 |
 |
 |
| |
Fibrosis Progression Over 6-Fold
Higher in NAFLD With vs Without HIV
|
| |
| |
CROI 2020, March 8-11, 2020, Boston
Mark Mascolini
Liver fibrosis progression rate proved more than 6-fold greater in people with HIV and nonalcoholic fatty liver disease (NAFLD) than in the general NAFLD population [1]. Visceral adiposity predicted fibrosis progression in this analysis of participants in a small randomized trial.
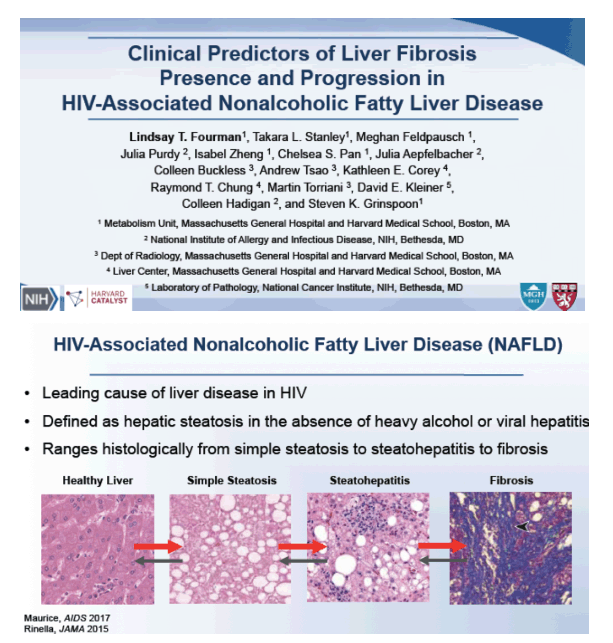
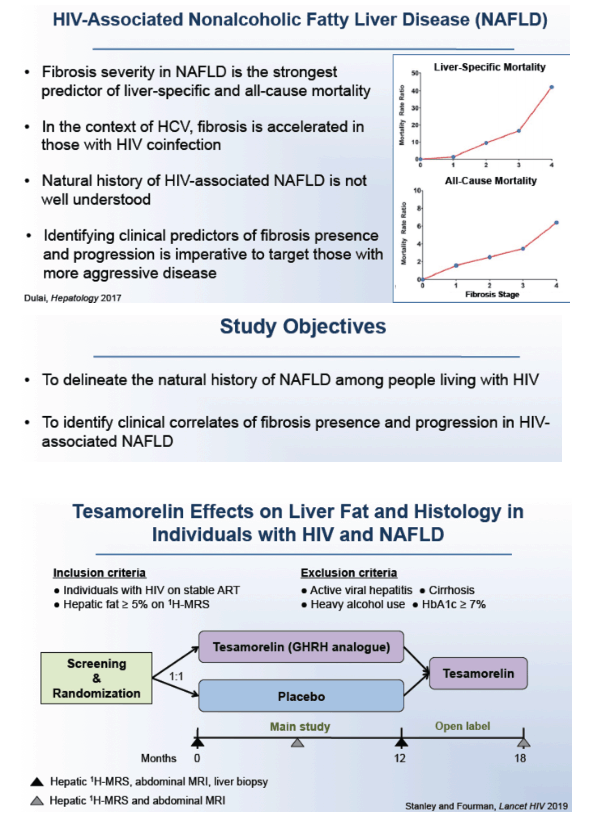
NAFLD remains a prime cause of liver disease in people with HIV infection. Fibrosis severity emerged as the strongest predictor of liver-specific and all-cause mortality with NAFLD in the general population [2]. Because the natural history of HIV-associated NAFLD remains poorly understood, a group at Massachusetts General Hospital and other centers conducted this study to pinpoint clinical predictors of fibrosis presence and progression to help target those at risk with more aggressive therapy.
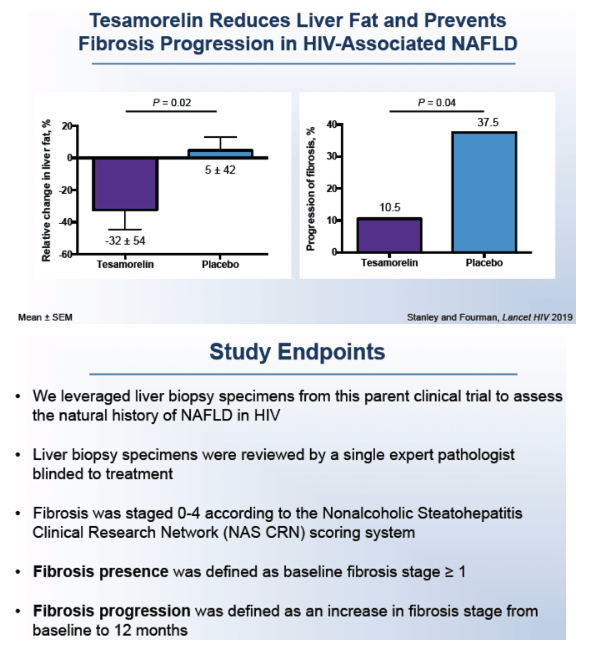
The study involved HIV-positive people with fatty liver randomized to tesamorelin or placebo in a trial that excluded people with active viral hepatitis, cirrhosis, or heavy alcohol use [3]. After 12 months tesamorelin had significantly reduced liver fat and dampened fibrosis progression compared with placebo.
