 |
 |
 |
| |
The ASPIRE Trial: TMC435 in treatment-experienced patients with genotype 1 HCV infection who have failed previous PegIFN/RBV treatment: Week 24 interim analysis
|
| |
| |
Reported by Jules Levin EASL 2011 Berlin Germany March 30-April 3
Stefan Zeuzem,1 Graham R Foster,2 Michael W Fried,3 Christophe Hezode,4 Gideon M Hirschfield,5 Igor Nikitin,6 Fred Poordad,7 Oliver Lenz,8 Monika Peeters,8 Vanitha Sekar,9 Goedele De Smedt8
1J.W. Goethe University Hospital, Frankfurt, Germany; 2Queen Marys University of London, London, United Kingdom; 3University of North Carolina at Chapel Hill, North Carolina, USA; 4Hôpital Henri-Mondor, Université Paris-Est Créteil, France; 5Toronto Western Hospital Liver Centre, Toronto, Canada;
6Russian State Medical University, Moscow, Russia; 7Cedars-Sinai Medical Center, Los Angeles, USA; 8Tibotec BVBA, Mechelen, Belgium; 9Tibotec Inc, Yardley, PA, USA

INTRODUCTION
· TMC435 is an investigational potent, once-daily oral NS3/4A protease inhibitor currently in Phase III clinical development for the treatment of hepatitis C virus (HCV) infection.
· Phase I, IIa and IIb studies, in treatment-experienced and/or treatment-naïve patients infected with HCV, have demonstrated that TMC435 is generally well tolerated, has a pharmacokinetic profile that supports a once-daily dosing regimen, and has potent antiviral activity in patients infected with genotypes 1, 2, 4, 5 and 6.1-7
· Phase III clinical trials are now underway in treatment-naïve patients and in patients who relapsed after previous treatment.
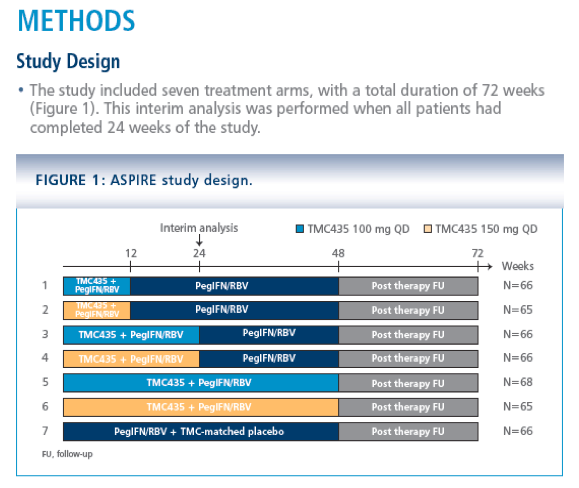
· ASPIRE (TMC435-C206; NCT00980330) is a Phase IIb, randomised, doubleblind, placebo-controlled trial to investigate the efficacy, tolerability, safety and pharmacokinetics of TMC435 as part of a treatment regimen including pegylated interferon a-2a and ribavirin (PegIFN/RBV).
· Patients enrolled in the ASPIRE trial were infected with HCV genotype 1, and had failed to respond or relapsed following at least one course of PegIFN/RBV therapy.

|
| |
|
 |
 |
|
|