| |
Tenofovir for patients with lamivudine-resistant hepatitis B virus (HBV) infection and high HBV DNA level during adefovir therapy
|
| |
| |
Hepatology august 2006
Volume 44, Issue 2, Pages 318-325
Florian van Bommel 1, Bernhard Zollner 2, Christoph Sarrazin 3, Ulrich Spengler 4, Dietrich Huppe 5, Bernd Moller 6, Heinz-Hubert Feucht 2, Bertram Wiedenmann 1, Thomas Berg 1 *
1Medizinische Klinik mit Schwerpunkt Hepatologie und Gastroenterologie, Charite - Campus Virchow-Klinikum; Universitatsmedizin Berlin, Berlin, Germany
2Institut fur Medizinische Mikrobiologie und Immunologie, Universitats-Krankenhaus Eppendorf, Hamburg, Germany
3Klinik fur Innere Medizin II, Universitatsklinikum des Saarlandes, Homburg/Saar, Germany
4Zentrum fur Innere Medizin, Universitatsklinikum Bonn, Bonn, Germany
5Gastroenterologische Gemeinschaftspraxis Herne, Herne, Germany
6Hepatologische Schwerpunktpraxis, Berlin, Germany
ABSTRACT
Incomplete virological response to adefovir dipivoxil (ADV) has been observed in patients with lamivudine-resistant hepatitis B virus (HBV) infection and may be associated with developing resistance and disease progression. We therefore investigated whether the efficacy of viral suppression could be improved by replacing ADV with tenofovir disoproxil fumarate (TDF).
Twenty patients with chronic HBV infection (18 HBeAg+), viral breakthrough during lamivudine therapy, and persistent viral replication (>10[4] copies/mL) after 15 months of ADV monotherapy (range 4-28 months) were treated with TDF 300 mg daily and were retrospectively analyzed. (Most patients had 6 to 7.5 logs HBV-DNA at baseline before starting tenofovir therapy).
A screening for nucleoside/nucleotide analogue resistance mutations within the HBV polymerase gene was performed in all patients by direct sequencing.
Within a median of 3.5 months, application of TDF led to undetectable HBV DNA in 19 of 20 patients, as demonstrated by suppression of HBV DNA below the detection limit of 400 copies/mL.
Initially elevated ALT levels had normalized in 10 of 14 patients by the end of follow-up (median 12 months, range 3-24 months).
Four patients lost HBeAg, after 3, 4, 5, and 16 months, and one patient seroconverted to anti-HBs after 16 months of TDF therapy.
Lamivudine-associated mutations (rtV173L, rtL180M, rtM204V/I) could be detected in 6 patients at baseline of TDF, but this obviously did not influence the response.
ADV-resistant mutations were not detected.
No side effects were reported.
In conclusion, these preliminary observations strongly suggest that TDF might be a highly effective rescue drug for HBV-infected patients with altered responsiveness to treatment with lamivudine and ADV.
Results
Clinical and Virological Response to Tenofovir.
Serum HBV DNA and ALT levels of the patients throughout the clinical course of the ADV and TDF treatments are shown in Figs. 1 and 2. In months 3 and 6 the median decrease of HBV DNA was -3.37 ± 1.0 log10 copies/mL (range -1.36 to -5.7) and -3.7 ± 1.1 log10 copies/mL (range -1.36 to -6.7), respectively. At the end of the observation period (median 12 months, range 3-24 months), the median decrease of HBV DNA was -3.8 ± 1.1 log10 copies/mL (range -1.36 to -6.7).
Figure 2. Median HBV DNA () and ALT () levels during ADV and consecutive TDF therapy. Standard deviation of median is indicated by error bars. Note that none of the baseline factors as described in Table 1 had a significant influence on the HBV DNA decline during the TDF period (*lower limit of detection, which was 400 copies/mL).
