 |
 |
 |
| |
Abacavir Use and Cardiovascular Disease Events:
A Meta-Analysis of Published & Unpublished Data
|
| |
| |
Reported by Jules Levin
18th Intl AIDS Conf July 18-23 2010 Vienna Austria
Cruciani M, Zanichelli V, Serpelloni G, Bosco O, Malena M, Mazzi R, Parisi S
Center of Community Medicine & HIV Outpatient Clinic, Verona and Dept of Histology and Medical Biotechnology, University of Padua, Padua Italy

BACKGROUND.
An association between combination antiretroviral therapy and the risk of myocardial infarction has been demonstrated . Data from the “Data collection of Adverse events of Anti-HIV Drugs Group†(DAD) study show an association between exposure to protease inhibitors and an increased risk of myocardial infarction (1, 2). The current or recent (within the last 6 months) use of abacavir has been associated with an increased risk of cardiovascular disease within the setting of cohort studies (2-4) and of a randomized trial (5). Of note, no association was found with the cumulative use of abacavir (ABC). Moreover, no excess risk of myocardial infarction with ABC therapy has been observed among 3,205 patients from 5 randomized studies (6) and among 14,174 patients in the aggregated clinical trials database maintained by the manufacturer of ABC ( 7).
The concerns about ABC use and myocardial infarction are based mostly on data from observational cohort studies. Though rigorous observational studies provide stronger evidence than uncontrolled case series, they constitute low quality evidence and, in general, not adequate to support recommendations (8). By contrast, randomized trials provide stronger evidence than do observational studies.
The review principal aim is to combine all the evidence from randomised trials to estimate the effect of cART containing ABC on myocardial infarction.
RESULTS.
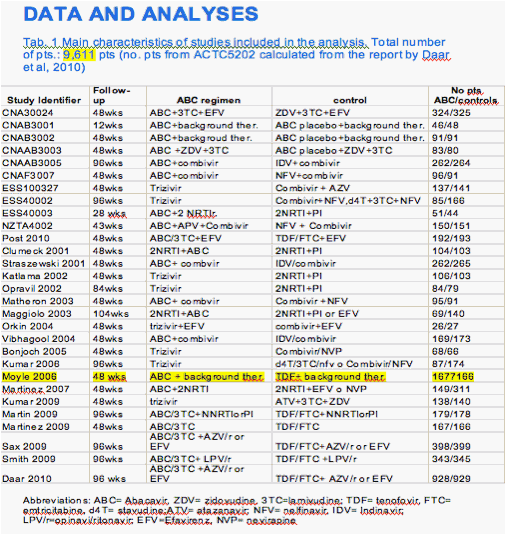
We obtained data from 29 RCTs (30 reports), for a total of 9,611 pts , conducted from 1996 to 2010, comparing cART with ABC to other NRTI (11-31). Data of 13 RCTs with at least 24 wks of ABC exposure were available from HIV data repository of the manufacturer of ABC (11). Data from 3 of these studies (ESS40003, CNB3014 and CNA109586) were also available from published material (Clumeck et al, Vibhagol et al, Post et al) and, to avoid duplicate records, we extracted data from the published material only (17, 29, 30).
