 |
 |
 |
| |
Pattern of serial HBV DNA level and HCC development in Patients with Liver Cirrhosis
|
| |
| |
AASLD Sunday, November 02, 2008
J. Kwon, J. Choi, H. Woo, J. Kim, C. You, S. Bae, S. Yoon, N. Han, C. Lee, Y. Lee, Internal Medicine, College of Medicine, Catholic University, Seoul, SOUTH KOREA;

ABSTRACT
Aims
Hepatitis B virus (HBV) DNA level was known to be a strong predictor of hepatocellular carcinoma (HCC) in REVEAL study. The majority of studies assessed the one time of HBV DNA level at the time of chronic hepatitis or/and HCC development. The aim of this study is to know whether the pattern of serial HBV DNA level is associated with the development of HCC.
Methods
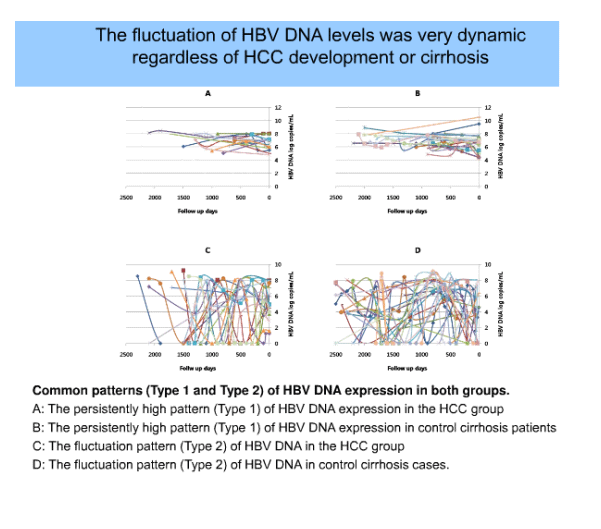
Among 352 patients who diagnosed a newly HBV related HCC between Jan 2005 and Dec 2007, 49 cirrhosis patients with serial HBV DNA level over 1 year before the HCC development was enrolled in the study. 98 consecutive cirrhosis patients with serial HBV DNA level during the same period were recruited as controls. 29 patients (59.2%) in HCC group and 52 patients (55.1%) in the control have been treated with antiviral agent. The changing patterns of serial HBV DNA were arbitrarily classified as follows; Type 1, persistently high pattern (≥104 copies/mL (C/mL))of DNA titer without interval change of 1-2 log C/mL, type 2, fluctuation pattern of DNA titer over the range of 2-3 log C/mL, type 3, decreasing pattern of DNA titer <104 C/mL, type 4, increasing pattern of DNA titer ≥104 C/mL, and type 5, persistently low pattern of DNA titer (<104 C/mL).
Results
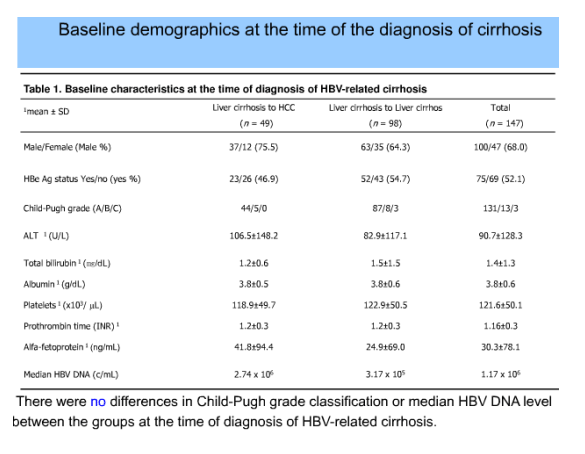
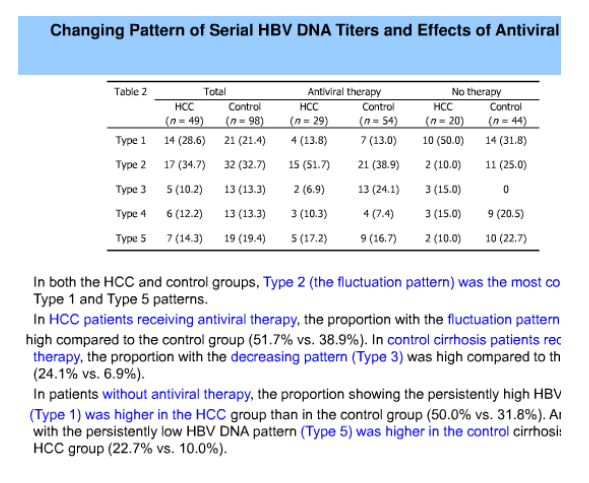
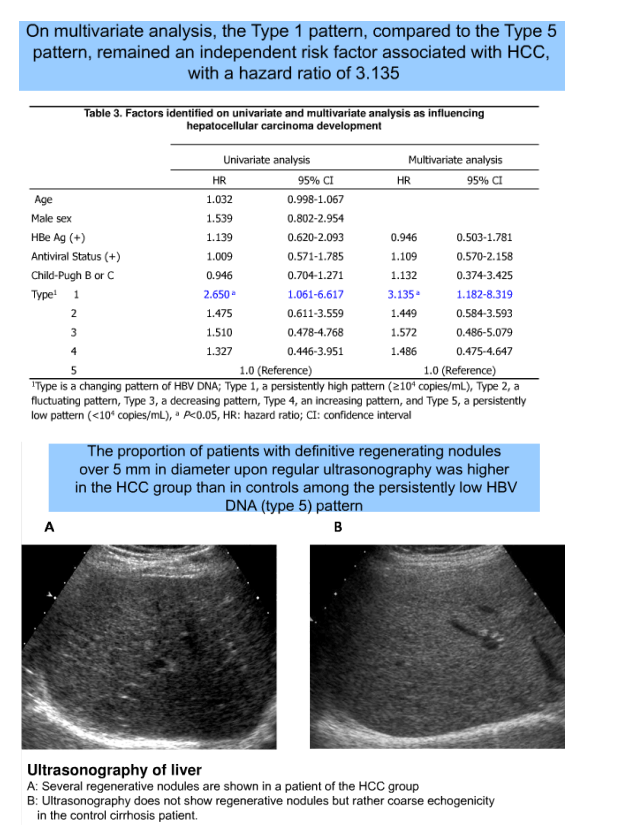
