 |
 |
 |
| |
HCV Late Breaker Posters this Morning at AASLD.....
|
| |
| |
ABT450, BMS790052 NS5A+proteaseBMS650032, BI 201335+HCV polymerase inhibitor BI 207127+ribavirin
by Jules Levin
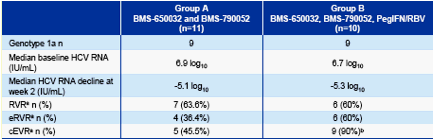
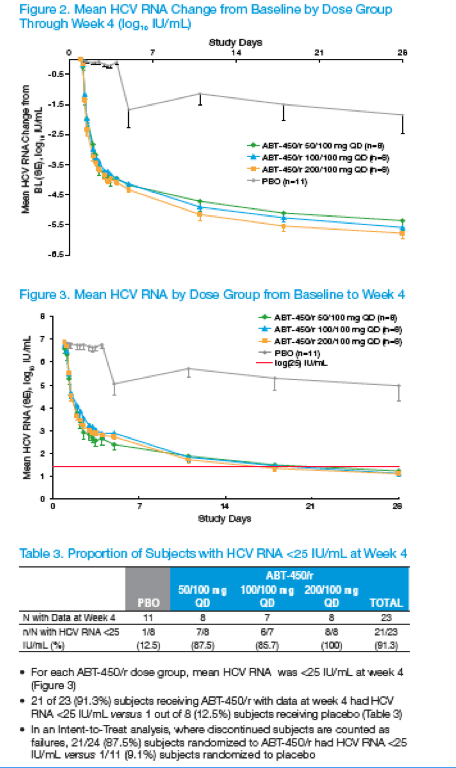
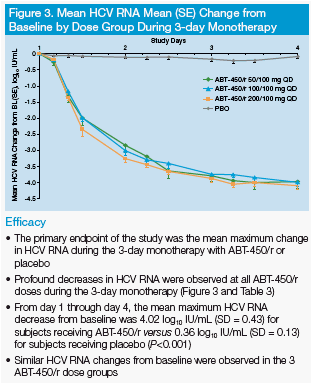
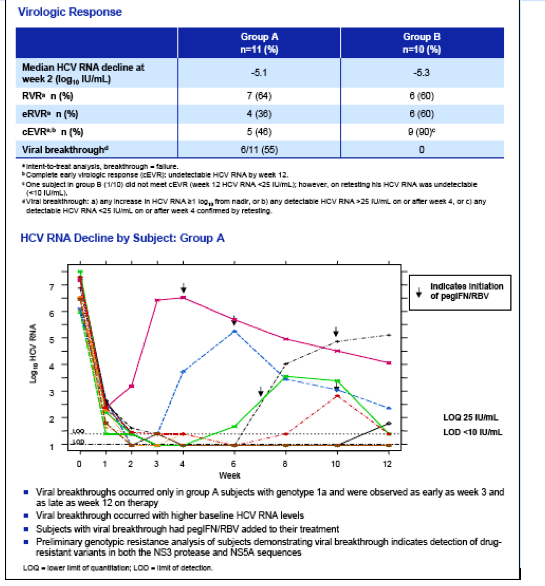
This morning was the Late Breaker HCV poster session where the Abbott protease inhibitor ABT450/r (boosted with low dose ritonavir) reported an impressive average 4 log reduction with once daily dosing after only 3 days of monotherapy. See pic below. There do not appear to be safety issues. Then Abbott also reported 4 weeks with ABT450/r + peg/rbv showing average 5.5 log reductions and 21/23 achieving undetectable viral load. Perhaps the most highly anticipated data is the BMS 2 oral HCV drug study where null-responder patients received the BMS protease + their NS5A inhibitor without peg/rbv in the poster titled: Combination Therapy With BMS-790052 and BMS-650032 Alone or With Pegylated Interferon and Ribavirin (pegIFN/RBV) Results in Undetectable HCV RNA Through 12 Weeks of Therapy in HCV Genotype 1 Null Responders-- with 6/11 patients having viral breakthrough by week 12, all genotype 1a but 5/11 sustaining undetectable viral load with 2 orals only. In the 10 null-responders receiving the 2 oral drugs+peg/rbv everyone was undetectable after 12 weeks. Of note it appears viral failures can be rescued with peg/rbv right after viral rebound with the 2 orals. (see pics below)
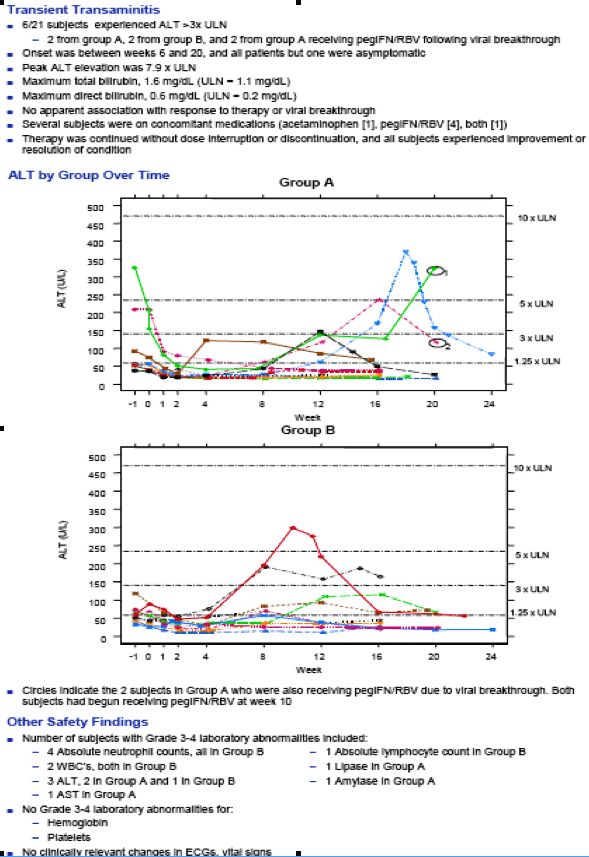
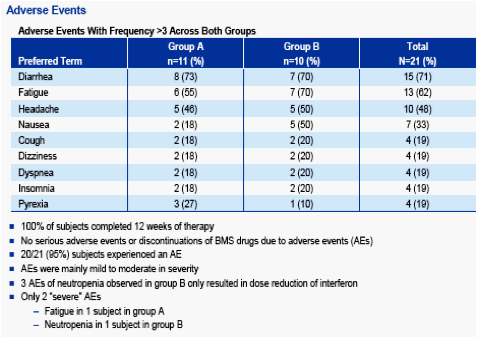