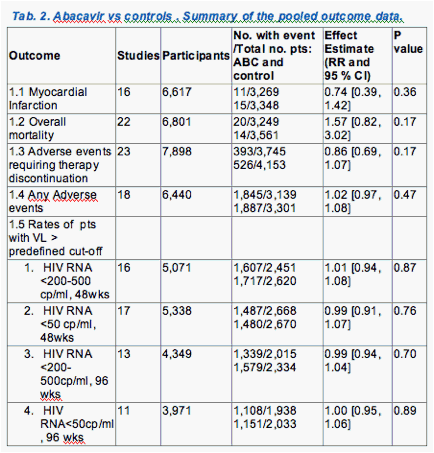
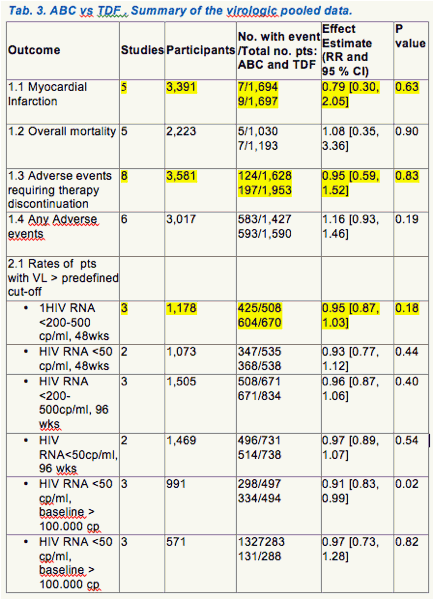
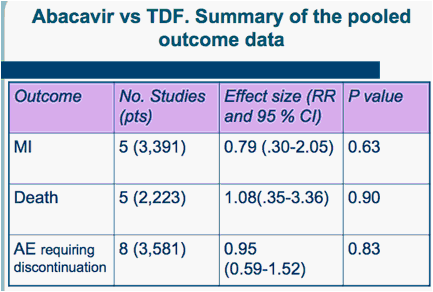
The main features of included studies are summarized in Table 1. Table 2 summarizes the pooled outcome data. Figure 1.1-1.5, are forest plots showing RR and 95 % CI for individual studies and pooled estimates of the meta-analysis. Table 3 and fig. 2.1-2.5 show the outcome data for the subgroup of studies from where a comparison between ABC and TDF was available (12-15, 23, 24, 30, 31)
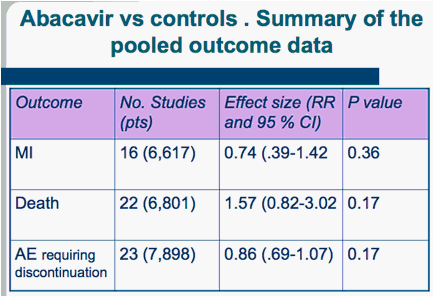
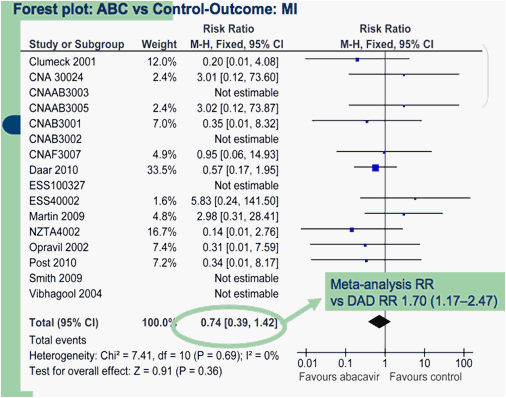
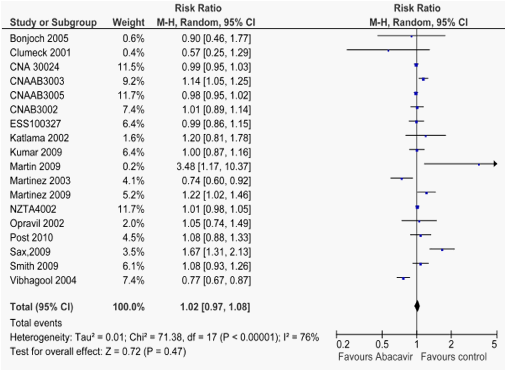
Data on MI were available from 16 RCTs (6,617 pts; 3,629 from published trials and 2,988 from data repository). There were 26 episodes of MI, 11 in ABC recipients, 15 in controls. In this calculation, however, we included data from the ACTG5202 (Daar et al, 2010), which include major vascular endpoint (e.g., coronary artery disease, infarct, ischemia, angina, cerebrovascular accident, transient ischemic attack or peripheral vascular disease) and not only MI (15). Compared to the controls, ABC use did not increase the occurrence of MI (RR, 0.74; 95 % CI, 0.39-1.42; p=0.36) (figure 1.1, table 2), the overall mortality (RR, 1.57; 95 % CI, 0.82-3.02; p=0.17) (table 2, fig. 1.2), and the occurrence of . adverse events, including those requiring discontinuation of therapy (table 2, fig 1.3, 1.4). The results were much the same in studies comparing ABC to tenofovir (tab. 3, fig 2.1.2.4)
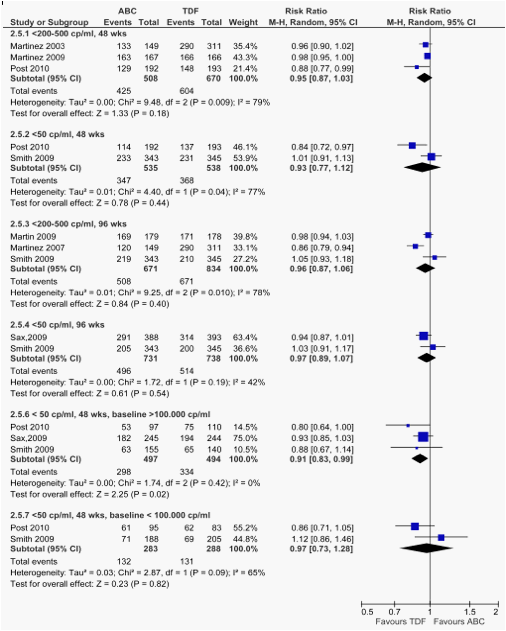
Rates of pts. with viral load below the predefined cut-off (<200-500, or < 50 copies/ml) at 48 and 96 wks are shown in table 2 and fig. 1.5 and, for the subgroup of studies with a direct comparison between ABC and TDF, in table 3 and fig 2.1. Rates were similar among ABC recipients and controls in all possible comparison, with the exception of the comparison between ABC and TDF at 48 wks in a subgroup of pts with baseline VL > 100,000 copies/ml .
DISCUSSION