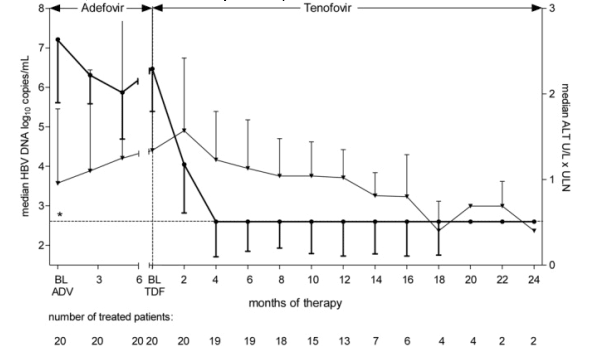
Suppression of HBV DNA to an undetectable level (detection limit 400 copies/mL) was achieved in 19 of the 20 patients after a median duration of TDF treatment of 3.5 months (range 1-8 months). The only patient who remained viremic had received a reduced TDF dose (patient 4, 300 mg every second day) because of renal insufficiency. A mild flare of ALT levels was observed in 13 patients, 8 of whom already had elevated ALT at the beginning of the TDF treatment (Fig. 1). However, at the end of the observation period, 16 of the 20 patients had normal ALT values. Significant side effects or changes in creatinine levels did not occur. Four patients (patients 7, 12, 13, and 16) lost the HBeAg, after 5, 16, 3, and 4 months of TDF therapy, respectively. Anti-HBe could not be detected within the short observation period. In month 16 patient 12 additionally seroconverted from HBsAg to anti-HBs at a titer of 1000 IU/mL.
Mutations Within HBV Polymerase Gene.
At baseline of the ADV therapy, serum samples from 11 patients were available for sequence analysis of the HBV polymerase gene. In 8 of these patients, mutations associated with lamivudine resistance were detectable (rtV173L, rtL180M, rtM204V, and rtM204I, Fig. 3A). All patients in whom the rtM204V mutation was found had the HBV genotype A. At baseline of the TDF treatment, sequence analysis revealed the lamivudine resistance-associated mutations had persisted in 6 of the patients after a median duration of ADV treatment of 15 months (range 6-24 months; Fig. 3B, Table 1). Mutations previously described as associated with ADV resistance (rtA181V or rtN236T) were not present in any of the 20 patients. In addition, no other described mutations or newly introduced stop codons were found in the polymerase gene or in the overlapping S gene (Fig. 3B and Table 1). The presence of the mutations at rt180 and rt204 apparently had no influence on the efficacy of the consecutive TDF therapy.
The HBV polymerase gene of patient 4, who was found to have only a weak response to TDF therapy, was again sequenced after 12 months of TDF treatment. However, no newly introduced amino acid exchanges could be found (data not shown).
Discussion
This analysis, although only including a small number of patients, provides the first clear evidence of the high anti-HBV efficacy of TDF at a dosage of 300 mg daily in patients with lamivudine resistance showing persistently high-level HBV replication during therapy with ADV. The patients described here all had a similar clinical course and treatment response. Thus, all patients still had elevated HBV DNA levels (>10[4] copies/mL) when lamivudine was switched to ADV, and they remained elevated and even partially increased during further ADV therapy. Some patients also showed an increase in initially elevated ALT levels.
The unresponsiveness to both a nucleoside and a nucleotide analogue is rather surprising, considering that ADV is known to inhibit viral polymerase in a manner similar to that of lamivudine regardless of the presence of mutations associated with lamivudine resistance (rtV173L, rtL180M, and rtM204V).[28] Moreover, these mutations were found to persist in only 6 patients through the ADV treatment period, making it very unlikely that they had a significant influence on the response to ADV in the 20 patients described here. The presence of YMDD mutations also had no influence on the consecutive TDF therapy.
All the patients in this study had undergone sequential therapy, first with lamivudine and then, after developing a viral breakthrough, with ADV. Treating treatment-naive patients with the combination of lamivudine and ADV is controversial; however, in lamivudine-resistant HBV-infected individuals, combination therapy was shown to be more effective than ADV monotherapy.[29][30] Moreover, a recent study by Lampertico et al. demonstrated that the addition of ADV to ongoing lamivudine in an early stage of lamivudine resistance was significantly more effective in suppressing HBV DNA than was delayed onset of combination therapy after HBV DNA increased again to levels greater than 8 log10 copies/mL.[31] Thus, early combination therapy with lamivudine and ADV might have prevented the incomplete response to ADV seen in the patients described in our study.
