 |
 |
 |
| |
High Prevalence of Bone Demineralization in a Cohort of HIV-Infected Postmenopausal Women
|
| |
| |
Reported by Jules Levin
18th Intl AIDS Conf July 18-23 2010 Vienna Austria
Chia-ching J. Wang, MD1; Geetha Gopalakrishnan2; Erna M. Kojic3, and Susan Cu-Uvin, MD3
1Alpert Medical School of Brown University, 2Women and Infants Hospital, 3The Miriam Hospital Providence, Rhode Island, USA
"STUDY OBJECTIVE: To assess the prevalence of decreased bone mineral density among HIV-infected postmenopausal women in the HIV Menopause Clinic at Miriam Hosp, Rhode Island.......It is estimated that by 2015, almost half of those living with HIV/AIDS in the US will be 50+ years old. Therefore, in the era of HAART, a growing number of women will experience menopausal transition while being HIV-infected. .....For older women, sorting out the interplay between HIV, aging/menopause, and the side effects of medications can be very difficult.....54% were vitamin D deficient (25-OH vitamin D level < 30 ng/mL).....18% were diagnosed with osteoporosis....59%% were osteopenic"

ABSTRACT
Background:
In the era of HAART, HIV-infected women are living longer and many will experience changes related to menopause. Osteopenia is prevalent in persons with HIV and is part of a normal sequence of aging in women. However, there is very little data on bone metabolism in HIV-infected postmenopausal women.
Methods:
HIV-infected women age > 45 were referred to the HIV Menopause Clinic at the Miriam Hospital (Providence, RI). A woman was considered postmenopausal if she was status-post bilateral salpingo-oophorectomy with or without hysterectomy, or if she had no menses for more than 1 year with elevated FSH and/or LH. Bone mineral density (BMD) was assessed by dual-energy X-ray absorptimetry (DEXA) in the lumbar spine and hip. We then calculated 10-year fracture risk for postmenopausal women with osteopenia using the FRAX tool, which was developed by WHO based on models that integrate the risks associated with clinical risk factors and BMD at the femoral neck.
Results:
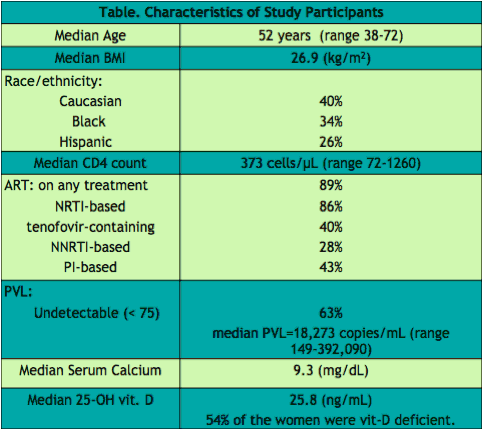
35 postmenopausal women were included. Median age was --52 years (range 38-72); 40% Caucasian, 34% African-American, 26% Latino. Median weight was 151 lb (range 99-261). Median follow-up since HIV diagnosis was 14 years. Median CD4 count was 373 cells/µL (range 72-1260). 86% were on NRTI-based HAART: 40% with TDF, 28% with NNRTI, and 43% with PI. 63% of subjects had plasma viral loads (PVL) <75 copies/mL. For the remainder, the median PVL was 18,273 copies/mL (range 149-392,090). 40% were current tobacco-smokers. 14% were on methadone maintenance. 17% had history of alcohol abuse. 40% self-reported their physical activity being inadequate. 54% did not consume sufficient amount of calcium. Mean serum level of calcium was 9.3 mg/dL.
54% were vitamin D deficient (25-OH vitamin D level < 30 ng/mL).
Based on WHO criteria, 18% were diagnosed with osteoporosis (t-score <-2.5 SD below normal) and 59% were osteopenic (t-score -1.0 to -2.5 SD below normal).
No patients in this cohort had a fracture since being infected with HIV.
Using the FRAX tool, we found the average 10-year risk for major osteoporotic fracture was ---7% and that for hip fracture was 1% for women with osteopenia.
Conclusions:
This cohort-based cross-sectional survey showed a high prevalence of osteopenia and osteoporosis. Although these women have not had fractures, they are relatively young. As they age, their bone demineralization will likely become more significant for their health and quality of life. Further studies are needed to investigate bone disorders in HIV-infected women.






|
| |
|
 |
 |
|
|