 |
 |
 |
| |
Diabetes & Lipids Associated with Liver Disease
|
| |
| |
Reported by Jules Levin
These studies were reported at the 40th annual EASL liver meeting in Paris (April 2005). The studies support numerous previous studies that insulin resistance and diabetes can contribute to advancing liver disease, particularly in people with viral hepatitis C or B. As well, elevated lipids may contribute.
Impact of Overweight & Diabetes on Liver-Related Death in Patients with Alcoholic & Viral Hepatitis C Cirrhosis
G. N'Kontchou1, M. Tin Tin Htar1, J. Paries2, F. Kazemi1, V. Bourcier1, N. Ganne-Carrie1, P. Nahon1, V. Grando-Lemaire1, J.C. Trinchet1, M. Beaugrand1
1 Liver Unit, Jean Verdier Hospital, Bondy, France
2 Public Health Unit, Jean Verdier Hospital, Bondy, France
Obesity and diabetes have been suggested to be risk factors of liver-related death in recent population-based cohort studies. This study was aimed to assess prospectively the impact of these factors on liver-related death (including liver transplantation).
Overweight & diabetes type II are risk factors of cirrhosis in patients with alcoholic & viral HCV. They are also risk factors for liver cancer (hepatocellular carcinoma). Their influence on liver-related death in patients has not yet been evaluated.
A large cohoht of 963 patients with compensated cirrhosis regularly followed for a screening program for HCC were included. All clinical and biological variables were collected at inclusion. Ultrasonography & alfa-feto protein were used for follow-up evaluation. Outcomes evaluated were: liver-related death, liver-related death including liver transplantation (HCC, liver failure, portal hypertension), & occurrence of HCC was also recorded.
Predictive factors for overall and liver-related death were determined by log-rank test and Cox proportional hazards model. Survival to events was estimated by Kaplan-Meier method.
BASELINE CHARACTERISTICS n=963:
Age: 57
63% male
Etiologies: (alcohol/HCV/mixed): 484/322/157
Diabetes: 298 (31%)
BMI (kg/m2): 25/6 +/-4.7
Prothrombine time: 72+/-17
Platelet counts: 137 +/-64
Bilirubin: 28 mmol/l
Albumin (g/l): 39+/-6
AST (N): 2
ALT (N): 2
AP (N): 1.4
y-GT (N): 3.9
Results
-There were 484 alcoholic cirrhosis, 322 HCV, 157 HCV+alcohol.
-Mean age was 57.2±11 yr and mean BMI was 25.6 kg/m2.
-607 were male patients.
-298 patients were diabetic.
-After a mean follow-up of 66.7±45.2 months, 384 patients died, of which 279 were liver-related deaths (liver failure: 142; hepatocellular carcinoma: 117; portal hypertension: 20).
In univariate analysis, factors associated with liver-related death were:
--BMI ³27.5 [OR 1.9; 1.5-2.4; p < 0.0001]
--age >57 yr [OR 1.6; 1.3-2.0; p < 0.0001]
--male sex [1.7; 1.3-2.1; p < 0.0001]
--platelet count <140,000/mm3 [OR 1.9; 1.5-2.5; <0.0001]
--serum albumin <42 g/l [2.8; 2.0-3.9; p < 0.0001]
--prothrombin activity <82% [2.3; 1.7-3.1; p < 0.0001]
--alkaline phosphatase >1.4 ULN [OR 1.9; 1.5-2.4; p < 0.0001]
--total bilirubin >17 mm/ml [OR 1.9; 1.5-2.4, p < 0.0001].
Diabetes was not significantly related.
In multivariate analysis, independent risk factors for liver-related death were:
--serum albumin <42 g/l [OR 2.00; 1.4-2.9; p = 0.0004]
--BMI ³27.5: [OR 1.8; 1.4-2.4; p < 0.0001]
--age >57 yr [OR 1.7; 1.3-2.3; p = 0.0002]
--male sex [OR 1.5; 1.1-2.1; p = 0.01]
--prothrombin activity <82% [OR 1.6; 1.1-2.2 p = 0.02]
--alkaline phosphatase >1.4 ULN [OR 1.4; 1.0-1.9; p = 0.03].
These results were confirmed in different etiological subgroups.
Conclusion: Overweight was an independent and important predictive factor of liver-related death in patients with compensated HCV and alcohol cirrhosis.
