 |
 |
 |
| |
"Viral Load is a Strong Predictor of Hepatocellular Carcinoma (HCC) Risk in People Chronically Infected With Hepatitis B Virus (HBV) Independent of Serum Alanine Aminotransaminase Level (ALT)"
|
| |
| |
The Risk Evaluation of Viral load Elevation and Associated Liver Disease/Cancer Study (The R.E.V.E.A.L.-HBV Study)
Authors; Uchenna H Iloeje1, Hwai-I Yang2, Jun Su1, Chin-Lan Jen2, Edward Kuo3, San-Lin You2, Chien-Jen Chen2
1Pharmaceutical Research Institute Bristol-Myers Squibb, Wallingford, USA; 2National Taiwan University, Taipei, Taiwan; 3Bristol-Myers Squibb, Taipei, Taiwan
Reported by Jules Levin
Yesterday I reported the study from these same authors on association between HBV DNA & the risk for developing cirrhosis. This study examines association between HBV DNA & risk for developing hepatocellular carcinoma (liver cancer). This study found that the higher HBV DNA levels were (HBV viral load) the greater the risk for liver cancer to develop; that, elevated HBV DNA is a strong predictor for liver cancer, regardless of ALT. Here is the information & data presented in this poster at DDW May 2005. As you can see from Table 6 just below, using <1,000 copies/ml HBV DNA as a reference with a 1.0 relative risk for liver cancer, HBV DNA of 10,000 increased risk by 2.2 (1.2-3.9), and HBV DNA of 100,000 copies/ml or more increased risk by 6.6 (4.1-10.7) for liver cancer.
INTRODUCTION:
Ongoing viral replication is a risk for the development of HCC either through the development of liver inflammation, with subsequent fibrosis and cirrhosis (a risk factor for HCC) or by other mechanisms including the incorporation of viral proteins into the host genome.
Treatment of people chronically infected with HBV is aimed at suppressing viral
replication and preventing or slowing disease progression to liver complications.
Serum ALT level is an important factor in deciding who gets treated by current treatment guidelines.1,2 However, serum ALT levels are known to fluctuate, and as a result, physicians may miss periods of ALT elevation unless patients are monitored very frequently with blood tests.
1. Lok A, Heathcote E, Hoofnagle J. Gastroenterology. 2001;120:1828-5183.
2. Lok A, McMahon B. Hepatology. 2004;39(3):857-861.
In this analysis we evaluated the risk associated with HBV DNA levels in subjects who had normal serum ALT levels at enrollment and would not therefore qualify for therapy.

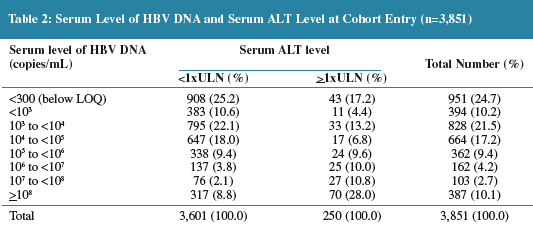
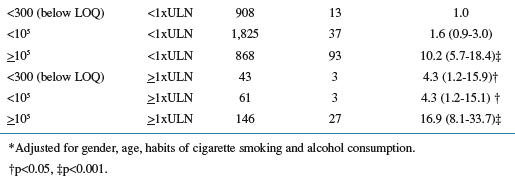
In Table 4 below viral load from 300 to 1,000 slightly increases risk by 10% compared to <300 as a reference with no risk; 1,000 to 10,000 is associated with 2.4 times greater risk than if viral load is <300; viral load of 10,000 to 100,000 is associated with 8 times greater risk than if viral load is <300; and, viral load of >1 million is associated with 12.3 times greater risk than if viral load is <300.
AUTHOR CONCLUSION:
--Population-based prospective cohort study with a mean follow-up of 11 years
--In this cohort of untreated chronic HBV-infected subjects, in participants with normal serum ALT, cohort entry HBV DNA level was a strong predictor of HCC risk.
--There was a dose-dependent relationship between increasing HBV DNA levels and HCC incidence
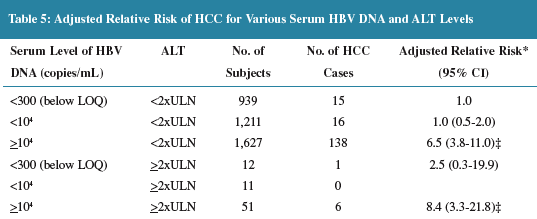
--The majority of HCC cases 114/143 (80%) were seen in people with HBV DNA≥104 copies/mL (10,000 copies/ml).
--The absolute risk over the study period in this group was 7.5% (114/1515)
--In subjects with HBV DNA ≥105 copies/mL (100,000 copies/ml), 93/868 (10.7%) developed HCC, and for subjects with HBV DNA ≥106 copies/mL (1 million copies/ml), 60/530 (11.3%) developed HCC
--The relative risk of HCC increased across a biological gradient of HBV DNA level when compared to the group with undetectable HBV DNA
--The risk gradient remained regardless of how HBV DNA level and normal serum ALT were defined.
