 |
 |
 |
| |
HBV Viral Load Predicts Cirrhosis Risk
|
| |
| |
"Viral Load is a Strong Predictor of Liver Cirrhosis Risk in People Chronically Infected with HBV Regardless of HBeAg Status: the R.E.V.E.A.L.-HBV Study"
Authors: CJ Chen1, Hi Yang1, J Su2, CLJen1, E Kuo3, SL You1, UH Iloeje2
1National Taiwan University of Taiwan, Taiwan;
2Bristol Myers Squibb Co, Wallingford, CT; 3Private Medical Practice, previously Bristol Myers Squibb, Taipei, Taiwan
Reported by Jules Levin
Ongoing viral replication of HCV or HBV is associated with inflammation of the liver, which over the course of years may increase risk for fibrosis & subsequent cirrhosis & liver cancer. Several studies recently presented at EASL & DDW have found that ongoing detectable levels of HBV DNA, viral load, can increase risk for cirrhosis & liver cancer. This study examines the association between increasing HBV DNA levels & the risk for developing cirrhosis.
AUTHOR CONCLUSIONS:
In this patient cohort of untreated HBV-infected subjects, entry HBV DNA level was a strong predictor of cirrhosis risk.
The effect of increasing HBV DNA on patients risk of cirrhosis was independent of HCV status.
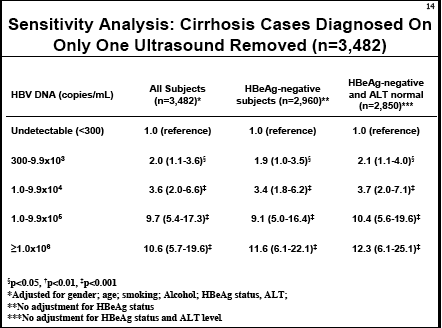
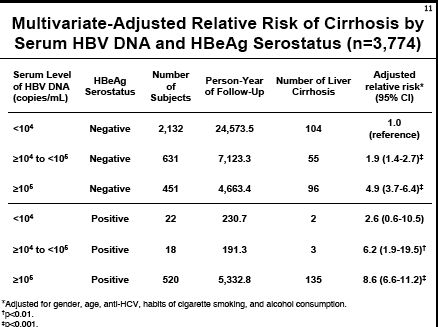
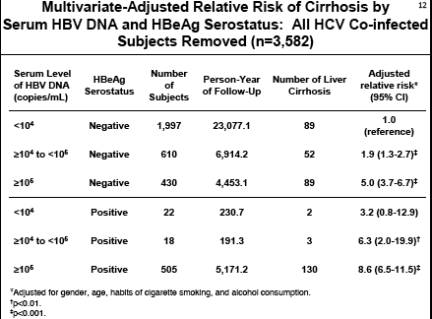
As you can see, as HBV DNA (viral load) increases this study finds the risk for developing cirrhosis increases. In multivariate models, removing HCV coinfected subjects, risk of cirrhosis started increasing at HBV DNA level >=300 copies/ml: for both HBeAg negative & HBeAg positive subjects(see table in report below) risks rates are similar:
--undetectable (<300) reference, risk 1.0;
--300 to 1,000: 1.4 Relative Risk;
--1,000 to 10,000: 2.4 RR;
--10,000 to 100,000: RR 5.4;
-- >1 million: RR 6.7
It is therefore expected that reducing HBV DNA should decrease cirrhosis risk for patients. This is unlike in HCV where HCV viral load does not appear to be associated with increased risk for disease progression, you could have a low HCV viral load & have cirrhosis.
THE STUDY
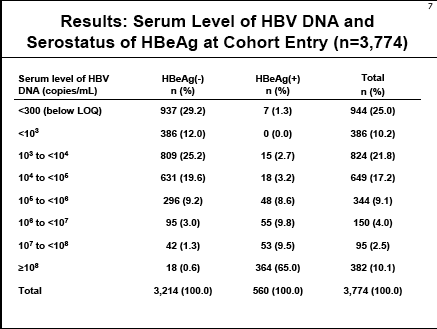
All study subjects provided a serum sample, underwent a structured interview, han an ultrasound exam, were free of liver cancer. All samples were tested for HBsAg, ALT, HBeAg status, & anti-HCV antibody status.
All HBV DNA analysis done using COBAS Amplicor Roche Diagnostics; LOQ 300 copies/ml.
The protocol called for HBsAg+ subjects to have an ultrasound every 6-12 months: cirrhosis patients every 3-6 months. During follow-up, 63% had between 1-5; 28% 6-10; 9% >10 ultrasonograms.
This is a population based cohort study with a mean follow-up of 11 years. All adult residents of 7 townships in Taiwan aged 30-65 were invited to participate (89,293) in 1991-1992 (47,079 males & 42,214 females). 23,000 enrolled in the study (11,973 males & 11,847 females):
--4,155 HBsAg positive (2,455 males & 1,710 females); 3,851 with HBV DNA test of enrollment serum sample (2,367 males & 1,484 females)---3,774 included in
analysis: 395 with cirrhosis
--19,665 HBsAg negative: 9,528 males& 10,137 females
STUDY METHODS
Person-years of follow-up for each participant was calculated from the date of enrollment to date one of the following, whichever came first:
--diagnosis of cirrhosis
--date of death
--last date of linked data available from National Health Insurance profiles (June 30, 2004)
Cumulative incidence of cirrhosis within each serum HBeAg status derived for three categories of HBV DNA consistent with current guidelines:
<10,000 copies/ml
>=10,000 to <100,000 copies/ml
>=100,000 copies/ml
Cox proportional hazards modeling was used to estimate the relative risk of liver cirrhosis.
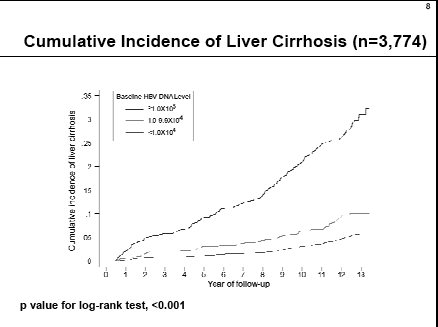
Three HBV DNA levels are depicted below: <10,000, 10,000 to 100,000, and >100,000 copies/ml. You can see the differences in the cumulative incidence of liver cirrhosis in the graph between each group, as viral load increases incidence of cirrhosis increases.
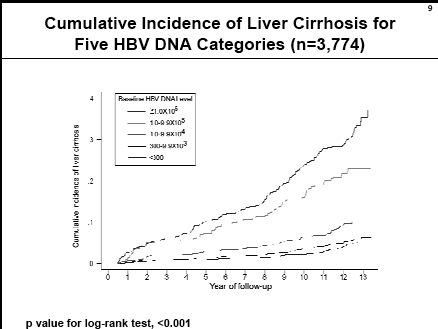
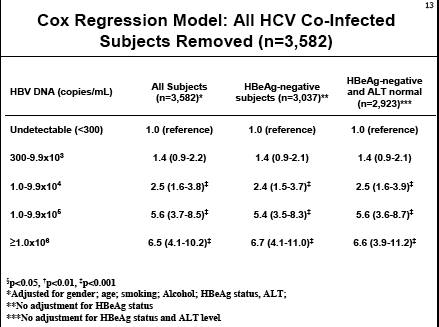
The graph below breaks it down by 5 HBV DNA levels starting with <300 copies/ml, next is 300 to 1,000 & the highest level is >1 million copies/ml. Again, as viral load increases risk increases.

|
|
| |
| |
|
 |
 |
|
|