 |
 |
 |
| |
HCV INCIDENCE AMONG HIV-INFECTED MSM IN FRANCE: RESULTS FROM THE FHDH-ANRS CO4 COHORT
|
| |
| |
CROI 2020
Reported by Jules Levin
Mathieu Castry1, Anthony Cousien1, Jonathan Bellet1, Karen Champenois1, Gilles Pialoux2, Yazdan Yazdanpanah3, Dominique Costagliola1, Sophie Grabar1, Sylvie Deuffic-Bu
1INSERM, Paris, France,2Tenon Hospital, Paris, France,3AP–HP, Hôpital Bichat-Claude Bernard, Paris, France
Program Abstract
Despite the availability of highly effective directly acting antivirals (DAAs), sexual transmission of hepatitis C virus (HCV) in men who have sex with men (MSM) is still ongoing, associated with high-risk sexual behaviors. The objective of this study was to estimate the incidence of primary HCV infection among HIV-positive MSM in France in the post-DAA era.
We used data from a large French hospital cohort of HIV-positive individuals (FHDH-ANRS CO4) prospectively collected between 2014 and 2017. HCV infection rates were calculated using person-time methods, among HIV-positive MSM with a negative anti-HCV test at cohort entry and subsequent HCV tests. HCV negative status was assigned to individuals never testing HCV positive throughout follow-up, discontinued on December 31th 2017. Incident HCV infection was based on any positive HCV test (RNA and/or antibodies) during follow-up; the date of HCV infection was the midpoint between the last negative and first positive test. Individuals were considered lost to follow-up if they had no clinical visit for 18 months; follow-up was ceased 6 months after last clinical visit.
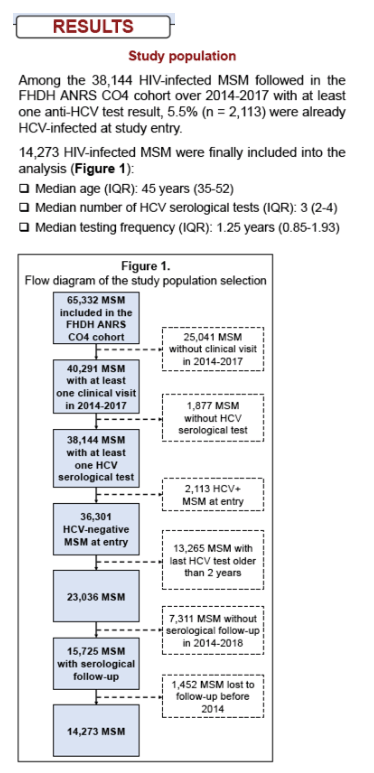
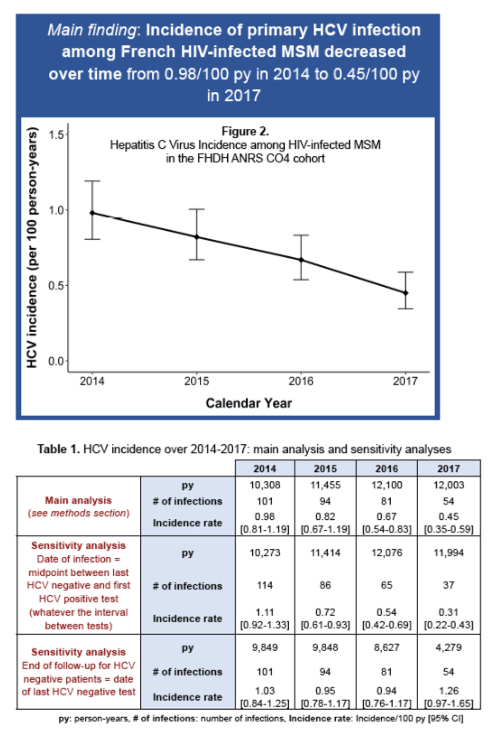
A total of 15,692 HIV-positive MSM were included. Their median age was 45 years (interquartile range (IQR): 35-52). The median number of HCV serology tests during follow-up for each individual was 3 (IQR: 2-4), with a median testing interval of 1.25 years (IQR: 0.85-1.93) between two tests. Overall, 330 incident HCV infections occurred over 45,866 person-years (py) of follow-up. Incidence of first HCV infection decreased significantly (p-trend=0.04) over time during the study period: 0.98/100py (2014), 0.82/100py (2015), 0.67/100py (2016) and 0.45/100py (2017). The stronger decrease occurred in 2017 (33% reduction from 2016 to 2017). In sensitivity analyses, similar trends were observed when the date of first positive HCV was used as a proxy for the time of infection, or when follow-up was ceased at the date of last clinical visit or 12 months after for patients lost to follow-up.
The observed decrease in primary HCV infections among HIV-infected MSM may be related to a concomitant and continuous scaling-up in DAA use, which was especially marked in HIV-HCV coinfected individuals. The declining trend may also be considered in parallel with the rising incidence of HCV infection recently reported among HIV-negative MSM receiving preexposure prophylaxis (PrEP), suggesting a transfer of the epidemic from the former to the latter.
Acute HCV & PrEP/MSM HIV+ & HIV-Neg http://www.natap.org/2019/HCV/011720_02.htm
HCV incidence in HIV-infected and in PrEP-using MSM - New HCV Rate Similar in HIV+ MSM and HIV- MSM on PrEP in France


|
| |
|
 |
 |
|
|