 |
 |
 |
| |
CLEARANCE OF HPV ANAL HIGH-GRADE INTRAEPITHELIAL LESIONS WITH LOW-DOSE POMALIDOMIDE
|
| |
| |
Pomalidomide Clears Anal Cancer Precursor in High Proportion With or Without HIV - (03/11/20)
CROI 2020
Reported by Jules Levin
Mark Polizzotto1, David Van Bockel1, Carmella Law2, Jennifer Roberts3, Susanne Just1, Griselda Buckland1, Simon Comben2, Mary Poynten1, Richard Hillman2, Ri
1Kirby Institute, Sydney, NSW, Australia,2St. Vincent's Hospital, Sydney, NSW, Australia,3Douglass Hanly Moir Pathology, Macquarie Park, Australia,4Mortimer Market Centre, London, UK,5MRC Clinical Trials Unit at UCL, London, UK
Abstract
People with HIV (PLWH) have an increased risk of anal cancer. This is preceded by high-grade squamous intraepithelial lesions (HSIL). Spontaneous clearance of HSIL is associated with systemic T-cell response to human papillomavirus (HPV) oncogene E6. Pomalidomide may enhance immune responses to HPV and be therapeutic in HSIL.
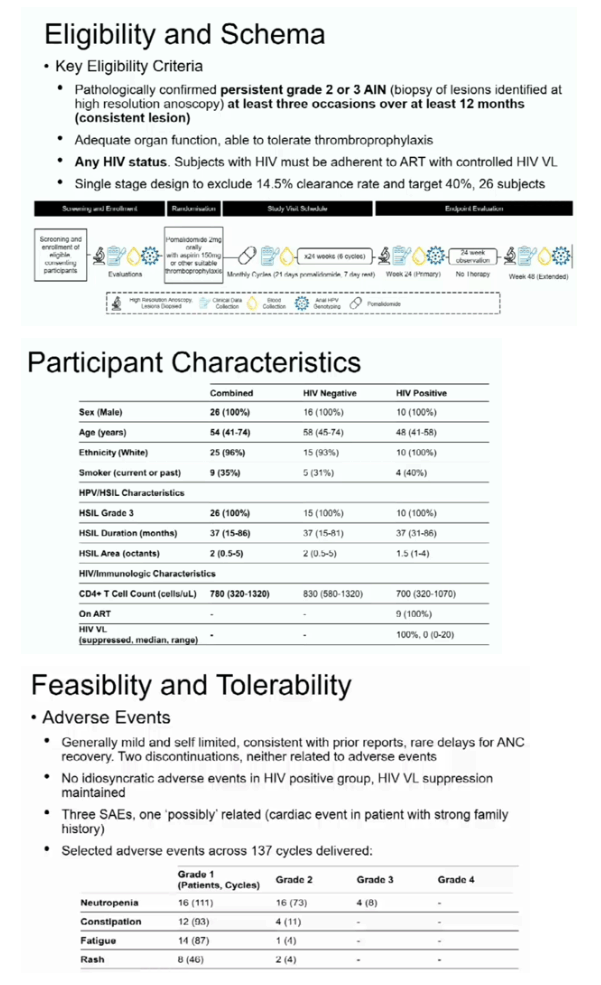
This phase II single centre study (NCT3113942) recruited participants with persistent (>12 months) biopsy-proven anal HSIL. Therapy was oral pomalidomide 2mg 21/28 days for 6 months. PLWH were eligible if on ART with viral load (VL)<200 copies/mL and CD4 count >200 cells/μL. Primary outcome was response at end therapy (CR defined as histological clearance; PR as ≥50% reduction in area); secondary included response after a further 6 months without therapy. Immune activation was assessed by flow cytometry. Antigen-specific CD4+ T-cell responses to HPV16 E6 and E7 were assessed by OX40 assay.