Whether exposure to ABC increases the risk for MI is a debatable issue. Much of the evidence about the association between current or recent use of ABC and increased risk of cardiovascular disease is from the D:A:D study (2, 3). Since cohort studies do not control for all the potential confounding, this study has been subject to several criticisms. Potential confounding not adjusted for in the D:A:D study have been reported, including the fact that ABC had been preferentially prescribed to those with metabolic syndromes, lipoatrophy, dyslipidemia, renal disease, and CHD and that the study results reflected provider prescribing bias. Additionally it was noted that there was an inadequate duration of time to evaluate the effects of tenofovir, a nucleotide similarly prescribed as ABC except among those with renal disease (32). Actually, a significant independent association between decreased kidney function and increased risk of cardiovascular events in HIV-1-infected patients has been reported (33).
Some limitations of our analysis need to be addressed. First of all, pts in the D:A:D cohort were followed for period of time much longer that those recorded in the RCTs analyzed. However, it may be pointed out that only current or recent (within the last 6 months) use of ABC has been associated with an increased risk of cardiovascular disease within the setting of the DAD studies, and that a 24-96 week trial should be able to detect that. Moreover, these studies were not designed specifically to investigate differences in cardiovascular disease, though the occurrence of AE was consistently recorded.
Strenghts of our data include its high and consistent quality, collected from RCT, often double blind, designed to investigate comparatively the efficacy and safety of ABC containing HAART regimes
In summary, our analysis of randomised trial data from 29 RCTs and 9,611 pts showed that compared to the controls, ABC use did not increase the occurrence of MI (RR, 0.74; 95 % CI, 0.39-1.42; p=0.36) , the overall mortality (RR, 1.57; 95 % CI, 0.82-3.02; p=0.17)., and the occurrence of adverse events requiring discontinuation of therapy (RR 0.86; 95 % CI, 0.69-1.07; p=0.17).
Rates of pts. with viral load below the predefined cut-off (<200-500, or < 50 copies/ml) at 48 and 96 wks were similar among ABC recipients and controls in all possible comparison, with the exception of the comparison between ABC and TDF at 48 wks in a subgroup of pts with baseline VL > 100,000 copies/ml .