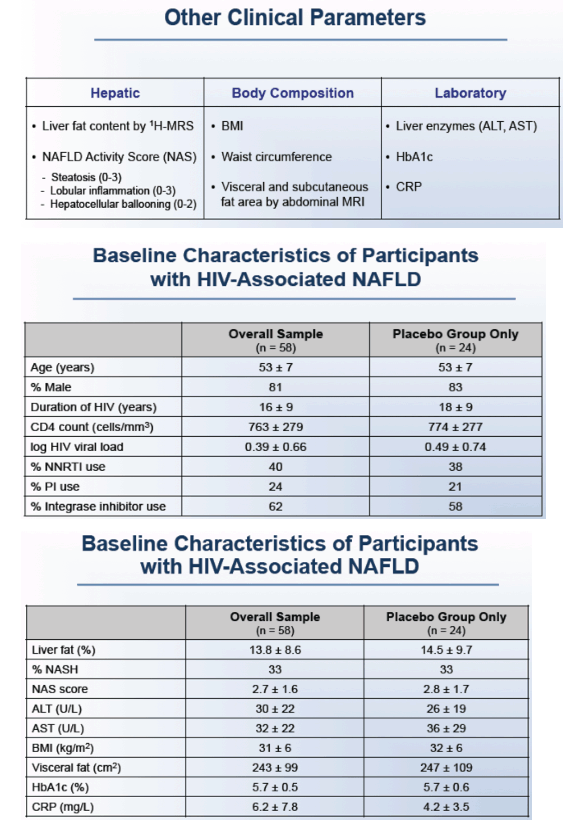
The Mass General team defined fibrosis presence as fibrosis stage 1 or greater. Fibrosis progression meant an increase in fibrosis stage from baseline to month 12. The study included 58 people with HIV-associated NAFLD, 47 of them (81%) men. The group averaged 53 years in age and had diagnosed HIV infection for an average 16 years. Their CD4 count averaged 763.
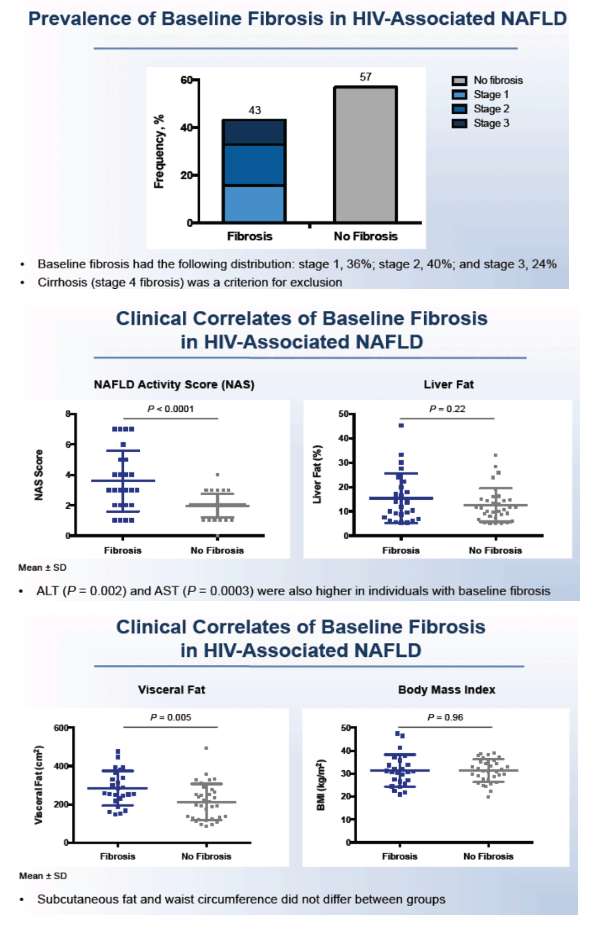
Twenty-five people (43%) had fibrosis at baseline, and of them 36% had stage 1 fibrosis, 40% stage 2, and 24% had stage 3. No one had stage 4 fibrosis (cirrhosis) because the trial excluded people with cirrhosis. Compared with participants without fibrosis, those with fibrosis had a significantly higher NAFLD activity score (P < 0.0001), higher ALT (P = 0.002), and higher AST (P = 0.0003) but similar liver fat levels. Visceral fat was significantly greater in people with than without NAFLD (P = 0.005), but body mass index did not differ between the two groups.
