| |
Depressive Disorders in HIV/AIDS:....older PLWH, social isolation, stigma, survivor guilt, shame & guilt, existential issues
|
| |
| |
A Clinically Focused Narrative Review
Download the PDF here
April 3 2020 - Harvard Review of Psychiatry - Gustavo C. Medeiros, MD, Felicia A. Smith, MD, Madhukar H. Trivedi, MD, and Scott R. Beach, MD
From theDepartment of Psychiatry,University of Texas SouthwesternMedical Center, Dallas, TX (Drs. Medeiros and Trivedi); Harvard Medical School (Drs. Smith and Beach);Department of Psychiatry,Massachusetts GeneralHospital, Boston, MA (Drs. Smith and Beach).
In these times of COVID mental health for all but particularly for PLWH & more for oder & elderly HIV+. Jules
Depressive disorders in older seropositive individuals may also present unique treatment challenges. First, depressed older adults are more prone to have cognitive problems.125 Difficulties with executive functioning, memory, and attention may negatively affect compliance to medication and to treatment in general. Second, older patients tend to have more medical comorbidities and to be on polypharmacy. These factors, in combination with poorer drug metabolism, further increase the risk of side effects with neuropsychiatric medication.125
Third, grief and losses, such as the death of a loved one, are common and may be important contributing factors to the mood disturbance. Older individuals may also be more likely to manifest survivor's guilt as a result of having lived through the early days of the epidemic.
Text Box 2 presents some "clinical pearls" for managing
depressive disorders in HIV/AIDS. see below
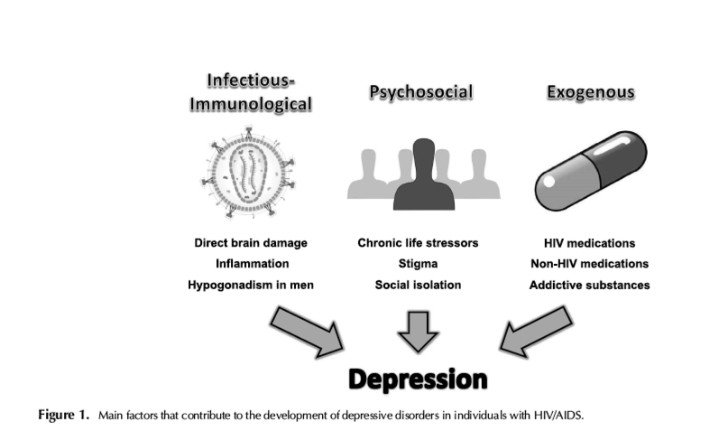
HIV/AIDS is associated with infectious-immunological changes that predispose seropositive individuals to depressive disorders. The infectious-immunological changes include direct brain damage by the virus as well as an abnormally prolonged immunological response to the virus. The virus has a strong tropism for the CNS and reaches it early in the disease course.81 The viral proteins gp120 and Tat have neurotoxic properties, especially toward CNS dopaminergic pathways
The intensity of inflammatory responses over the course of HIV/AIDS fluctuates, varying from intense activation in the infection's early phases to immune deficiency in later phases.
Psychosocial factors contributing to the development of depressive disorders in HIV/AIDS include chronic life stressors, stigma, and social isolation.
Stigma is a significant psychosocial factor that is associated with depressive disorders inHIV/AIDS.93 Approximately 80% of HIV+ individuals report experiencing some type of stigma related to HIV/AIDS status.94 Stigma may be experienced in three different ways: (1) enacted stigma, where seropositive persons experience overt stigmatizing behavior, (2) anticipated stigma, where these individuals are concerned about being victim of stigma in the future, and (3) internalized stigma, where these individuals have negative beliefs and self-image because of their HIV/AIDS status.67 All three types of stigma seem to be distressing. Data obtained from seropositive MSM, however, suggest that anticipated stigma seems to be the most significant stigma-related risk factor for MDD68 and possibly also for other depressive disorders.
Shame and guilt are commonly seen as two subconstructs of internalized stigma that may have an important impact on health outcomes in persons living with HIV/AIDS. Shame is a distressing, self-conscious emotion wherein the individual sees himself as defective and a failure;79 by contrast, guilt is a feeling of deserving blame for past actions or behaviors
Social isolation is another common psychological concern in individuals with HIV/AIDS.93 A multinational survey of
2035 individuals with HIV found that 37% of participants reported loneliness and social isolation resulting from their HIVstatus.94 Social isolation is even more pronounced in older adults with HIV/AIDS (45% of patients in the United States with HIV are over 50 years old),66,93 and it represents a risk factor for mood disturbances in all seropositive persons. Social support may act as a protective factor against depressive disorders in HIV/AIDS by buffering chronic and multiple life stressors.69,93,94 There is also a negative correlation between social support and perceived stigma, where seropositive persons with increased concern about discrimination may avoid socialization because of their fear of rejection.
Patients with HIV/AIDS also struggle with existential issues that may affect their mood. Seropositive patients often feel that they do not have control over their own lives and that they failed to make meaningful contributions during their lives, and they may have a heightened perception of their mortality. 70 Survivor's guilt is also common, particularly among individuals who acquired the illness in the beginning of the epidemic, many of whom witnessed the deaths of friends and loved ones.95 All of these existential concerns have been shown to be correlated with increased rates of depression.
