 |
 |
 |
| |
ANAL PRECANCER SCREENING AMONG MSM: WHAT IS THE BEST STRATEGY?
|
| |
| |
CROI 2020
Reported by Jules Levin
Jing Sun1, Dorothy J. Wiley2, Teresa Darragh3, Hilary K. Hsu2, Nancy Joste4, Stephen Young5, W. David Hardy6, Susheel Reddy7, Jeremy J. Martinson8, Gypsyamb
1Johns Hopkins Bloomberg School of Public Health, Baltimore, MD, USA,2University of California Los Angeles, Los Angeles, CA, USA,3University of California San Francisco, San Francisco, CA, USA,4University of New Mexico, Albuquerque, NM, USA,5Tricore Reference Laboratories, Albuquerque, NM, USA,6Johns Hopkins University School of Medicine, Division of Infectious Diseases, Washington, DC, USA,7Northwestern University, Chicago, IL, USA,8University of Pittsburgh, Pittsburgh, PA, USA
Abstract Body:
Risks of non-AIDS defining cancers has increased among people living with HIV since the advent of potent ART. Anal cancer is rare in the general population, but men who have sex with men (MSM) have elevated risk. We evaluated three screening strategies (single anal cytology [aCyt], sequential aCyt, and co-testing [aCyt plus oncogenic HPV]) and their ability to predict anal precancer (anal histological high-grade squamous intraepithelial grade 2+ [hHSIL/AIN2+]) among MSM.
1027 MSM from the Multicenter AIDS Cohort Study (MACS) had repeated aCyt and HPV testing. Men with abnormal aCyt and a subset with normal aCyt were referred for high-resolution anoscope (HRA). All men had HRA (N=430) within 5 years of their aCyt, 72% of HRAs performed in Pittsburg and LA study sites. Multivariable logistic regression models evaluated risk of AIN2+ within 5 years of screening using the three screening strategies adjusted for age, race, HIV status, number of anal sex partners, and study site. Sensitivity and specificity were calculated among participants who had HRA and results were corrected for potential verification bias (in all participants who had screening tests) using Begg and Greenes’s method.
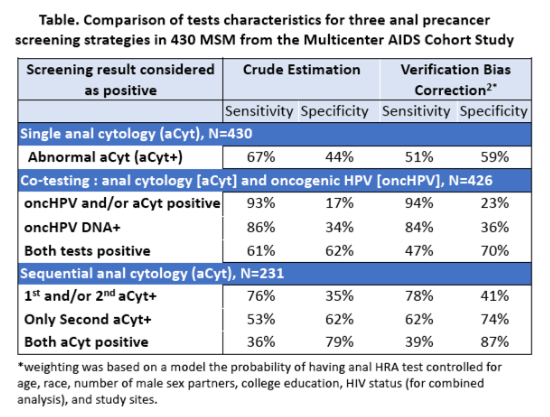
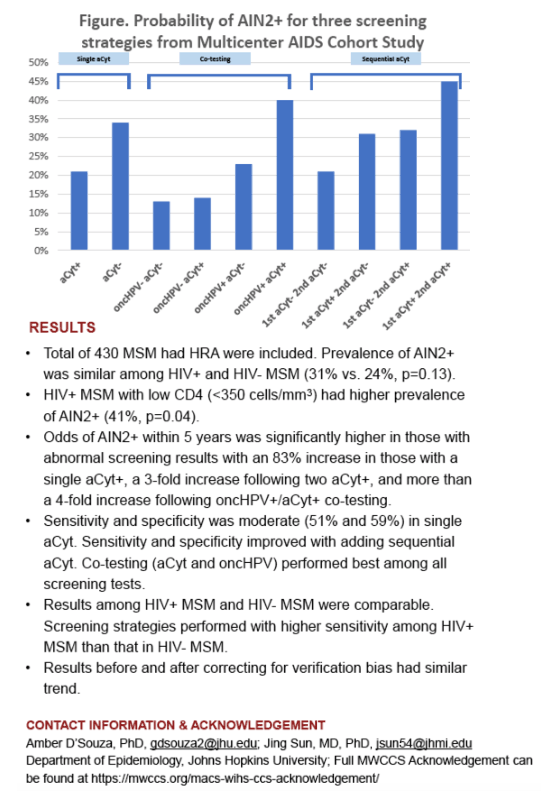
Among those who had HRA tests, the median age at time of HRA was 48 years, 70 % were HIV+, 81% non-Hispanic white, and 9% had CD4 cell count<350 (cells/mm3). Prevalence of AIN2+ was similar among HIV+ MSM than HIV- MSM (31% vs 24%, p=0.13), but was higher among the subgroup with CD4<350 (41%, p=0.04). Odds of AIN2+ was significantly higher in those with abnormal screening results with an 83% increase (95% CI: 1.1-3.04) in those with a single aCyt+, a 3-fold increase (95% CI: 1.33-7.11) following two aCyt+, and more than a 4-fold increase (95% CI: 1.93-10.29) following oncHPV+/aCyt+ co-testing. Specificity was low in single aCyt (44%) but increased with sequential aCyt testing (79%) or oncHPV co-testing (62%). Sensitivity was moderate in single aCyt+ (67%) or dual positive cotests (61%), and high in cotests where positivity on either marker was considered as positive (93%). Sensitivity was only 36% among those with sequential aCyt+ results. After correcting for potential verification bias, specificity increased but sensitivity reduced in all strategies.
Anal cytology screening had moderate specificity and sensitivity among HIV+ and HIV- MSM. Sequential aCyt testing or adding an HPV co-test to aCyt improved test performance.


|
| |
|
 |
 |
|
|