Diabetes is Strongly Associated with Advanced Fibrosis;
Elevated Lipids May Be Associated with Fibrosis
--Patient Populations with High prevalence of Diabetes, like Hispanics, May Be Particularly At Risk for Advancing Liver Disease
"ASSOCIATION BETWEEN DIABETES, OVERWEIGHT, OBESITY AND DYSLIPIDEMIA WITH FIBROSIS PROGRESSION IN CHRONIC HEPATITIS C PATIENTS"
A. Loaeza-del Castillo, F. Vargas-Vorackova
1 Department of Gastroenterology, Instituto Nacional de Ciencias Mdicas y Nutricin, Mexico
2 Department of Gastroenterology, Instituto Nacional de Ciencias Mdicas y Nutricin, Mexico
Fibrosis progression in chronic hepatitis C (CHC) patients is variable, factors associated with an accelerated progression have been identified, but they do not account for the heterogeneity seen between individuals.
Aim: To determine the prevalence of diabetes, overweight, obesity and dyslipidemia in CHC patients and the association of these metabolic factors with liver fibrosis progression.
Method: Patients with CHC seen in our institution between 1993 and 2003 were retrospectively studied (n = 1618). Patients with a known duration of infection acquired by transfusion with a liver biopsy performed before any antiviral treatment were included. Patients with overt hepatic insufficiency were excluded. The diagnoses of diabetes, overweight, obesity and dyslipidemia were investigated and liver fibrosis stage (METAVIR). Variables were tested for their association with significant fibrosis (F2, F3, F4).
RESULTS
--108 patients were included, 71 (66%) female and 37 (34%) male,
--mean age was 48.7+12.2 years.
--Age at infection was 24.7±13 years, acquired between 1944-2000.
--78% were HCV-genotype 1.
--Fibrosis stage was: F0 = 15 (14%), F1 = 38 (35%), F2 = 9 (8%), F3 = 8 (8%) and F4 = 38 (35%).
--Mean fibrosis progression rate was 0.106±0.101 (0-0.44).
--26 patients (24%) had diabetes, 10 (9%) glucose intolerance, 24 (22%) obesity [body mass index (BMI) ³30 kg/m2] and 49 (45%) overweight (25 £ BMI < 30 kg/m2).
--Dyslipidemia was investigated in 75 patients and confirmed in 25 (33.3%). Association between these variables and fibrosis is depicted in the table.
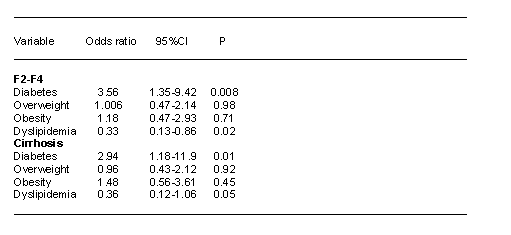
Conclusions: Diabetes is a factor strongly associated with advanced fibrosis and cirrhosis. In populations with a high prevalence of diabetes, such as Hispanics, this association must be taken into account. Lipid metabolism has a specific role in the pathogenesis of CHC and the possible protector role of dyslipidemia for significant liver fibrosis should be investigated in further studies.
"INSULIN RESISTANCE PROMOTES FIBROSIS PROGRESSION AND PREDICTS NECRO-INFLAMMATORY ACTIVITY IN PATIENTS WITH NON-ALCOHOLIC FATTY LIVER DISEASE"
D. Sanchez-Munoz1, E. Suarez1, M.V. Galan1, L. Grande1, G. Munoz2, M. Romero-Gmez1
1 Hepatology Unit, Hospital Universitario de Valme, Sevilla, Spain
2 Pathology Unit, Hospital Universitario de Valme, Sevilla, Spain
Aims: To assess the presence of metabolic syndrome X (MSx) and insulin resistance (IR), and its relationship with histologic damage, in patients with non-alcoholic fatty liver disease (NAFLD).
Patients and Methods: Thirty-five patients, 25 male and 10 female, with an average age of 45.7±12.7 [24-76] years, diagnosed by NAFLD, were included. Liver biopsy was carried out after persistence for, at least, six months of altered liver enzymes with appropriate diet and physical activity therapies. Histological damage was assessed according to Brunt criteria (Semin Liver Dis 2001; 21: 3-16). Body mass index (BMI) was calculated. MSx was diagnosed according to ATP III criteria. IR was calculated using the HOMA-IR index = [Glucose(mmol/l) _ Insulin(UI/ml)]/22.5.
RESULTS
Only one patient (2.5%) showed normal weight; 17/35 (48.6%) patients showed overweight and 17/35 (48.6%) patients were obese.
--MSx was present in 14/35 (42.5%) patients;
--central obesity in 65.7%,
--high triglyceride levels in 62.9%,
--altered glucose metabolism in 28.6%,
--hypertension in 31.4% and
--low HDL-colesterol levels in 24%.