As already previously discussed, it seems quite likely the differences in dosage between the two drugs are primarily responsible for the failure of ADV to confer a sustained virological response.[32] Indeed, in one study analyzing viral suppression, it was clearly documented that a dose of 30 mg ADV was superior to 10 mg.[3] In this respect, it is intriguing that the only patient who did not become HBV DNA negative during the observation period received a reduced TDF dose because of renal insufficiency. Differences between TDF and ADV in intracellular phosphorylation kinetics and possibly in immunoregulatory mechanisms should also be considered as responsible for the observed differences in the antiviral effects of the two drugs.[33][34]
This follow-up study of patients with incomplete virological response to ADV has demonstrated, in agreement with our previous findings, the superiority of TDF over ADV in suppressing HBV replication in lamivudine-resistant HBV infections.[14] However, many questions remain. For instance, it would be beneficial to know whether TDF is capable of clearing both the replicating forms in the hepatocyte cytoplasm and the HBV covalently closed circle DNA (cccDNA) inside the nucleus, which is the intrahepatic replicative intermediate of HBV.[35] A decline of intrahepatic cccDNA was observed during long-term ADV therapy.[36] Interestingly, in this study no correlation could be found between the changes in HBV cccDNA levels and changes in aminotransferase levels or histology. Again, in our study only 10 of the 14 patients with elevated ALT at the beginning of TDF therapy achieved normal ALT levels, whereas HBV DNA was undetectable (less than 400 copies/mL, the limit of detectability) in 19 of the 20 patients after a median duration of 3.5 months. The mild flare of aminotransferase levels observed in 13 patients during TDF treatment could be an indicator of heightened immunological activity and breakage of HBV tolerance, providing favorable conditions for HBeAg seroconversion.
In conclusion, before we can definitively determine if TDF is superior to ADV in achieving a sustained viral response - as these individual observations suggest - we need to follow these patients for much longer periods. These long-term studies certainly would clarify the very important question of whether indeed HBV will have lower drug resistance to TDF than to ADV.
Article Text
Complete and sustained suppression of viral replication remains the most important goal in the treatment of patients with chronic hepatitis B virus (HBV) infection.[1][2] In this respect, the introduction of the nucleoside analogue lamivudine and the nucleotide analogue adefovir dipivoxil (ADV) largely improved the outcome in these patients, also by preventing hepatitic decompensation or the development of hepatocellular carcinoma.[3-5] These compounds also have a place when interferon-alpha based therapy is contraindicated, as in patients with acute liver failure, decompensated cirrhosis, or extrahepatic manifestations.
However, a major disadvantage of nucleoside/nucleotide analogues is that resistant hepatitis B virus mutants develop during long-term treatment, limiting the efficacy of these analogues in suppressing viral replication. As demonstrated in recent studies, approximately 70% of patients receiving lamivudine therapy for more than 4 years suffer the emergence of lamivudine-resistant HBV variants caused by mutations in the C domain of the HBV polymerase gene.[6]
In contrast, previous studies showed ADV to be effective against lamivudine-resistant HBV in vivo, hardly showing any viral resistance during 60 weeks of treatment.[7] It was therefore hoped that prolonged suppression of HBV replication by ADV might offer an optimal therapeutic option for lamivudine-resistant patients.[8][9]
Unfortunately, it has turned out that genotypic HBV resistance also occurs with ADV, most likely after treatment for more than 1 year and in patients with persistent HBV DNA replication during ADV treatment.[10][11] The two mutations, rtA181V and rtN236T, mapped in the B and D domains of the HBV polymerase gene could be identified as mediating ADV resistance. In the meantime, resistance rates of 18% and up to 28% were reported after 4 and 5 years of treatment, respectively.[12][13] Moreover, clinical studies of patients with lamivudine resistance have demonstrated an initially weak response or nonresponse to ADV in up to 28% of patients with a decrease of HBV DNA of <1 log10 copies/mL after 48 weeks of treatment without association to known viral mutations.[8][9][14]
Tenofovir disoproxil fumarate (TDF), another antiviral drug with a molecular structure related to ADV is licensed for the treatment of HIV infection at an oral dose of 300 mg. In long-term treatment of HIV infection, TDF has shown strong antiviral activity and a favorable safety profile. Nevertheless, several cases of TDF-associated renal toxicity were reported.[15] Recently, in a series of small studies, TDF was also shown to possess potent anti-HBV activity.[14][16-21] Most important, TDF was shown to be able to reduce HBV DNA more rapidly, more consistently, and in a significantly higher proportion of patients compared to with lamivudine and ADV. Remarkably, no significant side effects were noted, resistance was nil, and efficacy was not affected by coexistent HIV infection or concomitant lamivudine therapy. However, only a few studies have evaluated TDF in HBV-infected patients with failure of lamivudine and ADV therapy.[22] Here we describe 20 patients with chronic HBV infection who suffered a viral breakthrough during lamivudine therapy followed by an incomplete virological response to ADV with persistently high viral replication and who showed a rapid virological response when TDF was applied at a dosage of 300 mg/day.
Patients.
