 |
 |
 |
| |
Post-Discharge Outcomes Following Acute Coronary Syndrome in HIV [ Disparities for PLWH ]
|
| |
| |
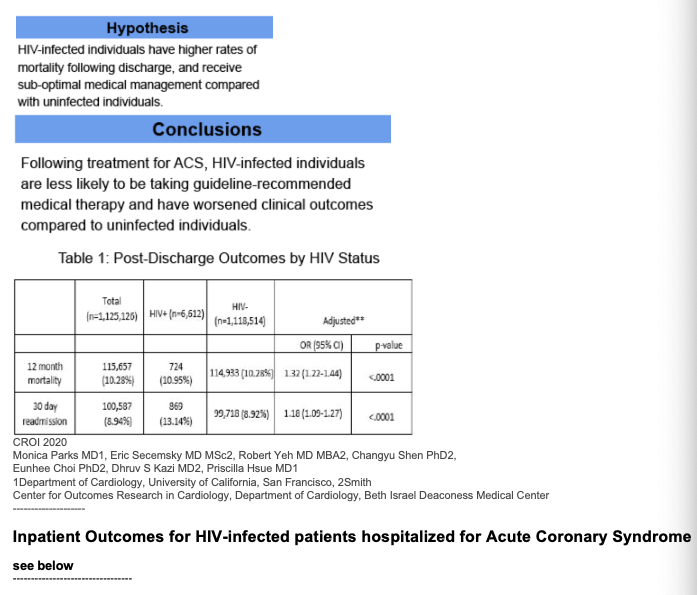
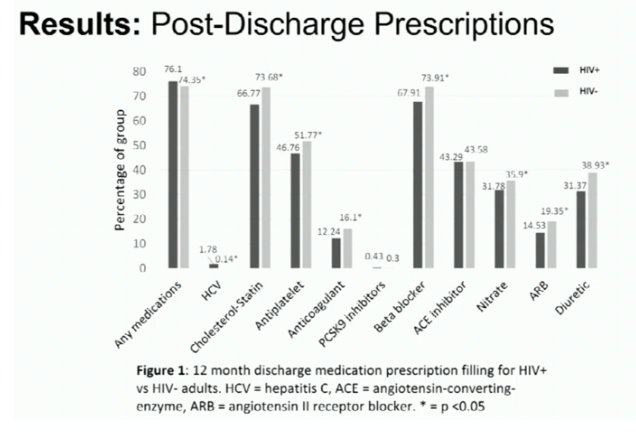
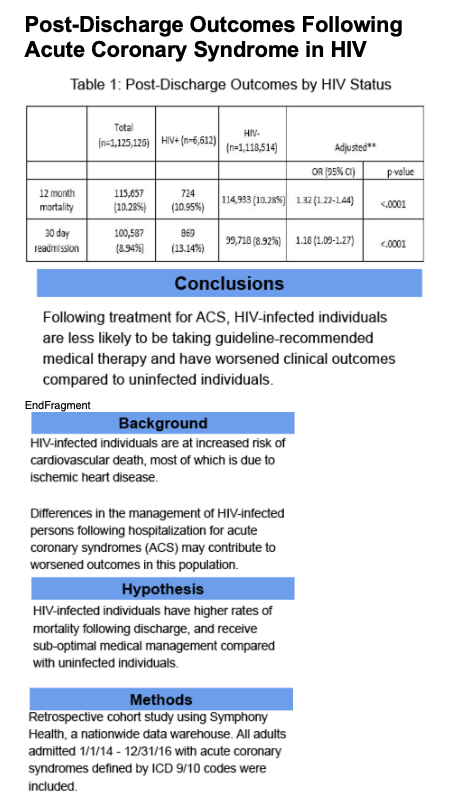
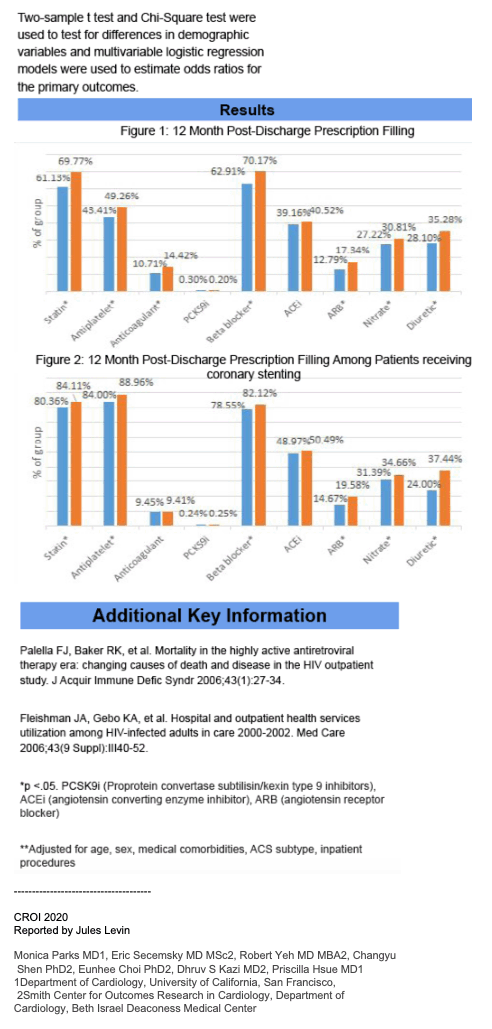
HIV+ have worse mortality, worse 30-day readmission, do not receive adequate & appropriate medications as much as HIV- including statins and others, see table below. Jules
CROI 2020
Monica Parks MD1, Eric Secemsky MD MSc2, Robert Yeh MD MBA2, Changyu Shen PhD2, Eunhee Choi PhD2, Dhruv S Kazi MD2, Priscilla Hsue MD1
1Department of Cardiology, University of California, San Francisco, 2Smith Center for Outcomes Research in Cardiology, Department of Cardiology, Beth Israel Deaconess Medical Center
METABOLIC COMPLICATIONS OF HIV AND ITS THERAPIES (03/17/20)
Themed Discussion:
http://www.croiwebcasts.org/console/player/44613?mediaType=slideVideo&
Abstract
HIV-infected adults have excess morbidity and mortality from cardiovascular disease. Differences in the presentation and management of acute coronary syndromes (ACS) in this population may drive these findings. We hypothesized that HIV-infected adults admitted with ACS are less likely to receive percutaneous coronary intervention and have greater adverse outcomes compared with uninfected patients.