CONCLUSIONS
Observational studies are prone to biases and should be interpreted with caution given the potential for confounding. By contrast, randomized trials provide stronger evidence than do observational studies. Our meta-analysis was based on RCTs, and did not show an increase in the occurrence of Myocardial Infarction , overall mortality, and occurrence of severe adverse events in ABC recipients.
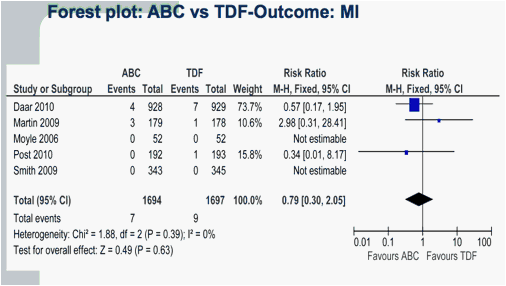
Figg. 2.1-2.2. Forest plot of comparison: ABC vs TDF : Myocardial Infarctiom (MI) and overall mortality.
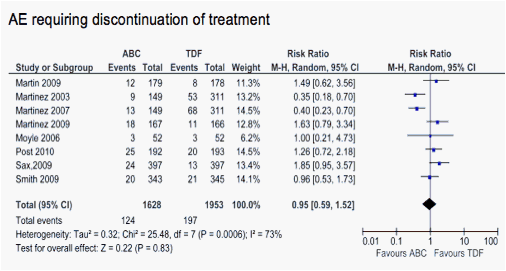
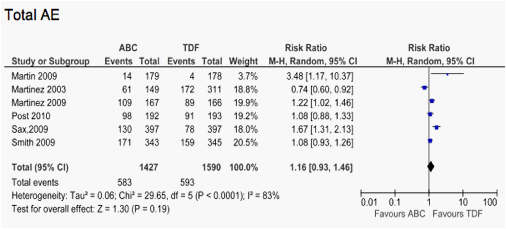
Figg 2.3-2.4. Forest plot of comparison: ABC vs TDF: Adverse Events (AE). Data from ACTG5202 (Sax et al) take account of reported grade 4 AE
1.1. Forest plot of comparison: Abacavir vs controls, outcome: Myocardial infarction. Data of ACTG5202 (Daar et al, 2010) refer to overall vascular events. RR calculated according to the Mantel -Haenszel (M-H) procedure. Not estimable= frequencies 0 in both treatment groups.


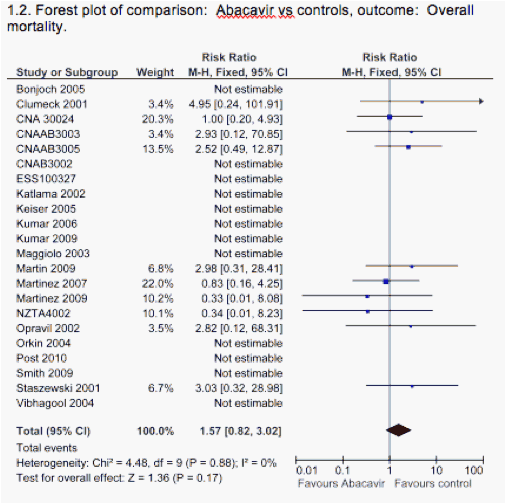
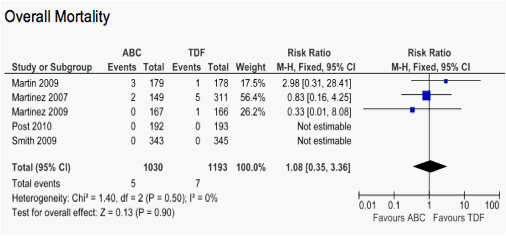
There were 34deaths, 20 in ABC, 14 in controls. Causes of death were reported only in 15 episodes (10 ABC, 6 controls), and were as follows: ABC: Lintoma or other cancer (4), Stevens-Johnson syndrome or hypersensitivity reaction (2 pts not screened for HLAB57), renal failure (1), accident (1), myocardial infarction (1), arrythmia (1). Controls: cancer (2), overdose (1), hepatic failure (1), sudden death (1).
