 |
 |
 |
| |
Mortality 4-Fold Higher With HIV in Canadian Group--in Sync With Comorbidity Tally
|
| |
| |
"Excess mortality among PLWH with multimorbidity compared to HIV-negative controls"
CROI 2020, March 8-11, 2020, Boston
Mark Mascolini
Age-standardized all-cause mortality proved more than 4-fold higher in a British Columbia group with HIV than in a matched HIV-negative group [1]. Excess mortality with versus without HIV held true in people with 0, 1, 2, or 3 or more comorbidities.
Researchers in the Canadian province of British Columbia set out to compare prevalence of multimorbidity and all-cause mortality in people with HIV and HIV-negative people grouped by neighborhood income level. They also planned to weigh the impact of multimorbidity on all-cause mortality in people with HIV and figure which comorbidities led to higher mortality with HIV. Antiretroviral therapy is free in British Columbia.
The analysis began with HIV-positive adults matched 1-to-4 by age and sex to HIV-negative people. All participants were at least 19 years old and enrolled for at least 1 year in the Comparative Outcomes and Service Utilization Trends (COAST) cohort study between 2001 and 2012. The researchers used marginal structural models adjusted for key time-varying confounders to estimate risk of all-cause mortality in people with HIV and 1, 2, or 3 or more comorbidities versus no comorbidities. Those confounders, measured every year, were age, lowest CD4 count, viral suppression, antiretroviral-naive status, and antiretroviral adherence. Time-fixed confounders were sex at birth, HIV risk group, and antiretroviral initiation era.
The study had 8031 people with HIV and 32,124 HIV-negative people with a median baseline age of 40 years. Median follow-up measured 9 years in the HIV group and 11 years in the HIV-negative group. Most participants, 82%, were men.
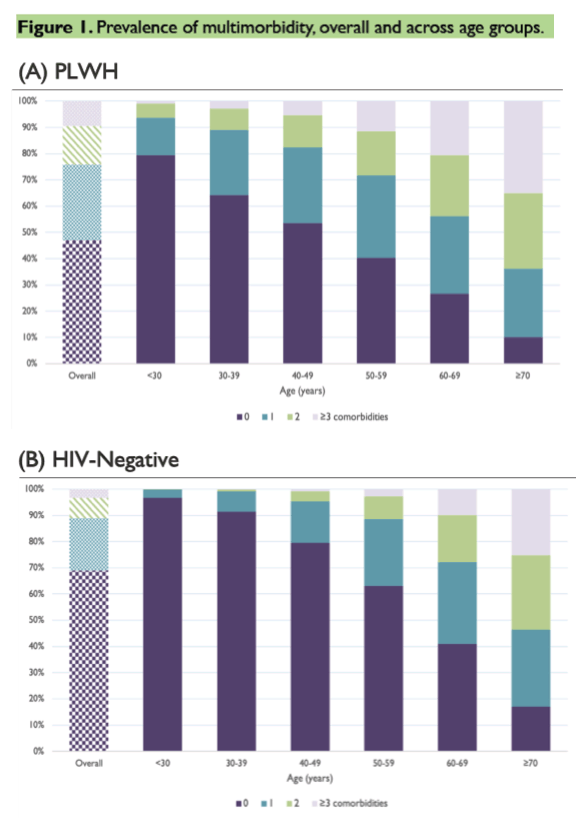
Analysis of 10-year age groups found consistently higher multimorbidity rates in people with HIV--rates comparable to those of HIV-negative people 10 to 20 years older than the HIV groups. For example, among 50- to 59-year-old people with HIV, about 60% had 1 or more comorbidities, compared with about 40% of people that age without HIV. The 60- to 69-year-old HIV-negative group had a comorbidity rate similar to the 50- to 59-year-old HIV group.
