 |
 |
 |
| |
The Utility of Olfactory Function in Distinguishing Early Stage Alzheimer's Disease from HIV-associated Neurocognitive Disorder: A Pilot Study........"supports that these PLWH may be on an AD-like cognitive trajectory"
|
| |
| |
----
From Jules: it is accepted that aging older HIV+ have problem with sensory nervous system decline, although not discussed very much and not well appreciated by patients community, but many older aging HIV+ suffer decline in their sensory nerves. Unfortunately much of the complicated science surrounding HIV & aging is ignored by the advocates & patient communities, it gets very little attention, and the suffering & need for better care & support services of many older HIV+ also gets little attention by advocates, and federal & local HIV officials, and at key agencies CDC, HRSA, RWCA, HHS:
The sensory nervous system is a part of the nervous system responsible for processing sensory information. A sensory system consists of sensory neurons (including the sensory receptor cells), neural pathways, and parts of the brain involved in sensory perception. Commonly recognized sensory systems are those for vision, hearing, touch, taste, smell, and balance. In short, senses are transducers from the physical world to the realm of the mind where we interpret the information, creating our perception of the world around us.[1]
The olfactory system, or sense of smell, is the part of the sensory system used for smelling (olfaction). Most mammals and reptiles have a main olfactory system and an accessory olfactory system. The main olfactory system detects airborne substances, while the accessory system senses fluid-phase stimuli.
The senses of smell and taste (gustatory system) are often referred to together as the chemosensory system, because they both give the brain information about the chemical composition of objects through a process called transduction.
----------------------------
NOTE:

10th International Workshop on HIV and Aging, October 10-11, 2019, New York
Reported by Jules Levin
Erin E. Sundermann, PhD
HIV Neurobehavioral Research Center, UC San Diego
HIV & Aging International Workshop 2019
New York, NY