There was no difference of age, sex, HBe Ag status, antiviral therapy status and Child-Pugh class in HCC and control group. For a median 1,682 (365-2521) interval days, type 1 and type 2 were frequent in the HCC group compared with the control (28.6% vs 21.4%, 34.7% vs 32.7%, respectively). Frequency of type 3 and type 5 were lower in the HCC group than in the control (10.2% vs 13.3%, 14.3% vs 19.4%, respectively). With reference to the pattern of type 5, the patients of type 1 had the highest risk of HCC (HR=2.650; 95% CI, 1.061-6.617; P=0.037). On multivariate analysis adjusted by age, sex, HBe Ag status and antiviral therapy status, type 1 (HR 3.109; 95% CI, 1.161-8.327, P=0.024) and age (HR 1.042; 95% CI, 1.007-1.077, P=0.017) were independent risk factors of HCC. Among the patients with type 5, the number of patients with regenerating nodules on the ultrasonography was more in the HCC group than in the control (42.8% vs 27.7%).
Conclusions
The cirrhosis patients with persistently high pattern (≥104 C/mL) of HBV DNA titer have more than three times of risk of HCC than those with persistently low pattern (<104 C/mL). Our results suggest that sequential analysis and persistent suppressing of HBV DNA are important in the monitoring of cirrhosis patients for the HCC development. Even in those with persistently low pattern of HBV DNA titer, the patients with regenerating nodules should be carefully observed for the HCC development.
Disclosure: Jung Hyun Kwon: No conflict of interest; Jong Young Choi: No conflict of interest; Hyun Young Woo: No conflict of interest; Jin Dong Kim: No conflict of interest; Chan Ran You: No conflict of interest; Si Hyun Bae: No conflict of interest; Seung Kew Yoon: No conflict of interest; Nam Ik Han: No conflict of interest; Chang Don Lee: No conflict of interest; Young Sok Lee: No conflict of interest


|
| |
|
 |
 |
|
|