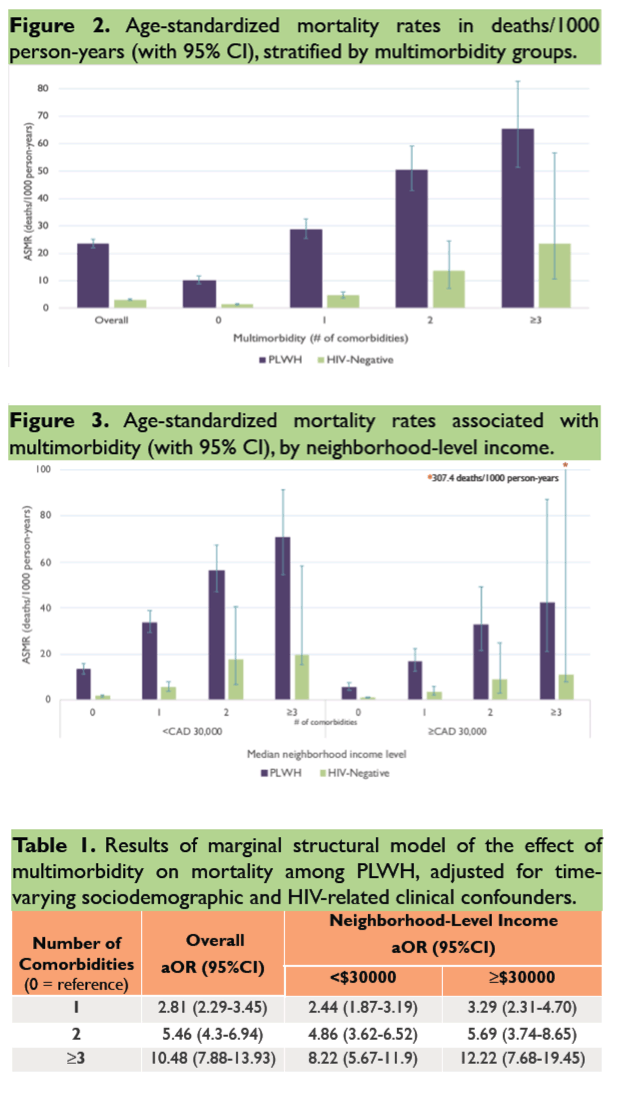
Overall age-standardized mortality proved higher in people with than without HIV (just above 20% versus less than 5%). And this higher mortality held true in (1) subgroups with 0, 1, 2, or 3 or more comorbidities and (2) HIV-positive and negative people with the same number of comorbidities and the same neighborhood income level. The three comorbidity pairs linked to the highest mortality were cancer-liver disease, cancer-chronic obstructive pulmonary disease (COPD), and cancer-kidney disease.
Among people with HIV, compared with no comorbidities, those with 1 comorbidity had almost tripled odds of death (adjusted odds ratio [aOR] 2.81, 95% confidence interval [CI] 2.29 to 3.45), those with 2 comorbidities had more than 5-fold higher odds of death (aOR 5.46, 95% CI 4.3 to 6.94), and those with 3 or more comorbidities had more than 10-fold higher odds of death (aOR 10.48, 95% CI 7.88 to 13.93). These associations remained consistent when the researchers further classified HIV-positive participants by neighborhood income below or above $30,000 yearly.
Compared with HIV-negative people with a similar socioeconomic status, the researchers concluded, people with HIV have substantially higher multimorbidity rates and associated mortality. Odds of mortality rose in tandem with the number of comorbidities people had. The British Columbia team believes their findings "highlight the critical role that additional comorbidities pose as drivers of morbidity and mortality in people living with HIV within a publicly funded antiretroviral therapy program."
Reference
1. Nanditha NGA, Zheng G, Tafessu HM, et al. Excess mortality among PLWH with multimorbidity compared to HIV-negative controls. Conference on Retroviruses and Opportunistic Infections (CROI). March 8-11, 2020. Boston. Abstract 869.
--------------------------------
Excess Mortality among PLWH with Multimorbidity Compared To HIV-Negative Controls:
A Population-Based Cohort Study in British Columbia, Canada
Session: P-Q04
Life Expectancy and Mortality
Ni Gusti Ayu Nanditha1,2, Grace Zheng2, Hiwot M. Tafessu1, Taylor McLinden1, Andreea Bratu1, Robert S. Hogg1, Julio S. G. Montaner1,2, Viviane D. Lima1,2
1British Columbia Centre for Excellence in HIV/AIDS; 2University of British Columbia, Faculty of Medicine -Vancouver, Canada
dnanditha@cfenet.ubc.ca



|
| |
|
 |
 |
|
|