"Six (54.5%) group A subjects experienced viral breakthrough, while all subjects in group B maintained viral suppression. Viral breakthrough occurred exclusively in individuals infected with GT 1a, occurring as early as week 3 and as late as week 12. The 2 GT 1b subjects in group A remained HCV RNA undetectable. The 6 subjects with viral breakthrough had pegIFN/RBV added to their regimen. HCV RNA levels fell to UD in 2 subjects and to <25 IU/mL in another 2 subjects, while the other 2 subjects had ≥1.5 log10 decreases in HCV RNA levels. No deaths, serious adverse events, or discontinuations due to adverse events were recorded during the analysis period. Diarrhea was the most common adverse event and was mainly mild to moderate in severity. Conclusions: Treatment with BMS-790052 and BMS-650032 with or without pegIFN/RBV demonstrated similar RVR rates in HCV-infected GT 1 null responders. Six of 11 subjects receiving 2 direct-acting antiviral agents alone experienced viral breakthrough by week 12 while a 4-drug combination maintained viral suppression in all subjects. Should this activity predict SVR, these results will have significant implications for future combination HCV antiviral therapy."
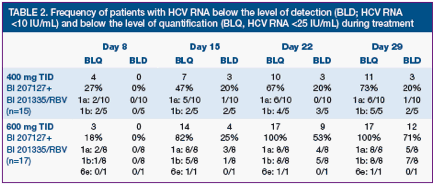
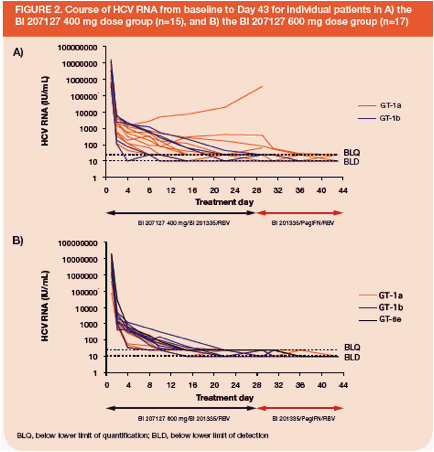
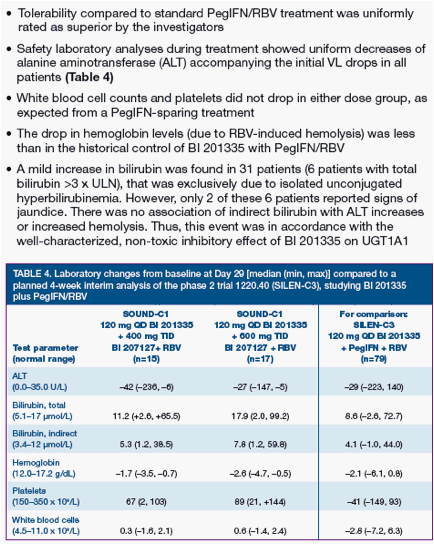
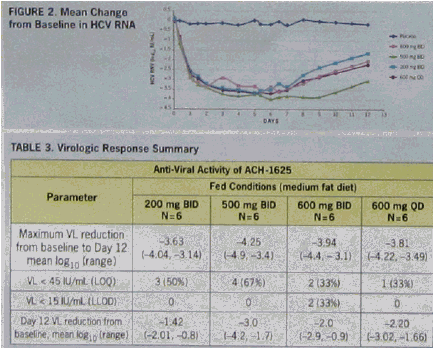
Today at Late Breakers: Achillion presented a poster on their HCV protease showing 4-l0g reductions with 6 days monotherapy but they saw some bilirubin elevations so they will try a lower dose. Boerhinger Ingelheim presented very interested data combining 2 oral HCV drugs, their protease plus a NNRTI with ribavirin and saw 17/17 undetectable in their study titled: "Strong antiviral activity and safety of IFN-sparing treatment with the protease inhibitor BI 201335, the HCV polymerase inhibitor BI 207127, and ribavirin, in patients with chronic hepatitis C: the SOUND-C1 trial".