1.3. Forest plot of comparison: Abacavir vs controls, outcome: Adverse events requiring therapy discontinuation
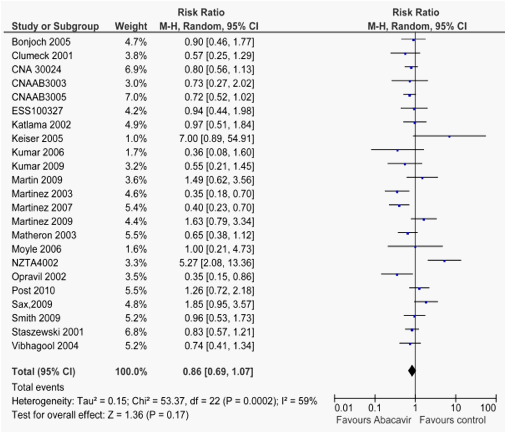
1.4. Forest plot of comparison: Abacavir vs controls, outcome: adverse events (any)
1.5. Forest plot of comparison: Abacavir vs controls, outcome: % of pts with HIV RNA < predefined cut-off, at 48 and 96 wks.
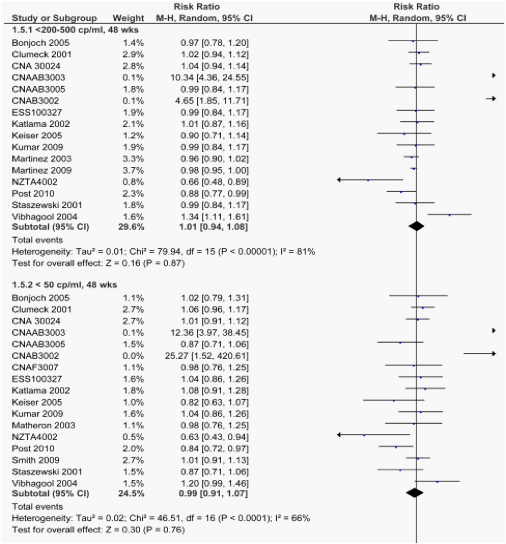
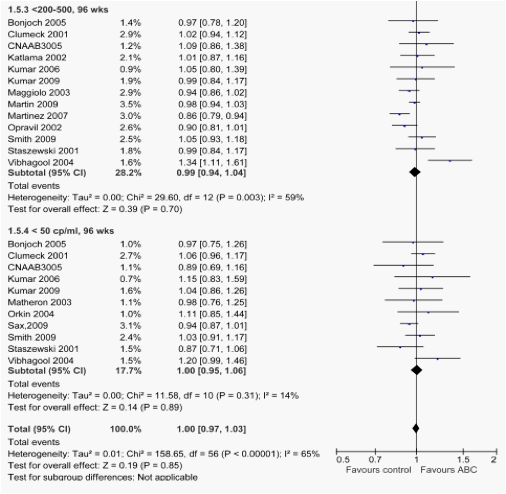
Fig. 2.5. Forest plot of comparison: Abacavir vsTDF, outcome: % of pts with HIV RNA < predefined cut-off, at 48 and 96 wks.
REFERENCES
1. The DAD Study Group. N Engl J Med 2007; 356(17):1723-35.
2. D:A:D Study Group, Sabin CA, Worm SW, Weber R, et al. Lancet 2008;371(9622):1417-26.
3. Lundgren J, Reiss P, Worm S et al. In: Abstract of the 16th Conference on retrovirus and opportunistic Infection (CROI), Montreal, february 2009. Abst. 44LB. 2009.
4. Lang S, Mary-Krause M, Cotte L et al.. In: 16th Conference on Retroviruses and Opportunistic Infections (CROI), Montreal, abstract 43LB, 2009.
