 |
 |
 |
| |
The SENSE Trial: Etravirine (ETR) shows fewer Neuropsychiatric Adverse Events than Efavirenz (EFV) in Treatment-naïve HIV-1 Infected Patients
|
| |
| |
Reported by Jules Levin
18th Intl AIDS Conf July 2010 Vienna Austria
IAC: The impact of switching to etravirine on efavirenz-related CNS toxicity - (08/04/10)
1. Brian Gazzard, St Stephen's Centre, Chelsea and Westminster Hospital, London, UK, 2. G Di Perri, Ospedale Amedeo di Savoia, Turin, Italy, 3. H Furrer, Inselspital, Berne, Switzerland, 4. P Domingo, Hospital de la Santa Cruz I Sant Pablo, Barcelona, Spain, 5. Andrew Hill, Pharmacology Research Laboratories, University of Liverpool, Liverpool, UK, 6. Yvon van Delft, Janssen-Cilag B.V., Tilburg, Netherlands, 7. Johan Vingerhoets, Tibotec BVBA, Beerse, Belgium, 8. Thomas Stark, Janssen-Cilag EMEA, Neuss, Germany, 9. Stephan Marks, Janssen-Cilag B.V., Tilburg, The Netherlands. Contact Details for Correspondence: Prof Brian Gazzard, St Stephens Centre, Chelsea and Westminster Hospital, London. Email: brian.gazzard@chelwest.nhs.uk
Author Conclusions
After 12 weeks, first-line treatment with etravirine 400mg once daily + 2NRTIs led to significantly fewer neuropsychiatric adverse events than efavirenz + 2NRTIs.
There were larger rises in Total Cholesterol and LDL cholesterol during treatment with efavirenz plus 2 NRTIs, compared with etravirine + 2NRTIs.
The short-term virologic and immunologic efficacy profiles were similar in the two arms.
Background
Neuropsychiatric adverse events (AEs) are a common problem with efavirenz treatment.
A pilot study has shown reductions in neuropsychiatric adverse events in patients who switched from efavirenz to etravirine [1].
Pharmacokinetic data support the use of etravirine once daily [2].
The SENSE trial was designed to evaluate whether 12 weeks of treatment with once-daily etravirine plus two nucleoside analogues could lead to fewer neuropsychiatric adverse events than treatment with efavirenz plus two nucleoside analogues.
Methods
In the randomised, double-blinded, SENSE trial, 157 treatment-naïve patients with HIV RNA >5000 copies/mL were randomised to etravirine 400mg once daily (n=79) or efavirenz 600mg once daily (n=78), plus two investigator-selected NRTIs (TDF/FTC, ABC/3TC or ZDV/3TC).
Patients with screening HIV RNA levels above 5000 copies/mL and no genotypic resistance to NRTIs, NNRTIs or PIs were recruited. The randomisation was stratified by screening HIV RNA levels (above versus at or below 100,000 copies/mL). Patients were also genotyped after trial discontinuation.
The primary endpoint was the percentage of patients with Grade 1-4 drug-related treatment-emergent neuropsychiatric adverse events up to Week 12. The treatment arms were compared using logistic regression adjusting for the stratification factor of screening HIV RNA (above versus at or below 100,000 copies/mL).
Neuropsychiatric adverse events were defined prospectively from all reported adverse events, under double-blinded conditions. Adverse events in the System Organ Classes of "Nervous System" or "Psychiatric Disorders" were included, plus a limited number of adverse events in other System Organ Classes (eg. vertigo, irritability, photophobia).
Results
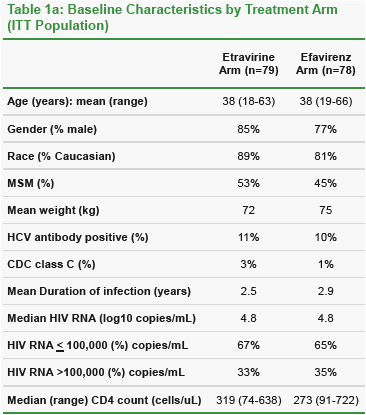
Baseline characteristics were well balanced between the treatment arms (Table 1a). Overall, the patients were 81% male and 85% Caucasian, with median age 36 years, baseline CD4 count 302 cells/uL and HIV RNA 4.8 log10 copies/mL, well balanced between the arms.
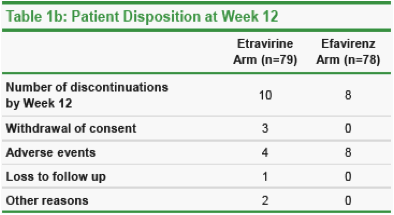
Eighteen patients discontinued the trial by Week 12 (10 in the etravirine arm, 8 in the efavirenz arm). Details are shown in Table 1b.