"At baseline, mean age was 51 ± 11 years, mean body mass index 23.8 ± 3.4 kg/m2, mean VL 6.48 log10. All patients had a rapid and sharp VL decline during the first 2 days, followed by a slower second phase decline in all except 2 patients. One patient experienced VL breakthrough (increase by >1 log10 from nadir during treatment) and 1 other experienced a 0.7 log10 VL increase. Both were in the lower dose group and were GT-1a patients with high baseline VL. On Day 29, all patients were switched per protocol to treatment with BI 201335 and PegIFN/RBV. Virological response rates (VL <25 IU/mL) after 1, 2, 3 and 4 weeks of oral treatment are shown in the table." see pics below."
BMS Protease+ NS5A only & with peg/rbv

ABT-450/r
Achillion Protease
PRESS RELEASES
Presented: Tuesday, 2 November 2010, 9:15 am
Final Results of Clinical Trial on Boceprevir
The final results of the RESPOND-2 trial demonstrated that combination therapy with Boceprevir yields higher sustained virologic response (SVR) rates for patients with hepatitis C virus (HCV) genotype 1 who did not respond to or relapsed after treatment with peginterferon and ribavirin.
"We are excited to have new therapies for treatment of HCV patients who failed to respond to treatment, said Bruce Bacon, MD, "triple therapy appears to be a significant advance in the fight against hepatitis C."
Three arms were randomly selected from 403 HCV genotype 1 patients who previously failed treatment--partial/non-responders or relapsers.
· Control arm received peginterferon alpha 2b and ribavirin for 48 weeks
· Second arm received 4 weeks of lead-in therapy of peginterferon alpha 2b and ribavirin followed by response-guided therapy of peginterferon alpha 2b and ribavirin combined with 800 mg of Boceprevir three times a day
· Third arm received 4 weeks of lead-in therapy of peginterferon alpha 2b and ribavirin followed by 44 weeks of peginterferon alpha 2b and ribavirin combined with 800 mg of Boceprevir
At 24 weeks after conclusion of treatment, the control arm achieved a SVR of 21 percent. Adding Boceprevir to the treatment increased SVR to 59 percent for the second arm and 67 percent for the third arm. It was noted that previous relapsers fared better than nonresponders in all arms. The therapy was well-tolerated, and the most common reason for discontinuing treatment was for patients who still had detectable HCV-RNA at week 12.
"Patients who previously failed to respond to treatment now have a hope for viral eradication," added Dr. Bacon.
Abstract title:
HCV RESPOND-2 Final Results: High Sustained Virologic Response Among Genotype 1 Previous Non-Responders and Relapsers to Peginterferon/Ribavirin when Re-Treated with Boceprevir Plus PEGINTRON (Peginterferon alfa-2b)/Ribavirin
-----------------------------------------
Presented: Tuesday, 2 November 2010, 8:00 am
Increased SVR and Decreased Adverse Events Reported in Final Results of Phase 3 Study on Telaprevir
The Phase 3 results from the ADVANCE study confirm the clinical benefits of telaprevir-based combination therapy regimens. The study reports an improvement in treatment discontinuation rates due to adverse events compared to Phase 2 studies, and demonstrates an increase in sustained viral response (SVR) in patients with hepatitis C virus (HCV). The primary endpoint for this study was SVR 24 weeks after last treatment.