5. Strategies for Management of Anti-Retroviral Therapy/INSIGHT; DAD Study Groups. Use of nucleoside reverse transcriptase inhibitors and risk of myocardial infarction in HIV-infected patients. AIDS 2008;22(14):F17-24.
6. Benson C, Ribaudo H, Zheng E et al. . 16th Conference on Retroviruses and Opportunistic Infections (CROI), Montreal, Abst. 721.
7. Brothers CH, Hernandez JE, Cutrell AG et al. Journal of the Acquired Immune Deficiency Syndrome. 2009;51:20-8.
8. Guyatt GH, Oxman AD, Kunz R, et al. BMJ. 2008; 336(7651):995-8.
9. Higgins JPT, Green S (editors). Cochrane Handbook for Systematic Reviews of Interventions Version 5.0.2 [updated September 2009]. The Cochrane Collaboration, 2009. Available from www.cochrane-handbook.org
10. Higgins J, Thompson S, Deeks J, Altman DTI. British Medical Journal 2003;32(7414):557-60.
11. GSK repository data on file
12. Smith KY, Patel P, Fine D, et al. 2009 Jul 31;23(12):1547-56.
13. Martin A, Bloch M, Amin J, Baker D, et al. Clin Infect Dis. 2009 Nov 15;49(10):1591-601.
14. Sax PE, Tierney C, Coclie AC et al. N Engl J Med, 2009 361 : 2230-40.
15 Daar E, Tierney C, Fischl M, et al. ACTG 5202: 17th Conference on Retroviruses & Opportunistic Infections (CROI 2010). San Francisco. February 16-19, 2010. Abstract 59LB.
16. Bonjoch A, Paredes R, Galvez J, et al.. J Acquir Immune Defic Syndr. 2005 Jul 1;39(3):313-6.
17 Clumeck N, Goebel F, Rozenbaum W, et al. AIDS. 2001 Aug 17;15(12):1517-26.
18. Katlama C, Fenske S, Gazzard B, et al. HIV Med. 2003 Apr;4(2):79-86.
19. Keiser PH, Sension MG, DeJesus E, et al. BMC Infect Dis. 2005 Jan 12;5(1):2.
20. Kumar PN, Rodriguez-French A, Thompson MA, et al. HIV Med. 2006 Mar;7(2):85-98.
21. Kumar PN, Salvato P, Lamarca A, et al. AIDS Res Ther. 2009 Apr 9;6:3.
22. Maggiolo F, Ripamonti D, Ravasio L, et al. AIDS. 2007; 21(3):367-9.
23 MartÃnez E, Arnaiz JA, Podzamczer D, et al. N Engl J Med. 2003 Sep 11;349(11):1036-46.
24 MartÃnez E, Arnaiz JA, Podzamczer D, et al. 2007 Jan 30;21(3):367-9.
25. MartÃnez E, Arranz JA, Podzamczer D, et al. J Acquir Immune Defic Syndr. 2009; 51(3):290-7.
26. Opravil M, Hirschel B, Lazzarin A, et al. J Infect Dis. 2002; 185(9):1251-60.
27. Orkin C, Stebbing J, Nelson M, Bower M, Johnson M, Mandalia S, Jones R, Moyle G, Fisher M, Gazzard B. J Antimicrob Chemother. 2005; 55(2):246-51.
28. Staszewski S, Keiser P, Montaner J, et al. JAMA. 2001 Mar 7;285(9):1155-63.
29. Vibhagool A, Cahn P, Schechter M, et al. Curr Med Res Opin. 2004 Jul;20(7):1103-14.
30. Post FA, Moyle GJ, Stellbrink HJ, et al. J Acquir Immune Defic Syndr. 2010 Apr 24.
31. Moyle GJ, Sabin CA, Cartledge J et al AIDS. 2006;20:2043-50
32. Aberg JA, Ribaudo H. J Infect Dis. 2010;201:315-7.
33. George E, Lucas GM, Nadkarni GN, Fine DM, Moore R, Atta MG. AIDS. 2010; 24:387-94.
|
| |
|
 |
 |
|
|