 |
 |
 |
| |
EXPLOSIVE HIV AND HCV EPIDEMICS
DRIVEN BY NETWORK VIREMIA AMONG PWID
|
| |
| |
from Jules: this study along with 2 studies from CROI I reported yesterday & day before which highlighted 44% of PWIDs in USA with HCV & 38% in SF from van testing - these show the underestimates of HCV & the high barrier & unrecognized challenges to Ending The Epidemic globally for HIV and HCV.
See attached pdf for full slide presentation
Download the PDF here
http://www.croiwebcasts.org/console/player/44836?mediaType=slideVideo&


CROI 2020
Reported by Jules Levin
Steven J. Clipman1, Shruti H. Mehta1, Aylur K. Srikrishnan2, Katie J. Zook3, Priya Duggal1, Shobha Mohapatra2, Shanmugam Saravanan2, Nandagopal Paneerselvam2, Muniratn
1Johns Hopkins Bloomberg School of Public Health, Baltimore, MD, USA,2YR Gaitonde Center for AIDS Research and Education, Chennai, India,3Johns Hopkins University School of Medicine, Baltimore, MD, USA
Program Abstract
While much attention has focused on the US opioid crisis, misuse of opioids is rapidly becoming a global epidemic with >80% of drug seizures in Africa/Asia in part due to increased use of opioids to manage pain and expansion of heroin trafficking routes. Little is known about the drug using networks in these settings which contribute to HIV/HCV transmission.
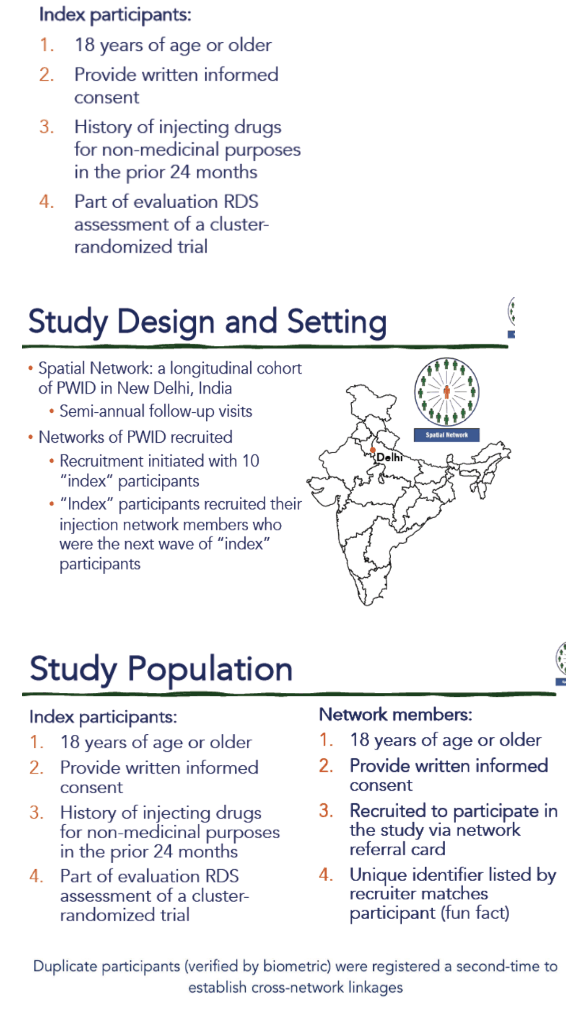
2512 people who inject drugs (PWID) in New Delhi, India were recruited (2017-19) into a cohort by a chain referral approach. Index participants were asked to name and recruit people they injected with in the past month (egocentric network of the index). Each recruit was asked to name and recruit their recent injection network members (egocentric network of recruit; sociometric network of index). Biometrics were used to identify duplicates and cross-network linkages. Participants underwent a survey and blood draw semi-annually. Blood was tested for HIV and HCV antibodies, HIV RNA and HCV RNA. Network viral load was calculated as the number of egocentric network members with HIV RNA>150 copies/ml. Poisson regression was used to identify predictors of incident HIV.
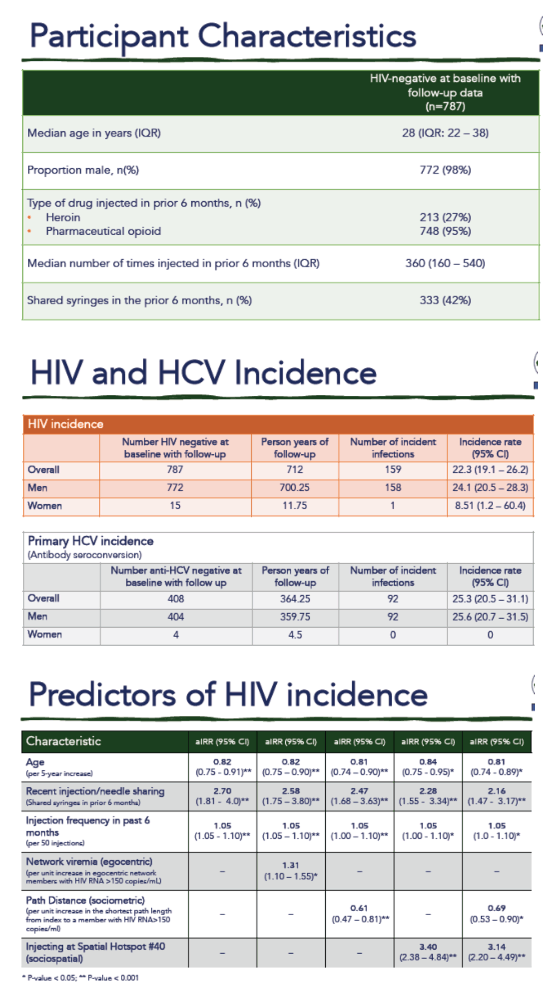
At baseline, 36.9% had HIV infection of whom only 7.4% were virologically suppressed;
HCV prevalence was 65.1%; recent heroin and other opioid use were 26.6% and 95.3%, respectively.
Among 1,066 with at least one follow-up as of 9/1/19, 96 seroconversions were observed in 370 person-years (p-y) (HIV incidence: 25.9 per 100 p-y); 64 HCV antibody seroconversions were observed in 188 p-y (primary HCV incidence: 34.0 per 100 p-y). Of 96 incident HIV cases, 74% were directly connected to at least one viremic person in their egocentric network (Figure). In multivariable analysis adjusting for recent needle sharing and injection frequency, HIV incidence increased by 23% per unit increase in egocentric network member with detectable HIV RNA (incidence rate ratio [IRR]: 1.23; p<0.01); further, every increased step in the path between a participant and a sociometric network member with detectable HIV RNA decreased HIV incidence by 37% (IRR: 0.63; p<0.01).
We observed explosive HIV and HCV epidemics among PWID in New Delhi, largely driven by exposure to viremic individuals in both egocentric and sociometric networks, highlighting the importance of achieving broad viral suppression in order to curb transmission. Expanding treatment and prevention efforts in such disenfranchised populations will be critical for epidemic control.



|
| |
|
 |
 |
|
|