoms and substance use: Changes overtime among a cohort of HIV-positive and HIV-negative MSM. 10th IAS Conference on HIV Science (IAS 2019), July 21-24, 2019, Mexico City. Abstract WEPED779. For e-poster: https://programme.ias2019.org//PAGMaterial/eposters/4344.pdf
2. Cholera R, Pence BW, Bengtson AM, et al. Mind the gap: gaps in antidepressant treatment, treatment adjustments, and outcomes among patients in routine HIV care in a multisite U.S. clinical cohort. PLoS One. 2017;12:e0166435.
3. Grelotti DJ, Hammer GP, Dilley JW, et al. Does substance use compromise depression treatment in persons with HIV? Findings from a randomized controlled trial. AIDS Care. 2017;29:273-279.
4. The mSTUDY. Why is HIV impacting our communities more than others? themstudy.org.


|
| |
|
 |
 |
|
|