--IR was present (HOMA-IR >2) in 23/33 (74.3%) patients.
--The histologic diagnosis was simple hepatocyte steatosis (HS) in 8/35 (22.9%) patients and steatohepatitis (NASH) in 27/35 (77.1%) patients: Fibrosis degree was: absent in 13 patients, mild fibrosis (F1-F2) in 6 patients, bridging fibrosis (F3) in 7 patients and cirrhosis (F4) in 1 patient.
Patients with HS showed lower triglyceride levels (99±43 vs 169±85 mg/dl; p = 0.034) and HOMA-IR (2.54±0.9 vs 4.5±2.5; p = 0.002) than patients with NASH.
Triglycerides >180 mg/dl or HOMA IR >4.5 was associated with NASH (Specificity: 100% and Sensitivity: 54.3%.
Fibrosis correlated with age (r = 0.37; p = 0.027), AST (r = 0.5; p = 0.002), and HOMA-IR (r = 0.45; p = 0.007).
In multiple lineal regression, the only factor associated with fibrosis was the HOMA-IR (R = 0.60; p = 0.0001). All of the patients with advanced fibrosis (F3-F4) showed a HOMA-IR index >4.5, but only 8/26 (30%) patients with F0-F2; p < 0.001.
Conclusions: Insulin resistance is present in the majority of the patients with non-alcoholic fatty liver disease. HOMA-IR index >4.5 or triglyceride levels >180 mg/dl are predictors of the presence of NASH. Insulin resistance may play a role in the pathogenesis of fibrosis progression in patients with NAFLD. Drugs able to decrease insulin resistance could be useful in the therapy of this disease.
Total Calories May Contribute to Development of Fatty Liver
"LIVER STEATOSIS (Fatty Liver) IN OPEN POPULATION: PREVALENCE AND RELATIONSHIP TO THE DIET. PRELIMINARY RESULTS OF THE "ARSITA-ONE" PROJECT"
I. Petridis1, E. Lattanzi1, B. Marraccini1, I. Carderi1, E. Claar1, C. Liani1, S. Lobello1, O. Di Andrea2, M. Chiaramonte1
1 Hepato-Gastroenterology and Nutrition Unit - Dept. of Internal Medicine and Public Health - L'Aquila University, L'Aquila, Italy
2 Arsita Family Doctor, Italy
Background and Aim: This study, part of a larger epidemiological study for liver and metabolic diseases carried out on Arsita (Abruzzo) (805 adult registered inhabitants), was designed: 1) to assess the prevalence of liver steatosis; 2) to evaluate the relationship with the diet.
Materials and Methods: All subjects aged over 18 yr were invited to have liver ultrasound (US) and an alimentary questionnaire computer analyzed (Winfood 1.5). Liver steatosis was classified as none, mild, moderate and severe. Diet was classified as: diet 1, a traditional local diet, hypercaloric (3500-4500 kcal), hyperlipidic (55% of calories); diet 2, similar but with less calories (2500-3500 kcal); diet 3, classic Mediterranean (2000-2500 kcal).
RESULTS
--541 subjects (253 M and 288 F), completed the US and diet study.
--Moderate/severe steatosis was found in 89/253 (35%) males and 75/288 (26%) females; in 41/164 (25%) subjects under 40 yr, in 63/119 (33%) subjects aged 40-59 yrs and in 92/196 (47%) subjects over 60 yr.
--143/253 males (57.5%) and 86/288 females (30%) followed diet 1, which was related to obesity (BMI > 30) in 61% of males and 69% of females, while 14% of subjects having diet 2 were obese.
--All subjects with mediterranean diet had normal BMI.
--In diet 1 group, 71.5% of males and 64.5% of females had steatosis, while in diet 2 this was respectively 25.1% and 31.3%.
--In subjects with steatosis, alcohol consumption was present in 82% of males and in 48% of females, while BMI > 30 was present in 61% of males and 78% of females.
--Out of 164 subjects with steatosis 22 (13%) had altered AST and/or ALT (13 anti-HCV+).
Conclusions: Prevalence of steatosis is increasing with age and is more frequent in males. In females severe steatosis is mainly correlated with overweight and in males with alcohol abuse. The amount of total calories instead of the proportion of fat seems to be related to liver steatosis. Elderly people had moderate/severe in 47%, however in most cases steatosis is indolent. Hepato cytolisis, without virus, seems to be very rare. Liver steatosis without "a second hit" seems to be a benign condition.
|
|
| |
| |
| |
|
 |
 |
|
|