 |
 |
 |
| |
Comorbidities Canadians: >70 HIGH Rates
|
| |
| |
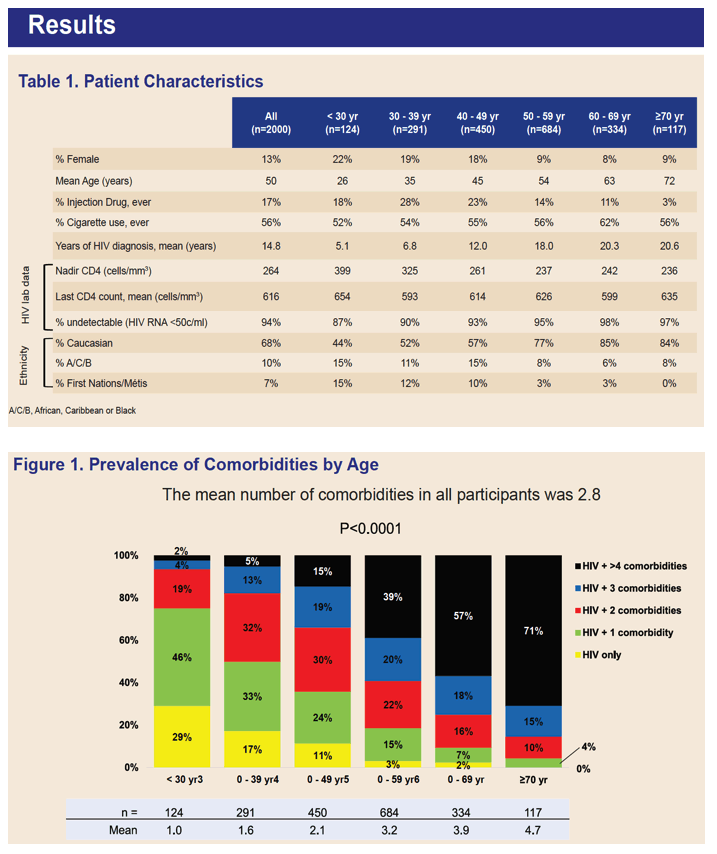
- 97% undetectable Viral Load, nadir cd4 235, 635 current CD4
• 71% over 70 years old had >4 Comorbidities. (Figure 1)
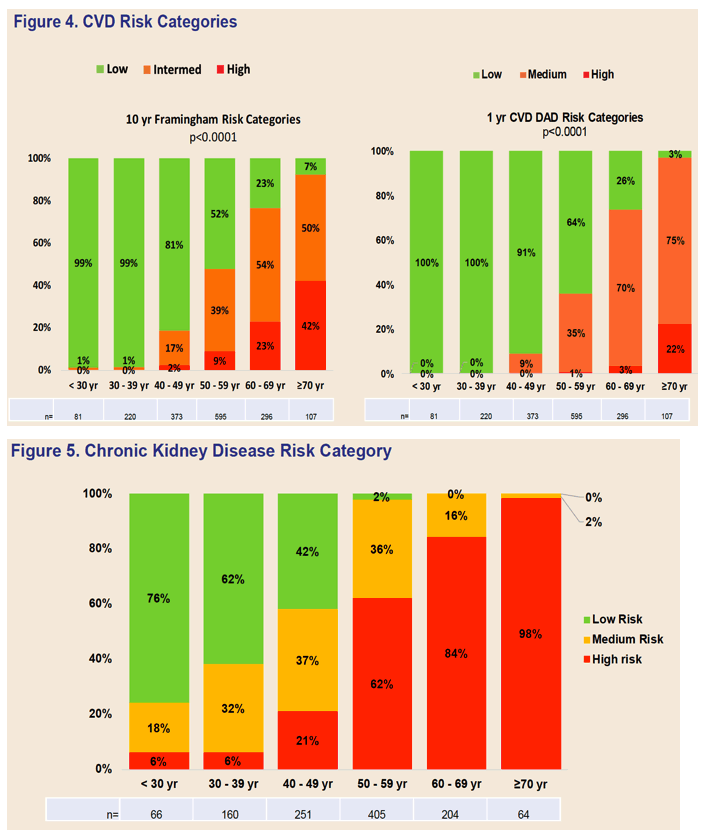
• 98% over 70 years old had High risk kidney disease (figure 5), 84% 60-69
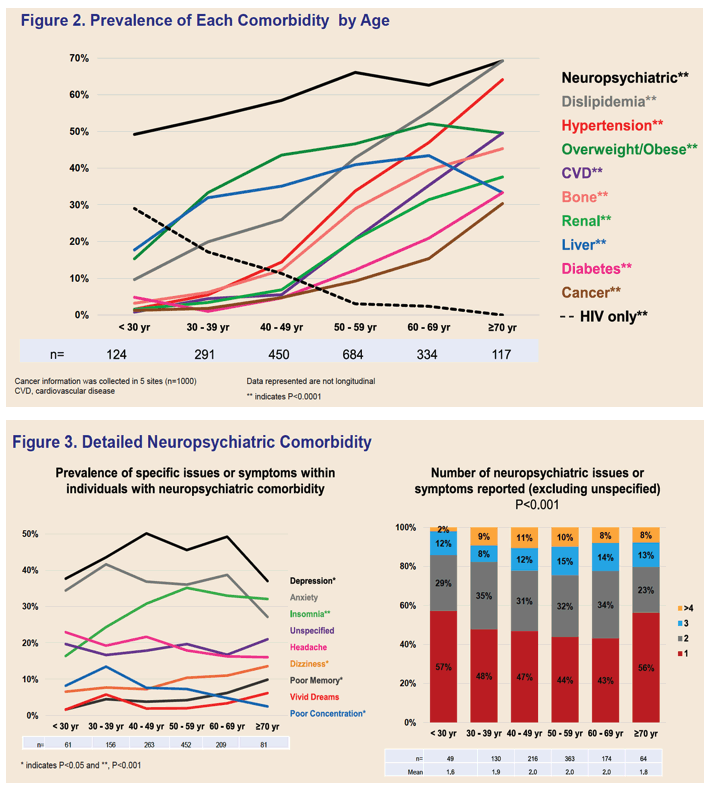
• HIV+ >70: 70% had neuropsychiatric & lipids comorbidities;
• 63% hypertension; 50% cardiovascular disease - 22% to 42% high risk CVD, 93% to 97% medium or high risk CVD (figure 4);
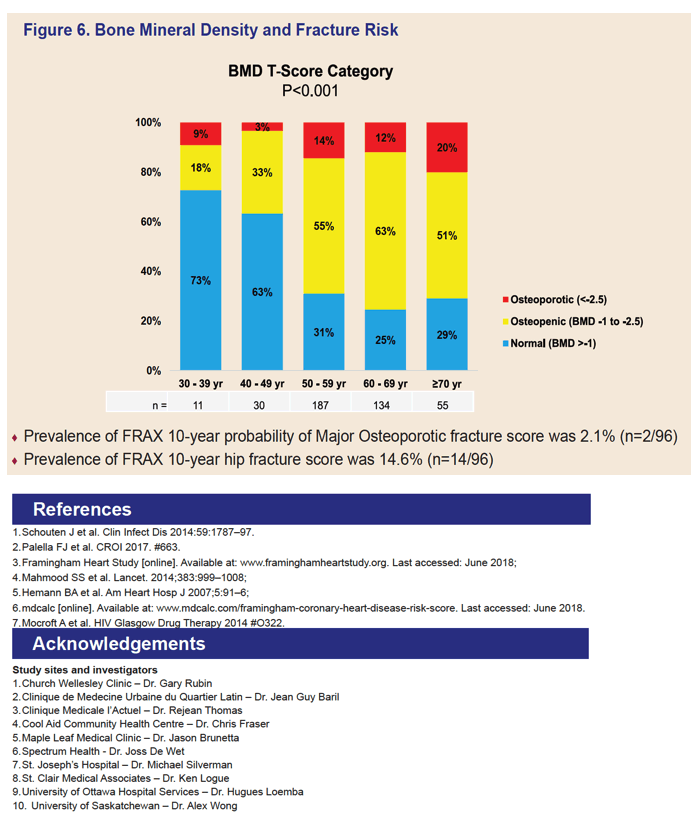
• 37% depression; 27% anxiety; 10% poor memory; 15% dizziness; 8% vivid dreams (figure 3); 20% bone disease: osteopenia or osteoporosis (figure 6)

Characterizing Canadians living with HIV to improve management of comorbidities
J. Brunetta1, G. Rubin2, A. Wong3, R. Thomas4, J. De Wet5, H. Loemba6, C. Fraser7, J.G. Baril8, K. Logue9, M. Silverman10, J. Palmart11, R.P. Lorgeoux12, H. Tossonian12, C. Kim12
1Maple Leaf Medical Clinic, Toronto, Canada, 2Church Wellesley Health Center, Toronto, Canada, 3University of Saskatchewan, Regina, Canada, 4Clinique Medicale l'Actuel, Montreal, Canada, 5Spectrum