 |
 |
 |
| |
HPTN 078: HIGH INCIDENCE OF HEPATITIS C VIRUS INFECTIONS AMONG MSM
|
| |
| |
CROI 2020
Reported by Jules Levin
Risha Irvin1, Jowanna Malone1, Theresa Gamble2, James Hughes3, Jason Farley1, Kenneth H. Mayer4, Carlos del Rio5, D. Scott Batey6, Michael Murphy1, Oliver L
1Johns Hopkins University, Baltimore, MD, USA,2FHI 360, Durham, NC, USA,3University of Washington, Seattle, WA, USA,4Harvard Medical School, Boston, MA, USA,5Emory University, Atlanta, GA, USA,6University of Alabama at Birmingham, Birmingham, AL, USA,7Columbia University, New York, NY, USA
Abstract Body:
Annual hepatitis C virus (HCV) testing is recommended in HIV-infected (HIV+) men who have sex with men (MSM) due to sexual transmission risk. While there is no HCV testing guideline for HIV-uninfected MSM, incident HCV infections have been noted. More data on incident HCV infection in MSM are needed.
HPTN 078 assessed the efficacy of an integrated strategy to achieve HIV viral suppression; MSM were screened using respondent driven sampling and direct recruitment to identify HIV+ MSM who were not in care in Atlanta, Birmingham, Baltimore and Boston. At screening, demographic and behavioral questionnaires were completed, along with HIV and HCV testing. To identify subjects with recent HCV infection, HCV antibody (Ab) and RNA+ samples were tested using a modified Green Cross antibody avidity assay. Incidence rate was calculated using the Assay-Based Incidence Estimation Model. Phylogenetic analysis was used to assess clustering. Univariable logistic regression was used to evaluate associations with recent HCV infection.
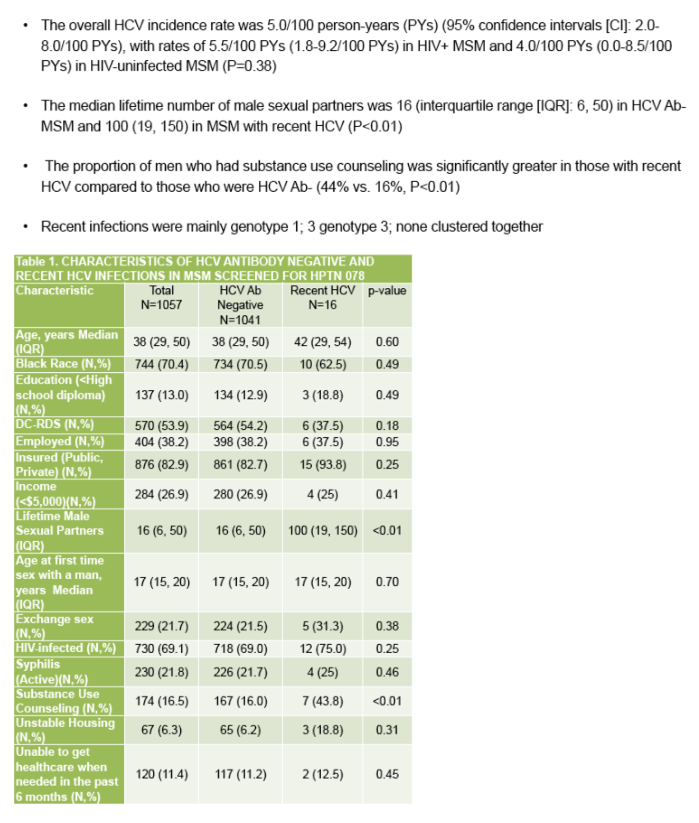
This study included 1041 HCV Ab- MSM and 96 HCV Ab+/HCV RNA+ MSM who were tested for recent infection. Of the 96, 16 had a recent infection (12 HIV+), so further analyses were restricted to these 16 plus the 1041 HCV Ab- MSM. Of these 1057 men, median age 38 years, 70% Black, 83% insured, 38% employed, and 69% HIV+ (Table 1). The overall HCV incidence rate was 5.0/100 person-years (PYs) (95% confidence intervals [CI]: 2.0-8.0/100 PYs), with rates of 5.5/100 PYs (1.8-9.2/100 PYs) in HIV+ MSM and 4.0/100 PYs (-0.4-8.5/100 PYs) in HIV-uninfected MSM (P=0.38). The median lifetime number of male sexual partners was 16 (interquartile range [IQR]: 6, 50) in HCV Ab- MSM and 100 (19, 150) in MSM with recent HCV (P<0.01). The proportion of men who had substance use counseling was significantly greater in those with recent HCV compared to those who were HCV Ab- (44% vs. 16%, P<0.01). These associations were similar in the HIV+ group. Recent infections were mainly genotype 1; 3 genotype 3; none clustered together.
Although recent HCV infection was more common in HIV+ than in HIV-uninfected MSM, it was higher in both groups than in other studies. This suggests that HCV risk counseling should be considered in both HIV+ and HIV-uninfected MSM, particularly in those with a high number of lifetime sexual partners and substance use. Integrating HCV prevention into substance use counseling should be explored.


|
| |
|
 |
 |
|
|