This was a retrospective cohort study using inpatient claims data from Symphony Health, a nationwide data warehouse. All adults admitted between January 1st, 2014 and December 31st, 2016 with ACS were included. Patient characteristics and outcomes were defined by ICD-9 or ICD-10 billing codes. Logistic regression adjusted for clinical characteristics was used to evaluate outcomes.
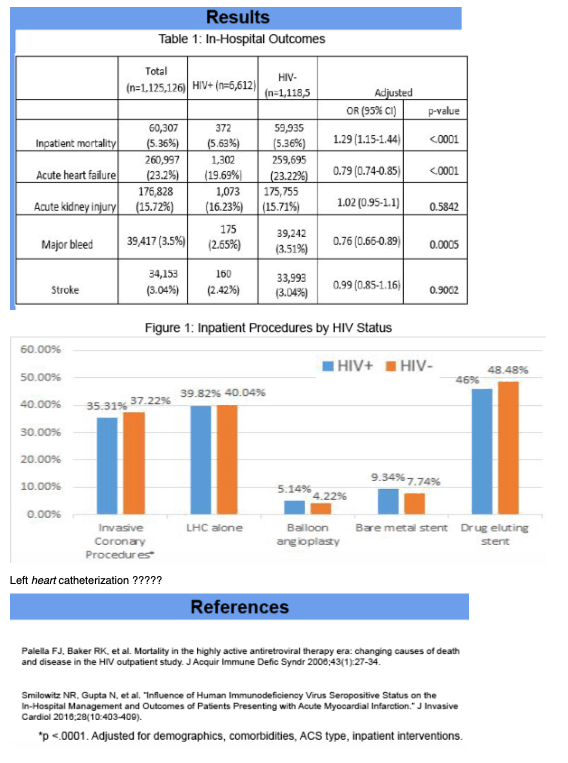
A total of 1,125,126 patients were included, of whom 6,612 (0.59%) had HIV. The HIV-infected group was younger (57 vs 67 years old, p<0.0001) and had a higher burden of medical comorbidities such as diabetes and substance abuse (p<0.0001). Rates of ST-elevation myocardial infarction were similar between groups. In adjusted analysis, HIV-infected individuals were less likely to receive coronary angiogram (31.6% vs 33.4%, OR 0.85, 95% CI 0.80-0.89, p <0.0001) or drug eluting stents (16.5% vs 18.2%, OR 0.88, 95% CI 0.82-0.94, p =0.0001). They also had significantly higher inpatient mortality (5.5% vs 5.3%, OR 1.28, 95% CI 1.15-1.43, p <0.0001) despite having fewer complications such as acute heart failure (19.9% s 23.2%, OR 0.82, 95% CI 0.76-0.88, p <0.0001) or major bleeding (2.8% vs 3.5%, OR 0.82, 95% CI 0.70-0.95, p =0.0074).
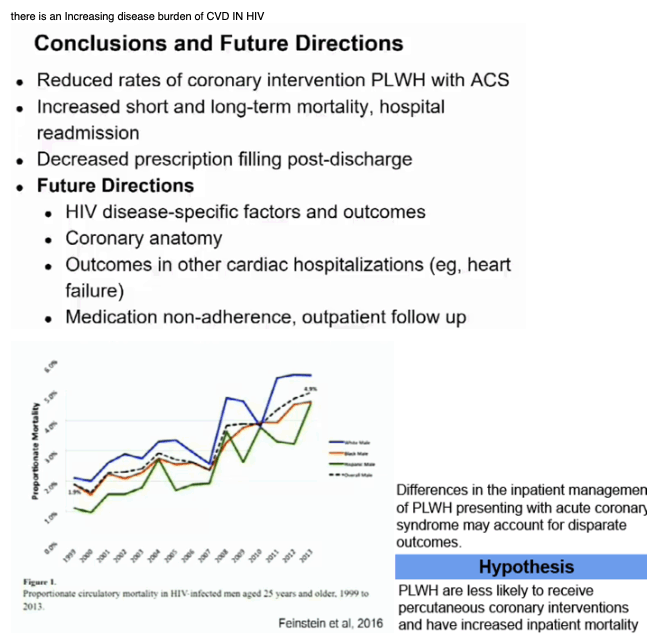
Among contemporary HIV-infected patients hospitalized with acute coronary syndrome, disparities in treatment persist, with less use of percutaneous coronary interventions. Further attention is needed in order to improve the use of guideline-based therapies with the goal of optimizing the care and outcomes among persons living with HIV.



|
| |
|
 |
 |
|
|