One hundred and twenty-seven patients with chronic HBV infection who had suffered a viral breakthrough during lamivudine therapy (defined as >1 log10 increase of HBV DNA from nadir) were consecutively treated with ADV monotherapy at five centers in Germany. Because of an insufficient virological response to ADV, 20 of these patients were switched to TDF monotherapy and included in this retrospective report. All patients had self-reported good compliance to ADV treatment. Before TDF was prescribed at a daily dose of 300 mg, all patients gave written informed consent for the nonapproved use of TDF. The baseline characteristics of the patients are shown in Table 1. None of the patients was immunocompromised or had an HIV coinfection. ADV and TDF were administered as monotherapy, and there was no time gap when ADV was switched to TDF. One patient, who had HBV-associated glomerulonephritis (patient 4), was found to have renal insufficiency with a creatinine clearance of 34 mL/min. On average baseline HBV-DNA at start of TDF therapy was 6 to 8 logs. One patient had 9.31 logs HBV-DNA before starting TDF.
Insufficient virological response to ADV was defined as a reduction in HBV DNA of less than 1 log copies/mL, a persistently high level of HBV replication (greater than 10[6] copies/mL after 4 months), or an HBV DNA level still greater than 10[5] copies/mL after 12 months of ADV treatment.
Treatment Schedules Prior to Application of Tenofovir.
Prior to treatment with ADV, the patients had been treated with lamivudine for a mean of 25.5 months (range 6-60 months). After an initial response to lamivudine, all patients suffered a viral breakthrough in the course of therapy as a consequence of lamivudine resistance. In this situation lamivudine was replaced by ADV at a daily dose of 10 mg.
Following ADV therapy, HBV DNA levels decreased only slightly (median -0.58 log10copies/mL, range -3.4 to +4.3 log10copies/mL) or even increased (in 7 patients). ALT levels normalized in 1 of 11 patients with initially elevated ALT and increased in 8 patients. After a median duration of 15.5 ± 6 months of therapy (range 4-28 months), all patients still had HBV DNA elevated by greater than 4 log10 copies/mL (median 3.0 _ 10[6] copies/mL, range 1 _ 10[4]-2.0 _ 10[9] copies/mL) and were thus eligible for treatment with TDF at a daily dose of 300 mg. At this time, 14 of the 20 patients still had elevated liver enzymes. The patient suffering from renal insufficiency (patient 4) was treated with a dose of 300 mg every second day according to the manufacturer's dose reduction recommendation. All antiviral drugs were applied as monotherapy, and there was no time gap when the drugs were switched.
Detection of HBV Markers.
Serum antibody to hepatitis B virus s antigen (HBsAg), antibody to hepatitis B e antigen (HBeAg), and antibody to hepatitis B core antigen-specific immunoglobulin G and immunoglobulin M were measured using commercially available immunoassays (Bayer HealthCare Diagnostics, Tarrytown, NY). Serum HBV-DNA was measured before and during treatment with ADV and TDF using a polymerase chain reaction (PCR) assay (linear dynamic range 400-200,000 copies/mL, Hoffmann-La Roche Limited, Basel, Switzerland). Samples with HBV DNA greater than 200,000 copies/mL were diluted to achieve the absolute level.
Sequencing of Patient-Derived HBV DNA and Genotyping of HBV.
The HBV polymerase gene was sequenced from frozen serum, stored at -70 C, obtained from all 20 patients when ADV was switched to TDF. In addition, serum samples of 11 patients were available for sequencing from the time point when lamivudine was switched to ADV. HBV DNA was extracted from 200 L of serum as previously described.[23] To investigate mutations associated with drug resistance, the HBV polymerase region was amplified as previously described by Allen et al.[24] We are using recently published nomenclature for amino acid positions in the polymerase gene.[25] With nested PCR and using primers 252 (5-AGACTCGTGGTGGACTTCTCT-3) and 1309 (5-AGAATGTTTGCTCCAGACC-3) as external primers and 377 (5-GGATGTGTCTGCGGCGTTT-3) and 998 (5-ACGTTGACAGACTTTCCAATC-3) as internal primers, a PCR product bridging the polymerase region from codon rt88 to codon rt282 was amplified. The PCR products were separated on 2% agarose gel (NuSieve 3:1, FMC, Rockland), eluted with Gene-Clean (Bio 101 Inc., Vista, USA), and directly sequenced using a BigDye Terminator Cycle Sequencing Ready Reaction Kit (Applied Biosystems) with an automated sequencer (AbiPrism). The derived sequences of both strands of the amplification products were investigated for lamivudine-resistance-associated mutations rtV173L, rtL180M, and rtM204I/V/S, as well as for ADF-resistance-associated mutations rtA181V and rtN236T. HBV genotypes were determined by sequence alignment of the overlapping hepatitis B surface antigen with HBV sequences derived from the gene bank as previously described.[26][27]
|
|
| |
| |
|
|
|