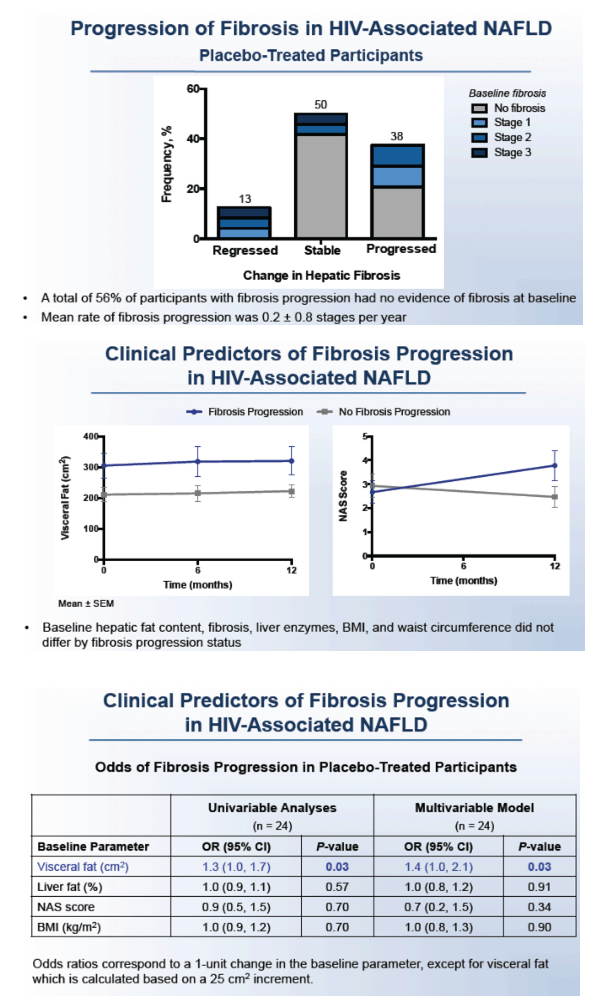
Among 24 people randomized to placebo, 38% had fibrosis progression, 50% had stable liver fibrosis, and 13% had regression. This fibrosis progression rate is more than 6-fold higher than in reports of NAFLD-related fibrosis in the general population. More than half of people with fibrosis progression, 56%, had no baseline evidence of fibrosis. For the group fibrosis progressed at an average rate of 0.2 stages per year.
People with versus without fibrosis progression could not be distinguished by baseline liver fat content, baseline fibrosis, liver enzymes, body mass index, or waist circumference. Among baseline variables in placebo-treated people, a multivariate model singled out only one independent predictor of fibrosis progression: every cm2 greater visceral fat level at baseline raised odds of fibrosis progression 40% (odds ratio 1.4, 95% confidence interval 1.0 to 2.1, P = 0.03). Nonpredictive variables in this analysis were percent liver fat, NAFLD activity score, and body mass index.
Three lab measures increased significantly with versus without fibrosis progression: NAFLD activity score (P < 0.0001), percent HbA1c (P = 0.02), and C-reactive protein (P = 0.02). Changes in hepatic fat content or liver enzymes did not differ by fibrosis progression status.
The researchers believe this is the first longitudinal assessment of HIV-associated NAFLD in a well-defined population. Because visceral adiposity emerged as the only clinical predictor of fibrosis progression, the investigators suggested that "therapies to reduce visceral fat may be particularly effective in HIV-associated NAFLD."
References
1. Fourman LT, Stanley TL, Feldpausch M, et al. Clinical predictors of liver fibrosis presence and progression in HIV-associated NAFLD. Conference on Retroviruses and Opportunistic Infections (CROI). March 8-11, 2020. Boston. Abstract 128.
2. Dulai PS, Singh S, Patel J, et al. Increased risk of mortality by fibrosis stage in nonalcoholic fatty liver disease: Systematic review and meta-analysis. Hepatology. 2017;65:1557-1565. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5397356/
3. Stanley TL, Fourman LT, Feldpausch MN, et al. Effects of tesamorelin on non-alcoholic fatty liver disease in HIV: a randomised, double-blind, multicentre trial. Lancet HIV. 2019;6:e821-e830. http://www.natap.org/2019/HIV/PIIS2352301819303388.pdf


|
| |
|
 |
 |
|
|