ABSTRACT
Introduction: Treatment guidelines exclude chronic hepatitis B patients with normal serum ALT from therapy. This study was carried out to examine the risk of HCC in this population of patients with emphasis on the role of serum HBV DNA level.
Methods: A cohort of 3,851 participants with chronic HBV infection was recruited from seven townships in Taiwan between 1991 and 1992. Cohort entry serum samples were tested for HBsAg, HBeAg, HBV DNA by PCR, and serum ALT. The diagnosis of HCC was ascertained through data linkage with computerized profiles of the National Cancer Registry and Death Certification System in Taiwan. Multivariable adjusted relative risks (RRadj) were derived using Cox proportional hazard models.
Results: Overall, during 43,993 person-years of follow-up, 176 patients were newly diagnosed with HCC among the 3,851 participants. Of the 3,851 participants, 3,270 (85%) were seronegative for HBeAg, of which 1,121 (34%) had serum HBV DNA level >104 copies/mL (10,000 copies/ml) and 1,052 (94%) of them had a normal serum ALT level. 581 participants (15%) were HBeAg positive of which 557 (96%) had serum HBV DNA >104 copies/mL at cohort entry and 463 (83%) of them had normal serum ALT levels. There was a dose-dependent relationship between HBV DNA and HCC risk in people
with normal serum ALT variably defined as either <1 x ULN or <2 x ULN.
Conclusion: Elevated serum HBV DNA is a strong predictor of HCC in patients
regardless of serum ALT.



STUDY DESIGN
--All 89,293 adult residents of 7 townships in Taiwan between the ages of 30 and 65 were invited to participate in a prospective cohort study
--23,820 (27%) subjects gave informed consent and were enrolled in the cohort
At entry, subjects:
--Provided informed consent
--Provided a serum sample which was separated on the day of collection and frozen at -70°C
--Underwent a structured interview by a trained public health nurse
--Had an ultrasound examination
--All samples were tested for HBsAg, HBeAg, and serum ALT
ANALYSES:
- HBV DNA of cohort entry serum samples by PCR (COBAS Amplicor, Roche
Diagnostics Co., Indianapolis, IN) (LOQ=300 copies/mL)
- HBsAg and HBeAg by radioimmunoassay (Abbott Laboratories, North Chicago, IL)
- Anti-HCV antibody by 2nd generation ELISA kits (Abbott Laboratories, North Chicago, IL)
- ALT by serum chemistry autoanalyzer (Model 736, Hitachi Co., Tokyo, Japan) using commercial reagents (bioMérieux, Mercy-l’Etoile, France)
STUDY POPULATION/METHODS:
Of the 23,820 cohort members:
- 4,155 tested HBsAg-positive
- 3,851 of 4,155 (93%) had entry serum tested for HBV DNA
- Data cut off for these analyses was June 30, 2004
Demographics of Study Cohort:
N=3,851
61% male
median age: 45
HBeAg-positive: 15%
Median HBV DNA HBeAg-positive subjects: >10 8 (>100 million copies/ml)
Median HBV DNA HBeAg-negative subjects: >103 (>1,000 copies/ml)
All HBsAg-positive individuals had regular ultrasounds (a minimum of once a year) and health examinations.
--The person-years of follow-up for each participant was calculated from the date of enrollment to the date of the diagnosis of HCC, the date of death or the last date of linked data available from National Health Insurance profiles (June 30, 2004), whichever came first.
--Cases of HCC were detected by follow-up abdominal ultrasonography and serum
_-fetoprotein level or ascertained by computerized data linkage with the profiles of National Cancer Registry in Taiwan from January 1, 1991 through June 30, 2004. To ensure complete ascertainment, data linkage with the National Death Certification and National Health Insurance profiles was also carried out
All HCC cases were confirmed based on either:
- Cytopathology
- Two positive coincident imaging techniques
- One positive imaging technique with an elevated serum alpha-fetoprotein level >400 ng/mL
Cox proportional hazards modelling was used to derive the adjusted relative risk of HCC by HBV DNA level after adjusting for several variables including age, gender, smoking, alcohol consumption, serum HBeAg status, and anti-HCV antibody status.
--The statistical software Stata (StataCorp LP, College Station, TX) was used to obtain the corresponding estimates and figures.
RESULTS
--89,293 adults invited to participate in 1991-1992 (47,079 males & 42, 214 females).
--23,820 enrolled in study (11,973 males & 11,827 females):
4,155 HBsAg-positive (2,455 males & 1,710 females: 3,851 with HBV DNA test of enrollment serum sample (2,367 males & 1,484 females): 176 HCC cases
--19,665 HBsAg-negative (9,528 males & 10,137 females)
|
|
| |
| |
|
 |
 |
|
|