The study was conducted on 1088 treatment-naïve HCV patients, all of whom had genotype 1. For the three arms of the trial, one group of patients was treated with 750 mg of telaprevir every eight hours in combination with peginterferon alfa-2a 180 ug/week and ribavirin 1000-1200 mg/day for 12 weeks, while the second group was given the same treatment but for only 8 weeks. Patients in the first group (T12PR) were treated for an additional 12 weeks of peginterferon and ribavirin if HCV RNA was undetectable at weeks 4 and 12, for a total of 24 weeks of treatment, and an additional 36 weeks if HCV RNA was detectable at week 4 or week 12, for a total of 48 weeks' treatment. Patients in the second group (T8PR) were treated with peginterferon and ribavirin for an additional 16 weeks if HCV RNA was undetectable at weeks 4 and 12, and for an additional 40 weeks if HCV RNA was detectable at either week 4 or 12, for a total of 24 or 48 weeks of treatment, respectively. Patients in the control group were treated with peginterferon alfa-2a and ribavirin for 48 weeks.
SVR was 75 percent for those receiving telaprevir combination treatment for 12 weeks, 69 percent for those receiving telaprevir combination treatment for 8 weeks, and 44 percent for those receiving standard of care. Extended rapid virologic response (HCV RNA undetectable at weeks 4 and 12) was attained in 58 percent, 57 percent, and 8 percent, respectively. During the telaprevir/placebo treatment phase, adverse events leading to treatment discontinuation occurred in 7 percent of patients in the arm receiving telaprevir combination treatment for 12 weeks, 8 percent in telaprevir for 8 weeks, and 4 percent in the peginterferon alfa-2a and ribavirin arm.
Abstract title:
Telaprevir in Combination with Peginterferon and Ribavirin in Genotype 1 HCV Treatment-Naïve Patients: Final Results of Phase 3 ADVANCE Study
----------------------------------------
Hepatitis Debrief to Debut at The Liver Meeting: Interview with Dr. Paul Pockros
By Morgan Fincham, AASLD Staff
Paul J. Pockros, MD, head of the Division of Gastroenterology/Hepatology and Director of the SC Liver Research Consortium at the Scripps Clinic and Adjunct Associate Professor at The Scripps Research Institute, provides a look at the first ever Hepatitis Debrief being launched at The Liver Meeting 2010.
Telapravir and Boceprevir have completed phase 3 trials and are both being formally presented at the meeting. "We expect widespread use of these drugs in the US and the EU," Dr. Pockros cautions, "but there is a significant concern that there will be improper use of these drugs because of a poor understanding of treatment regimens, treatment of special populations, and monitoring for antiviral resistance. "The focus group developed by AASLD earlier this year decided to establish the viral hepatitis debrief as a way to address these concerns," Dr. Pockros explains. AASLD is worried that physicians with improper education will use these new drugs in a casual manner, resulting in antiviral resistance to the class of drug, as happened with HIV. Dr. Pockros elucidates that HIV treatment and subsequent antiviral drug resistance is the model of caution used to formulate this debrief.
The rate of antiviral drug development will increase rapidly in the next 12-24 months. "What we are discussing this year is the first era of antivirals to be out in 2011," Dr. Pockros elaborates. "Many of the other drugs presented at The Liver Meeting won't be approved by the FDA until 2014 or later." The Hepatitis Debrief will be held every year, rapidly synthesizing the new data and keeping medical professionals current and correctly educated.
The clinical task force collaborating with Dr. Pockros as chair is comprised of Douglas Dieterich, MD; Fred Poordad, MD; Kirti Shetty, MD; and Donald Jensen, MD. They have designed the program to cover changes in pre-treatment predictors of response, monitoring of resistance during treatment, treatment of special populations, lessons from the phase 3 trials, and an overarching theme of what will be different about therapy that doctors can expect next year. There is also a list of new acronyms of antivirals and virology that doctors will have to learn.
To aid medical professionals in learning this new information, an enduring document will be made available for reference a few short months following the meeting, both online and in print. "We cannot make true AASLD guidelines," Dr. Pockros elaborates, "until the drugs are labeled by the FDA. However, we can provide a set of rules to follow for anyone treating patients with hepatitis C." The slides of the Hepatitis Debrief will be available as part of the Best of The Liver Meeting.
"All hepatologists don't know about these antivirals yet," Dr. Pockros expounds. "These rules are new and our knowledge in special populations such as HIV-coinfected patients and decompensated cirrhosis patients is lacking. This program will benefit anyone who is seeing patients in the next year, hepatologists and non-hepatologists alike." Attendees will walk away from this half-hour presentation with up-to-date information they may use in treating hepatitis C patients in 2011.
|
| |
|
 |
 |
|
|