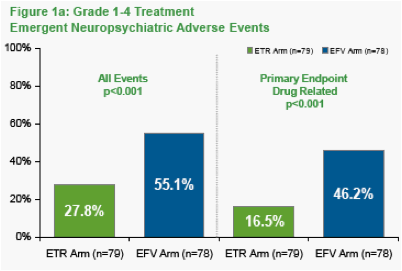
Figure 1a shows the percentage of patients with Grade 1-4 neuropsychiatric adverse events in the two treatment arms. In the Intent to Treat analysis, 13/79 patients (16.5%) in the etravirine arm versus 36/78 (46.2%) in the efavirenz arm reported at least one Grade 1-4 drug-related treatment-emergent neuropsychiatric adverse event (p<0.001).
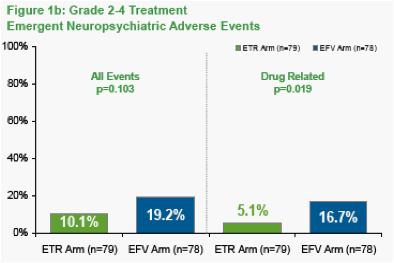
The number of patients with at least one Grade 2-4 treatment-emergent drug-related neuropsychiatric adverse events was 4/79 (5.1%) in the etravirine arm versus 13/78 (16.7%) in the efavirenz arm (p=0.019) (Figure 1b).
In the HIV-Patient Symptoms Profile questionnaire, patients in the etravirine arm also reported better neuropsychiatric tolerability than patients in the efavirenz arm.
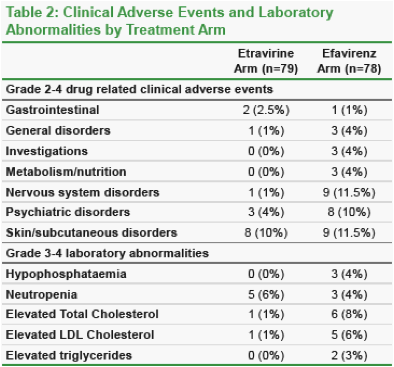
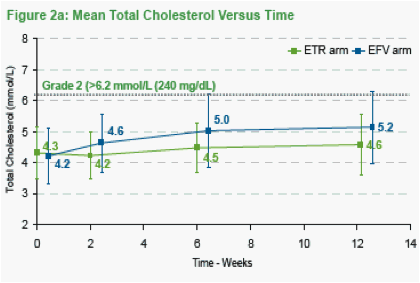
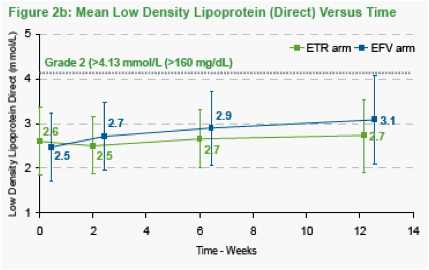
Table 2 shows clinical and laboratory adverse events by treatment arm. There were fewer Grade 3-4 elevations in total cholesterol and LDL cholesterol in the etravirine arm (1 and 1 patients) versus the efavirenz arm (6 and 5 patients).
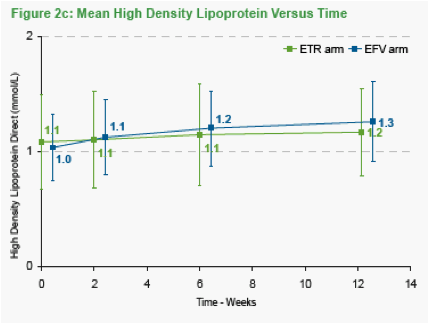
Figure 2 shows the mean Total Cholesterol, LDL and HDL Cholesterol by treatment arm. There were greater rises in Total Cholesterol and LDL in the efavirenz arm then the etravirine arm. The ratio of HDL to Total Cholesterol remained stable over time in both arms.
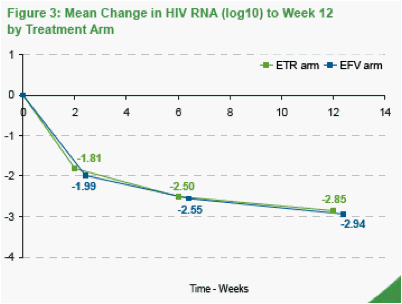
The mean change in HIV RNA to Week 12 was -2.9 log10 in both treatment arms (Figure 3). The median change in CD4 count was +146 cells/uL in the etravirine arm and +121 cells/uL in the efavirenz arm. The initial dynamics of log10 reduction in HIV RNA were similar between the treatment arms (Figure 3).
The percentage of patients with HIV RNA levels under 400 copies/mL at Week 12 was 87.9% in the etravirine arm versus 92.6% in the efavirenz arm. One patient in the efavirenz arm with persistently high HIV RNA levels during the trial had treatment emergent NRTI and NNRTI mutations.
|
| |
|
 |
 |
|
|