Program abstract
The utility of olfactory function in distinguishing early stage Alzheimer's disease from HIV-associated neurocognitive disorder: a pilot study
Sundermann E1
1University Of California, San Diego, La Jolla, United States
Background: Given the rising rate of older people living with HIV (PLWH), it becomes important to differentiate Alzheimer's disease (AD) and its precursor, amnestic mild cognitive impairment (aMCI) from HIV-Associated Neurocognitive Disorders (HAND). Identifying aMCI among PLWH is challenging given the overlap in neurocognitive profiles between aMCI and HAND. There are, however, differences between aMCI/AD and HAND that may allow us to distinguish between the conditions. In this preliminary study, we examined whether olfactory function could contribute to distinguishing between aMCI/AD and HAND since olfactory dysfunction represents one of the earliest signs of AD and tends to be specific to AD versus other age-associated dementias.
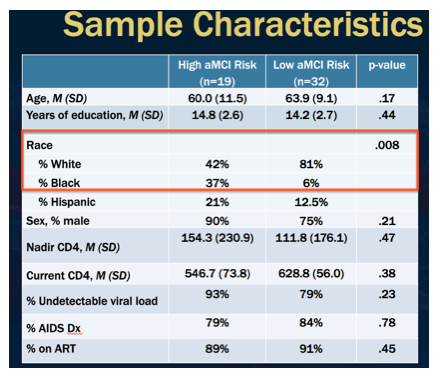
Materials & Methods: We assessed 51 HIV-seropositive participants (mean age=62.4, [SD=10.1], mean education=14.4yrs [SD=2.7], 80% male, 67% White) from the California NeuroAIDS Tissue Network that were administered the University of Pennsylvania Smell Identification Test (UPSIT; higher scores=better smell identification) and the Story Recall Test. In the Story Recall Test, participants learned a 20-unit story to 90% criterion (i.e., 18 out of 20 units) and then completed free recall and recognition trials at 30-minute (in-person) and 1-week (via telephone) delays. In addition, participants completed a standard, comprehensive seven-domain neuropsychological battery and a neuromedical evaluation. Participants were classified as HAND+ versus HAND- according to Frascati criteria. Participants were also classified as aMCI/AD+ versus aMCI/AD- based on an adapted diagnostic schema for aMCI (Jak/Bondi), which requires impairment (>1.0 SD below demographically-corrected normative mean) on two tests of memory recall and/or recognition (at least one recognition impairment required) from the Hopkins Verbal Learning Test-Revised (HVLT-R) and the Brief Visuospatial Memory Test-Revised (BVMT-R). Differences in UPSIT scores between the aMCI/AD and HAND groups were examined while adjusting for age, education, sex, race/ethnicity and any clinical or HIV disease characteristic that differed by aMCI group (i.e., lifetime major depressive disorder). We also examined correlations between UPSIT scores and Story Recall Test scores.
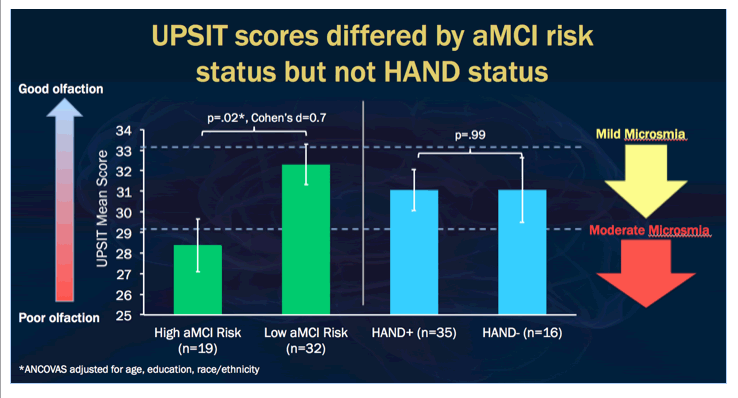
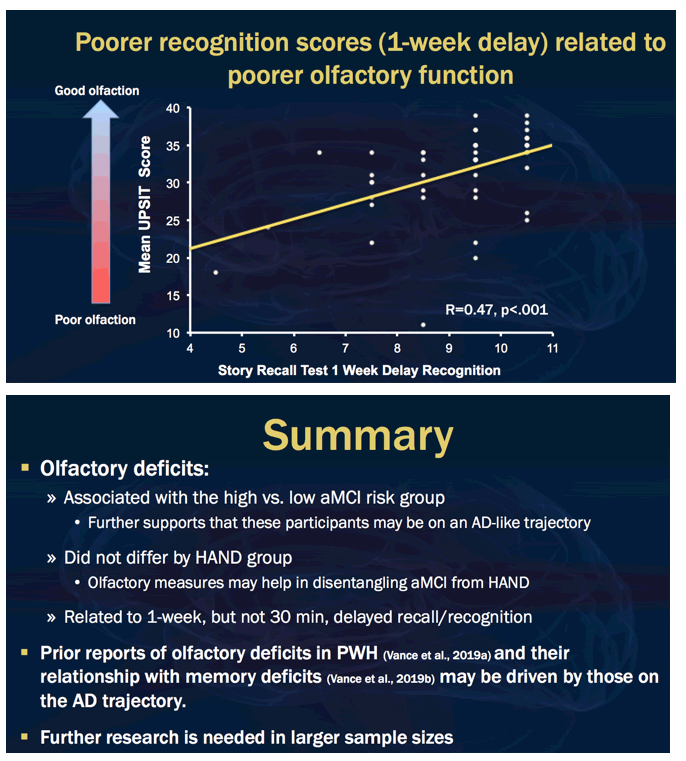
Results: Sixty-eight percent of participants were classified as HAND+ (n=34) and 37% were classified as aMCI/AD+ (n=19; 95% HAND). UPSIT scores were significantly lower in the aMCI/AD+ versus the aMCI/AD- group (F[1,48]=5.7, p=.02, Cohen's d=0.7), but did not differ between HAND groups (p=.99). Among the Story Recall Test outcomes, UPSIT scores showed a moderate correlation with lower 1-week recognition scores (R=0.48, p<.001).
Conclusions: The aMCI/AD+ group showed olfactory deficits relative to the aMCI/AD- group, which further supports that these PLWH may be on an AD-like cognitive trajectory. Olfactory function correlated with 1-week story recognition and differed between aMCI/AD groups, but not HAND groups. Results suggest that olfactory assessments may help in detecting early aMCI/AD that exists among PLWH, and may allow for more targeted and appropriate interventions in early disease stages.



|
| |
|
 |
 |
|
|