Exogenous factors that may potentially contribute to the development or worsening of depressive disorders include anti-retroviral therapy, other medications, and addictive substances.
Depressive disorders are not only underrecognized in HIV/AIDS but, when diagnosed, are often not treated or properly
managed.22,33 For example, only 18% of seropositive individuals with MDD receive treatment, and just 7% have access to adequate therapeutic interventions.
Management of Contributing Factors
One of the most important interventions in addressing depression in seropositive patients is to ensure proper care of
HIV/AIDS. Poor infectious-immunological status predisposes individuals to HIV-associated fatigue, neurological damage, opportunistic infections, hypogonadism, and other factors that may worsen depressive symptoms. In depressive disorders secondary to other causes such as substance/medications or medical conditions, co-treatment of the underlying cause of mood changes is the most important intervention. Psychoeducation
is another low-cost intervention that may reduce stigma and improve adherence to treatment. Psychoeducational interventions may be delivered in group settings, by lay health workers, or online.
Reduced functionality due to HIV/AIDS, multiple contacts with health services, substance use, living single, and low
socioeconomic status have also been described as risk factors for suicidality. Suicidal ideation should be regularly assessed in seropositive persons.

Abstract
Depressive disorders and human immunodeficiency virus/acquired immunodeficiency syndrome (HIV/AIDS) are associated with major socioeconomic burdens.
The negative impact of depressive disorders on HIV/AIDS is well known, including on treatment outcomes.
Unfortunately, depressive disorders are underdiagnosed and undertreated in seropositive persons.
This review summarizes clinically useful information on depressive disorders in HIV/AIDS.
More specifically, we address assessment, differential diagnosis, contributing factors, management, and common challenges in the treatment of depressive disorders in seropositive individuals.
Assessment and diagnosis of depression may be challenging in seropositive persons because of several biopsychosocial particularities associated with HIV/AIDS.
One of the difficulties is the overlap between depression and HIV/AIDS symptoms, particularly in individuals with advanced AIDS, requiring consideration of a broad differential diagnosis.
Several factors related to HIV/AIDS status contribute to the higher rates of depressive disorders, including infectious-immunological, psychosocial, and exogenous factors. The treatment of depressive disorders in HIV/AIDS involves three groups of interventions: (1) pharmacological interventions, (2) psychotherapeutic interventions, and (3) management of other contributing factors.
Challenges in management include poor adherence to treatment and the risk of suicide. We provide evidence-based recommendations to improve assessment and management of depressive disorders in seropositive persons.
Depressive disorders and human immunodeficiency virus/acquired immunodeficiency syndrome (HIV/AIDS) are associated with major socioeconomic burden.
Globally, depressive disorders are a leading cause of disability, 1(p 1817, Table 1) while HIV/AIDS ranks eleventh.2
Depressive disorders are a group of disorders characterized by the presence of sad, empty, or irritable mood, accompanied by somatic and cognitive changes that significantly affect the individual's capacity to function.
Included in this context are conditions such as major depressive disorder (MDD), substance/medication induced depressive disorder, and depressive disorder due to another medical condition.3 The main depressive disorder in
terms of prevalence and burden is MDD, with approximately 300 million individuals affected worldwide.4
Previous evidence suggests that persons with HIV/AIDS have a significantly greater risk of developing depressive disorders than the general population, including a two- to four-fold higher risk of developing MDD.5-9
MDD is also the most common psychiatric condition in individuals with HIV/AIDS,10 with an estimated prevalence ranging from 20 to 42%.5,8,11-13
The negative impact of depressive disorders on HIV/AIDS is well known. For example, MDD is associated with poorer
compliance to anti-retroviral therapy (ART),14,15 higher rates of detectable viral load,16 lower CD4 counts,17 poorer functionality, and lower quality of life.16,18,19
Depressive disorders have also been associated with greater mortality.20,21 For example, Sudfeld and colleagues20 found that 36% of the deaths in Tanzanian women with HIV over the course of two years were attributable to depression.
Depressive disorders are underdiagnosed and undertreated in individuals with HIV/AIDS.22 Proper detection and management of depressive disorders improves HIV/AIDS outcomes, leading to better compliance to ART, higher CD4 counts, and increased rates of undetectable viral load.14,23-27 Therefore, a practical review addressing clinically relevant aspects of depressive disorders in HIV/AIDS is timely.
Despite vast and good-quality research on depression in HIV/AIDS, clinician-friendly, updated reviews of the scientific
literature are much needed. In spite of their strengths, the majority of literature reviews on this subject tend to focus on particular aspects of depression in HIV/AIDS such as adherence to ART 25,28,29 or HIV/AIDS progression,17,30 or on specific types of treatment for depression.7,31,32
The objective of this literature review is to provide an updated, practical, and global overview of depressive disorders in HIV/AIDS.
More specifically, we will address the following questions:
(1) How should clinicians assess and diagnose depressive disorders in HIV/AIDS?
(2)What are the factors contributing to the development of depressive disorders in HIV/AIDS?
(3) How should clinicians manage depressive disorders in HIV/AIDS?
(4) What are common challenges in the treatment of depressive disorders in HIV/AIDS, and how should clinicians
approach these?
excerpts





|
|
| |
| |
|
|
|