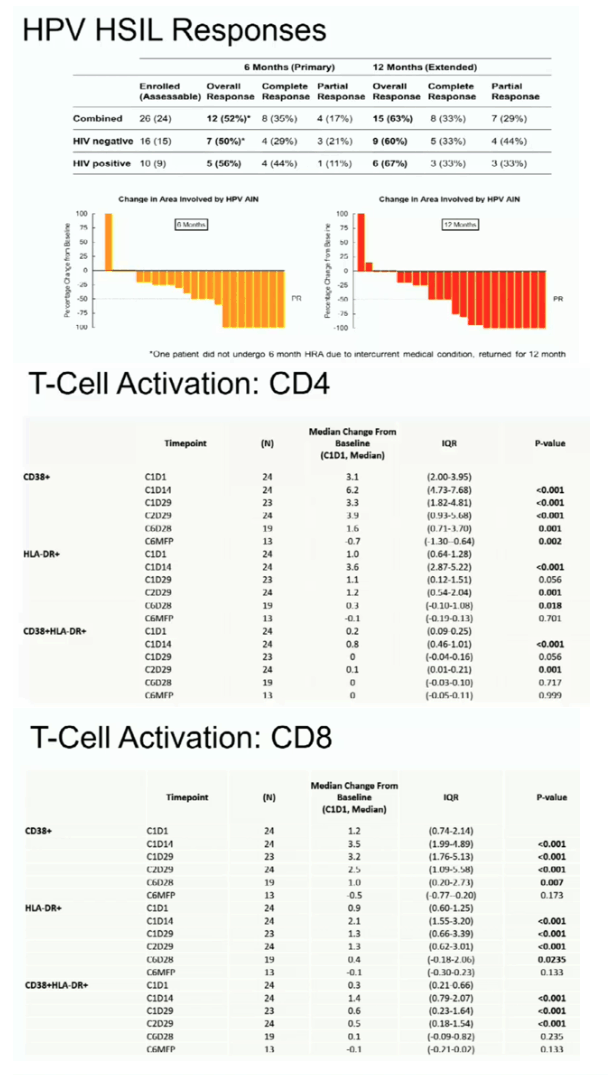
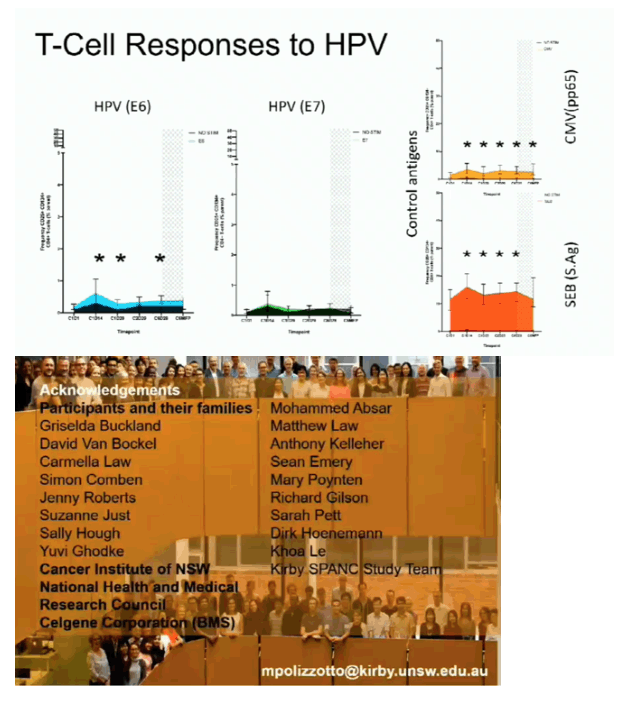
26 participants enrolled, 24 evaluable for response. All male; median age 54 (range 41-74). 10 (38%) PLWH: median CD4 700 cells/uL (320-1070), all HIV VL <20 copies/mL. All AIN3 HSIL, median duration HSIL 37 months (15-86), median octants 2 (0.5-5); HPV16 in 55%; multiple high risk HPV types in 50%. Overall response (CR+PR) was 52% (CI: 31-73) at end therapy, increasing to 63% (95% CI 40-81) after 6 months observation. Responses were comparable in PLWH. Adverse events (AEs) were mild and self-limited, including cytopenias, constipation, rash, with no idiosyncratic AEs in PLWH. HIV suppression was maintained. Over 137 cycles (c), attributable grade (g) 3/4 events were g3 neutropenia (4c) and g3 angina (1c). Systemic CD4+ T-cell responses to HPV E6 but not E7 increased during therapy, peaking day 14: baseline 0.06%, IQR 0.01 0.12%), median increase day 14 0.13% (IQR: 0.02 0.26%), p=0.001. CD4+ and CD8+ cell activation (CD38, HLA DR, CD38+HLA-DR) increased during therapy.
Low dose pomalidomide was well tolerated and induced durable continuing clearance of anal HSIL of multiple genotypes in even in chronic extensive disease irrespective of HIV status. Induction of HPV-specific CD4+ responses and immune activation support an immunological mechanism of action.
http://www.croiwebcasts.org/console/player/44673?mediaType=slideVideo&


|
| |
|
 |
 |
|
|