Health, Vancouver, Canada, 6University of Ottawa Health Services, Ottawa, Canada, 7Cool Aid Community Health Centre, Victoria, Canada, 8Clinique de Médecine Urbaine du Quartier Latin, Montreal, Canada, 9St. Clair Medical Associates, Toronto, Canada, 10St. Joseph's Hospital, London, Canada, 11Advisory Physicians Research Services Inc., Sooke, Canada, 12Gilead Sciences Canada, Toronto, Canada
Background: Management of non-HIV related comorbidities in persons living with HIV (PLHIV) is an important concern since PLHIV experience disproportionately high comorbidity rates.
Methods: This retrospective analysis characterized 200 most recently seen PLHIV in each of 10 Canadian HIV clinics via chart review. Data on demographics, comorbidities and lab results were collected, and risk categories of developing chronic kidney disease (CKD), cardiovascular disease (CVD) and fractures were calculated by D:A:D, Framingham, and FRAX equations. Sub-analyses compared younger (< 50 years) vs older individuals (•50 years) using Cochran-Mantel-Haenszel testing.
Results: Most persons were Caucasian (68%), male (87%) with a median age of 52 (57% •50 years). The median CD4 count was 583 cells/uL and nearly all (97%) had HIV-RNA < 400 copies/mL.
Comorbidities were common (mean of 2.8/person; 31% had •4); only 8% of patients had no documented comorbidity.
Frequent comorbidities included central nervous system (61%), overweight/obesity (43%), hepatic (37%), dyslipidemia (37%), hypertension (27%), bone (23%), CVD (18%), and renal (17%). Although younger patients (n=865) were less likely to have comorbid conditions than older patients (n=1135; 16% vs 3%; p< 0.001), 54% had •2 comorbidities. Of note, older individuals were 4.8-times more likely to have •4 co-morbidities compared to younger patients (48% vs 10%).
Risk stratification revealed that 48% had high-risk CKD scores (n=554/1150), while 47% had medium/high CVD risk score (n=782/1672). Older patients were 5.2 and 13.5-fold more likely to score high for CKD (72% vs 14%) and CVD (18% vs 1.3%) than younger patients, respectively.
were osteoporotic. Using FRAX (n=96), 15% of patients were at high risk of hip fractures and 2.1% for major osteoporotic fractures.
Conclusions: Routine clinical practice should be optimized to prevent and manage the high rates of comorbidities and risks Canadian PLHIV are experiencing, especially in aging patients.


|
| |
|
 |
 |
|
|